Abstract
Background
Laparoscopic transcystic common bile duct exploration (LTCBDE) is used to treat cholecystolithiasis and choledocholithiasis. This study aimed to investigate the safety, effectiveness and generalisability of LTCBDE in patients with cholecystolithiasis and choledocholithiasis based on our LTCBDE experience within 8 years.
Methods
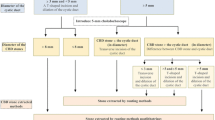
Four hundred patients with cholecystolithiasis and choledocholithiasis (including 62 of cholecystolithiasis and choledocholithiasis with common bile duct no-dilatation) treated with LTCBDE at a single centre from January 2014 to February 2022 were retrospectively evaluated. They were divided into the first 200 and last 200 LTCBDE cases. The disease characteristics, cystic duct incision methods, surgical outcomes and follow-up data were analysed retrospectively. Each patient was followed up for > 3 months.
Results
Four hundred patients underwent LTCBDE, including 188 males and 212 females aged from 15 to 91 years (average age: 56 years). LTCBDE was successful in 377 (94.3%) patients, while treatment was converted to laparoscopic choledocholithotomy with T-tube drainage in 23 (5.8%), owing to intraoperative choledochoscope insertion failure. The CBD diameter (10.89 ± 1.76 vs 9.97 ± 2.39, P < 0.05), cystic duct diameter (4.62 ± 1.03 vs 5.03 ± 1.29, P < 0.05), and operation time (164.60 ± 24.30 vs 135.34 ± 30.00, P < 0.05). Residual stones were found in six (1.5%) patients and removed during the second operation; post-operative bile leakage was found in one (0.3%) patient, who was discharged safely after the second operation.
Conclusions
Phase I LTCBDE is safe and effective in treating cholecystolithiasis and choledocholithiasis. With continuous technological advances, LTCBDE has been effectively promoted and applied.


Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author, [Lu Fang], upon reasonable request.
References
1 Tazuma S. Gallstone disease: Epidemiology, pathogenesis, and classification of biliary stones (common bile duct and intrahepatic). Best practice & research Clinical gastroenterology 2006;20(6):1075-1083.
2 Zhang W, Wang BY, Du XY, Fang WW, Wu H, Wang L, Zhuge YZ, Zou XP. Big-data analysis: A clinical pathway on endoscopic retrograde cholangiopancreatography for common bile duct stones. World journal of gastroenterology 2019;25(8):1002-1011.
3 Portincasa P, Di Ciaula A, de Bari O, Garruti G, Palmieri VO, Wang DQ. Management of gallstones and its related complications. Expert review of gastroenterology & hepatology 2016;10(1):93-112.
4 Elmunzer BJ, Noureldin M, Morgan KA, Adams DB, Coté GA, Waljee AK. The Impact of Cholecystectomy After Endoscopic Sphincterotomy for Complicated Gallstone Disease. The American journal of gastroenterology 2017;112(10):1596-1602.
5 Boerma D, Schwartz MP. Gallstone disease. Management of common bile-duct stones and associated gallbladder stones: Surgical aspects. Best practice & research Clinical gastroenterology 2006;20(6):1103-1116.
6 Williams EJ, Green J, Beckingham I, Parks R, Martin D, Lombard M. Guidelines on the management of common bile duct stones (CBDS). Gut 2008;57(7):1004-1021.
7 Khaled YS, Malde DJ, de Souza C, Kalia A, Ammori BJ. Laparoscopic bile duct exploration via choledochotomy followed by primary duct closure is feasible and safe for the treatment of choledocholithiasis. Surgical endoscopy 2013;27(11):4164-4170.
8 Aawsaj Y, Light D, Horgan L. Laparoscopic common bile duct exploration: 15-year experience in a district general hospital. Surgical endoscopy 2016;30(6):2563-2566.
9 Lyass S, Phillips EH. Laparoscopic transcystic duct common bile duct exploration. Surgical endoscopy 2006;20 Suppl 2:S441-445.
10 van Dijk AH, Lamberts M, van Laarhoven CJ, Drenth JP, Boermeester MA, de Reuver PR. Laparoscopy in cholecysto-choledocholithiasis. Best practice & research Clinical gastroenterology 2014;28(1):195-209.
11 Lacitignola S, Minardi M. Management of common bile duct stones: a ten-year experience at a tertiary care center. JSLS : Journal of the Society of Laparoendoscopic Surgeons 2008;12(1):62-65.
12 Petelin JB. Laparoscopic common bile duct exploration. Surgical endoscopy 2003;17(11):1705-1715.
13 Loperfido S, Angelini G, Benedetti G, Chilovi F, Costan F, De Berardinis F, De Bernardin M, Ederle A, Fina P, Fratton A. Major early complications from diagnostic and therapeutic ERCP: a prospective multicenter study. Gastrointestinal endoscopy 1998;48(1):1-10.
14 Wang P, Li ZS, Liu F, Ren X, Lu NH, Fan ZN, Huang Q, Zhang X, He LP, Sun WS, Zhao Q, Shi RH, Tian ZB, Li YQ, Li W, Zhi FC. Risk factors for ERCP-related complications: a prospective multicenter study. The American journal of gastroenterology 2009;104(1):31-40.
15 Ahmed I, Pradhan C, Beckingham IJ, Brooks AJ, Rowlands BJ, Lobo DN. Is a T-tube necessary after common bile duct exploration? World journal of surgery 2008;32(7):1485-1488.
16 Wu X, Yang Y, Dong P, Gu J, Lu J, Li M, Mu J, Wu W, Yang J, Zhang L, Ding Q, Liu Y. Primary closure versus T-tube drainage in laparoscopic common bile duct exploration: a meta-analysis of randomized clinical trials. Langenbeck's archives of surgery 2012;397(6):909-916.
17 Yin Z, Xu K, Sun J, Zhang J, Xiao Z, Wang J, Niu H, Zhao Q, Lin S, Li Y. Is the end of the T-tube drainage era in laparoscopic choledochotomy for common bile duct stones is coming? A systematic review and meta-analysis. Annals of surgery 2013;257(1):54-66.
18 Estellés Vidagany N, Domingo Del Pozo C, Peris Tomás N, Díez Ares J, Vázquez Tarragón A, Blanes Masson F. Eleven years of primary closure of common bile duct after choledochotomy for choledocholithiasis. Surgical endoscopy 2016;30(5):1975-1982.
19 Shapiro SJ, Gordon LA, Daykhovsky L, Grundfest W. Laparoscopic exploration of the common bile duct: experience in 16 selected patients. Journal of laparoendoscopic surgery 1991;1(6):333-341.
20 Fang L, Wang J, Dai WC, Liang B, Chen HM, Fu XW, Zheng BB, Lei J, Huang CW, Zou SB. Laparoscopic transcystic common bile duct exploration: surgical indications and procedure strategies. Surgical endoscopy 2018;32(12):4742-4748.
21 Fang L, Huang J, Zheng H, Duan ZQ, Liu TD, Xiong H, Li W, Fu XW, Gao JF, Le H, Hu W, Liang B, Zhu XG. Laparoscopic transcystic common bile duct exploration in patients with a nondilated common bile duct. Annals of palliative medicine 2021;10(12):12845-12856.
Phillips EH, Rosenthal RJ, Carroll BJ, Fallas MJ. Laparoscopic trans-cystic-duct common-bile-duct exploration. Surgical endoscopy 1994;8(12):1389–1393; discussion 1393–1384.
23 Zhu HY, Xu M, Shen HJ, Yang C, Li F, Li KW, Shi WJ, Ji F. A meta-analysis of single-stage versus two-stage management for concomitant gallstones and common bile duct stones. Clinics and research in hepatology and gastroenterology 2015;39(5):584-593.
24 Zhao ZH, Hu LH, Ren HB, Zhao AJ, Qian YY, Sun XT, Su S, Zhu SG, Yu J, Zou WB, Guo XR, Wang L, Li ZS, Liao Z. Incidence and risk factors for post-ERCP pancreatitis in chronic pancreatitis. Gastrointestinal endoscopy 2017;86(3):519-524.e511.
25 Lyu Y, Cheng Y, Wang B, Xu Y, Du W. What is impact of nonsteroidal anti-inflammatory drugs in the prevention of post-endoscopic retrograde cholangiopancreatography pancreatitis: a meta-analysis of randomized controlled trials. BMC gastroenterology 2018;18(1):106.
26 Vezakis A, Fragulidis G, Polydorou A. Endoscopic retrograde cholangiopancreatography-related perforations: Diagnosis and management. World journal of gastrointestinal endoscopy 2015;7(14):1135-1141.
27 Czerwonko ME, Pekolj J, Uad P, Mazza O, Sanchez-Claria R, Arbues G, de Santibañes E, de Santibañes M, Palavecino M. Laparoscopic Transcystic Common Bile Duct Exploration in the Emergency Is as Effective and Safe as in Elective Setting. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract 2019;23(9):1848-1855.
28 Feng Q, Huang Y, Wang K, Yuan R, Xiong X, Wu L. Laparoscopic Transcystic Common Bile Duct Exploration: Advantages over Laparoscopic Choledochotomy. PloS one 2016;11(9):e0162885.
29 Manes G, Paspatis G, Aabakken L, Anderloni A, Arvanitakis M, Ah-Soune P, Barthet M, Domagk D, Dumonceau JM, Gigot JF, Hritz I, Karamanolis G, Laghi A, Mariani A, Paraskeva K, Pohl J, Ponchon T, Swahn F, Ter Steege RWF, Tringali A, Vezakis A, Williams EJ, van Hooft JE. Endoscopic management of common bile duct stones: European Society of Gastrointestinal Endoscopy (ESGE) guideline. Endoscopy 2019;51(5):472-491.
30 Poulose BK, Arbogast PG, Holzman MD. National analysis of in-hospital resource utilization in choledocholithiasis management using propensity scores. Surgical endoscopy 2006;20(2):186-190.
31 Lei J, Wang J, Li Q, Wu P, Yuan R, Zhu H, Zou S, Shao J, Fang L. Laparoscopic Transcystic Common Bile Duct Exploration: T-Shaped Incision of Cystic Duct with FREDDY Laser Lithotripsy. Journal of laparoendoscopic & advanced surgical techniques Part A 2016;26(8):646-651.
Acknowledgements
We would like to thank the contributions of all of the patients in our retrospective study.
Funding
This work was supported by the National Natural Science Foundation of China (Grant No. 82160578); the Natural Science Foundation of Jiangxi Province (Grant Nos. 20212BCJ23024, 20202BAB216029, and 20202BABL206095); the Health Department of Jiangxi Province (Grant Nos. 20198020, 202210033); and the Education Department of Jiangxi Province (Grant No. GJJ190019).
Author information
Authors and Affiliations
Contributions
Conception and design of the manuscript: Bo Liang, Lu Fang, and Jian Huang. Acquisition of data: Yuting Fan, Liangzhi Xu, Jinghang Liu, Xinguo Tang, and Wei Hu. Analysis and interpretation of data: Lu Fang, Jian Huang, Tiande Liu, Hu Xiong, Wen Li, and Xiaowei Fu. Drafting of the manuscript: all the authors. Critical revision of the final version to be published: all the authors. Approval of the final version to be published: all the authors.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huang, J., Hu, W., Liu, J. et al. Laparoscopic Transcystic Common Bile Duct Exploration: 8-Year Experience at a Single Institution. J Gastrointest Surg 27, 555–564 (2023). https://doi.org/10.1007/s11605-023-05594-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-023-05594-z