Background
Roux-en-Y gastric bypass (RYGBP) effectively produces massive weight reduction, improving health in morbidly obese patients. The mechanisms for the weight loss, and the fate of the excluded gastric mucosa, are not fully clarified. To what extent the appetite-stimulating gastric peptide ghrelin is affected remains controversial.
Methods
Circulating concentrations of ghrelin, pancreatic polypeptide (PP), pepsinogen I (PGI) and gastrin were examined in 15 morbidly obese patients (median BMI 45 kg/m2) preoperatively, and on days 1, 2, 4, 6 and at months 1, 6 and 12 after RYGBP.
Results
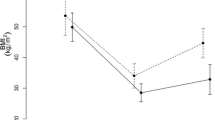
Ghrelin levels fell on postoperative day 1 and increased after 1 month to preoperative levels, and rose further at 6 and 12 months. PP concentrations decreased on day 1 and subsequently returned to preoperative levels. PGI levels peaked transiently the first days after surgery and subsequently declined to lower than preoperative levels. Gastrin levels were gradually reduced postoperatively.
Conclusion
Ghrelin and PP fall transiently after surgery, possibly due to vagal dysfunction, and ultimately, as weight loss ensues, ghrelin secretion increases to higher than preoperative levels. The RYBGP procedure affects the gastric mucosa, as reflected by a transient increase in circulating PGI, and subsequently, the mucosa in the excluded stomach is at rest, as shown by low levels of PGI and gastrin.
Similar content being viewed by others
References
Cummings DE, Weigle DS, Frayo RS et al. Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery. N Engl J Med 2002; 346: 1623–30.
Flier JS, Maratos-Flier E. The stomach speaks – ghrelin and weight regulation. N Engl J Med 2002; 346: 1662–3.
Frühbeck G, Diez Caballero A, Gil MJ. Fundus functionality and ghrelin concentrations after bariatric surgery. N Engl J Med 2004; 350: 308–9.
Frühbeck G, Rotellar F, Hernandez-Lizoain JL et al. Fasting plasma ghrelin concentrations 6 months after gastric bypass are not determined by weight loss or changes in insulinemia. Obes Surg 2004; 14: 1208–15.
Maier C, Schaller G, Buranyi B et al. The cholinergic system controls ghrelin release and ghrelin-induced growth hormone release in humans. J Clin Endocrinol Metab 2004; 89: 4729–33.
Broglio F, Gottero C, van Koetsveld P et al. Acetycholine regulates ghrelin secretion in humans. J Clin Endocrinol Metab 2004; 89: 2429–33.
le Roux CW, Neary NM, Halsey TJ et al. Ghrelin does not stimulate food intake in patients with surgical procedures involving vagotomy. J Clin Endocrinol Metab 2005; 90: 4521–4.
Katsuura G, Asakawa A, Inui A. Roles of pancreatic polypeptide in regulation of food intake. Peptides 2002; 23: 323–9.
Schwartz TW. Pancreatic polypeptide: a hormone under vagal control. Gastroenterology 1983; 85: 1411–25.
Schwartz TW, Holst JJ, Fahrenkrug J et al. Vagal, cholinergic regulation of pancreatic polypeptide secretion. J Clin Invest 1978; 61: 781–9.
Katschinski M. Nutritional implications of cephalic phase gastrointestinal responses. Appetite 2000; 34: 189–96.
Vozarova de Courten B, Weyer C, Stefan N et al. Parasympathetic blockade attenuates augmented pancreatic polypeptide but not insulin secretion in Pima Indians. Diabetes 2004; 53: 663–71.
Balaji NS, Crookes PF, Banki F et al. A safe and noninvasive test for vagal integrity revisited. Arch Surg 2002; 137: 954–8.
Greydanus MP, Vassallo M, Camilleri M et al. Neurohormonal factors in functional dyspepsia: Insights on pathophysiological mechanisms. Gastroenterology 1991; 100: 1311–8.
Taylor IL, Feldman M, Richardson CT et al. Gastric and cephalic stimulation of human pancreatic polypeptide release. Gastroenterology 1978; 75: 432–7.
Feldman M, Richardson CT. Role of thought, sight, smell, and taste of food in the cephalic phase of gastric acid secretion in humans. Gastroenterology 1986; 90: 428–33.
Mårdh E, Mårdh S, Mårdh B et al. Diagnosis of gastritis by means of a combination of serological analyses. Clin Chim Acta 2002; 320: 17–27.
Samloff IM, Varis K, Ihamaki T et al. Relationships among serum pepsinogen I, serum pepsinogen II, and gastric mucosal histology. A study in relatives of patients with pernicious anaemia. Gastroenterology 1982; 83: 204–9.
Lindgren A, Burman P, Kilander AF et al. Serum antibodies to H+, K+−ATPase, serum pepsinogen A and Helicobacter pylori in relation to gastric mucosa morphology in patients with low or low-normal concentrations of serum cobalamins. Eur J Gastroenterol Hepatol 1998; 10: 583–8.
Samloff IM, Stermmermann GN, Heilbrun K et al. Elevated serum pepsinogen I and II levels differ as risk factors for duodenal ulcer and gastric ulcer. Gastroenterology 1986; 90: 570–6.
Ohkusa T, Takashimizu I, Fujiki K et al. Changes in serum pepsinogen, gastrin, and immunoglobulin G antibody titers in helicobacter pylori-positive gastric ulcer after eradication of infection. J Clin Gastroenterol 1997; 25: 317–22.
Kodoi A, Yoshihara M, Sumii K et al. Serum pepsinogen in screening for gastric cancer. J Gastroenterology 1995; 30: 452–60.
Yoshihara M, Sumii K, Haruma K et al. Correlation of ratio of serum pepsinogen I and II with prevalence of gastric cancer and adenoma in Japanese subjects. Am J Gastroenterol 1998; 93: 1090–6.
Kitahara F, Kobayashi K, Sato T et al. Accuracy of screening for gastric cancer using serum pepsinogen concentrations. Gut 1999; 44: 693–7.
Sundbom M, Mardh E, Mardh S et al. Reduction in serum pepsinogen I after Roux-en-Y gastric bypass. J Gastrointest Surg 2003; 7: 529–35.
Holdstock C, Engstrom BE, Ohrvall M et al. Ghrelin and adipose tissue regulatory peptides: effect of gastric bypass surgery in obese humans. J Clin Endocrinol Metab 2003; 88: 3177–83.
Faraj M, Havel PJ, Phelis S et al. Plasma acylationstimulating protein, adiponectin, leptin, and ghrelin before and after weight loss induced by gastric bypass surgery in morbidly obese subjects. J Clin Endocrinol Metab 2003; 88: 1594–602.
Vendrell J, Broch M, Vilarrasa N et al. Resistin, adiponectin, ghrelin, leptin, and proinflammatory cytokines: relationships in obesity. Obes Res 2004; 12: 962–71.
Stoeckli R, Chanda R, Langer I et al. Changes of body weight and plasma ghrelin levels after gastric banding and gastric bypass. Obes Res 2004; 12: 346–50.
Tritos NA, Mun E, Bertkau A et al. Serum ghrelin levels in response to glucose load in obese subjects postgastric bypass surgery. Obes Res 2003; 11: 919–24.
Lin E, Gletsu N, Fugate K et al. The effects of gastric surgery on systemic ghrelin levels in the morbidly obese. Arch Surg 2004; 139: 780–4.
Latarjet A. Section des rameaux gastriques du vague. La Presse Med 1921; 41: 409.
McCrea ED. The abdominal distribution of the vagus. J Anat (London) 1924; 59: l8–40.
Asakawa A, Inui A, Kaga T et al. Ghrelin is an appetite-stimulatory signal from stomach with structural resemblance to motilin. Gastroenterology 2001; 120: 337–45.
Date Y, Murakami N, Toshinai K et al. The role of the gastric afferent vagal nerve in ghrelin-induced feeding and growth hormone secretion in rats. Gastroenterology 2002; 123: 1120–8.
Arosio M, Ronchi CL, Beck-Peccoz P et al. Effects of modified sham feeding on ghrelin levels in healthy human subjects. J Clin Endocrinol Metab 2004; 89: 5101–4.
Simonian HP, Kresge KM, Boden GH et al. Differential effects of sham feeding and meal ingestion on ghrelin and pancreatic polypeptide levels: evidence for vagal efferent stimulation mediating ghrelin release. Neurogastroenterol Motil 2005; 17: 348–54.
Granstrom L, Backman L, Uvnas-Moberg K. Serum gastrin, insulin and somatostatin levels in normal and obese subjects before and after gastric banding. Acta Chir Scand 1988; 154: 117–21.
Sundbom M, Nyman R, Hedenstrom H et al. Investigation of the excluded stomach after Roux-en-Y gastric bypass. Obes Surg 2001; 11: 25–37.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sundbom, M., Holdstock, C., Engström, B.E. et al. Early Changes in Ghrelin following Roux-en-Y Gastric Bypass: Influence of Vagal Nerve Functionality?. OBES SURG 17, 304–310 (2007). https://doi.org/10.1007/s11695-007-9056-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-007-9056-8