Abstract
Behçet’s syndrome (BS) is a complex vasculitis, characterised by peculiar histological, pathogenetic and clinical features. Superficial venous thrombosis (SVT) and deep vein thrombosis (DVT) are the most frequent vascular involvements, affecting altogether 15–40% of BS patients. Atypical thrombosis is also an important clinical feature of BS, involving the vascular districts of the inferior and superior vena cava, suprahepatic veins with Budd–Chiari syndrome, portal vein, cerebral sinuses and right ventricle. On the other hand, arterial involvement, although affecting only 3–5% of patients, represents a unique feature of BS, with aneurysms potentially affecting peripheral, visceral and pulmonary arteries. Vascular events in BS are promoted by inflammation, with neutrophils playing a key role in the pathogenesis of thrombotic events; in turn, coagulative components such as fibrinogen, thrombin, factor Xa and factor VIIa amplify the inflammatory cascade. Understanding the contribution of inflammatory and coagulation components in the pathogenesis of BS vascular events is crucial to define the most effective therapeutic strategy. Control of vascular thrombosis is achieved with immunosuppressants drugs rather than anticoagulants. In particular, use of azathioprine and cyclosporine in association with low-dose corticosteroids should be considered in DVT and SVT cases, while treatment with cyclophosphamide together with anti-TNF-α agents can be effectively used in arterial involvement. More recently, the anti-TNF-α drugs have also been reported as a valid alternative for the treatment also of venous events, especially DVT. An exception to the use of anticoagulant in BS could be represented by cerebral veins thrombosis. In this review, we will depict the main characteristics of the vascular involvement in BS, briefly describing histological and pathogenetic features, while focusing on the clinical and therapeutical approaches of the vascular manifestations of BS.


Similar content being viewed by others
References
Silvestri E, Emmi G, Prisco D (2013) Vascular Behçet’s disease: new insights in the management of thrombosis. Expert Rev Cardiovasc Ther 11:1583–1585. https://doi.org/10.1586/14779072.2013.836449
Yazici H, Ugurlu S, Seyahi E (2012) Behçet syndrome: is it one condition? Clin Rev Allergy Immunol 43:275–280. https://doi.org/10.1007/s12016-012-8319-x
International Team for the Revision of the International Criteria for Behçet’s Disease (ITR-ICBD) F, Assaad-Khalil S, Calamia KT et al (2014) The International Criteria for Behçet’s Disease (ICBD): a collaborative study of 27 countries on the sensitivity and specificity of the new criteria. J Eur Acad Dermatol Venereol 28:338–347. https://doi.org/10.1111/jdv.12107
Jennette JC, Falk RJ, Bacon PA et al (2013) 2012 revised international chapel hill consensus conference nomenclature of vasculitides. Arthritis Rheum 65:1–11. https://doi.org/10.1002/art.37715
McDonald DR, Lee C, Fowler RA, Abuhaleeqa K (2007) Behcet’s disease. CMAJ 176:1273–1274. https://doi.org/10.1503/cmaj.061136
Boyd SR, Young S, Lightman S (2001) Immunopathology of the noninfectious posterior and intermediate uveitides. Surv Ophthalmol 46:209–233
Hirohata S, Kikuchi H (2009) Histopathology of the ruptured pulmonary artery aneurysm in a patient with Behçet’s disease. Clin Exp Rheumatol 27:S91–S95
Ergun T, Gürbüz O, Harvell J et al (1998) The histopathology of pathergy: a chronologic study of skin hyperreactivity in Behçet’s disease. Int J Dermatol 37:929–933
Verity DH, Wallace GR, Vaughan RW, Stanford MR (2003) Behçet’s disease: from Hippocrates to the third millennium. Br J Ophthalmol 87:1175–1183
Emmi G, Silvestri E, Squatrito D et al (2014) Behçet’s syndrome pathophysiology and potential therapeutic targets. Intern Emerg Med 9:257–265. https://doi.org/10.1007/s11739-013-1036-5
Consolandi C, Turroni S, Emmi G et al (2015) Behçet’s syndrome patients exhibit specific microbiome signature. Autoimmun Rev 14:269–276. https://doi.org/10.1016/j.autrev.2014.11.009
Aldinucci A, Bonechi E, Biagioli T et al (2018) CSF/serum matrix metallopeptidase-9 ratio discriminates neuro Behçet from multiple sclerosis. Ann Clin Transl Neurol 5:493–498. https://doi.org/10.1002/acn3.538
Emmi G, Silvestri E, Della Bella C et al (2016) Cytotoxic Th1 and Th17 cells infiltrate the intestinal mucosa of Behcet patients and exhibit high levels of TNF-α in early phases of the disease. Medicine 95:e5516. https://doi.org/10.1097/MD.0000000000005516 (Baltimore)
Aksu K, Donmez A, Keser G (2012) Inflammation-induced thrombosis: mechanisms, disease associations and management. Curr Pharm Des 18:1478–1493
Emmi G, Silvestri E, Squatrito D et al (2015) Thrombosis in vasculitis: from pathogenesis to treatment. Thromb J 13:15. https://doi.org/10.1186/s12959-015-0047-z
Matsumura N, Mizushima Y (1975) Leucocyte movement and colchicine treatment in Behcet’s disease. Lancet 2:813 (London, England)
Kawakami T, Ohashi S, Kawa Y et al (2004) Elevated serum granulocyte colony-stimulating factor levels in patients with active phase of sweet syndrome and patients with active behcet disease: implication in neutrophil apoptosis dysfunction. Arch Dermatol 140:570–574. https://doi.org/10.1001/archderm.140.5.570
Erkan F, Gül A, Tasali E (2001) Pulmonary manifestations of Behçet’s disease. Thorax 56:572–578
Mantovani A, Cassatella MA, Costantini C, Jaillon S (2011) Neutrophils in the activation and regulation of innate and adaptive immunity. Nat Rev Immunol 11:519–531. https://doi.org/10.1038/nri3024
Becatti M, Emmi G, Silvestri E et al (2016) Neutrophil activation promotes fibrinogen oxidation and thrombus formation in Behçet disease. Circulation 133:302–311. https://doi.org/10.1161/CIRCULATIONAHA.115.017738
Nasr H, Scriven JM (2015) Superficial thrombophlebitis (superficial venous thrombosis). BMJ 350:h2039. https://doi.org/10.1136/bmj.h2039
Sarr SA, Fall PD, Mboup MC et al (2015) Superior vena cava syndrome revealing a Behçet’s disease. Thromb J 13:7. https://doi.org/10.1186/s12959-015-0039-z
Lakhanpal S, Tani K, Lie JT et al (1985) Pathologic features of Behçet’s syndrome: a review of Japanese autopsy registry data. Hum Pathol 16:790–795
Hamuryudan V, Er T, Seyahi E et al (2004) Pulmonary artery aneurysms in Behçet syndrome. Am J Med 117:867–870. https://doi.org/10.1016/j.amjmed.2004.05.027
Saadoun D, Wechsler B, Desseaux K et al (2010) Mortality in Behçet’s disease. Arthritis Rheum 62:2806–2812. https://doi.org/10.1002/art.27568
Hughes JP, Stovin PG (1959) Segmental pulmonary artery aneurysms with peripheral venous thrombosis. Br J Dis Chest 53:19–27
Khalid U, Saleem T (2011) Hughes–Stovin syndrome. Orphanet J Rare Dis 6:15. https://doi.org/10.1186/1750-1172-6-15
Hatemi G, Christensen R, Bang D et al (2018) 2018 update of the EULAR recommendations for the management of Behçet’s syndrome. Ann Rheum Dis 77:808–818. https://doi.org/10.1136/annrheumdis-2018-213225
Vitale A, Rigante D, Lopalco G et al (2016) New therapeutic solutions for Behçet’s syndrome. Expert Opin Investig Drugs 25:827–840. https://doi.org/10.1080/13543784.2016.1181751
Ahn JK, Lee YS, Jeon CH et al (2008) Treatment of venous thrombosis associated with Behcet’s disease: immunosuppressive therapy alone versus immunosuppressive therapy plus anticoagulation. Clin Rheumatol 27:201–205. https://doi.org/10.1007/s10067-007-0685-z
Alibaz-Oner F, Karadeniz A, Ylmaz S et al (2015) Behçet disease with vascular involvement. Medicine 94:e494. https://doi.org/10.1097/MD.0000000000000494 (Baltimore)
Desbois AC, Wechsler B, Resche-Rigon M et al (2012) Immunosuppressants reduce venous thrombosis relapse in Behçet’s disease. Arthritis Rheum 64:2753–2760. https://doi.org/10.1002/art.34450
Emmi G, Vitale A, Silvestri E et al (2018) Adalimumab-based treatment versus DMARDs for venous thrombosis in Behçet syndrome. A retrospective study of 70 patients with vascular involvement. Arthritis Rheumatol 70:1500–1507. https://doi.org/10.1002/art.40531
Hamzaoui A, Fatima J, Thouraya BS et al (2014) Vena cava thrombosis in Behçet’s disease. Anadolu Kardiyol Derg 14:292–293. https://doi.org/10.5152/akd.2014.5042
Seyahi E, Caglar E, Ugurlu S et al (2015) An outcome survey of 43 patients with Budd–Chiari syndrome due to Behçet’s syndrome followed up at a single, dedicated center. Semin Arthritis Rheum 44:602–609. https://doi.org/10.1016/j.semarthrit.2014.10.014
Seyahi E, Hamuryudan V, Hatemi G et al (2007) Infliximab in the treatment of hepatic vein thrombosis (Budd–Chiari syndrome) in three patients with Behcet’s syndrome. Rheumatology 46:1213–1214. https://doi.org/10.1093/rheumatology/kem103 (Oxford)
Ben Ghorbel I, Belfeki N, Houman MH (2016) Intracardiac thrombus in Behçet’s disease. Reumatismo 68:148–153. https://doi.org/10.4081/reumatismo.2016.887
Wang H, Guo X, Tian Z et al (2016) Intracardiac thrombus in patients with Behcet’s disease: clinical correlates, imaging features, and outcome: a retrospective, single-center experience. Clin Rheumatol 35:2501–2507. https://doi.org/10.1007/s10067-015-3161-1
Prisco D, Silvestri E, Di Scala G, Emmi G (2018) Behçet’s disease as a cause of cerebral sinus vein thrombosis: an emerging role. Rheumatology. https://doi.org/10.1093/rheumatology/key279 (Oxford)
Uluduz D, Midi I, Duman T et al (2018) Behçet’s disease as a causative factor of cerebral venous sinus thrombosis: subgroup analysis of data from the VENOST study. Rheumatology 55:464. https://doi.org/10.1093/rheumatology/key153 (Oxford)
Saadoun D, Wechsler B, Resche-Rigon M et al (2009) Cerebral venous thrombosis in Behçet’s disease. Arthritis Rheum 61:518–526. https://doi.org/10.1002/art.24393
Shi J, Huang X, Li G et al (2018) Cerebral venous sinus thrombosis in Behçet’s disease: a retrospective case-control study. Clin Rheumatol 37:51–57. https://doi.org/10.1007/s10067-017-3718-2
Seyahi E, Melikoglu M, Akman C et al (2012) Pulmonary artery involvement and associated lung disease in Behçet disease: a series of 47 patients. Medicine 91:35–48. https://doi.org/10.1097/MD.0b013e318242ff37 (Baltimore)
Zhang X, Dai H, Ma Z et al (2015) Pulmonary involvement in patients with Behçet’s disease: report of 15 cases. Clin Respir J 9:414–422. https://doi.org/10.1111/crj.12153
Rossi GM, Emmi G, Vaglio A (2018) Hemoptysis in Behçet’s syndrome: from bedside to bench? Intern Emerg Med 13:467–469. https://doi.org/10.1007/s11739-018-1863-5
Voiriot G, Parrot A, Antoine M et al (2018) Transcatheter embolotherapy of pulmonary artery aneurysms as emergency treatment of hemoptysis in Behcet patients: experience of a referral center and a review of the literature. Intern Emerg Med 13:491–500. https://doi.org/10.1007/s11739-018-1817-y
Hamuryudan V, Seyahi E, Ugurlu S et al (2015) Pulmonary artery involvement in Behçet׳s syndrome: effects of anti-Tnf treatment. Semin Arthritis Rheum 45:369–373. https://doi.org/10.1016/j.semarthrit.2015.06.008
Hamuryudan V, Yurdakul S, Moral F et al (1994) Pulmonary arterial aneurysms in Behçet’s syndrome: a report of 24 cases. Rheumatology 33:48–51. https://doi.org/10.1093/rheumatology/33.1.48
Uzun O, Erkan L, Akpolat I et al (2008) Pulmonary involvement in Behçet’s disease. Respiration 75:310–321. https://doi.org/10.1159/000101954
Balcioglu O, Ertugay S, Bozkaya H et al (2015) Endovascular repair and adjunctive immunosuppressive therapy of aortic involvement in Behçet’s disease. Eur J Vasc Endovasc Surg 50:593–598. https://doi.org/10.1016/j.ejvs.2015.07.011
Kwon Koo B, Shim W-H, Yoon Y-S et al (2003) Endovascular therapy combined with immunosuppressive treatment for pseudoaneurysms in patients with Behçet’s disease. J Endovasc Ther 10:75–80. https://doi.org/10.1177/152660280301000116
Seyahi E (2016) Behçet’s disease: how to diagnose and treat vascular involvement. Best Pract Res Clin Rheumatol 30:279–295. https://doi.org/10.1016/j.berh.2016.08.002
Vitale A, Emmi G, Lopalco G et al (2017) Adalimumab effectiveness in Behçet’s disease: short and long-term data from a multicenter retrospective observational study. Clin Rheumatol 36:451–455. https://doi.org/10.1007/s10067-016-3417-4
Fabiani C, Vitale A, Rigante D et al (2018) Predictors of sustained clinical response in patients with Behçet’s disease-related uveitis treated with infliximab and adalimumab. Clin Rheumatol 37:1715–1720. https://doi.org/10.1007/s10067-018-4092-4
Fabiani C, Sota J, Vitale A et al (2018) Cumulative retention rate of adalimumab in patients with Behçet’s disease-related uveitis: a 4-year follow-up study. Br J Ophthalmol 102:637–641. https://doi.org/10.1136/bjophthalmol-2017-310733
Fabiani C, Vitale A, Emmi G et al (2017) Efficacy and safety of adalimumab in Behçet’s disease-related uveitis: a multicenter retrospective observational study. Clin Rheumatol 36:183–189. https://doi.org/10.1007/s10067-016-3480-x
Lopalco G, Emmi G, Gentileschi S et al (2017) Certolizumab Pegol treatment in Behcet’s disease with different organ involvement: a multicenter retrospective observational study. Mod Rheumatol 27:1031–1035. https://doi.org/10.1080/14397595.2017.1285857
Vitale A, Emmi G, Lopalco G et al (2018) Correction to: long-term efficacy and safety of golimumab in the treatment of multirefractory Behçet’s disease. Clin Rheumatol 5:123. https://doi.org/10.1007/s10067-018-4302-0
Acknowledgements
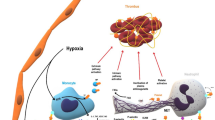
This study was not funded. The authors wish to thank Stefano Salvati and Javier Hernández Plasencia for their help in preparing Fig. 2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no conflict of interest.
Statement of human and animal rights
This study does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent is not applicable to this study (review).
Additional information
This article is part of the topical collection “Behcet Disease”.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Emmi, G., Bettiol, A., Silvestri, E. et al. Vascular Behçet’s syndrome: an update. Intern Emerg Med 14, 645–652 (2019). https://doi.org/10.1007/s11739-018-1991-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-018-1991-y