Abstract
Objective
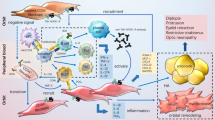
Thyroid-associated ophthalmopathy (TAO) is an autoimmune disorder involving the orbital tissue. This study aimed to understand the role of regulatory T cells (Tregs) in TAO during 12-week systemic glucocorticoid (GC) treatment.
Methods
Thirty-two moderate-severe TAO patients with a clinical activity score (CAS) ≥3/7 or with prolonged T2 relaxation time (T2RT) on at least one side of extraocular muscle (EOM) were enrolled. The percentage of the peripheral CD4+CD25(high)CD127(−/low) Tregs was analyzed using flow cytometry before and after the GC treatment. The activity and severity of TAO, T2RT, and the clinical outcomes after the GC treatment were assessed. Their correlation with the peripheral Tregs was investigated.
Results
There was no significant association between the baseline Treg fraction and the activity and severity of TAO or the treatment response. A significant reduction of Tregs was observed after the GC therapy merely in patients without any clinical improvement.
Conclusion
Treg reduction after systemic GC therapy is indicative of a poor therapeutic response. Accordingly, dynamic alterations of Tregs could help to evaluate the effectiveness of the GC treatment.
Similar content being viewed by others
References
Rotondo Dottore G, Torregrossa L, Caturegli P, et al. Association of T and B Cells Infiltrating Orbital Tissues With Clinical Features of Graves Orbitopathy. JAMA Ophthalmol, 2018,136(6):613–619
Potgieser PW, Wiersinga WM, Regensburg NI, et al. Some studies on the natural history of Graves’ orbitopathy: increase in orbital fat is a rather late phenomenon. Eur J Endocrinol, 2015,173(2):149–153
Hiromatsu Y, Eguchi H, Tani J, et al. Graves’ ophthalmopathy: epidemiology and natural history. Intern Med, 2014,53(5):353–360
Bahn RS. Graves’ ophthalmopathy. N Engl J Med, 2010,362(8):726–738
Bartalena L, Baldeschi L, Boboridis K, et al. The 2016 European Thyroid Association/European Group on Graves’ Orbitopathy Guidelines for the Management of Graves’ Orbitopathy. Eur Thyroid J, 2016,5(1):9–26
Gorman CA, Garrity JA, Fatourechi V, et al. A Prospective, Randomized, Double-blind, Placebo-controlled Study of Orbital Radiotherapy for Graves’ Ophthalmopathy. Ophthalmology, 2020,127(4S):S160–S171
Perez-Moreiras JV, Varela-Agra M, Prada-Sanchez MC, et al. Steroid-Resistant Graves’ Orbitopathy Treated with Tocilizumab in Real-World Clinical Practice: A 9-Year Single-Center Experience. J Clin Med, 2021,10(4):706
Vannucchi G, Campi I, Covelli D, et al. Efficacy Profile and Safety of Very Low-Dose Rituximab in Patients with Graves’ Orbitopathy. Thyroid, 2021,31(5):821–828
Kahaly GJ, Riedl M, König J, et al. Mycophenolate plus methylprednisolone versus methylprednisolone alone in active, moderate-to-severe Graves’ orbitopathy (MINGO): a randomised, observer-masked, multicentre trial. Lancet Diabetes Endocrinol, 2018,6(4):287–298
Strianese D, Iuliano A, Ferrara M, et al. Methotrexate for the treatment of thyroid eye disease. J Ophthalmol, 2014,2014:128903
Huang Y, Fang S, Li D, et al. The involvement of T cell pathogenesis in thyroid-associated ophthalmopathy. Eye (Lond), 2019,33(2):176–182
Brusko TM, Putnam AL, Bluestone JA. Human regulatory T cells: role in autoimmune disease and therapeutic opportunities. Immunol Rev, 2008,223:371–390
Shao S, Yu X, Shen L. Autoimmune thyroid diseases and Th17/Treg lymphocytes. Life Sci, 2018,192:160–165
Pawlowski P, Wawrusiewicz-Kurylonek N, Eckstein A, et al. Disturbances of modulating molecules (FOXP3, CTLA-4/CD28/B7, and CD40/CD40L) mRNA expressions in the orbital tissue from patients with severe graves’ ophthalmopathy. Mediators Inflamm, 2015,2015:340934
Rodriguez-Munoz A, Vitales-Noyola M, Ramos-Levi A, et al. Levels of regulatory T cells CD69(+)NKG2D(+) IL-10(+) are increased in patients with autoimmune thyroid disorders. Endocrine, 2016,51(3):478–489
Pawlowski P, Grubczak K, Kostecki J, et al. Decreased Frequencies of Peripheral Blood CD4+CD25+CD127-Foxp3+ in Patients with Graves’ Disease and Graves’ Orbitopathy: Enhancing Effect of Insulin Growth Factor-1 on Treg Cells. Horm Metab Res, 2017,49(3):185–191
Li C, Yuan J, Zhu YF, et al. Imbalance of Th17/Treg in Different Subtypes of Autoimmune Thyroid Diseases. Cell Physiol Biochem, 2016,40(1–2):245–252
Tachibana S, Murakami T, Noguchi H, et al. Orbital magnetic resonance imaging combined with clinical activity score can improve the sensitivity of detection of disease activity and prediction of response to immunosuppressive therapy for Graves’ ophthalmopathy. Endocr J, 2010,57(10):853–861
He Y, Mu K, Liu R, et al. Comparison of two different regimens of intravenous methylprednisolone for patients with moderate to severe and active Graves’ ophthalmopathy: a prospective, randomized controlled trial. Endocr J, 2017,64(2):141–149
Ye X, Bo X, Hu X, et al. Efficacy and safety of mycophenolate mofetil in patients with active moderate-to-severe Graves’ orbitopathy. Clin Endocrinol (Oxf), 2017,86(2):247–255
Chen W, Hu H, Chen HH, et al. Utility of T2 mapping in the staging of thyroid-associated ophthalmopathy: efficiency of region of interest selection methods. Acta Radiol, 2020,61(11): 1512–1519
Hou K, Ai T, Hu WK, et al. Three dimensional orbital magnetic resonance T2-mapping in the evaluation of patients with Graves’ ophthalmopathy. J Huazhong Univ Sci Technolog Med Sci, 2017,37(6):938–942
Ziegler SF. FOXP3: of mice and men. Annu Rev Immunol, 2006,24:209–226
Arbelaez CA, Glatigny S, Duhen R, et al. IL-7/IL-7 Receptor Signaling Differentially Affects Effector CD4+ T Cell Subsets Involved in Experimental Autoimmune Encephalomyelitis. J Immunol, 2015,195(5):1974–1983
Liu WH, Putnam AL, Zhou XY, et al. CD127 expression inversely correlates with FoxP3 and suppressive function of human CD4+ T reg cells. J Exp Med, 2006,203(7):1701–1711
Yu N, Li X, Song W, et al. CD4(+)CD25 (+)CD127 (low/−) T cells: a more specific Treg population in human peripheral blood. Inflammation, 2012,35(6):1773–1780
Seddiki N, Santner-Nanan B, Martinson J, et al. Expression of interleukin (IL)-2 and IL-7 receptors discriminates between human regulatory and activated T cells. J Exp Med, 2006,203(7):1693–1700
Lin SC, Chen KH, Lin CH, et al. The quantitative analysis of peripheral blood FOXP3-expressing T cells in systemic lupus erythematosus and rheumatoid arthritis patients. Eur J Clin Invest, 2007,37(12):987–996
Kawashiri SY, Kawakami A, Okada A, et al. CD4+CD25(high)CD127(low/-) Treg cell frequency from peripheral blood correlates with disease activity in patients with rheumatoid arthritis. J Rheumatol, 2011,38(12):2517–2521
Matsuzawa K, Izawa S, Okura T, et al. Implications of FoxP3-positive and -negative CD4(+) CD25(+) T cells in Graves’ ophthalmopathy. Endocr J, 2016,63(8):755–764
Glick AB, Wodzinski A, Fu P, et al. Impairment of regulatory T-cell function in autoimmune thyroid disease. Thyroid, 2013,23(7):871–878
Mao C, Wang S, Xiao Y, et al. Impairment of Regulatory Capacity of CD4+CD25+ Regulatory T Cells Mediated by Dendritic Cell Polarization and Hyperthyroidism in Graves’ Disease. J Immunol, 2011,186(8):4734–4743
Siomkajlo M, Mizera L, Szymczak D, et al. Effect of systemic steroid therapy in Graves’ orbitopathy on regulatory T cells and Th17/Treg ratio. J Endocrinol Invest, 2021,44(11):2475–2484
Strehl C, Ehlers L, Gaber T, et al. Glucocorticoids-All-Rounders Tackling the Versatile Players of the Immune System. Front Immunol, 2019,10:1744
Sbiera S, Dexneit T, Reichardt SD, et al. Influence of short-term glucocorticoid therapy on regulatory T cells in vivo. PLoS One, 2011,6(9):e24345
Cari L, De Rosa F, Nocentini G, et al. Context-Dependent Effect of Glucocorticoids on the Proliferation, Differentiation, and Apoptosis of Regulatory T Cells: A Review of the Empirical Evidence and Clinical Applications. Int J Mol Sci, 2019,20(5):1142
Kikuchi J, Hashizume M, Kaneko Y, et al. Peripheral blood CD4(+)CD25(+)CD127(low) regulatory T cells are significantly increased by tocilizumab treatment in patients with rheumatoid arthritis: increase in regulatory T cells correlates with clinical response. Arthritis Res Ther, 2015,17:10
Ciccocioppo F, Lanuti P, Pierdomenico L, et al. The Characterization of Regulatory T-Cell Profiles in Alzheimer’s Disease and Multiple Sclerosis. Sci Rep, 2019,9(1):8788
Quirant-Sanchez B, Hervas-Garcia JV, Teniente-Serra A, et al. Predicting therapeutic response to fingolimod treatment in multiple sclerosis patients. CNS Neurosci Ther, 2018,24(12):1175–1184
Miyabe C, Miyabe Y, Strle K, et al. An expanded population of pathogenic regulatory T cells in giant cell arteritis is abrogated by IL-6 blockade therapy. Ann Rheum Dis, 2017,76(5):898–905
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflicts of interest.
Author Shi-ying SHAO is a member of the Youth Editorial Board for Current Medical Science. The paper was handled by other editors and has undergone rigorous peer review process. Author Shi-ying SHAO was not involved in the journal’s review of, or decision related to, this manuscript.
Additional information
This work was supported by the National Natural Science Foundation of China (No. 81100581) and the Beijing Bethune Charitable Foundation (No. 2021).
Supplementary data
Rights and permissions
About this article
Cite this article
Xu, Qq., Zhang, Xl., Luo, B. et al. Role of Peripheral Regulatory T Lymphocytes in Patients with Thyroid Associated Ophthalmopathy During Systemic Glucocorticoid Treatment: A Prospective Observational Study. CURR MED SCI 43, 130–138 (2023). https://doi.org/10.1007/s11596-022-2671-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2671-8