Abstract
Background
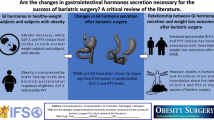
The Roux-en-Y gastric bypass (RYGB) is the gold standard bariatric operation. However, a major concern in late follow-up is the substantial weight regain. Understanding the role of gastrointestinal hormone secretion in this situation is relevant.
Methods
The aim of the present study was to evaluate the influence of gastrointestinal hormones comparing postprandial secretion of ghrelin, glucose-dependent insulinotropic polypeptide (GIP), glucagon-like peptide 1 (GLP-1), and leptin between patients with weight regain and those with favorable weight control. Twenty-four patients with follow-up from 27 to 59 months were divided into two groups according to sustained weight loss: group A (14 patients) had sustained weight losses, and group B (10 patients) had significant weight regain. Basal serum levels of ghrelin, GIP, GLP-1, and leptin after fasting and 30, 60, 90, and 120 min after a standard meal were measured.
Results
There was no difference in the ghrelin secretion. There was a difference in the GIP secretion, with a higher percentage increase in 30 min in group A (330 % × 192.2 %; p = 0.01). There were also differences in the GLP-1 secretion, with higher increases in absolute (p = 0.03) and percentage values after 30 min in group A (124 % × 46.5 %; p = 0.01). There was also a difference between baseline leptin values, with higher levels in group B (p = 0.02).
Conclusions
The secretion of gut hormones in patients with weight regain after RYGB is different from that in patients with satisfactory weight outcome. After meal stimulation, reduced levels of GIP and GLP-1 may indicate the influence of gut hormones in the process of weight regain.





Similar content being viewed by others
References
Campos JM, Lins DC, Silva LB, et al. Metabolic surgery, weight regain and diabetes re-emergence. Arq Bras Cir Dig. 2013;26 Suppl 1:57–62.
Chikunguwo SM, Wolfe LG, Dodson P, et al. Analysis of factors associated with durable remission of diabetes after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2010;6(3):254–9.
DiGiorgi M, Rosen DJ, Choi JJ, et al. Re-emergence of diabetes after gastric bypass in patients with mid- to long-term follow-up. Surg Obes Relat Dis. 2010;6(3):249–53.
Pajecki D, Dalcanalle L, Souza de Oliveira CP, et al. Follow-up of roux-en-Y gastric bypass patients at 5 or more years postoperatively. Obes Surg. 2007;17(5):601–7.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Magro DO, Geloneze B, Delfini R, et al. Long-term weight regain after gastric bypass: a 5-year prospective study. Obes Surg. 2008;18(6):648–51.
Sjöström L, Lindroos AK, Peltonen M, et al. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351(26):2683–93.
Bastos ECL, Barbosa EMWG, Soriano GMS, et al. Fatores determinantes do reganho ponderal no pós-operatório de cirurgia bariátrica. ABCD, Arq Bras Cir Dig. 2013;26 Suppl 1:26–32.
Biron S, Hould FS, Lebel S, et al. Twenty years of biliopancreatic diversion: what is the goal of the surgery? Obes Surg. 2004;14(2):160–4.
Himpens J, Coromina L, Verbrugghe A, et al. Outcomes of revisional procedures for insufficient weight loss or weight regain after roux-en-Y gastric bypass. Obes Surg. 2012;22(11):1746–54.
Shah M, Simha V, Garg A. Review: long-term impact of bariatric surgery on body weight, comorbidities, and nutritional status. J Clin Endocrinol Metab. 2006;91(11):4223–31 [Review].
Valezi AC, Mali J, de Menezes MA, et al. Weight loss outcome after Silastic ring roux-en-Y gastric bypass: 8 years of follow-up. Obes Surg. 2010;20(11):1491–5.
Meguid MM, Glade MJ, Middleton FA. Weight regain after roux-en-Y: a significant 20% complication related to PYY. Nutrition. 2008;24(9):832–42.
Le Roux CW, Welbourn R, Werling M, et al. Gut hormones as mediators of appetite and weight loss after roux-en-Y gastric bypass. Ann Surg. 2007;246(5):780–5.
Pedersen SD. The role of hormonal factors in weight loss and recidivism after bariatric surgery. Gastroenterol Res Pract. 2013;2013:528450.
Murphy KG, Bloom SR. Gut hormones and the regulation of energy homeostasis. Nature. 2006;444(7121):854–9.
Brunner E, Puri ML. Nonparametric methods in factorial designs. Stat Pap. 2001;42(1):1–52.
R Core Team. R: A language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2013.
Christou NV, Look D, Maclean LD. Weight gain after short- and long-limb gastric bypass in patients followed for longer than 10 years. Ann Surg. 2006;244(5):734–40.
Karmali S, Brar B, Shi X, et al. Weight recidivism post-bariatric surgery: a systematic review. Obes Surg. 2013;23(11):1922–33.
Das SK, Roberts SB, McCrory MA, et al. Long-term changes in energy expenditure and body composition after massive weight loss induced by gastric bypass surgery. Am J Clin Nutr. 2003;78(1):22–30.
Le Roux CW, Bueter M, Theis N, et al. Gastric bypass reduces fat intake and preference. Am J Physiol Regul Integr Comp Physiol. 2011;301(4):R1057–66.
Begg DP, Woods SC. The endocrinology of food intake. Nat Rev Endocrinol. 2013;9(10):584–97.
Berthoud HR, Shin AC, Zheng H. Obesity surgery and gut-brain communication. Physiol Behav. 2011;105(1):106–19.
Beglinger C, Degen L. Gastrointestinal satiety signals in humans—physiologic roles for GLP-1 and PYY? Physiol Behav. 2006;89(4):460–4 [Review].
Cummings DE, Overduin J. Gastrointestinal regulation of food intake. J Clin Invest. 2007;117(1):13–23.
Meier JJ, Gallwitz B, Nauck MA. Glucagon-like peptide 1 and gastric inhibitory polypeptide: potential applications in type 2 diabetes mellitus. Biodrugs. 2003;17(2):93–102 [Review].
Ferrannini E, Camastra S, Gastaldelli A, et al. Beta-cell function in obesity: effects of weight loss. Diabetes. 2004;53 Suppl 3:S26–33.
Mingrone G. Role of the incretin system in the remission of type 2 diabetes following bariatric surgery. Nutr Metab Cardiovasc Dis. 2008;18(8):574–9.
Näslund E, Kral JG. Impact of gastric bypass surgery on gut hormones and glucose homeostasis in type 2 diabetes. Diabetes. 2006;55 Suppl 2:S92–7.
De Silva A, Bloom SR. Gut hormones and appetite control: a focus on PYY and GLP-1 as therapeutic targets in obesity. Gut Liver. 2012;6(1):10–20.
Umeda LM, Silva EA, Carneiro G, et al. Early improvement in glycemic control after bariatric surgery and its relationships with insulin, GLP-1, and glucagon secretion in type 2 diabetic patients. Obes Surg. 2011;21(7):896–901.
Dirksen C, Damgaard M, Bojsen-Møller KN, et al. Fast pouch emptying, delayed small intestinal transit, and exaggerated gut hormone responses after roux-en-Y gastric bypass. Neurogastroenterol Motil. 2013;25(4):346–e255.
Cummings DE, Weigle DS, Frayo RS, et al. Plasma ghrelin levels after diet-induced weight loss or gastric bypass surgery. N Engl J Med. 2002;346(21):1623–30.
Geloneze B, Tambascia MA, Pilla VF, et al. Ghrelin: a gut-brain hormone: effect of gastric bypass surgery. Obes Surg. 2003;13(1):17–22.
Rindi G, Torsello A, Locatelli V, et al. Ghrelin expression and actions: a novel peptide for an old cell type of the diffuse endocrine system. Exp Biol Med (Maywood). 2004;229(10):1007–16.
Rubino F. Bariatric surgery: effects on glucose homeostasis. Curr Opin Clin Nutr Metab Care. 2006;9(4):497–507.
Korner J, Bessler M, Inabnet W, et al. Exaggerated glucagon-like peptide-1 and blunted glucose-dependent insulinotropic peptide secretion are associated with roux-en-Y gastric bypass but not adjustable gastric banding. Surg Obes Relat Dis. 2007;3(6):597–601.
Laferrère B, Teixeira J, McGinty J, et al. Effect of weight loss by gastric bypass surgery versus hypocaloric diet on glucose and incretin levels in patients with type 2 diabetes. J Clin Endocrinol Metab. 2008;93(7):2479–85.
Laferrère B, Reilly D, Arias S, et al. Differential metabolic impact of gastric bypass surgery versus dietary intervention in obese diabetic subjects despite identical weight loss. Sci Transl Med. 2011;3(80):80re2.
Rao RS, Kini S. GIP and bariatric surgery. Obes Surg. 2011;21(2):244–52.
DePaula AL, Macedo AL, Schraibman V, et al. Hormonal evaluation following laparoscopic treatment of type 2 diabetes mellitus patients with BMI 20–34. Surg Endosc. 2009;23(8):1724–32.
Reinehr T, Roth CL, Schernthaner GH, et al. Peptide YY and glucagon-like peptide-1 in morbidly obese patients before and after surgically induced weight loss. Obes Surg. 2007;17(12):1571–7.
Santoro S, Castro LC, Velhote MC, et al. Sleeve gastrectomy with transit bipartition: a potent intervention for metabolic syndrome and obesity. Ann Surg. 2012;256(1):104–10.
Dirksen C, Jørgensen NB, Bojsen-Møller KN, et al. Gut hormones, early dumping and resting energy expenditure in patients with good and poor weight loss response after Roux-en-Y gastric bypass. Int J Obes. 2013;37(11):1452–9.
Morínigo R, Vidal J, Lacy AM, et al. Circulating peptide YY, weight loss, and glucose homeostasis after gastric bypass surgery in morbidly obese subjects. Ann Surg. 2008;247(2):270–5.
Geloneze B, Tambascia MA, Pareja JC, et al. Serum leptin levels after bariatric surgery across a range of glucose tolerance from normal to diabetes. Obes Surg. 2001;11(6):693–8.
Acknowledgments
We thank Mrs. Marta Rodrigues, librarian, for the bibliographical references, Ms. Priscila Caproni, biologist, for organization of data and laboratory tests collection, and Prof. Julio Pereira and Dr. Márcio Diniz for the statistical analyses.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Funding
No grant support
Rights and permissions
About this article
Cite this article
Santo, M.A., Riccioppo, D., Pajecki, D. et al. Weight Regain After Gastric Bypass: Influence of Gut Hormones. OBES SURG 26, 919–925 (2016). https://doi.org/10.1007/s11695-015-1908-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-015-1908-z