Abstract
Background
Marginal ulcer (MU) is a well-described complication of pancreatoduodenectomy (PD) whose incidence remains unclear. Gastric antisecretory medications likely attenuate the risk of marginal ulceration after PD; however, the true relationship between antisecretory medication and marginal ulceration after PD is not precisely known. The aims of this study were to document the incidence of MU after PD, identify any relationship between MU and gastric antisecretory medication, and survey current practice of MU prophylaxis among experienced pancreatic surgeons.
Methods
the MEDLINE, EMBASE, Cochrane Central Registrar of Controlled Trials, and Cochrane Database of Systematic Reviews databases were searched from their inception to May 2014 for abstracts documenting ulceration after pancreatoduodenectomy. Two reviewers independently graded abstracts for inclusion in this review. Contemporary practice was assessed through a four-question survey distributed globally to 200 established pancreatic surgeons.
Results
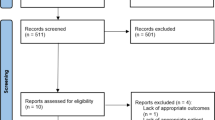
After a review of 208 abstracts, 54 studies were graded as relevant. These represented a cohort of 212 patients with marginal ulcer after PD (n = 4794). A meta-analysis of the included references shows mean incidence of ulceration after PD of 2.5 % (confidence interval (CI) 1.8–3.2 %) with a median time to diagnosis of 15.5 months. Pylorus preservation was associated with a MU rate of 2.0 % (CI 1.0–2.9 %), while “classic” PD procedures report an overall rate of 2.6 % (CI 1.6–3.6 %). Documented use of postoperative antisecretory medication was associated with a reduced rate of 1.4 % (CI 0.1–1.7 %). One hundred forty-four of 200 (72 %) surveys were returned, from which it was determined that 92 % of pancreatic surgeons have dealt with this complication, and 86 % routinely prescribe prophylactic antisecretory medication after PD.
Conclusions
The incidence of MU after PD is 2.5 % with a median time to occurrence of 15.5 months postoperatively. Gastric antisecretory medication prescription may affect the incidence of MU. The majority of pancreatic surgeons surveyed have encountered MU after PD; most (86 %) routinely prescribe prophylactic gastric antisecretory medication.







Similar content being viewed by others
References
Dragstedt, L.R., Some Physiologic Principles Involved in Surgical Treatment of Gastric and Duodenal Ulcer Ann. Surg, 1935. 102: p. 563-580
Owens, F., The Problem of Peptic Ulcer Following Pancreatic. Annals of Surgery, 1948. 128(1): p. 15-20.
DerSimonian, R., Combining evidence from clinical trials. Anesth Analg., 1990. 70: p. 475-6.
Abdel-Wahab, M., et al., Modified pancreaticoduodenectomy: experience with 81 cases, Wahab modification. Hepatogastroenterology, 2001. 48(42): p. 1572-6.
Bassi, C., et al., Open pancreaticogastrostomy after pancreaticoduodenectomy: a pilot study. J Gastrointest Surg, 2006. 10(7): p. 1072-80.
Basso, N., et al., Retained antral mucosa in pancreaticoduodenectomy patients. Am J Surg, 1977. 134(2): p. 259-62.
Braasch, J.W., et al., Pyloric and gastric preserving pancreatic resection. Experience with 87 patients. Ann Surg, 1986. 204(4): p. 411-8.
Cameron, J.L., et al., One hundred and forty-five consecutive pancreaticoduodenectomies without mortality. Ann Surg, 1993. 217(5): p. 430-5; discussion 435-8.
Caronna, R., et al., Functional results of a personal technique of reconstruction after pancreaticoduodenectomy. J Exp Clin Cancer Res, 2003. 22(4 Suppl): p. 187-9.
De Bernardinis, G., et al., An original reconstructive method after pylorus-preserving pancreatoduodenectomy. Surg Today, 1993. 23(6): p. 481-5.
Fink, A.S., et al., Long-term evaluation of pylorus preservation during pancreaticoduodenectomy. World J Surg, 1988. 12(5): p. 663-70.
Flautner, L., T. Tihanyi, and A. Szecseny, Pancreatogastrostomy: an ideal complement to pancreatic head resection with preservation of the pylorus in the treatment of chronic pancreatitis. Am J Surg, 1985. 150(5): p. 608-11.
Grant, C.S. and J.A. Van Heerden, Anastomotic ulceration following subtotal and total pancreatectomy. Ann Surg, 1979. 190(1): p. 1-5.
Hayashibe, A. and M. Kameyama, The clinical results of duct-to-mucosa pancreaticojejunostomy after pancreaticoduodenectomy in consecutive 55 cases. Pancreas, 2007. 35(3): p. 273-5.
Herter, F.P., et al., Surgical experience with pancreatic and periampullary cancer. Ann Surg, 1982. 195(3): p. 274-81.
Hishinuma, S., et al., Complications after pylorus-preserving pancreatoduodenectomy with gastrointestinal reconstruction by the Imanaga method. J Am Coll Surg, 1998. 186(1): p. 10-6.
Holbrook, R.F., K. Hargrave, and L.W. Traverso, A prospective cost analysis of pancreatoduodenectomy. Am J Surg, 1996. 171(5): p. 508-11.
Hoshal, V.L., Jr., et al., Personal experience with the Whipple operation: outcomes and lessons learned. Am Surg, 2004. 70(2): p. 121-5; discussion 126.
Itani, K.M., et al., Pylorus-preserving pancreatoduodenectomy. A clinical and physiologic appraisal. Ann Surg, 1986. 204(6): p. 655-64.
Jimenez, R.E., et al., Outcome of pancreaticoduodenectomy with pylorus preservation or with antrectomy in the treatment of chronic pancreatitis. Ann Surg, 2000. 231(3): p. 293-300.
Kim, H.C., et al., Exocrine and endocrine stomach after gastrobulbar preserving pancreatoduodenectomy. Ann Surg, 1987. 206(6): p. 717-27.
Kim, K.H., et al., Effect of a single layer continuous suture between pancreatic parenchyma and jejunum after duct-to-mucosa anastomosis in pancreaticoduodenectomy: a single surgeon's experiences. Hepatogastroenterology, 2007. 54(77): p. 1368-72.
Kingsnorth, A.N., J.D. Berg, and M.R. Gray, A novel reconstructive technique for pylorus-preserving pancreaticoduodenectomy: avoidance of early postoperative gastric stasis. Ann R Coll Surg Engl, 1993. 75(1): p. 38-42.
Klinkenbijl, J.H., et al., The advantages of pylorus-preserving pancreatoduodenectomy in malignant disease of the pancreas and periampullary region. Ann Surg, 1992. 216(2): p. 142-5.
Kozuschek, W., et al., A comparison of long term results of the standard Whipple procedure and the pylorus preserving pancreatoduodenectomy. J Am Coll Surg, 1994. 178(5): p. 443-53.
Lerut, J., et al., Pylorus-preserving pancreatoduodenectomy. Experience in 20 patients. HPB Surg, 1991. 4(2): p. 109-17; discussion 117-9.
Lupo, L.G., et al., Is pyloric function preserved in pylorus-preserving pancreaticoduodenectomy? Eur J Surg, 1998. 164(2): p. 127-32.
Lygidakis, N.J., et al., Reappraisal of a method of reconstruction after pancreatoduodenectomy. Hepatogastroenterology, 2005. 52(64): p. 1077-82.
Ma, Y.G., et al., Pancreaticoduodenectomy with Roux-Y anastomosis in reconstructing the digestive tract: report of 26 patients. Hepatobiliary Pancreat Dis Int, 2002. 1(4): p. 611-3.
Matsuno, S., et al., Pancreatic function and rehabilitation after pancreaticoduodenectomy. Jpn J Surg, 1988. 18(1): p. 23-30.
McAfee, M.K., J.A. van Heerden, and M.A. Adson, Is proximal pancreatoduodenectomy with pyloric preservation superior to total pancreatectomy? Surgery, 1989. 105(3): p. 347-51.
Miedema, B.W., et al., Complications following pancreaticoduodenectomy. Current management. Arch Surg, 1992. 127(8): p. 945-9; discussion 949-50.
Mosca, F., et al., Pancreaticoduodenectomy with pylorus preservation. Ital J Surg Sci, 1984. 14(4): p. 313-20.
Newman, K.D., et al., Pyloric and gastric preservation with pancreatoduodenectomy. Am J Surg, 1983. 145(1): p. 152-6.
Nishikawa, M., et al., Gastric pH monitoring after pylorus preserving pancreaticoduodenectomy with Billroth I type of reconstruction. J Am Coll Surg, 1994. 179(2): p. 129-34.
Ohtsuka, T., et al., Postoperative pancreatic exocrine function influences body weight maintenance after pylorus-preserving pancreatoduodenectomy. Am J Surg, 2001. 182(5): p. 524-9.
Oida, T., et al., Gastric marginal ulcer after pancreaticoduodenectomy with pancreaticogastrostomy due to delayed gastric emptying and Helicobacter pylori infection. Hepatogastroenterology, 2012. 59(115): p. 899-902.
Pannala, R., et al., Afferent limb syndrome and delayed GI problems after pancreaticoduodenectomy for pancreatic cancer: single-center, 14-year experience. Gastrointest Endosc, 2011. 74(2): p. 295-302.
Patel, A.G., et al., Pylorus-preserving Whipple resection for pancreatic cancer. Is it any better? Arch Surg, 1995. 130(8): p. 838-42; discussion 842-3.
Pellegrini, C.A., et al., An analysis of the reduced morbidity and mortality rates after pancreaticoduodenectomy. Arch Surg, 1989. 124(7): p. 778-81.
Porter, M.R., Carcinoma of the pancreatico-duodenal area; operability and choice of procedure. Ann Surg, 1958. 148(4): p. 711-23; discussion 723-4.
Riediger, H., et al., Long-term outcome after resection for chronic pancreatitis in 224 patients. J Gastrointest Surg, 2007. 11(8): p. 949-59; discussion 959-60.
Roder, J.D., et al., Pylorus-preserving versus standard pancreatico-duodenectomy: an analysis of 110 pancreatic and periampullary carcinomas. Br J Surg, 1992. 79(2): p. 152-5.
Ruilova, L.A. and C.D. Hershey, Experience with 21 pancreaticoduodenectomies. Arch Surg, 1976. 111(1): p. 27-30.
Safioleas, M.C., et al., How necessary is vagotomy after pancreaticoduodenectomy and total pancreatectomy. Hepatogastroenterology, 2005. 52(61): p. 251-2.
Sakaguchi, T., et al., Marginal ulceration after pylorus-preserving pancreaticoduodenectomy. J Hepatobiliary Pancreat Surg, 2000. 7(2): p. 193-7.
Sakorafas, G.H., et al., Long-term results after surgery for chronic pancreatitis. Int J Pancreatol, 2000. 27(2): p. 131-42.
Schmidt, U., et al., Quality of life and functional long-term outcome after partial pancreatoduodenectomy: pancreatogastrostomy versus pancreatojejunostomy. Ann Surg Oncol, 2005. 12(6): p. 467-72.
Scott, H.W., Jr., et al., The role of vagotomy in pancreaticoduodenectomy. Ann Surg, 1980. 191(6): p. 688-96.
Shan, Y.S., et al., Reconsideration of delayed gastric emptying in pancreaticoduodenectomy. World J Surg, 2005. 29(7): p. 873-9; discussion 880.
Shinchi, H., et al., Gastric acidity following pancreaticogastrostomy with pylorus-preserving pancreaticoduodenectomy. World J Surg, 2000. 24(1): p. 86-90; discussion 90-1.
Shyr, Y.M., et al., Non-stented pancreaticogastrostomy after pylorus-preserving pancreaticoduodenectomy. Zhonghua Yi Xue Za Zhi (Taipei), 2002. 65(6): p. 254-9.
Tanaka, T., Y. Matsugu, and Y. Fukuda, Use of ultrasonically activated shears improves the safety of pancreaticojejunostomy after pancreaticoduodenectomy. Arch Surg, 2002. 137(11): p. 1258-61.
Traverso, L.W. and R.A. Kozarek, Pancreatoduodenectomy for chronic pancreatitis: anatomic selection criteria and subsequent long-term outcome analysis. Ann Surg, 1997. 226(4): p. 429-35; discussion 435-8.
Walsh, D.B., et al., Adenocarcinoma of the ampulla of Vater. Diagnosis and treatment. Ann Surg, 1982. 195(2): p. 152-7.
Wu, J.M., et al., Reflux esophagitis and marginal ulcer after pancreaticoduodenectomy. J Gastrointest Surg, 2011. 15(5): p. 824-8.
Yamaguchi, K., et al., ERT following IORT improves survival of patients with resectable pancreatic cancer. Hepatogastroenterology, 2005. 52(64): p. 1244-9.
Elliott, D.W., Effect of lost pancreatic juice on gastric acid and peptic ulcer. Am J Surg, 1974. 127(6): p. 658-62.
Grace, P.A., et al., Decreased morbidity and mortality after pancreatoduodenectomy. Am J Surg, 1986. 151(1): p. 141-9.
Crist, D.W., J.V. Sitzmann, and J.L. Cameron, Improved hospital morbidity, mortality, and survival after the Whipple procedure. Ann Surg, 1987. 206(3): p. 358-65.
Traverso, L.W. and W.P. Longmire, Jr., Preservation of the pylorus in pancreaticoduodenectomy a follow-up evaluation. Ann Surg, 1980. 192(3): p. 306-10.
Traverso, L.W. and W.P. Longmire, Jr., Preservation of the pylorus in pancreaticoduodenectomy. Surg Gynecol Obstet, 1978. 146(6): p. 959-62.
K, W., Carcinoma of the ampula of Vater: sucessful radical resection. Br J Surg, 1944. 31: p. 368-373.
Pearlman, N.W., et al., Acid and gastrin levels following pyloric-preserving pancreaticoduodenectomy. Arch Surg, 1986. 121(6): p. 661-4.
Sudo, T., et al., Changes in plasma gastrin and secretin levels after pancreaticoduodenectomy. Surg Gynecol Obstet, 1984. 158(2): p. 133-6.
Takada, T., et al., Postprandial plasma gastrin and secretin concentrations after a pancreatoduodenectomy. A comparison between a pylorus-preserving pancreatoduodenectomy and the Whipple procedure. Ann Surg, 1989. 210(1): p. 47-51.
Gumbs, A.A., A.J. Duffy, and R.L. Bell, Incidence and management of marginal ulceration after laparoscopic Roux-Y gastric bypass. Surg Obes Relat Dis, 2006. 2(4): p. 460-3.
Wilson, J.A., et al., Predictors of endoscopic findings after Roux-en-Y gastric bypass. Am J Gastroenterol, 2006. 101(10): p. 2194-9.
Coblijn, U.K., et al., Development of Ulcer Disease After Roux-en-Y Gastric Bypass, Incidence, Risk Factors, and Patient Presentation: A Systematic Review. Obes Surg, 2013.
Drepper, M.D., L. Spahr, and J.L. Frossard, Clopidogrel and proton pump inhibitors--where do we stand in 2012? World J Gastroenterol, 2012. 18(18): p. 2161-71.
Katz, M.H., Failing the acid test: benefits of proton pump inhibitors may not justify the risks for many users. Arch Intern Med, 2010. 170(9): p. 747-8.
Lepage C, R.B., Jooste V et al., Continuing rapid increase in esophageal adenocarcinoma in England and Wales. The American Journal of Gastroenterology 2008. 103(11): p. 2694-9.
PJ, R., Could proton pump inhibitors cause cancer? Archives of Internal Medicine, 2010. 170(19): p. 1775-6.
Brunner, G., C. Athmann, and A. Schneider, Long-term, open-label trial: safety and efficacy of continuous maintenance treatment with pantoprazole for up to 15 years in severe acid-peptic disease. Alimentary Pharmacology & Therapeutics, 2012. 36(1): p. 37-47.
Fiocca, R., et al., Gastric exocrine and endocrine cell morphology under prolonged acid inhibition therapy: results of a 5-year follow-up in the LOTUS trial. Aliment Pharmacol Ther, 2012. 36(10): p. 959-71.
Acknowledgments
We thank Kellie Kaneshiro of the Indiana University Ruth Lilly Medical Library for assistance with reference search and retrieval.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Butler, J.R., Rogers, T., Eckart, G. et al. Is Antisecretory Therapy After Pancreatoduodenectomy Necessary? Meta-analysis and Contemporary Practices of Pancreatic Surgeons. J Gastrointest Surg 19, 604–612 (2015). https://doi.org/10.1007/s11605-015-2765-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2765-8