Abstract
Background
The stemless Simpliciti shoulder prosthesis has been available since 2010. To date, there are no scientific results on this type of prosthesis with a follow-up of more than 24–35 months. The aim of this retrospective study was to evaluate the clinical and radiological results of the Simpliciti shoulder system in a mid-term follow-up of 4–8 years.
Material and methods
Between April 2011 and December 2014, the Simpliciti shoulder system was implanted in 110 shoulders in 93 patients. After a mean follow-up of 72 (49–106) months, 98 shoulders (89.1%) in 93 patients with an average age of 72.7 years were available for clinical and radiological follow-up. There were 10 hemi-shoulder arthroplasties (HSA) and 88 total shoulder arthroplasties (TSA). Clinical examination, ultrasound of the rotator cuff, Subjective Shoulder Value (SSV), Quick-DASH (QDASH), Constant score (CS), range of motion, and radiographs were evaluated.
Results
All shoulders showed good clinical results. The mean SSV was 86% (HSA 79%, TSA 87%). The mean QDASH was 12 points (HSA 22, TSA 10). The mean CS improved from 32.2 to 75.4 ± 10.9 points (p < 0.005; HSA 70.4, TSA 76.0). The average age-adjusted CS was 89.7% ± 12.4% (HSA 82.1%, TSA 90.7%). The mean flexion was 141.4°, the mean abduction was 124.5°, and the mean external rotation was 47.2°. A pain reduction from 3.7 to 13.3 points in CS was achieved. Good anatomical reconstruction of the center of rotation and radius of curvature was evaluated in the postoperative radiographs. Bone resorption in unloaded bone of the humeral head was frequent but without any clinical impact.
Conclusion
The stemless Simpliciti shoulder prosthesis demonstrated very good clinical and radiological mid-term results, comparable to stemmed prostheses. Further follow-up is needed to determine the long-term results.
Zusammenfassung
Hintergrund
Die schaftfreie Simpliciti-Schulterprothese (Fa. Stryker, Kalamazoo, MI, USA) ist seit 2010 erhältlich. Derzeit liegen keine wissenschaftlichen Ergebnisse zu diesem Prothesentyp vor, die über ein Follow-up von mehr als 24–35 Monaten hinausgehen. Ziel dieser retrospektiven Studie war es, klinische und radiologische Ergebnisse des Simpliciti-Schultersystems mit einem mittelfristigen Follow-up von 4–8 Jahren zu untersuchen.
Material und Methoden
Zwischen April 2011 und Dezember 2014 wurde das Simpliciti-Schultersystem in 110 Schultern bei 93 Patienten implantiert. Nach einem mittleren Follow-up von 72 (49–106) Monaten standen 98 Schultern (89,1 %) von 93 Patienten mit einem Durchschnittsalter von 72,7 Jahren für die klinische und radiologische Nachuntersuchung zur Verfügung. Es wurden 10 Hemiendoprothesen (HSA) und 88 Totalendoprothesen (TSA) nachuntersucht. Ausgewertet wurden, die klinischen Untersuchungsergebnisse, Ultraschalluntersuchung der Rotatorenmanschette, Subjective Shoulder Value (SSV), Quick-DASH (QDASH), Constant-Score (CS), Bewegungsumfang und Röntgenaufnahmen der operierten Schulter.
Ergebnisse
Alle Schultern zeigten gute klinische Ergebnisse. Der mittlere SSV betrug 86 % (HSA 79 %; TSA 87 %). Der mittlere QDASH betrug 12 Punkte (HSA 22; TSA 10). Der mittlere CS verbesserte sich von 32,2 auf 75,9 ± 10,9 Punkte (p < 0,005; HSA 70,4; TSA 76,0). Der durchschnittliche alters- und geschlechtsadaptierte CS betrug 89,7 % ± 12,4 % (HSA 82,1 %; TSA 90,7 %). Die durchschnittliche Flexion lag bei 141,4°, die durchschnittliche Abduktion bei 124,5° und die durchschnittliche Außenrotation bei 47,2°. Es wurde eine Schmerzreduktion von 3,7 auf 13,3 Punkte im CS erreicht. In den postoperativen Röntgenbildern wurde eine gute anatomische Rekonstruktion des Rotationszentrums und des Krümmungsradius nachgewiesen. Knochenresorption im unbelasteten Knochen des Humeruskopfs wurde häufig beobachtet, hatte aber keinerlei klinische Relevanz.
Schlussfolgerung
Die schaftfrei Simpliciti-Schulterprothese zeigte im mittelfristigen Follow-up sehr gute klinische und radiologische Ergebnisse, die mit denen von Schaftprothesen vergleichbar sind. Weitere Nachuntersuchungen sind erforderlich, um die Langzeitergebnisse zu ermitteln.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Since Neer’s stemmed monoblock shoulder prosthesis from 1955, shoulder prostheses have evolved and become more anatomic with shorter stems and more modularity options to enable an exact recreation of the shoulder joint. Stemless shoulder prostheses have been available since the early 2000s and ever since then there has been a clear trend toward stemless implants [9]. With the use of stemless implants, stem-related complications such as periprosthetic fractures or stress shielding can be avoided. The metaphyseal fixation also offers several advantages including shorter operation time, less blood loss, and conservation of meta- and diaphyseal bone stock [10, 18].
For most stemless shoulder protheses, only short-term results are available, and for a few implants mid- to long-term results have been published showing very good clinical and radiological results, absolutely comparable to stemmed prostheses [1, 6, 7, 10].
The stemless press-fit Simpliciti shoulder system (Stryker, Kalamazoo, MI, USA) has been available since 2010 but to date only short-term results are available [2, 4]. The aim of this retrospective study was to evaluate the clinical and radiological results of the stemless Simpliciti shoulder prosthesis in a mid-term follow-up of 4–8 years.
Materials and methods
The study was reviewed by the local ethics committee (study number AZ-319/17) and informed consent was obtained from all individual participants included in the study.
A single-center, retrospective, single-arm study was performed. The first consecutive 105 patients (110 shoulders) with implantation of the Simplicti shoulder system between April 2011 and December 2014 were assessed.
Simplicti shoulder system
The stemless Simpliciti shoulder prosthesis is a two-piece system consisting of a humeral component called “the nucleus” and “the humeral head” implant. The nucleus is available in three sizes and has a three-fin design with a sintered porous coating on the fins and on the undersurface. The coating enables a press-fit impaction with a stable initial fixation and excellent bone ingrowth for long-term stability. A female morse taper in the nucleus facilitates exploration of the glenoid with the nucleus in place in the case of a revision operation. With several humeral heads in a variety of heights and diameters, an anatomical reconstruction and good soft-tissue balancing can be achieved. The humeral head and the nucleus are connected by press-fit. It can be used as hemi-shoulder arthroplasty (HSA) or as total shoulder arthroplasty (TSA). In this study, for TSA the cemented Aequalis keeled glenoid (former Wright Medical Group N.V., Memphis, TN, USA) was used until January 2014 and after that the cemented Tornier Perform anatomic glenoid (Stryker, Kalamazoo, MI, USA) was implanted.
Surgical technique
All surgical procedures were performed by one specialized high-volume shoulder surgeon with the patient in beach chair position and under general anesthesia. A standard deltopectoral surgical approach was used and subscapularis management was performed by peel-off. All patients underwent soft-tissue tenodesis of the long head of the biceps. Humeral osteotomy was performed at the anatomic neck. In the case of isolated humeral osteoarthritis, an HSA was performed. If the head and glenoid were involved, a TSA was performed. Subscapularis repair was carried out by using three transosseous non-absorbable sutures. All patients had a standardized rehabilitation protocol with the arm immobilized in a shoulder sling for 6 weeks and continuous passive motion exercises on day 1 after surgery.
Clinical examination and scores
During follow-up, all patients underwent a standardized clinical examination for motion (ROM) and function of the rotator cuff (RC). In addition to the clinical examination, the integrity of the RC was assessed by ultrasound at the follow-up appointment. The Subjective Shoulder Value (SSV), Quick-DASH (QDASH), Constant Score (CS), and age- and gender-adjusted Constant Score (nCS) were determined. Abduction strength for CS was measured using the IsoForceControl® EVO2 dynamometer (Herkules Kunststoff AG, Oberburg, Switzerland).
Radiographic assessment
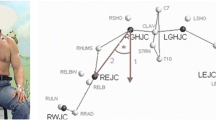
Preoperative and postoperative x‑rays from the day of the follow-up examination in anteroposterior, axillary, and lateral views were evaluated by one shoulder-trained examiner. Superior migration of the humerus was defined as a loss of the “gothic arch.” Anatomical reconstruction of the humerus was evaluated by comparing the deviation of the center of rotation (COR) and the radius of curvature (ROC) of the prosthetic humeral head from the native anatomy. Therefore, the best-fit circle technique and a coordinate system, as described by Youderian et al. [21], were used (Fig. 1). Radiolucent lines, subsidence, and bone loss around the nucleus were analyzed. For evaluation of radiolucent lines and bone loss, 18 zones around the nucleus in the anteroposterior and axillary x‑ray plane were defined (Fig. 2).
Deviation between the anatomical center of rotation (green circle with anatomical radius of curvature) and prosthetic center of rotation (red circle with prosthetic radius of curvature). Direction of deviation of center of rotation: SL superolateral, IL inferolateral, IM inferomedial, SM superomedial
Zones for evaluation of radiolucent lines and bone resorption under the nucleus. Black: in anteroposterior view from superior (1) to inferior (7). Blue: in axillary view from dorsal (8) to ventral (14). Zones S (superior), I (inferior) in anteroposterior view and zones D (dorsal), V (ventral) in axillary view are areas where there is no direct contact between prosthetic humeral head and humeral bone. Modified from [3], published with permission from Stryker
Statistical analysis
Statistical analyses were performed with SPSS 27 (IBM Corp., Ehningen, Germany). The level of significance was set at p < 0.05. Data were tested for normality of distribution using the Shapiro–Wilk test. The paired Student’s t test was used for comparison of the normal distribution of pre- and postoperative means and the Wilcoxon signed-rank test was used for data with non-normal distribution. Pearson correlation analysis was performed to determine correlations between two metric-scaled parameters.
Results
From April 2011 to December 2014, 110 Simpliciti prosthesis were implanted in 105 patients. During follow-up, four patients died, three patients were lost to follow-up, four patients had to be excluded from this study because of neurological illness, and one patient did not want to participate. Due to the COVID-19 pandemic in 2020, not all patients could be examined clinically, but the SSV and QDASH scores were collected from four patients in telephone interviews.
In total, follow-up of 89.1% of patients was achieved. Data from 98 (98/110) Simpliciti shoulder prostheses in 93 patients (38 men, 55 women) were evaluated for this study. Specifically, 10 HSA and 88 TSA were analyzed. The mean age at surgery was 66.7 years (32–83 years). At follow-up the mean age was 72.7 years (36–90 years). A mean follow-up of 71.5 months (49–106 months) was achieved. Patients with primary omarthrosis, posttraumatic omarthrosis, primary humeral head necrosis, secondary humeral head necrosis after fracture, omarthrosis in glenoid defect, and omarthrosis in glenoid dysplasia were included in the analysis.
Clinical and ultrasound results
Clinical results were collected for 94 shoulders. A mean active flexion of 141.4° ± 26.9° was achieved in the entire study group (HSA 132.3° ± 26.5°, TSA 142.3° ± 26.9°). The mean active abduction was 124.5° ± 30.1° (HSA 122.8° ± 25.6°, TSA 124.7° ± 30.7°) and active external rotation was possible on average up to 47.2° ± 13.4° (HSA 37.7° ± 16.8°, TSA 48.3° ± 12.6°).
A sonographic examination of the shoulder was performed on 95 shoulders and was normal without pathological findings in 79 shoulders (83.2%). A ruptured biceps tenodesis was visualized in two cases (2.1%), a partial rupture of one tendon of the RC was seen in 13 cases (13.7%; four subscapularis, seven supraspinatus, two infraspinatus), and a complete rupture of an RC tendon was detected in three cases (3.2%; two subscapularis, one supraspinatus).
Radiographic outcomes
Radiographs of 95 shoulders were evaluated in anteroposterior, axillary, and lateral views. Superior migration of the humerus, which was interpreted as a loss of the Gothic arch, was observed in 26 cases (27.4%).
None of the examined prostheses showed radiolucent lines around the nucleus or radiological signs of loosening. Bone resorption next to the nucleus occurred in 41 (41.8%) implanted prostheses. The outer edges (zones 1, 7, 8, and 14; Fig. 2) and the zones where the humeral head protrudes over the nucleus (zones S, I, D and V; Fig. 2) were mainly affected. Resorptions were found most frequently in zones S, I, D, and V (Fig. 3).
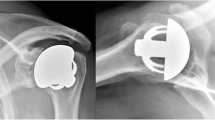
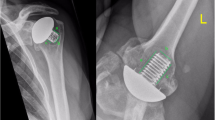
Typical bone resorption (12 months postoperatively) in the outer zones where the humeral head protrudes beyond the nucleus and no force transmission to the bone can be achieved: a in anteroposterior view, zones S, I; b in axillary view, zones V, D. Circles: typical bone resorption, Arrow: edge of the collar of the prosthesis
Three patients who were initially treated with HSA showed slight central glenoid wear, but the humeral head was still well centered. As all patients showed good clinical results and subjective satisfaction, no surgical treatment was required.
The difference between pre- and postoperative COR and between pre- and postoperative ROC could only be determined if exact pre- and postoperative true anteroposterior image were available. This was the case in 61 shoulders. The postoperative COR deviated from the preoperative COR by 3.7 mm ± 1.9 mm (range: 0.3–8.2 mm). Overall, 39.3% of the measured shoulders showed a deviation of less than 3 mm. The direction of deviation was superior–medial (SM) in one case, superior–lateral (SL) in one case, inferior–medial (IM) in four cases, and inferior–lateral (IL) in 55 cases. The postoperative ROC was on average 3.2 mm ± 1.3 mm larger than the preoperative ROC.
No significant correlation between the deviation in COR and ROC nor clinical scores from the study collective could be demonstrated (p > 0.05).
Scores
The SSV was collected from 98 shoulders and was 86.1% ± 16.0% in the entire collective (HSA 78.5% ± 17.7%, TSA 87.0% ± 15.3%), without significant differences between HSA and TSA (p = 0.112).
A valid QDASH score was obtained from 88 patients. The QDASH score averaged 11.7 ± 13.8 points in the entire collective (HSA 21.6 ± 15.6 points, TSA 10.4 ± 13.2 points). There was a significant difference in QDASH between the HAS and TSA groups (p = 0.015).
The CS was collected for 93 shoulders. The mean CS for the entire cohort was 75.4 ± 10.9 points (HSA 70.4 ± 10.4 points, TSA 76.0 ± 10.8 points), without a significant difference between the HSA and TSA groups (p = 0.221). Preoperative CS was available for 86 patients. A case-by-case comparison between preoperative and postoperative CS was carried out for 82 patients. In the entire study collective, the operation showed an average improvement of the CS of 43.8 ± 11.7 points from 32.2 ± 10.4 points preoperatively (p ≤ 0.05). In HSA, the CS increased by 42.1 ± 15.0 points from 28.3 ± 12.6 preoperatively (p ≤ 0.05), and in TSA, from 32.7 ± 10.1 by 44.1 ± 11.3 points (p ≤ 0.05).
The nCS was collected from 93 shoulders postoperatively. The overall nCS reached 89.7% ± 12.4% (HSA 82.1% ± 13.5%, TSA 90.7% ± 12.0%). A significant difference between HSA and TSA was determined (p = 0.039).
All collected scores are summarized in Table 1.
Complications
There were no intraoperative complications. No postoperative infections were detected, and no neurological complications related to the operation were observed.
One patient sustained a traumatic undisplaced fracture of the tuberculum majus 18 months postoperatively, which could be treated conservatively. Three patients developed a secondary frozen shoulder, which was treated with arthroscopic 360° arthrolysis. All three patients were symptom-free after arthrolysis. In one patient, a periprosthetic subcapital fracture of the humerus caused by a fall was treated with an angle-stable plate osteosynthesis around the prosthesis ex domo. Two patients had radiological signs of glenoid loosening. In one of these cases revision to a reverse shoulder prosthesis (RSA) was performed. At revision the Simpliciti prosthesis was still well fixed.
One patient treated with HSA suffered from glenoid wear and hereby irritation with a metal suture anchor placed in the glenoid before the prosthetic implantation occurred and a revision to RSA was performed. Three weeks after the implantation of the prosthesis, one patient had a serious fall downstairs due to an epileptic seizure with tearing of the entire greater tuberosity. At revision the Simpliciti was stable despite only the inferior half of the nucleus being within the humeral bone. Both of these patients were excluded from the study because no data on the original Simpliciti could be collected.
The complication rate in the collective was 7.1% (7/98). The revision rate was 5.1% (5/98) including three arthroscopic releases, one osteosynthesis of a periprosthetic fracture, and one conversion to RSA. There was not a single case of revision due to loosening of the Simpliciti prosthesis.
Discussion
Stemless shoulder prostheses have been available since the early 2000s but mid- and long-term results are still scarce [18]. Beck et al. [1] showed good clinical and radiographic results for the stemless TESS (Biomet, Warsaw, IN, USA) with a follow-up of 94.7 months and an average CS of 68.8 points. Currently the Eclipse (Arthrex, Naples, FL, USA) prosthesis is the stemless shoulder prosthesis with the longest evaluated follow-up of 108 months; with an average CS of 62 points, good clinical and functional results were achieved [7]. For the Simpliciti shoulder system, Churchill et al. [3] demonstrated good short-term results with a 2-year follow-up. The CS improved from 44.3 to 80.7 points and a gain in the nCS from 55% to 104% was achieved. Collin et al. [4] showed good results for the Simpliciti with a mean follow-up of 35 months. The current study is the first to report mid-term results for the Simpliciti shoulder system.
It is under debate whether TSA or HSA provides more reliable outcomes. In our study, TSA achieved statistically significantly better postoperative results only in QDASH and nCS compared to HSA, but in no other measured parameter. This could be because the HSA group, with an average age of 63.7 years, consisted of younger patients than the TSA group, with an average age of 73.7 years. Furthermore, the gender distribution in the HSA group was a balanced gender ratio between women and men, whereas there were 54 women and 34 men in the TSA group. Both age and sex have a great influence on the nCS, because the mean CS is significantly higher in male patients than in female patients, and the nCS is also significantly different in each age group [15]. Therefore, it is easier to achieve a high nCS for older, female patients.
In the observation period, no lysis around the nucleus or displacement of the Simpliciti was detected on the X‑ray images and the prosthesis showed good bony ingrowth. There was no loosening of the implant in any patient.
Bone resorption occurred in the marginal areas of the prosthesis, where the humeral head protrudes over the nucleus and no direct contact or force transmission between the prosthesis head and the bone exists (areas S, I, V, D; Figs. 2 and 3). According to Wolff’s law [20], the missing load transmission leads to bone resorption. All bone resorptions detected were without clinical relevance and all Simpliciti prostheses were firmly anchored in the humeral bone. Similar findings were reported by Churchill et al. [3]. They also reported on bone resorption around the humeral medial calcar up to the neck of the nucleus in about 50% of their patients without any signs of prosthetic loosening or clinical relevance.
In our study, a mean deviation of the postoperative COR from the preoperative COR of 3.7 mm ± 1.9 mm was determined. Overall, 39.3% of the measured shoulders showed a deviation of less than 3 mm. The postoperative ROC, which is determined by the prosthesis design, differed by 3.1 mm ± 1.3 mm from the preoperative anatomical ROC. No significant correlation was determined between the deviation in the COR and the ROC with the collected scores. Gallacher et al. [5] reported a deviation in the postoperative COR of less than 3 mm in 76% of cases with the Eclipse, whereas Kadum et al. [8] reported a deviation of less than 3 mm in 82% of the cases using the stemless TESS. A possible explanation for the fact that the reconstruction with a deviation in the COR of less than 3 mm was only achieved in 39.3% of the cases in our study may be found in the prosthesis design of the Simpliciti. When choosing the humeral head component, surgeons orient themselves at the resected bony humeral head and the resection level. When implanting the prosthesis head, care is taken to ensure that the prosthesis does not protrude beyond the resection level and is flush with the metaphyseal bone. The Simpliciti humeral head has rounded edges (Fig. 4a). The surgeon uses this edge to check the size of the prosthesis. Due to the rounded edges, the actual measured diameter of the prosthesis head does not correspond to the printed prosthesis size (Fig. 4b). The printed prosthesis size results from the curvature of the surface of the prosthesis and is achieved when the curvature of the prosthesis surface is continued and intersects the undersurface of the prosthesis with a sharp edge (Fig. 4c). The postoperative measurements of the COR and the ROC on the X‑ray image were carried out similar to Fig. 4c by a best-fitting circle that runs through three points on the prosthesis surface and thus corresponds to the completion of the surface curvature. Due to the rounded edges of the Simpliciti, which intraoperatively merge flush into the humeral bone, an apparently too large ROC is measured on the postoperative X‑ray image. The Eclipse and the TESS do not have rounded edges like the Simpliciti. Here, the printed diameter corresponds to the measured diameter. It is therefore questionable whether this method of measuring the COR and the ROC is equally suitable for the Simpliciti as for the TESS or Eclipse prosthesis.
No intraoperative complications occurred in the present study. Three patients developed secondary shoulder stiffness, which is a rather rare complication of shoulder prostheses. In the affected patients, all implant- and patient-specific factors were excluded and an arthroscopic 360° arthrolysis was performed. It can be assumed that in these cases that the scarring found in the sliding layers was the cause of the stiffness, since none of the patients reported any complaints in the subsequent course, which is also consistent with the results reported by Thorsness et al. [16].
In two of the prostheses examined (2/98), a periprosthetic fracture occurred postoperatively as a result of a fall. One of these fractures could be treated conservatively; in the second, osteosynthesis was performed using an angle-stable plate. Primary implant removal was not necessary in any case. Incidence rates of 1.6–2.8% for postoperative periprosthetic humeral fractures are reported in the literature [12]. Thus, our incidence of 2.0% is within the range described in the literature. Periprosthetic humeral fractures represent a major surgical challenge. The design of the Simpliciti offers more space for the insertion of osteosynthesis material during osteosynthesis and in the event of a fracture with prosthesis loosening, the small implant enables revisions using a stemmed implant.
Radiological signs of loosening of the cemented glenoid were detected in two patients. One of the patients was lost to follow-up. The second patient underwent revision surgery due to glenoid loosening. The Simpliciti was found to be firmly anchored intraoperatively and well integrated with the humeral bone. The metaphyseal anchorage of the Simpliciti and the minimal loss of bone substance during explantation enabled implantation of a standard cemented RSA. Cancellous bone from the metaphysis and cancellous bone that had grown into the nucleus could be used to fill the glenoid defect, eliminating the need for cancellous bone harvest from the iliac crest or the use of allogeneic bone material.
The complication rate of 7.1% (7/98) and the revision rate of 5.1% (5/98) observed here correspond to those reported in the literature for stemless shoulder prostheses [10, 18, 19].
Wiater et al. [17] demonstrated no significant functional or clinical difference between stemmed and stemless shoulder prostheses in their prospective, blinded, randomized controlled trial. So do several current meta-analyses [11, 13, 14]. These data are also in line with the data collected in our study, showing the Simpliciti shoulder system to perform as well as stemmed prostheses at mid-term follow-up.
Limitations
The study has some limitations. It was a single-center, retrospective study and there was no control group. Preoperative CS and nCS were only available for 88.2% (82/93) of the patients examined. The SSV and QDASH were only recorded postoperatively for all patients. However, in the 82 patients for whom preoperative score values (CS, nCS) existed, a significant increase in the score values was observed. Due to the study design, statements can only be made about the evaluated observation period.
Practical conclusion
-
In the mid-term follow-up of 4–8 years (71.5 ± 13.1 months) in the current study, the stemless Simpliciti shoulder prosthesis showed good to very good clinical and radiographic results, which correspond to those of shaft-guided shoulder prostheses.
-
The complication rate of stemless shoulder prostheses is low and shaft-associated complications can be avoided.
-
Bone resorption of unloaded bone of the humeral head was frequent but without any clinical impact.
-
The stemless Simpliciti shoulder prosthesis is a reliable therapeutic option for the prosthetic treatment of the shoulder joint, especially in young patients. Long-term results are still pending and must be the subject of further investigations.
References
Beck S, Beck V, Wegner A et al (2018) Long-term survivorship of stemless anatomical shoulder replacement. Int Orthop 42:1327–1330
Churchill RS (2020) Comparison of intraoperative bone quality and bone quantity with 2‑year radiographic results of the simpliciti stemless total shoulder arthroplasty system. J Shoulder Elbow Surg 29:e166–e167
Churchill RS, Chuinard C, Wiater JM et al (2016) Clinical and radiographic outcomes of the simpliciti canal-sparing shoulder arthroplasty system: a prospective two-year multicenter study. J Bone Joint Surg Am 98:552–560
Collin P, Matsukawa T, Boileau P et al (2017) Is the humeral stem useful in anatomic total shoulder arthroplasty? Int Orthop 41:1035–1039
Gallacher S, Williams HLM, King A et al (2018) Clinical and radiologic outcomes following total shoulder arthroplasty using arthrex eclipse stemless humeral component with minimum 2 years’ follow-up. J Shoulder Elbow Surg 27:2191–2197
Habermeyer P, Lichtenberg S, Tauber M et al (2015) Midterm results of stemless shoulder arthroplasty: a prospective study. J Shoulder Elbow Surg 24:1463–1472
Hawi N, Magosch P, Tauber M et al (2017) Nine-year outcome after anatomic stemless shoulder prosthesis: clinical and radiologic results. J Shoulder Elbow Surg 26:1609–1615
Kadum B, Hassany H, Wadsten M et al (2016) Geometrical analysis of stemless shoulder arthroplasty: a radiological study of seventy TESS total shoulder prostheses. Int Orthop 40:751–758
Kircher J, Ohly B, Albers S et al (2022) Versorgungsrealität in Deutschland: ein Auszug aus dem Schulterendoprothesenregister der Deutschen Vereinigung für Schulter- und Ellenbogenchirurgie e. V. (DVSE). Obere Extrem 17:92–98
Liu EY, Kord D, Horner NS et al (2020) Stemless anatomic total shoulder arthroplasty: a systematic review and meta-analysis. J Shoulder Elbow Surg 29:1928–1937
Looney AM, Day J, Johnson JL et al (2022) Outcomes between stemmed and stemless total shoulder arthroplasty: a systematic review and meta-analysis of randomized controlled trials. J Am Acad Orthop Surg 6:
Novi M, Porcellini G, Dona A et al (2021) A long-term follow-up of post-operative periprosthetic humeral fracture in shoulder arthroplasty. Geriatr Orthop Surg Rehabil 12:21514593211039908
Peng W, Ou Y, Wang C et al (2019) The short- to midterm effectiveness of stemless prostheses compared to stemmed prostheses for patients who underwent total shoulder arthroplasty: a meta-analysis. J Orthop Surg Res 14:469
Shin YS, Lee WS, Won JS (2021) Comparison of stemless and conventional stemmed shoulder arthroplasties in shoulder arthropathy: a meta-analysis. Medicine 100:e23989
Tavakkolizadeh A, Ghassemi A, Colegate-Stone T et al (2009) Gender-specific constant score correction for age. Knee Surg Sports Traumatol Arthrosc 17:529–533
Thorsness RJ, Romeo AA (2016) Stiffness following shoulder arthroplasty: To manipulate or not. Semin Arthroplasty 27:104–107
Wiater JM, Levy JC, Wright SA et al (2020) Prospective, blinded, randomized controlled trial of stemless versus stemmed humeral components in anatomic total shoulder Arthroplasty: results at short-term follow-up. J Bone Joint Surg Am 102:1974–1984
Willems JIP, Hoffmann J, Sierevelt IN et al (2021) Results of stemless shoulder arthroplasty: a systematic review and meta-analysis. EFORT Open Rev 6:35–49
Wodarek J, Shields E (2021) Stemless total shoulder: a review of biomechanical fixation and recent results. J Shoulder Elb Arthroplast 5:24715492211008408
Wolf JH (1995) Julis Wolff and his “law of bone remodeling”. Orthopade 24:378–386
Youderian AR, Ricchetti ET, Drews M et al (2014) Determination of humeral head size in anatomic shoulder replacement for glenohumeral osteoarthritis. J Shoulder Elbow Surg 23:955–963
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
K. List is a consultant for the companies Arthrex and Stryker. B. Barth, J. Schmalzl, D. Böhm and D. Böhm declare that they have no competing interests.
All human studies described were conducted with the approval of the responsible ethics committee, in accordance with national law and the Declaration of Helsinki of 1975 (in the current, revised version). The study was approved by the Ethics Committee of the Julius-Maximilians-Universität Würzburg (processing number AZ-319/17). Informed consent was obtained from all participating patients.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.

Scan QR code & read article online
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Barth, B., Schmalzl, J., List, K. et al. Mid-term results (4–8 years) with the stemless Simpliciti shoulder system. Obere Extremität 19, 34–40 (2024). https://doi.org/10.1007/s11678-024-00785-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11678-024-00785-9