Abstract
The coronavirus disease 2019 (COVID-19) pandemic is an ongoing geriatric health emergency with a substantial increase in the prevalence of medical and mental health issues, particularly among older adults living in residential care homes. The knowledge of the risk and protective factors related to the psychological impact of the COVID-19 pandemic on older adults living in residential care homes is based on limited data. This study aimed to investigate whether loneliness mediates the effects of fear generated by a pandemic on depression. Additionally, we hypothesized that self-compassion moderates the effect of loneliness on depression. A sample comprised 323 older adults (females: n = 141, males: n = 182) with mean age = 74.98 years (standard deviation = 6.59, age 65–90) completed a survey comprising the Fear of COVID-19 Scale, De Jung Gierveld Loneliness Scale, the nine-item Patient Health Questionnaire, and the Self-compassion Scale. The results revealed that the total effect of fear on depression was statistically significant, with a medium effect size (Cohen’s f 2 = .14) and this association was partially mediated by loneliness (β = .11, SE = .04, P < .001, t = 2.91, 95% CI 0.04–0.19). The self-compassion also moderated the loneliness effect on depression. The findings of this study support COVID-19 evidence, indicating that a greater level of fear generated by the pandemic is linked to depression and loneliness. The findings support the notion that self-compassion mitigates the adverse effects of stressful events in older adults. Customized self-compassion programs may be effective loneliness-mitigating interventions for older adults living in residential care homes.
Similar content being viewed by others
The pandemic of coronavirus disease 2019 (COVID-19) is an ongoing geriatric health emergency (Malone et al., 2020), associated with a substantial increase in the prevalence of medical and mental health issues (Applegate & Ouslander, 2020; Vahia & Shah, 2020). Older adults (65 years and older) are considered the population most vulnerable to the COVID-19 pandemic (Brydon et al., 2022; Sharma, 2021), with more COVID-19-positive cases and higher mortality rates due to COVID-19 (Wynants et al., 2020). For older adults, research has predominantly concentrated on physical health problems such as infection and mortality rates. Scientific evidence reporting the psychological and social health impacts of COVID-19 among older adults is limited (Verbiest et al., 2022). Similar to any health disaster, the pandemic has generated fear, anxiety, stress, and emotional exhaustion. As older adults are at high risk of pre-existing disease, hospitalization (Stokes et al., 2020), developing a severe infection, and relatively high mortality rates, they reported higher levels of fear of COVID-19 than the general population (García-Portilla et al., 2021; Mistry et al., 2021).
Mental Health Problems During COVID-19
Fear of infection or infecting family members has been recognized as the most common psychological distress caused by the pandemic for all groups (Lin et al., 2020; Nazari et al., 2021a, 2021b). The fear generated by the COVID-19 outbreak has contributed to potentially impaired well-being and led to increased morbidity and mortality rates among older adults (Lebrasseur et al., 2021). Research has indicated that mood fluctuations, limited physical activity, loneliness (Savci et al., 2021), pre-existing medical diseases, and increased smoking are associated with higher levels of fear and psychological distress (Parlapani et al., 2021; Siegmund et al., 2021). Fear of COVID-19 increases levels of stress, anxiety, and depression. However, the negative impact of COVID-19 on older adults extends beyond the fear of an increased risk of infection. While social distancing can help curtail the spread of COVID-19, other unexpected impacts for older adults, such as increased feelings of loneliness, warrant concern (Vahia & Shah, 2020).
Social distancing measures and policies to minimize contagious infection may detrimentally affect the quality of life and lead to an increased risk of loneliness among older adults (Choi et al., 2021; Macdonald & Hülür, 2021). Loneliness is a threat to well-being across the lifespan, yet it has unique implications for older adults. Loneliness refers to a negative subjective sense of isolation that lacks the quality of expected social relations and is a highly prevalent problem among the aging population (Tyrrell & Williams, 2020). Loneliness significantly affects a range of medical conditions (e.g., cardiovascular disease (Golaszewski et al., 2022) and lowered immunity (Cole et al., 2015), including early all-cause mortality (Paul et al., 2021). In addition, research during the pandemic showed a strong link between loneliness, suicidality (Mendonça Lima et al., 2021), and psychopathology (Grossman et al., 2021; Manca et al., 2020; Palgi et al., 2020; Zhang et al., 2022), with the strongest association being depression (Santini et al., 2020). Although the precise association between loneliness and depression is difficult to determine, studies have indicated that loneliness is a predictor of depressive symptoms rather than the reverse (e.g., Cacioppo et al., 2010). Loneliness and COVID-19 psychological distress (e.g., fear) were significant predictors of deteriorating depressive symptoms (Raina et al., 2021). Depression is a strong predictor of quality of life in the aging population (Tesky et al., 2019; Zenebe et al., 2021). During the pandemic, older adults reported twice the odds of depressive symptoms compared to pre-COVID-19. Compared to non-depressed peers, depressed older persons are more likely to have cognitive impairments, recover more slowly from stroke, and have a disproportionate frequency of hospitalization (Atzendorf & Gruber, 2021; Matthews et al., 2022). Loneliness is associated with myriad adverse health outcomes, such as impaired immune functioning, which adds higher risk for coronavirus infection, complications, and death (Van Orden et al., 2021). Older adults are at combination risk, making effective management of loneliness and social isolation in our older patients a high priority target for preventive intervention. In the early stage of the pandemic, geriatric experts emphasized the importance of identifying protective mechanisms to reduce the adverse psychosocial impacts of the COVID-19 pandemic (Gardiner et al., 2020). However, pertinent evidence is limited.
Self-compassion as a Protective Factor
Self-compassion is conceptualized as the balance between decreased negative and increased positive self-responses (Neff, 2003). Research has shown that self-compassion is a protective factor against loneliness (Akin, 2010), psychological distress (Marsh et al., 2018), and depression (Fan et al., 2022). Self-compassion enhances well-being (Athanasakou et al., 2020), life satisfaction (Nazari et al., 2022), and emotion regulation (Zessin et al., 2015). Although empirical information on the aging population is lacking, emerging evidence suggests that self-compassion is linked to well-being (Bratt & Fagerström, 2020), quality of life, and positive attitudes toward aging (Brown et al., 2016; Kim & Ko, 2018). Self-compassion significantly predicts lower levels of depressive symptoms in aging populations (Homan, 2016), (Brown et al., 2019). Self-compassion facets (i.e., self-kindness, shared humanity, and mindfulness) have been shown to have negative relationships with feelings of loneliness and are associated with effective acceptance of aging limitations (e.g., physical limitation), higher motivation for self-care, and more resiliency (Smith, 2015). Treating kindness and friendliness to themselves rather than harshly self-criticism, (ii) being mindfully aware of painful events instead of over identification, and (iii) cognitively accepting unpleasant experiences as common experiences for humans instead of being isolated and avoidant may offer effective coping strategies to buffer against the negative impacts of stressful experiences (Allen & Leary, 2014; Smith, 2015). The key to overcoming loneliness has always been to find inner peace (Neff, 2016). People should be compassionate about themselves when suffering or in a crisis. This is in accordance with the cognitive approach to loneliness, which holds that in the face of loneliness, one may adjust expectations and be pleased with current sustained social interaction. Consequently, self-compassion can support well-being during high stress and loneliness (Schnepper et al., 2020). Self-compassion interventions significantly reduced depressive symptoms (Diedrich et al., 2017) via improvements in emotion regulation (Sloan et al., 2017). COVID-19 research among general populations indicated that low self-compassion elevated negative affects, causing depression (Beato et al., 2021). Additionally, depression was strongly associated with low self-compassion for COVID-19 (Gutiérrez-Hernández et al., 2021). Subsequently, self-compassion is suggested as a protective factor against mental health problems and psychological distress during the pandemic (Lau et al., 2020). In a systematic review of eleven research, self-compassion was associated with reduced depressive symptoms. Also, the findings showed that self-compassion moderated the associations between health issues and well-being (Brown et al., 2019). Another scoping review of the twelve studies for older adults (i.e., mean age 65 years) self-compassion appears to be a valuable resource for older adult psychological adjustment and may promote resilience connected to age-related challenges (Tavares et al., 2020).
Even before the current pandemic, loneliness was becoming a crucial public health issue. The pandemic and related containment efforts have raised awareness of loneliness concerns even more prominently (Gardiner et al., 2020). The current pandemic is labelled “a lonely pandemic” (Hartt, 2020). Only a few treatments have been suggested to reduce loneliness. Loneliness leads to cognitive deficits (i.e., hypervigilance to social threats) and impaired cognitive processing (i.e., negative bias toward social relationships) (Yu et al., 2020). Consequently, older people are at a higher risk of unsatisfactory social connections. While the quality of interactions is a predictor of loneliness, intervention strategies that specifically focus on increasing the number of social interactions may address social isolation (Masi et al., 2011). In addition, individuals who are more alone suffer more significant negative evolution toward themselves, which makes them more emotionally and socially hampered and hesitant to interact (Khan & Kadoya, 2021). Intervention strategies against loneliness that specifically focus on strengthening interpersonal skills and expanding access to social interaction may not be promising for reducing loneliness (Jarvis et al., 2020). Research indicates that one of the critical predictors of loneliness is a cognitive-affective attitude toward oneself (Borawski, 2019). Self-compassion is a cognitive-affective skill based on self-constructs and may be relevant in reducing loneliness and depression. There is a lack of studies exploring the role of self-compassion among older adults during the COVID-19 pandemic.
Purpose of This Study
This pandemic has brought unprecedented challenges to the care of older adults. These problems have been reported to be even more prevalent in older adults living in residential care homes (RCHs) (Van Tilburg et al., 2021). Globally, older adults in RCHs account for a disproportionate number of positive cases and have a much higher mortality rate of COVID-19 (Crotty et al., 2020; Heras et al., 2021). Living in RCHs was a risk factor for depression during the pandemic (Sams et al., 2021; Wang et al., 2021). Older adults in RCHs experience higher levels of loneliness during the COVID-19 pandemic (Flint et al., 2020; Ho et al., 2022). Older adults in RCHs have even fewer face-to-face encounters with their families and communities than normal adults. Additionally, residents of nursing homes may face diminished freedom owing to facility regulations, limited privacy due to shared accommodation, and struggles to have meaningful social connections (Trybusińska & Saracen, 2019). The current knowledge of the risk and protective factors related to the adverse psychological impact of the COVID-19 pandemic on older adults in RCHs is primarily based on limited data. Emotionally difficult conditions are linked with psychological and physical comorbidities; they must be closely monitored, practically in combination with potential risk and protective factors and health outcomes, to develop effective interventions to minimize the adverse effects of the pandemic.
Therefore, this study aimed to examine the relationships between sociodemographic characteristics, fear of COVID-19, loneliness, depression, and self-compassion. We hypothesized that the fear of COVID-19 would directly predict depressive symptoms. Also, it was hypothesized that loneliness mediates the link between COVID-19 fear and depression. Greater loneliness is expected to result in more depressive symptoms among older adults with higher levels of fear of COVID-19. Additionally, it was hypothesized that self-compassion would moderate the loneliness effect on depression. It was expected that for older adults a higher self-compassion level for lonely older adults would be associated with a lower level of depressive severity. Finally, it was hypothesized that self-compassion moderated the mediated loneliness effect (direct effect of fear of COVID-19 on depressive symptoms), as the direct effect was stronger (or weaker) when older adults’ self-compassion was high (or low).
Methods
Participants
The study’s participants (N = 323) were older adults living in RCHs who were recruited using convenience sampling. The inclusion criteria were (a) aged 65 years and older, (b) resident care home for over one year, (c) ability to read and complete the survey, (d) fluency in Persian, and (e) obtain a signed informed consent. Participants were excluded if they met the following criteria: (a) presence of a severe condition that would require prioritization for treatment (e.g., schizophrenia, psychosis); (b) cognitive problems (e.g., dementia); and (c) clear and current or history of substance dependence disorder or alcohol, and suicide.
Instruments
The survey comprised the Fear of COVID-19 Scale [FCV-19S; (Ahorsu et al., 2022)], the 6-item De Jung Gierveld Loneliness Scale [DJGLS-6; (Gierveld & Van Tilburg, 2006)], the Patient Health Questionnaire-9 [PHQ-9; (Kroenke et al., 2001)], and the Self-compassion scale [SCS; (Neff, 2003)].
The Fear Generated by COVID-19
The FCV-19S, a brief unidimensional self-report scale, was used to measure reactions of emotional fear to the pandemic. The respondents rated seven items reflecting emotional fear reactions towards the pandemic (e.g., “I am afraid of losing my life because of coronavirus-19”), on a Likert-type scale ranging from 1 (strongly disagree) to 5 (strongly agree). The total raw scores can range from 7 to 35. Higher scores indicate higher levels of fear generated by COVID-19 (Cronbach’s alpha = 0.89).
Depressive Symptoms
The nine-item PHQ-9 was used to screen major depression and subthreshold depression in the past 2 weeks. The respondents rated the items (e.g., “Trouble falling or staying asleep, or sleeping too much”) on a four-point scale ranging from 0 (not at all) to 3 (nearly every day). The PHQ-9 total score ranges from 0 to 27. Higher scores indicate more severe depressive symptoms (Cronbach’s alpha = 0.85).
Loneliness
The DJGLS-6 was used to measure loneliness. Respondents endorsed the 6 items (e.g., “I experience a general sense of emptiness”) on a scale from 0 to 2 and were then recoded as dichotomous (0 or 1). The total score ranges from zero (no loneliness) to six (extreme loneliness), with higher scores indicating higher loneliness (Cronbach’s alpha = 0.83).
Self-compassion
The SCS, a 26-item self-reporting instrument, was used to assess self-compassion. Statements on the SCS (e.g.; I’m kind to myself when I’m experiencing suffering) were scored on a Likert scale ranging from 1 (almost never) to 5 (almost always). A higher score indicates higher self-compassion (Cronbach’s alpha = 0.86).
Demographic Variables
Nursing staff provided information related to the age, sex, educational level, and medical conditions of the participants, such as underlying diseases (cancer, diabetes, heart disease, and lung disease), using each participant’s registered file.
Procedure
This study was adhered to the STROBE checklist and was found to follow the ethical principles of the Helsinki Declaration. The study, including all assessments and procedures, was reviewed by the National Institute for Medical Research and Development and the Institutional Human Research Ethics Committee (Research Proposal no. 993494). This cross-sectional study was conducted from October 2021 to June 2022 in Iran. Out of 15 official nursing homes, seven nursing homes were included in the research. In the first step, the care and nursing staff were informed about the research objectives, the data collection methods, and the eligibility criteria. Nursing staff identified potentially eligible older adults based on registered medical and personal documents. Next, the survey letters were distributed by the nursing staff. On the first page of the survey, an informed consent form was included. Also, the participants were informed about the objectives of the research, voluntary participation, how to obtain an informed consent form, and how to complete the questionnaire. The nurses provided information on how the participants signed the informed consent form and completed the survey. All the participants provided signed informed consent. No incentive types were offered to participate in this study. All subjects’ information was anonymized and de-identified by the nursing staff.
Sample Size
A priori power analysis was computed for structural equation modeling (SEM) online using the numbers of latent variables, observed variables, alpha of.05, and power level of 0.80 to detect the small effect size. The required sample size was 316 to the expected 10% dropout rate.
Data Analysis
Descriptive characteristics
There were no missing values in the assessed variables; therefore, no imputation method was implemented. Means and standard deviations (SD) were computed to describe continuous variables, and frequencies and percentages were computed to report categorical variables. Appropriate tests were performed to investigate sex-related differences. The data were checked for normality, as evaluated by absolute skewness and kurtosis values. Multicollinearity was checked by evaluating the variance inflation factor values (1 < VIF < 5). (Tabachnick & Fidell, 2018). A correlation analysis was conducted to evaluate the associations between sociodemographic characteristics and variables of interest.
Moderated Mediation Analysis
The moderated mediation model is shown as a conceptual diagram and a statistical diagram in Fig. 1. Moderated mediation analysis was conducted to examine the relationships between COVID-19 fear (X), loneliness (M), depression (Y), and self-compassion (V). The PROCESS macro for SPSS (model 4) was conducted to investigate whether loneliness mediates the link between fear and depression (path C). Next, PROCESS macro (model 14) was applied to determine whether self-compassion moderates the effects of loneliness (path b) and indirect fear of COVID-19 on depression via loneliness (path C’). The bias-corrected method was employed to generate 95% confidence intervals (CIs) with a point estimate and 5000 bootstrap samples (Hayes & Hayes, 2018).
Proposed model depicted as a conceptual model and a statistical diagram. Panel A = mediation model, panel B = final model for moderating effects of self-compassion. X: independent variable (fear of COVID-19), Y: dependent variable (Depression). M: Mediator (Loneliness), V: Moderator (self-compassion). MV: Interaction effect (Loneliness × self-compassion)
Simple slope analyses were performed to visualize the influence of the interaction effect and beta coefficients were calculated at low level (mean minus 1 SD), average level (mean), and high level (mean plus 1 SD) of self-compassion. To investigate the conditional indirect effect of fear on depression via loneliness as a function of different levels of the self-compassion, indirect effects were examined at three levels of the self-compassion (mean plus 1 SD, at the mean, and mean minus 1 SD). An effect was considered statistically significant if the 95% CIs did not include zero. The continuous predictors were centered on their means before computing the interaction terms to minimize multicollinearity. The benchmark suggested by Hu and Bentler (Hu & Bentler, 1999) was considered in evaluating the goodness of fit of the model: (1 < χ2/pdf < 3, comparative fit index (CFI) > 0.95, and root mean square error of approximation (RMSEA) < 0.06). SPSS (version 25, IBM Corp) and AMOS (version 24, IBM Corp) were utilized to test hypotheses (two-tailed). An alpha level of.05 was used to indicate statistical significance.
Results
Descriptive Statistics
Of the 420 returned surveys, data from 323 were included in the analysis (Table 1). A sample comprised 323 older adults (females: n = 141, 43.7%, males: n = 182, 56.3%) in RCHs with Mage = 74.98 years (SD = 6.59, age 65–90). Overall, the participants were less educated (χ2 = 27.92, P < 0.001). Men had significantly higher fear scores than women (t321 = 2.85, P = 0.006, Cohen’s d = 0.32, 95% CI 0.11–0.55. Women obtained significantly higher depression scores than men (t321 = 3.34, P = 0.001, Cohen’s d = − 0.36, 95% CI − 0.58 to − 0.13.
The values of skewness and kurtosis were within <|1| which suggested the absence of severe violations of normality. The VIF values were < 5, indicating the absence of multicollinearity (Table 2). Correlation analyses showed a moderate association between sociodemographic characteristics, fear of COVID-19, loneliness, depression, and self-compassion (see Table 2). Fear was correlated with loneliness (r = 0.31, 95% CI 0.24–0.37, P < 0.001), depression (r = 0.35, P < 0.001, 95% CI 0.29–0.41), self-compassion (r = − 0.29, P < 0.001, 95% CI − 0.35 to − 0.24), and physical comorbidity (r = 0.49, 95% CI 0.45–0.53, P < 0.001). Age was found to be moderately associated with loneliness (r = 0.39, P < 0.001, 95% CI 0.34–0.44).
Mediation Analysis
The final results are presented in Table 3. The total effect of fear on depression (path C) was medium (Cohen’s f 2 = 0.14). Fear of COVID-19 predicted loneliness (path a) with a small-to-medium effect size (Cohen’s f 2 = 0.12). Loneliness directly predicted depression (path b), with a large effect size (Cohen’s f 2 = 0.35). Fear generated by the pandemic directly (Cohen’s f 2 = 0.11) and indirectly predicted depressive symptoms through loneliness (path ab = indirect effect: β = 0.11, SE = 0.04, P < 0.001, t = 2.91, 95% CI 0.04–0.19). The direct effect of fear on depressive symptoms (path C) was statistically significant. Therefore, loneliness partially mediated the effect of fear of COVID-19 on depression.
Moderated Mediation Analysis
The model fit the data excellently (χ2/df = 1.22, CFI = 0.99, RMSEA = 0.02, 90% CI 0.01–0.05, with R2 = 0.53, F (4, 318) = 87.70, P < 0.001). The direct effect of self-compassion on depression (path b2) was significant with a small effect size (Cohen’s f 2 = 0.03). The interaction effect of self-compassion with loneliness (loneliness × self-compassion) on depression (path b3) was statistically significant, β = − 0.38, SE = 0.05, P < 0.001, t = 7.58, 95% CI − 0.48 to − 0.30, indicating that self-compassion moderated the effect of loneliness on depression, with ∆ R2 = 0.15, F (1, 318) = 102.74, P < 0.001. The direct effect of loneliness on depression (path b’) was statistically significant with a medium to large effect size (Cohen’s f 2 = 0.19). Therefore, the strong effect of loneliness on depression (path b) was partially moderated by self-compassion.
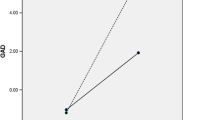
Simple slope analyses are illustrated in Fig. 2. Loneliness significantly predicted depression in older adults with lower levels (mean minus 1 SD) of self-compassion (Beta = 0.17, SE = 0.01, P < 0.001, 95% CI 0.15–0.19) and average levels (mean) of self-compassion (Beta = 0.09, SE = 0.01, P < 0.001, 95% CI 0.06–0.12). However, for participants with greater (mean plus 1 SD) self-compassion levels, the effect of loneliness on depression was not significant (Beta = –0.06, SE = 0.01, P = 0.70, 95% CI − 0.03–0.02.
The mediating effect of loneliness changed according to the level of the self-compassion and was weakest at self-compassion high level (1SD plus the mean). These indicate that older adults suffering from loneliness were less susceptible to depression when they were felt self-compassionate climate (Table 4).
Discussion
The COVID-19 pandemic has presented additional challenges to older adults in RCHs. This study investigated the relationships between fear generated by the pandemic, depression, self-compassion, and loneliness among older adults living in RCHs. Consistent with the literature, older adults reported high levels of fear of COVID-19 (Caycho-Rodríguez et al., 2022; García-Portilla et al., 2021; Mistry et al., 2021; Yadav et al., 2021). The findings of this study support COVID-19 evidence, indicating that a greater level of fear generated by the pandemic is linked to psychopathology in the form of depression (Parlapani et al., 2020; Yu & Mahendran, 2021) and loneliness (Cihan et al., 2021; Yadav et al., 2021). Attentional bias threat theory posits that individuals with greater levels of fear may provide a maladaptive attentional response (i.e., excessive or intensive) to threats, which can lead to negative emotions and rumination (Cannito et al., 2020; Yao et al., 2022). Rumination prevents adaptive coping with unpleasant experiences and predicts depressive symptoms (López et al., 2018). Loneliness is also associated with hypervigilance to social threats (Abdellaoui et al., 2019). Consequently, loneliness generates a vicious cycle in which individuals perceive social interactions as unpleasant or unfriendly.
The findings of the mediation analysis showed that loneliness mediates the association between fear and depression. The findings of this study amplify previous evidence that loneliness is a critical predictor of depressive symptoms in older adults (Berg-Weger & Morley, 2020). Loneliness is a major mental consequence of COVID-19 and a viable risk factor for depressive symptoms among older adults living in RCHs (Molas-tuneu et al., 2022). During COVID-19, higher loneliness levels are associated with an excessively high risk of exacerbated depressive symptoms (Liu et al., 2021; Zhao et al., 2019). Little is known about the causal mechanisms between loneliness and depression (Lee et al., 2021). Cognitive deficits are a characteristic of depression in older adults (Fiske et al., 2009). Loneliness leads to cognitive deficits (i.e., hypervigilance to social threats) and impaired cognitive processing (i.e., negative bias toward social relationships) (Yu et al., 2020). Lonely individuals suffer greater negative evaluations of themselves, which leads to more negative evaluations of social interactions (higher negative affect) or evaluates the interaction as a less rewarding experience (lower positive affect) (Khan & Kadoya, 2021). Depression is associated with lower levels of positive affect (i.e., extraversion) and a lower tendency to experience the world in an energetic and sociable manner (Fredrickson & Joiner, 2018). Individuals with higher levels of depression reported more ineffective coping strategies (e.g., rumination and self-blame) and a lower prevalence of adaptive emotion regulation behaviors (e.g., positive reappraisal and acceptance) when experiencing negative emotions ( Lyubomirsky,et al., 2015).
Moderation analysis showed that self-compassion played a buffering role against the strong loneliness effect on depression in older adults. The results of the moderated mediation analysis indicated that for older adults who were more self-compassionate about threatening the pandemic context, the impacts of loneliness and fear of COVID-19 on symptoms of depression were potentially less severe. Individual differences in adaptive emotional responses to psychological distress generated by stressful events, such as self-compassion, may be associated with mental health problems. These results support the notion that the adverse mental health effects of the pandemic are mitigated in self-compassionate older adults (Deniz, 2021; Lau et al., 2020; Matos et al., 2022). In line with the study findings, evidence has shown a medium-to-large association between self-compassion and depression among aging populations (Brown et al., 2019). The six dimensions of self-compassion address adaptive responses to stressful events and personal struggles. Over-identifying negative feelings and thoughts implies a self-centered ruminative response considerably associated with negative affect. Regarding stressful events, the promotion of emotion regulation skills has been suggested to underlie the benefits of mindfulness (Gross et al., 2011; Vandekerckhove & Wang, 2018). Maladaptive emotion regulation strategies (i.e., self-blame and rumination) are associated with higher levels of depression. For older adults, higher self-compassion and mindfulness levels facilitate adaptive emotion regulation and lessen the chance of maladaptive emotion responses (Hodgetts et al., 2021), which are negatively associated with loneliness (Lindsay et al., 2019) and depression (Yat et al., 2019). The feeling of common humanity includes accepting individuals’ experiences (e.g., mistakes, shortcomings, inadequacies) as part of shared human life rather than a feature that sets one split from society, which fosters feelings of connectedness instead of a sense of loneliness.
In contrast to the large body of evidence in general (Nazari et al., 2021a, 2021b) and in an aging population (Gokseven et al., 2022), men reported greater levels of fear than women. Age is positively associated with self-compassion. Self-compassion was higher in geriatric samples than in younger populations (Tavares et al., 2020). Age and medical comorbidities were associated with a higher level of fear of COVID-19, loneliness, and depression. Consistent with previous studies, among older adults, medical comorbidities are associated with depression (Agustini et al., 2020; Frost et al., 2019) and loneliness (Barnes et al., 2021; Sha et al., 2020).
Practical Implication
These findings have important clinical implications for treating and managing older adults with both physical and mental health problems. Older age is an independent risk factor for the adverse impact of the pandemic (Savage et al., 2021), and older adults with medical comorbidities are more vulnerable to the negative consequences of the pandemic, with a higher mortality risk due to COVID-19 (Péterfi et al., 2022). Approximately 80% of older adults (aged 65 years) have at least two chronic diseases, and these physical comorbidities can be risk factors for loneliness (National Academies of Sciences, 2020). There was a reciprocal association between loneliness and physical health risk factors. Therefore, physicians must pay equal attention to psychological and medical disorders. In geriatric settings, depression is underdiagnosed and undertreated. The fear generated by the pandemic directly predicts depressive symptoms and indirectly predicts via loneliness. Loneliness strongly predicted depressive symptoms among older adults in RCHs. Potentially, the evaluation of fear and loneliness can be added to standard and routine clinical evaluations in geriatric settings. In addition to pharmacological and medical treatments, geriatric experts can suggest psychological interventions for patients with depressive symptoms or loneliness to reduce both physical and mental health problems.
Self-compassion may lead to positive attitudes toward aging-related complications and is associated with greater acceptance of physical limitations and motivation for self-care (Tavares et al., 2020). Unlike the use of self-compassion interventions in research on younger populations, no manual treatment has been published for aging populations. According to social-emotional selectivity theory, older individuals tend to save positive feelings and regulate emotions (Carstensen et al., 2003). While emotion regulation approach has received less attention in the aging population. Despite the high rate of psychological problems, elderly people are usually excluded from interventional studies. Moreover, psychological resources play an increasingly important role in achieving subjective and psychological well-being in older age and adaptive coping with unavoidable changes and challenges related to aging (Haase, 2013). Self-compassion is considered a learnable internal resource that can be promoted via several therapeutic approaches (e.g., cognitive‒behavioral therapy; (Diedrich et al., 2014)). In addition to mental health promotion, the present findings suggest that interventions that focus on promoting self-compassion among older adults could yield positive physical health effects. However, empirical evidence to confirm such efforts is limited.
Limitations
The findings of this study should be interpreted in light of several limitations. The most important limitation of this study was its small sample size. However, similar studies have been conducted with small sample sizes. Another limitation was the limited evidence available to replicate the findings of this study. In addition, this study was cross-sectional; therefore, causation could not be determined. Another limitation of the present study was that the data relied entirely on self-report measures which have well established methodological biases. Further studies with larger sample sizes and more robust methodologies (e.g., longitudinal research) are required to replicate the findings of this study.
Conclusion
Despite these limitations, these findings make a significant contribution to the limited expanding evidence on COVID-19 adverse impacts on depression and loneliness among older adults in RCHs. This study makes an incremental contribution to the self-compassion literature by demonstrating that self-compassion is linked with lower levels of mental health problems during aging life. Our findings suggest that self-compassion may mitigate the adverse psychosocial impact of the COVID-19 pandemic. As a resilience component, self-compassion in older adults may lead to recovery from stressful life situations by reducing the risk of depressive symptoms. As an emotion regulation strategy, self-compassion may potentially lead to coping with negative and unpleasant emotions, such as loneliness, and reduce depressive symptoms. Our results add to the few growing studies showing that self-compassion may protect against depressive symptoms by influencing loneliness. Customized self-compassion interventions may be effective loneliness-mitigating interventions and depression treatments for older adults living in RCHs to enhance resilience and promote adaptive emotion skills. Self-compassion can be promising in enhancing older adults’ psychological well-being and reducing the impact of stressful events.
Data Availability
The datasets generated and/or analysed during the current study are not publicly available due to [local policy considerations and limitations of ethical approval involving the patient data and anonymity] but are available from the corresponding author on reasonable request.
References
Abdellaoui, A., Chen, H. Y., Willemsen, G., Ehli, E. A., Davies, G. E., Verweij, K. J. H., Nivard, M. G., de Geus, E. J. C., Boomsma, D. I., & Cacioppo, J. T. (2019). Associations between loneliness and personality are mostly driven by a genetic association with Neuroticism. Journal of Personality, 87(2), 386–397. https://doi.org/10.1111/jopy.12397
Agustini, B., Lotfaliany, M., Woods, R. L., McNeil, J. J., Nelson, M. R., Shah, R. C., Murray, A. M., Ernst, M. E., Reid, C. M., Tonkin, A., Lockery, J. E., Williams, L. J., Berk, M., & Mohebbi, M. (2020). Patterns of association between depressive symptoms and chronic medical morbidities in older adults. Journal of the American Geriatrics Society, 68(8), 1834–1841. https://doi.org/10.1111/jgs.16468
Ahorsu, D. K., Lin, C. Y., Imani, V., Saffari, M., Griffiths, M. D., & Pakpour, A. H. (2022). The fear of COVID-19 scale: Development and initial validation. International Journal of Mental Health and Addiction, 20(3), 1537–1545. https://doi.org/10.1007/s11469-020-00270-8
Akin, A. (2010). Self-compassion and loneliness. International Online Journal Education, 2(3), 702–718.
Allen, A. B., & Leary, M. R. (2014). Self-compassionate responses to aging. The Gerontologist, 54(2), 190–200. https://doi.org/10.1093/geront/gns204
Applegate, W. B., & Ouslander, J. G. (2020). COVID-19 presents high risk to older persons. Journal of the American Geriatrics Society, 68(4), 681–681. https://doi.org/10.1111/jgs.16426
Athanasakou, D., Karakasidou, E., Pezirkianidis, C., Lakioti, A., & Stalikas, A. (2020). Self-Compassion in clinical samples: A systematic literature review. Psychology, 11(02), 217–244. https://doi.org/10.4236/psych.2020.112015
Atzendorf, J., & Gruber, S. (2021). Depression and loneliness of older adults in Europe and Israel after the first wave of covid-19. European Journal of Ageing, 19(4), 849–861. https://doi.org/10.1007/s10433-021-00640-8
Barnes, T. L., MacLeod, S., Tkatch, R., Ahuja, M., Albright, L., Schaeffer, J. A., & Yeh, C. S. (2021). Cumulative effect of loneliness and social isolation on health outcomes among older adults. Aging & Mental Health, 26(7), 1327–1334. https://doi.org/10.1080/13607863.2021.1940096
Beato, A. F., da Costa, L. P., & Nogueira, R. (2021). Everything is gonna be alright with me: The role of self-compassion, affect, and coping in negative emotional symptoms during coronavirus quarantine. International Journal of Environmental Research and Public Health, 18(4), 2017. https://doi.org/10.3390/ijerph18042017
Berg-Weger, M., & Morley, J. E. (2020). Editorial: Loneliness and social isolation in older adults during the Covid-19 pandemic: Implications for gerontological social work. The Journal of Nutrition, Health & Aging, 24(5), 456–458. https://doi.org/10.1007/s12603-020-1366-8
Borawski, D. (2019). Authenticity and rumination mediate the relationship between loneliness and well-being. Current Psychology, Advance Online Publication. https://doi.org/10.1007/s12144-019-00412-9
Bratt, A., & Fagerström, C. (2020). Self-compassion in old age: Confirmatory factor analysis of the 6-factor model and the internal consistency of the self-compassion scale-short form. Aging & Mental Health, 24(4), 642–648. https://doi.org/10.1080/13607863.2019.1569588
Brown, L., Bryant, C., Brown, V., Bei, B., & Judd, F. (2016). Self-compassion, attitudes to ageing and indicators of health and well-being among midlife women. Aging and Mental Health, 20(10), 1035–1043. https://doi.org/10.1080/13607863.2015.1060946
Brown, L., Huffman, J. C., & Bryant, C. (2019). Self-compassionate aging: A systematic review. The Gerontologist, 59(4), e311–e324. https://doi.org/10.1093/geront/gny108
Brydon, A., Bhar, S., Doyle, C., Batchelor, F., Lovelock, H., Almond, H., Mitchell, L., Nedeljkovic, M., Savvas, S., & Wuthrich, V. (2022). National survey on the impact of COVID-19 on the mental health of Australian residential aged care residents and staff. Clinical Gerontologist, 45(1), 58–70. https://doi.org/10.1080/07317115.2021.1985671
Cacioppo, J. T., Hawkley, L. C., & Thisted, R. A. (2010). Perceived social isolation makes me sad: 5-year cross-lagged analyses of loneliness and depressive symptomatology in the Chicago Health, Aging, and Social Relations Study. Psychology and Aging, 25(2), 453–463. https://doi.org/10.1037/a0017216
Cannito, L., Di Crosta, A., Palumbo, R., Ceccato, I., Anzani, S., La Malva, P., Palumbo, R., & Di Domenico, A. (2020). Health anxiety and attentional bias toward virus-related stimuli during the COVID-19 pandemic. Scientific Reports, 10(1), 1–8. https://doi.org/10.1038/s41598-020-73599-8. 16476.
Carstensen, L. L., Fung, H. H., & Charles, S. T. (2003). Socioemotional selectivity theory and the regulation of emotion in the second half of life. Motivation and Emotion, 27(2), 103–123. https://doi.org/10.1023/a:1024569803230
Caycho-Rodríguez, T., Tomás, J. M., Barboza-Palomino, M., Ventura-León, J., Gallegos, M., Reyes-Bossio, M., & Vilca, L. W. (2022). Assessment of fear of COVID-19 in older adults: Validation of the fear of COVID-19 scale. International Journal of Mental Health and Addiction, 20(2), 1231–1245. https://doi.org/10.1007/s11469-020-00438-2
Choi, E. Y., Farina, M. P., Wu, Q., & Ailshire, J. (2021). COVID-19 social distancing measures and loneliness among older adults. The Journals of Gerontology: Series B, 77(7), 167–178. https://doi.org/10.1093/geronb/gbab009
Cihan, F. G., & Gökgöz Durmaz, F. (2021). Evaluation of COVID-19 phobia and the feeling of loneliness in the geriatric age group. International Journal of Clinical Practice, 75(6), e14089. https://doi.org/10.1111/ijcp.14089
Cole, S. W., Capitanio, J. P., Chun, K., Arevalo, J. M. G., Ma, J., & Cacioppo, J. T. (2015). Myeloid differentiation architecture of leukocyte transcriptome dynamics in perceived social isolation. Proceedings of the National Academy of Sciences, 112(49), 15142–15147. https://doi.org/10.1073/pnas.1514249112
Crotty, F., Watson, R., & Lim, W. K. (2020). Nursing homes: The titanic of cruise ships – will residential aged care facilities survive the coronavirus disease 2019 pandemic? Internal Medicine Journal, 50(9), 1033–1036. https://doi.org/10.1111/imj.14966
Deniz, M. E. (2021). Self-compassion, intolerance of uncertainty, fear of COVID-19, and well-being: A serial mediation investigation. Personality and Individual Differences, 177(2020), 110824. https://doi.org/10.1016/j.paid.2021.110824
Diedrich, A., Grant, M., Hofmann, S. G., Hiller, W., & Berking, M. (2014). Self-compassion as an emotion regulation strategy in major depressive disorder. Behaviour Research and Therapy, 58, 43–51. https://doi.org/10.1016/j.brat.2014.05.006
Diedrich, A., Burger, J., Kirchner, M., & Berking, M. (2017). Adaptive emotion regulation mediates the relationship between self-compassion and depression in individuals with unipolar depression. Psychology Psychotherapy Theory, Research Practice, 90(3), 247–263. https://doi.org/10.1111/papt.12107
Fan, Q., Li, Y., Gao, Y., Nazari, N., & Griffiths, M. D. (2022). Self-compassion moderates the association between body dissatisfaction and suicidal ideation in adolescents: A cross-sectional study. International Journal of Mental Health and Addiction, Advance Online Publication. https://doi.org/10.1007/s11469-021-00727-4
Fiske, A., Wetherell, J. L., & Gatz, M. (2009). Depression in older adults. Annual Review Clinical Psychology., 5, 363–389. https://doi.org/10.1146/annurev.clinpsy.032408.153621
Flint, A. J., Bingham, K. S., & Iaboni, A. (2020). Effect of COVID-19 on the mental health care of older people in Canada. International Psychogeriatrics, 32(10), 1113–1116. https://doi.org/10.1017/s1041610220000708
Fredrickson, B. L., & Joiner, T. (2018). Reflections on positive emotions and upward spirals. Perspectives on Psychological Science, 13(2), 194–199. https://doi.org/10.1177/1745691617692106
Frost, R., Bauernfreund, Y., & Walters, K. (2019). Non-pharmacological interventions for depression/anxiety in older adults with physical comorbidities affecting functioning: Systematic review and meta-analysis. International Psychogeriatrics, 31(8), 1121–1136. https://doi.org/10.1017/s1041610218001564
García-Portilla, P., de la Fuente Tomás, L., Bobes-Bascarán, T., Jiménez Treviño, L., Zurrón Madera, P., Suárez Álvarez, M., Menéndez Miranda, I., García Álvarez, L., Sáiz Martínez, P. A., & Bobes, J. (2021). Are older adults also at higher psychological risk from COVID-19? Aging & Mental Health, 25(7), 1297–1304. https://doi.org/10.1080/13607863.2020.1805723
Gardiner, C., Laud, P., Heaton, T., & Got, M. (2020). What is the prevalence of loneliness among older people living in residential and nursing care homes? A systematic review and meta-analysis. Age and Ageing, 49(5), 748–757. https://doi.org/10.1093/ageing/afaa049
Gierveld, J. D. J., & Tilburg, T. V. (2006). A 6-item scale for overall, emotional, and social loneliness. Research on Aging, 28(5), 582–598. https://doi.org/10.1177/0164027506289723
Gokseven, Y., Ozturk, G. Z., Karadeniz, E., Sarı, E., Tas, B. G., & Ozdemir, H. M. (2022). The fear of COVID-19 Infection in older people. Journal of Geriatric Psychiatry and Neurology, 35(3), 460–466. https://doi.org/10.1177/08919887211002651
Golaszewski, N. M., LaCroix, A. Z., Godino, J. G., Allison, M. A., Manson, J. E., King, J. J., Weitlauf, J. C., Bea, J. W., Garcia, L., Kroenke, C. H., Saquib, N., Cannell, B., Nguyen, S., & Bellettiere, J. (2022). Evaluation of social isolation, loneliness, and cardiovascular disease among older women in the US. JAMA Network Open, 5(2), e2146461–e2146461. https://doi.org/10.1001/jamanetworkopen.2021.46461
Gross, C. R., Kreitzer, M. J., Reilly-Spong, M., Wall, M., Winbush, N. Y., Patterson, R., Mahowald, M., & Cramer-Bornemann, M. (2011). Mindfulness-based stress reduction versus pharmacotherapy for chronic primary insomnia: A randomized controlled clinical trial. EXPLORE, 7(2), 76–87. https://doi.org/10.1016/j.explore.2010.12.003
Grossman, E. S., Hoffman, Y. S. G., Palgi, Y., & Shrira, A. (2021). COVID-19 related loneliness and sleep problems in older adults: Worries and resilience as potential moderators. Personality and Individual Differences, 168(2020), 110371. https://doi.org/10.1016/j.paid.2020.110371
Gutiérrez-Hernández, M. E., Fanjul, L. F., Díaz-Megolla, A., Reyes-Hurtado, P., Herrera-Rodríguez, J. F., del Enjuto-Castellanos, M., & P., & Peñate, W. (2021). COVID-19 Lockdown and mental health in a sample population in Spain: The role of self-compassion. International Journal of Environmental Research and Public Health, 18(4), 2103. https://doi.org/10.3390/ijerph18042103
Haase, C. M. (2013). Developmental Regulation across the Life Span : Toward a New Synthesis., 49(5), 964–972. https://doi.org/10.1037/a0029231
Hartt, M. (2020). COVID-19: A lonely pandemic. Cities & Health, 5(S1), S80–S82. https://doi.org/10.1080/23748834.2020.1788770
Hayes, A. F. (2018). Partial, conditional, and moderated moderated mediation: Quantification, inference, and interpretation. Communication Monographs, 85(1), 4–40. https://doi.org/10.1080/03637751.2017.1352100
Heras, E., Garibaldi, P., Boix, M., Valero, O., Castillo, J., Curbelo, Y., … & Piqué, J. M. (2021). COVID-19 mortality risk factors in older people in a long-term care center. European Geriatric Medicine, 12(3), 601–607. https://doi.org/10.1007/s41999-020-00432-w
Ho, K. H. M., Mak, A. K. P., Chung, R. W. M., Leung, D. Y. L., Chiang, V. C. L., & Cheung, D. S. K. (2022). Implications of COVID-19 on the loneliness of older adults in residential care homes. Qualitative Health Research, 32(2), 279–290. https://doi.org/10.1177/10497323211050910
Hodgetts, J., McLaren, S., Bice, B., & Trezise, A. (2021). The relationships between self-compassion, rumination, and depressive symptoms among older adults: The moderating role of gender. Aging & Mental Health, 25(12), 2337–2346. https://doi.org/10.1080/13607863.2020.1824207
Homan, K. J. (2016). Self-compassion and psychological well-being in older adults. Journal of Adult Development, 23(2), 111–119. https://doi.org/10.1007/s10804-016-9227-8
Hu, L., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal, 6(1), 1–55. https://doi.org/10.1080/10705519909540118
Jarvis, M.-A., Padmanabhanunni, A., Balakrishna, Y., & Chipps, J. (2020). The effectiveness of interventions addressing loneliness in older persons: An umbrella review. International Journal of Africa Nursing Sciences, 12(2019), 100177. https://doi.org/10.1016/j.ijans.2019.100177
Khan, M. S. R., & Kadoya, Y. (2021). Loneliness during the COVID-19 pandemic: A comparison between older and younger people. International Journal of Environmental Research and Public Health, 18(15), 7871. https://doi.org/10.3390/ijerph18157871
Kim, C., & Ko, H. (2018). The impact of self-compassion on mental health, sleep, quality of life and life satisfaction among older adults. Geriatric Nursing, 39(6), 623–628. https://doi.org/10.1016/j.gerinurse.2018.06.005
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Lau, B.H.-P., Chan, C.L.-W., & Ng, S.-M. (2020). Self-compassion buffers the adverse mental health impacts of COVID-19-related threats: Results from a cross-sectional survey at the first peak of Hong Kong’s outbreak. Frontiers in Psychiatry, 11, 585270. https://doi.org/10.3389/fpsyt.2020.585270
Lebrasseur, A., Fortin-Bédard, N., Lettre, J., Raymond, E., Bussières, E.-L., Lapierre, N., Faieta, J., Vincent, C., Duchesne, L., Ouellet, M.-C., Gagnon, E., Tourigny, A., Lamontagne, M. -È., & Routhier, F. (2021). Impact of the COVID-19 pandemic on older adults: Rapid review. JMIR Aging, 4(2), e26474. https://doi.org/10.2196/26474
Lee, S. L., Pearce, E., Ajnakina, O., Johnson, S., Lewis, G., Mann, F., Pitman, A., Solmi, F., Sommerlad, A., Steptoe, A., Tymoszuk, U., & Lewis, G. (2021). The association between loneliness and depressive symptoms among adults aged 50 years and older: A 12-year population-based cohort study. The Lancet Psychiatry, 8(1), 48–57. https://doi.org/10.1016/s2215-0366(20)30383-7
Lin, C.-Y., Broström, A., Griffiths, M. D., & Pakpour, A. H. (2020). Investigating mediated effects of fear of COVID-19 and COVID-19 misunderstanding in the association between problematic social media use, psychological distress, and insomnia. Internet Interventions, 21(March), 100345. https://doi.org/10.1016/j.invent.2020.100345
Lindsay, E. K., Young, S., Brown, K. W., Smyth, J. M., & Creswell, J. D. (2019). Mindfulness training reduces loneliness and increases social contact in a randomized controlled trial. Proceedings of the National Academy of Sciences, 116(9), 3488–3493. https://doi.org/10.1073/pnas.1813588116
Liu, J., Wei, W., Peng, Q., Xue, C., & Yang, S. (2021). The roles of life satisfaction and community recreational facilities in the relationship between loneliness and depression in older adults. Clinical Gerontologist, 45(2), 376–389. https://doi.org/10.1080/07317115.2021.1901166
López, A., Sanderman, R., & Schroevers, M. J. (2018). A close examination of the relationship between self-compassion and depressive symptoms. Mindfulness, 9(5), 1470–1478. https://doi.org/10.1007/s12671-018-0891-6
Lyubomirsky, S., Layous, K., Chancellor, J., & Nelson, S. K. (2015). Thinking about rumination: The scholarly contributions and intellectual legacy of Susan Nolen-Hoeksema. Annual Review of Clinical Psychology, 11(1), 1–22. https://doi.org/10.1146/annurev-clinpsy-032814-112733
Macdonald, B., & Hülür, G. (2021). Well-being and loneliness in swiss older adults during the COVID-19 pandemic: The role of social relationships. The Gerontologist, 61(2), 240–250. https://doi.org/10.1093/geront/gnaa194
Malone, M. L., Hogan, T. M., Perry, A., et al. (2020) COVID-19 in older adults. Key points for emergency department providers. Journal Geriatric Emergency Medicine, 1(4), 1–11. https://gedcollaborative.com/wp-content/uploads/2020/03/JGEM-COVID-19-in-Older-Adults.pdf. Accessed 9 Apr 2020
Manca, R., De Marco, M., & Venneri, A. (2020). The impact of COVID-19 infection and enforced prolonged social isolation on neuropsychiatric symptoms in older adults with and without dementia: A review. Frontiers in Psychiatry, 11, 585540. https://doi.org/10.3389/fpsyt.2020.585540
Marsh, I. C., Chan, S. W. Y., & MacBeth, A. (2018). Self-compassion and psychological distress in adolescents-a meta-analysis. Mindfulness, 9(4), 1011–1027. https://doi.org/10.1007/s12671-017-0850-7
Masi, C. M., Chen, H. Y., Hawkley, L. C., & Cacioppo, J. T. (2011). A meta-analysis of interventions to reduce loneliness. Personality and Social Psychology Review: An Official Journal of the Society for Personality and Social Psychology, Inc, 15(3), 219–266. https://doi.org/10.1177/1088868310377394
Matos, M., McEwan, K., Kanovský, M., Halamová, J., Steindl, S. R., Ferreira, N., Linharelhos, M., Rijo, D., Asano, K., Márquez, M. G., Gregório, S., Vilas, S. P., Brito-Pons, G., Lucena-Santos, P., da Silva Oliveira, M., de Souza, E. L., Llobenes, L., Gumiy, N., Costa, M. I., Habib, N., … &, Gilbert, P. (2022). Compassion protects mental health and social safeness during the COVID-19 pandemic across 21 countries. Mindfulness, 13(4), 863–880. https://doi.org/10.1007/s12671-021-01822-2
Matthews, T., Bryan, B. T., Danese, A., Meehan, A. J., Poulton, R., & Arseneault, L. (2022). Using a loneliness measure to screen for risk of mental health problems: A replication in two nationally representative cohorts. International Journal of Environmental Research and Public Health, 19(3), 1641. https://doi.org/10.3390/ijerph19031641
Mendonça Lima, C. A., De Leo, D., Ivbijaro, G., & Svab, I. (2021). Loneliness and abuse as risk factors for suicide in older adults: New developments and the contribution of the WPA section on old age psychiatry. World Psychiatry, 20(3), 455–456. https://doi.org/10.1002/wps.20899
Mistry, S. K., Ali, A. R. M. M., Akther, F., Yadav, U. N., & Harris, M. F. (2021). Exploring fear of COVID-19 and its correlates among older adults in Bangladesh. Globalization and Health, 17(1), 1–9. https://doi.org/10.1186/s12992-021-00698-0. 47.
Molas-Tuneu, M., Jerez-Roig, J., Minobes-Molina, E., Coll-Planas, L., Escribà-Salvans, A., Farrés-Godayol, P., Yildirim, M., Rierola-Fochs, S., Goutan-Roura, E., Bezerra de Souza, D. L., Skelton, D. A., & Naudó-Molist, J. (2022). Social and emotional loneliness among older people living in nursing homes in Spain: A cross-sectional study. https://doi.org/10.20944/preprints202201.0423.v1
National Academies of Sciences, Engineering, and Medicine (2020). Risk and protective factors for social isolation and loneliness. In Social Isolation and Loneliness in Older Adults: Opportunities for the Health Care System (pp. 63–91). National Academies Press, Washington (DC). Available from: https://www.ncbi.nlm.nih.gov/books/NBK557971/checkSave
Nazari, N., Safitri, S., Usak, M., Arabmarkadeh, A., & Griffiths, M. D. (2021a). Psychometric validation of the Indonesian version of the fear of COVID-19 scale: Personality traits predict the fear of COVID-19. International Journal of Mental Health and Addiction. https://doi.org/10.1007/s11469-021-00593-0
Nazari, N., Zekiy, A. O., Feng, L.-S., & Griffiths, M. D. (2021b). Psychometric validation of the persian version of the COVID-19-related psychological distress scale and association with COVID-19 fear, COVID-19 anxiety, optimism, and lack of resilience. International Journal of Mental Health and Addiction. https://doi.org/10.1007/s11469-021-00540-z
Nazari, N., Hernández, R. M., Ocaña-Fernandez, Y., & Griffiths, M. D. (2022). Psychometric validation of the Persian self-compassion scale youth version. Mindfulness, 13(2), 385–397. https://doi.org/10.1007/s12671-021-01801-7
Neff, K. D. (2003). The development and validation of a scale to measure self-compassion. Self and Identity, 2(3), 223–250. https://doi.org/10.1080/15298860309027
Neff, K. D. (2016). Does self-compassion entail reduced self-judgment, isolation, and over-identification? A response to Muris, Otgaar, and Petrocchi (2016). Mindfulness, 7(3), 791–797. https://doi.org/10.1007/s12671-016-0531-y
Palgi, Y., Shrira, A., Ring, L., Bodner, E., Avidor, S., Bergman, Y., Cohen-Fridel, S., Keisari, S., & Hoffman, Y. (2020). The loneliness pandemic: Loneliness and other concomitants of depression, anxiety and their comorbidity during the COVID-19 outbreak. Journal of Affective Disorders, 275, 109–111. https://doi.org/10.1016/j.jad.2020.06.036
Parlapani, E., Holeva, V., Nikopoulou, V. A., Sereslis, K., Athanasiadou, M., Godosidis, A., Stephanou, T., & Diakogiannis, I. (2020). Intolerance of uncertainty and loneliness in older adults during the COVID-19 pandemic. Frontiers in Psychiatry, 11, 842. https://doi.org/10.3389/fpsyt.2020.00842
Parlapani, E., Holeva, V., Nikopoulou, V. A., Kaprinis, S., Nouskas, I., & Diakogiannis, I. (2021). A review on the COVID-19-related psychological impact on older adults: Vulnerable or not? Aging Clinical and Experimental Research, 33(6), 1729–1743. https://doi.org/10.1007/s40520-021-01873-4
Paul, E., Bu, F., & Fancourt, D. (2021). Loneliness and risk for cardiovascular disease: Mechanisms and future directions. Current Cardiology Reports, 23(6), 68. https://doi.org/10.1007/s11886-021-01495-2
Péterfi, A., Mészáros, Á., Szarvas, Z., Pénzes, M., Fekete, M., Fehér, Á., Lehoczki, A., Csípő, T., & Fazekas-Pongor, V. (2022). Comorbidities and increased mortality of COVID-19 among the elderly: A systematic review. Physiology International. Advance online publication. https://doi.org/10.1556/2060.2022.00206
Raina, P., Wolfson, C., Griffith, L., Kirkland, S., McMillan, J., Basta, N., Joshi, D., Oz, U. E., Sohel, N., Maimon, G., Thompson, M., Costa, A., Anderson, L., Balion, C., Yukiko, A., Cossette, B., Levasseur, M., Hofer, S., Paterson, T., & Hogan, D. (2021). A longitudinal analysis of the impact of the COVID-19 pandemic on the mental health of middle-aged and older adults from the Canadian Longitudinal Study on Aging. Nature Aging, 1(12), 1137–1147. https://doi.org/10.1038/s43587-021-00128-1
Sams, N., Fisher, D. M., Mata-Greve, F., Johnson, M., Pullmann, M. D., Raue, P. J., … Areán, P. A. (2021). Understanding psychological distress and protective factors amongst older adults during the COVID-19 pandemic. American Journal of Geriatric Psychiatry, 29(9): 881–894. https://doi.org/10.1016/j.jagp.2021.03.005
Santini, Z. I., Jose, P. E., York Cornwell, E., Koyanagi, A., Nielsen, L., Hinrichsen, C., Meilstrup, C., Madsen, K. R., & Koushede, V. (2020). Social disconnectedness, perceived isolation, and symptoms of depression and anxiety among older Americans (NSHAP): A longitudinal mediation analysis. The Lancet. Public Health, 5(1), e62–e70. https://doi.org/10.1016/S2468-2667(19)30230-0
Savage, R. D., Wu, W., Li, J., Lawson, A., Bronskill, S. E., Chamberlain, S. A., Grieve, J., Gruneir, A., Reppas-Rindlisbacher, C., Stall, N. M., & Rochon, P. A. (2021). Loneliness among older adults in the community during COVID-19: A cross-sectional survey in Canada. BMJ Open, 11(4), e044517. https://doi.org/10.1136/bmjopen-2020-044517
Savci, C., & Çi̇l akinciA., Yildirim üşenmez, S., & Keleş, F. (2021). The effects of fear of COVID-19, loneliness, and resilience on the quality of life in older adults living in a nursing home. Geriatric Nursing, 42(6), 1422–1428. https://doi.org/10.1016/j.gerinurse.2021.09.012
Schnepper, R., Reichenberger, J., & Blechert, J. (2020). Being my own companion in times of social isolation – A 14-day mobile self-compassion intervention improves stress levels and eating behavior. Frontiers in Psychology, 11, 595806. https://doi.org/10.3389/fpsyg.2020.595806
Sha, S., Xu, Y., & Chen, L. (2020). Loneliness as a risk factor for frailty transition among older Chinese people. BMC Geriatrics, 20, 300. https://doi.org/10.1186/s12877-020-01714-5
Sharma, A. (2021). Estimating older adult mortality from COVID-19. The Journals of Gerontology: Series B, Psychological Sciences and Social Sciences, 76(3), e68–e74. https://doi.org/10.1093/geronb/gbaa161
Siegmund, L. A., Distelhorst, K., Bena, J., & Morrison, S. (2021). Relationships between physical activity, social isolation, and depression among older adults during COVID-19: A path analysis. Geriatric Nursing, 42(5), 1240–1244. https://doi.org/10.1016/j.gerinurse.2021.08.012
Sloan, E., Hall, K., Moulding, R., Bryce, S., Mildred, H., & Staiger, P. K. (2017). Emotion regulation as a transdiagnostic treatment construct across anxiety, depression, substance, eating and borderline personality disorders: A systematic review. Clinical Psychology Review, 57, 141–163. https://doi.org/10.1016/j.cpr.2017.09.002
Smith, J. L. (2015). Self-compassion and resilience in senior living residents. Seniors Housing & Care Journal, 23(1), 16–32.
Stokes, E. K., Zambrano, L., Anderson, K., Marder, E., & Raz, K. (2020). Coronavirus disease 2019 case surveillance — United States, January 22–May 30, 2020. MMWR. Morbidity and Mortality Weekly Report, 69, 759–765. https://doi.org/10.15585/mmwr.mm6924e2external
Tabachnick, B. G., & Fidell, L. S. (2018). Using multivariate statistics, 7th edn. Pearson India Education Services Pvt. Ltd, Uttar Pradesh, India.
Tavares, L. R., Vagos, P., & Xavier, A. (2020). The role of self-compassion in the psychological (mal)adjustment of older adults: A scoping review. International Psychogeriatrics, 1–14. Advance online publication. https://doi.org/10.1017/s1041610220001222
Tesky, V. A., Schall, A., Schulze, U., Stangier, U., Oswald, F., Knopf, M., König, J., Blettner, M., Arens, E., & Pantel, J. (2019). Depression in the nursing home: A cluster-randomized stepped-wedge study to probe the effectiveness of a novel case management approach to improve treatment (the DAVOS project). Trials, 20(1), 424. https://doi.org/10.1186/s13063-019-3534-x
Trybusińska, D., & Saracen, A. (2019). Loneliness in the context of quality of life of nursing home residents. Open Medicine, 14(1), 354–361. https://doi.org/10.1515/med-2019-0035
Tyrrell, C. J., & Williams, K. N. (2020). The paradox of social distancing: Implications for older adults in the context of COVID-19. Psychological Trauma: Theory, Research, Practice, and Policy, 12(S1), S214–S216. https://doi.org/10.1037/tra0000845
Vahia, V. N., & Shah, A. B. (2020). COVID-19 pandemic and mental health care of older adults in India. International Psychogeriatrics, 32(10), 1125–1127. https://doi.org/10.1017/s1041610220001441
Van Orden, K. A., Bower, E., Lutz, J., Silva, C., Gallegos, A. M., Podgorski, C. A., Santos, E. J., & Conwell, Y. (2021). Strategies to promote social connections among older adults during “Social distancing” restrictions. The American Journal of Geriatric Psychiatry: Official Journal of the American Association for Geriatric Psychiatry, 29(8), 816–827. https://doi.org/10.1016/j.jagp.2020.05.004
Van Tilburg, T. G., Steinmetz, S., Stolte, E., Van Der Roest, H., & De Vries, D. H. (2021). Loneliness and mental health during the COVID-19 pandemic: A study among dutch older adults. The Journals of Gerontology - Series B Psychological Sciences and Social Sciences, 76(7), E249–E255. https://doi.org/10.1093/geronb/gbaa111
Vandekerckhove, M., & Wang, Y. L. (2017). Emotion, emotion regulation and sleep: An intimate relationship. AIMS Neuroscience, 5(1), 1–17. https://doi.org/10.3934/Neuroscience.2018.1.1
Verbiest, M. E. A., Stoop, A., Scheffelaar, A., Janssen, M. M., van Boekel, L. C., & Luijkx, K. G. (2022). Health impact of the first and second wave of COVID-19 and related restrictive measures among nursing home residents: A scoping review. BMC Health Services Research, 22(1), 921. https://doi.org/10.1186/s12913-022-08186-w
Wang, F., Liu, S., Zhang, Q., Ng, C. H., Cui, X., Zhang, D., & Xiang, Y.-T. (2021). Prevalence of depression in older nursing home residents in high and low altitude regions: A comparative study. Frontiers in Psychiatry, 12, 669234. https://doi.org/10.3389/fpsyt.2021.669234
Wynants, L., Van Calster, B., Bonten, M. M. J., Collins, G. S., Debray, T. P. A., De Vos, M., Haller, M. C., Heinze, G., Moons, K. G. M., Riley, R. D., Schuit, E., Smits, L. J. M., Snell, K. I. E., Steyerberg, E. W., Wallisch, C., & van Smeden, M. (2020). Prediction models for diagnosis and prognosis of covid-19 infection: systematic review and critical appraisal. BMJ, 369, m1328. https://doi.org/10.1136/bmj.m1328
Yadav, U. N., Yadav, O. P., Singh, D. R., Ghimire, S., Rayamajhee, B., KantiMistry, S., Rawal, L. B., Ali, A. M., Kumar Tamang, M., & Mehta, S. (2021). Perceived fear of COVID-19 and its associated factors among Nepalese older adults in eastern Nepal: A cross-sectional study. PLOS ONE, 16(7), e0254825. https://doi.org/10.1371/journal.pone.0254825
Yao, N., Nazari, N., Veiskarami, H. A., & Griffiths, M. D. (2022). The role of healthy emotionality in the relationship between fear of COVID-19 and mental health problems: A cross-sectional study. Cognitive Processing, 23(4), 569–581. https://doi.org/10.1007/s10339-022-01101-5
Yat, S., Li, H., & Bressington, D. (2019). The effects of mindfulness-based stress reduction on depression, anxiety, and stress in older adults: A systematic review and meta-analysis. International Journal Mental Health Nursing, 28(3), 635–656. https://doi.org/10.1111/inm.12568
Yu, B., Steptoe, A., Chen, Y., & Jia, X. (2020). Social isolation, rather than loneliness, is associated with cognitive decline in older adults: The China Health and Retirement Longitudinal Study. Psychological Medicine, 51(14), 2414–2421. https://doi.org/10.1017/s0033291720001014
Yu, J., & Mahendran, R. (2021). COVID-19 lockdown has altered the dynamics between affective symptoms and social isolation among older adults: Results from a longitudinal network analysis. Scientific Reports, 11(1), 14739. https://doi.org/10.1038/s41598-021-94301-6
Zenebe, Y., Akele, B., & W, Selassie, M., & Necho, M. (2021). Prevalence and determinants of depression among old age: A systematic review and meta-analysis. Annals of General Psychiatry, 20, 55. https://doi.org/10.1186/s12991-021-00375-x
Zessin, U., Dickhäuser, O., & Garbade, S. (2015). The relationship between self-compassion and well-being: A meta-analysis. Applied Psychology: Health and Well-Being, 7(3), 340–364. https://doi.org/10.1111/aphw.12051
Zhang, C., Xiao, S., Lin, H., Shi, L., Zheng, X., Xue, Y., Dong, F., Zhang, J., & Xue, B. (2022). The association between sleep quality and psychological distress among older Chinese adults: A moderated mediation model. BMC Geriatrics, 22(1), 35. https://doi.org/10.1186/s12877-021-02711-y
Zhao, M., Gao, J., Li, M., & Wang, K. (2019). Relationship between loneliness and frailty among older adults in nursing homes: The mediating role of activity engagement. Journal of the American Medical Directors Association, 20(6), 759–764. https://doi.org/10.1016/j.jamda.2018.11.007
Funding
This study is supported by research on the pricing mechanism of institutional elderly care services in China (17BGL151).
Author information
Authors and Affiliations
Contributions
N.N: Conceptualization, Methodology, Writing—Original draft preparation. P.G: writing—original draft preparation, writing—revision draft preparation, funding acquisition. H.M: investigation, data collection, coordination; all authors: writing—reviewing and editing final draft.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
This study was adhered to the STROBE checklist and was found to follow the ethical principles of the Helsinki Declaration. The study, including all assessments and procedures, was reviewed by the East China Normal University Institutional Human Research Ethics Committee (Research Proposal No.219152510). All the participants provided signed informed consent.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gao, P., Mosazadeh, H. & Nazari, N. The Buffering Role of Self-compassion in the Association Between Loneliness with Depressive Symptoms: A Cross-Sectional Survey Study Among Older Adults Living in Residential Care Homes During COVID-19. Int J Ment Health Addiction (2023). https://doi.org/10.1007/s11469-023-01014-0
Accepted:
Published:
DOI: https://doi.org/10.1007/s11469-023-01014-0