Abstract
Purpose
The purpose of this study is to test the effects of a mild degree of head-of-bed elevation (HOBE) (7.5°) on obstructive sleep apnea (OSA) severity and sleep quality.
Methods
OSA patients were recruited from a single sleep clinic (Criciúma, Santa Catarina, Brazil). Following a baseline polysomnography (PSG), all patients underwent a PSG with HOBE (within 2 weeks). In addition, a subset of patients performed a third PSG without HOBE.
Results
Fifty-two patients were included in the study (age 53.2 ± 9.1 years; BMI 29.6 ± 4.8 kg/m2, neck circumference 38.9 ± 3.8 cm, and Epworth Sleepiness Scale 15 ± 7). Compared to baseline, HOBE significantly decreased the apnea-hypopnea index (AHI) from 15.7 [11.3–22.5] to 10.7 [6.6–16.5] events/h; p < 0.001 and increased minimum oxygen saturation from 83.5 [77.5–87] to 87 [81–90]%; p = 0.003. The sleep architecture at baseline and HOBE were similar. However, sleep efficiency increased slightly but significantly with HOBE (87.2 [76.7–90.7] vs 88.8 [81.6–93.3]; p = 0.005). The AHI obtained at the third PSG without HOBE (n = 7) returned to baseline values.
Conclusions
Mild HOBE significantly improves OSA severity without interfering in sleep architecture and therefore is a simple alternative treatment to ameliorate OSA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea (OSA) is a common disorder characterized by repetitive partial or complete obstruction of the upper airway during sleep [1,2,3]. The pathophysiology of OSA is complex and is caused by the interplay of both anatomical and non-anatomical factors including neuromuscular responsiveness, ventilatory instability, and arousal threshold [3]. Continuous positive airway pressure (CPAP) is the most common treatment for OSA. However, CPAP adherence is not ideal and may be even worse among subjects with milder forms of OSA [4, 5].
Alternative options for OSA treatment include oral appliances, upper airway surgery, oropharyngeal exercises, and positional therapy [6,7,8,9,10,11,12]. Head-of-bed elevation (HOBE) has been shown to effectively reduce OSA severity in small studies [13, 14]. However, HOBE was aggressive and ranged from 30° to 60°, making this approach difficult to be tolerated in clinical practice [13,14,15,16]. The evidence that HOBE may be useful to treat OSA also comes from physiological studies showing that HOBE decreases upper airway collapsibility and increases upper airway area as compared to supine position [13,14,15,16]. Mild HOBE is widely accepted to treat gastroesophageal reflux [17]. Therefore, mild HOBE may be an attractive and low-cost option to treat OSA either alone or in combination with other therapies. However, there is very little evidence to support HOBE effectiveness in clinical practice. We hypothesized that a mild HOBE (7.5°) will significantly improve OSA without interfering on sleep architecture and efficiency. In order to test these hypotheses, we studied patients with OSA by full polysomnography (PSG) without (baseline) and with HOBE.
Methods
Subjects
Men and women aged between 18 and 75 years were recruited from a sleep clinic in Criciúma, Santa Catarina, Brazil. Subjects with a body mass index (BMI) > 40 kg/m2, a previous diagnosis of heart failure, renal failure, and uncontrolled respiratory or neurological disease, and a baseline PSG showing an apnea-hypopnea index <5 events/h were excluded. The study was approved by the Hospital São José Ethics Committee, Criciúma, Santa Catarina, Brazil (protocol 167/2010). Written informed consent was obtained from all patients before any study procedure. The trial was registered at clinicaltrials.gov (NCT02088723).
Polysomnography
Polysomnographic recordings were performed using an Alice 5® polysomnography system (Philips Respironics) and comprised of electroencephalogram derivations (F4/M1, C4/M1, O2/M1, F3/M2, C3/M2, O1/M2), electrooculogram, submental and anterior tibialis electromyogram, and electrocardiogram. Airflow was monitored using an oronasal thermistor and a nasal pressure cannula. Thoracic and abdominal movements were registered using inductive plethysmography belts. Body position and oxygen saturation oximetry were also recorded. The studies were manually scored according to the latest American Academy of Sleep Medicine scoring manual [18]. Apnea was defined as a reduction of ≥90% of the oronasal thermistor flow amplitude for ≥10 s. Hypopnea was defined as the reduction ≥30% of nasal pressure flow amplitude for ≥10 s in association with either ≥3% arterial oxygen desaturation or an arousal [18]. Mild, moderate, and severe OSA was classified according to standard criteria (5–14.9, 15–30, >30 events/h, respectively) [19].
Study design
All patients were evaluated by a clinical interview and Epworth Sleepiness Scale (ESS) questionnaire was applied. A baseline diagnostic polysomnography was performed followed by a polysomnography with HOBE within 2 weeks. The laboratory bed was 2.10 m long and the mattress was at 0.6 m from the floor. A 15-cm-high piece of wood under the head-of-bed legs was used, resulting in a tilt of 7.5°. Because this was not a randomized trial, a third polysomnography without HOBE was performed within the subsequent 2 weeks in a subset of patients in order to exclude that the possible differences in OSA severity between baseline and intervention were not due to random variability.
Statistical analysis
Statistical analysis was performed using SPSS version 20.0. G Power version 3.0.10 was used for power calculations and α˂0.05 was considered significant. The Shapiro-Wilk test was used to test for normal distribution. Paired t test or Wilcoxon signed-rank test was used to compare baseline and HOBE data as appropriate. Sample size was calculated expecting a 30% decrease in the AHI after HOBE. A beta of 0.85 and alpha of 0.05 were used and 52 patients were necessary. A repeated measurement ANOVA was performed to test for the difference between the three polysomnographies in the subset of patients that underwent a third PSG without bed elevation. A post-hoc analysis (Tukey’s) was done to test for differences between polysomnographies. A positive response was defined as ≥50% reduction in AHI or AHI < 5 events/h during intervention. A partial response was defined as a decrease in AHI between 25 and 50%. A negative response was defined as <25% AHI reduction.
Results
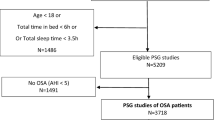
Sixty-two patients were initially evaluated. Ten patients were excluded because of concomitant chronic obstructive pulmonary disease (n = 6), BMI > 40 kg/m2 (n = 2) and two patients did not agree to participate. Therefore, 52 patients were included in the study. The time lag between the baseline and HOBE PSG was 8.9 ± 2.1 days. A subset of seven patients performed a third PSG without HOBE (9.7 ± 2.6 days after the HOBE PSG) (Fig. 1). The sample consisted of middle aged (53.2 ± 9.1 years) men and women (25 women) that were on average overweight (BMI 29.6 ± 4.8 kg/m2, neck circumference 38.9 ± 3.8 cm) with symptoms of excessive daytime sleepiness (EES 14.7 ± 6.9). Patients had, on average, moderate OSA at baseline PSG with an AHI ranging from 5.3 to 44.8 events/h. Twenty, 28, and 4 patients presented mild, moderate, and severe OSA, respectively. The median AHI in baseline PSG was 10.6 [7.6–12.1] events/h in mild, 17.6 [15.7–23.3] events/h in moderate, and 39.4 [36.8–42.4] events/h in severe OSA patients. Table 1 shows the sleep characteristics during baseline and HOBE PSG. HOBE did not promote any significant differences in sleep stages, arousal index (ArI), total sleep time (TST), or time in supine position. Although HOBE was associated with an increase in sleep efficiency (from 87.2% [76.7–90.7] to 88.8% [81.6–93.3], p = 0.005), the mean increase was 83.4 ± 9.2 to 91.4 ± 31.6, and this does not appear to be clinically relevant.
There was on average a 31.8% reduction in AHI during HOBE. HOBE significantly decreased AHI from 15.7 [11.3–22.5] to 10.7 [6.6–16.5] events/h (p < 0.001). HOBE promoted a greater reduction in the supine AHI (from 20.5 [10.0–33.2] to 11.3 [5.7–34.5] events/h, p = 0.023).The individual values of AHI at baseline and HOBE PSG can be observed in Fig. 2. Minimum oxygen saturation increased significantly during HOBE from 83.5 [77.5–87] to 87 [81–90]% (p = 0.003). HOBE was most effective to reduce hypopneas (from 12.9 [8.6–15.4] to 6.8 [3.7–11.3] events/h, p = 0.001) (Table 1).
Thirteen patients out of 52 patients (25%) presented positional OSA (defined as an AHI at lateral position less than 50% of the AHI at supine position). Among the 13 patients showing positional OSA during baseline PSG, 9 maintained positional OSA with HOBE. Apnea-hypopnea index of the 13 positional OSA patients at the baseline polysomnography (11.9 [10.4–14.3] events/h) did not reduce significantly during HOBE (9.0 [4.6–9.9] events/h), p = 0.174.
Thirty-two patients (61.5%) were classified as responders to HOBE (9 patients presented a positive response and 23 patients presented a partial response). In contrast, 20 patients (38.4%) did not respond to HOBE. Among the 7 subjects that underwent a third polysomnography without HOBE, the AHI during the third (22.0 ± 13.6 events/h) and baseline (20.8 ± 10.7events/h) PSGs was similar (p = 0.304) but was significantly higher than during the HOBE night (14.0 ± 9.1 events/h) p = 0.005.
Discussion
The major finding of the current study was that a mild degree of HOBE (7.5°) was able to reduce OSA severity by 31.8% on average among patients with predominantly mild to moderate OSA. HOBE had the largest impact in reducing hypopneas (47.3%) and supine-dependent respiratory events (44.9%). We believed that HOBE would reduce sleep efficiency because of some postural discomfort or falling sensation, but this did not occur. HOBE was associated with an increase in sleep efficiency, although this does not appear to be clinically relevant. HOBE may be a simple alternative treatment option for patients with mild to moderate OSA.
The findings of the present study are in line with previous reported small case series. For instance, McEvoy et al. studied 13 male patients during the same night and reported a reduction from 49 ± 5 to 20 ± 7 events/h from supine to sitting position at 60° [13]. Although the authors reported a greater decrease in AHI than in our study, the clinical applicability is limited because patients usually do not tolerate sleeping in the sitting position for prolonged periods. Skinner et al. reported a 22% reduction in AHI in 14 patients with a wide range of OSA severity when sleeping with a shoulder-head elevation pillow [20]. Our study extends these previous findings in a larger sample with clinical applicability by showing a 31.8% reduction in median AHI among patients with predominantly mild to moderate OSA using a HOBE of 7.5°. HOBE was obtained with a 15-cm wedge (5.9 in.). Similar elevation has been shown to be well tolerated and used in studies on gastroesophageal reflux disease [17]. The magnitude of reduction in AHI observed in the present study with HOBE (32%) is similar to that of other non-CPAP alternatives previously reported such as postural position therapy (46%) [21], oropharyngeal exercises (39%) [8], and compression stockings (36%) [22].
The pathophysiology of OSA is complex, may vary from patient to patient, and involves anatomical and non-anatomical components, such as respiratory control stability. The predominant control of hypopneas observed in our study is consistent with other alternative non-CPAP treatments for OSA [23,24,25]. Similar effects have been observed in therapeutic approaches that act on the respiratory control stability such as acetazolamide [23], dead space, and supplemental oxygen [24] as well as on the mechanical component of OSA such as the instillation of surfactant [25]. Two independent studies reported a significant reduction in pharyngeal critical closing pressure (Pcrit) with HOBE, indicating a protective effect by acting on the anatomical component of OSA. Neill AM et al. showed a significant reduction in Pcrit between natural sleep in the supine position and during 30° HOBE (0.3 ± 2.4 to −4.0 ± 3.2 cmH2O, respectively) [14]. In a second study, nine patients studied under general anesthesia with propofol and vecuronium, Pcrit also decreased from the supine to the sitting position at 62° 2.2 (0.84–6.12) to −3.5 (−8.51– −1.32) cmH2O, respectively [16]. In line with the physiological research, one study showed a significant increase in the mean upper airway volume (evaluated by cervical computed tomography) from the supine to the head elevation position with 44° (40.35 ± 16.43 vs 48.31 ± 16.21 cm3, respectively) [26]. HOBE may alleviate the force of gravity on the pharyngeal structures, especially the tongue. The tongue defines the anterior pharyngeal wall which is particularly susceptible to narrowing while sleeping supine [14, 16, 26, 27]. HOBE may also stabilize the upper airway by preventing rostral fluid shift during sleep, a mechanism that may contribute to upper airway obstruction not only in patients with edematous states, but also in typical OSA patients [28].
HOBE is very easy to be applied and well tolerated. HOBE could be a simple measure for patients that are waiting for OSA therapy, such as mandibular advanced device or surgery. HOBE could also be used in combination with other interventions such as oral appliance, oropharyngeal exercises, and weight loss in future studies. HOBE has also the potential of providing a better compliance than other alternative therapies for OSA such as oropharyngeal exercises and positional therapy. For instance, avoiding supine position with tennis ball therapy showed that the long-term patient compliance is poor, with less than 10% of adherence [29].
Our study has several potential limitations. Firstly, this was not a randomized study, and therefore, it is not possible to exclude the impact of difficult to control variables such as the first night PSG effect. However, in a small subgroup of patients that performed a third PSG with no HOBE, it clearly showed a return of OSA severity to the baseline levels. Secondly, one may argue that the effect of HOBE on OSA severity was mild and that a higher degree of bed elevation could be more effective in reducing OSA severity. The elevation adopted in our study was a compromise between effectiveness and comfort. A pilot study (data not shown) showed that patients did not tolerate sleeping with a 20-cm wedge because of sensation of falling. We therefore adopted a bed angulation that is well described in patients with gastroesophageal reflux. Thirdly, the majority of our patients had only mild to moderate OSA, and the effects were more pronounced in reducing hypopneas than apneas. Therefore, the effects of HOBE are more likely to be less evident in patients with severe OSA. Fourthly, HOBE may be contra indicated in patients with specific conditions such as lower limb edema and venous insufficiency.
Conclusions
HOBE is a simple measure that significantly improves OSA severity without compromising the sleep architecture. This positional intervention reduces AHI and has better effects in hypopnea index and supine AHI. Due its simplicity and low cost, HOBE can be an attractive alternative treatment for OSA.
References
Young T, Peppard PE, Gottleb DJ (2002) Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 165:1217–1239
Tufik S, Santos-Silva R, Taddei JA, Bittencourt LR (2010) Obstructive sleep apnea syndrome in the Sao Paulo Epidemiologic Sleep Study. Sleep Med 11:441–446
Eckert DS, White DP, Jorda AS, Malhotra A, Wellman A (2013) Defining phenotypic causes of obstructive sleep apnea. Identification of novel therapeutic targets. Am J Respir Crit Care Med 188:996–1004
Kribbs NB, Pack AI, Kline LR, Pack AI, Kline LR, Smith PL, Schwartz AR, Schubert NM, Redline S, Henry JN, Getsy JE, Dinges DF (1993) Objective measurement of patterns of nasal CPAP use by patients with obstructive sleep apnea. Am Rev Respir Dis 147:887–895
Bartlett D, Wong K, Richards D, Moy E, Espie CA, Cistulli PA, Grunstein R (2013) Increasing adherence to obstructive sleep apnea treatment with a group social cognitive therapy treatment intervention: a randomized trial. Sleep 36:1647–1654
Bixler EO, Vgontzas AN, Ten Have T, Tyson K, Kales A (1998) Effects of age on sleep apnea in men: I. Prevalence and severity. Am J Respir Crit Care Med 157:144–148
White DP (2006) Sleep apnea. Proc Am Thorac Soc 3:124–128
Guimaraes KC, Drager LF, Genta PR, Marcondes BF, Lorenzi-Filho G (2009) Effects of oropharyngeal exercises on patients with moderate obstructive sleep apnea syndrome. Am J Respir Crit Care Med 179:962–966
Meen EK, Chandra RK (2013) The role of the nose in sleep-disordered breathing. Am J Rhinol Allergy 27:213–220
Oksenberg A, Gadoth N (2014) Are we missing a simple treatment for most adult sleep apnea patients? The avoidance of the supine sleep position. J Sleep Res 23:204–210
Ravesloot MJ, van Maanen JP, Dun L, de Vries N (2013) The undervalued potential of positional therapy in position-dependent snoring and obstructive sleep apnea-a review of the literature. Sleep Breath 17:39–49
Hoekema A (2006) Efficacy and comorbidity of oral appliances in the treatment of obstructive sleep apnea-hypopnea: a systematic review and preliminary results of a randomized trial. Sleep Breath 10:102–103
McEvoy RD, Sharp DJ, Thornton AT (1986) The effects of posture on obstructive sleep apnea. Am Rev Respir Dis 133:662–666
Neill AM, Angus SM, Sajkov D, McEvoy RD (1997) Effects of sleep posture on upper airway stability in patients with obstructive sleep apnea. Am J Respir Crit Care Med 155:199–204
Martin SE, Marshall I, Douglas NJ (1995) The effect of posture on airway caliber with the sleep-apnea/hypopnea syndrome. Am J Respir Crit Care Med 152:721–724
Tagaito Y, Isono S, Tanaka A, Ishikawa T, Nishino T (2010) Sitting posture decreases collapsibility of the passive pharynx in anesthetized paralyzed patients with obstructive sleep apnea. Anesthesiology 113:812–818
Kaltenbach T, Crockett S, Gerson LB (2006) Are lifestyle measures effective in patients with gastroesophageal reflux disease? An evidence-based approach. Arch Intern Med 166:965–971
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Epstein LJ, Kristo D, Strollo PJ Jr, Friedman N, Malhotra A, Patil SP, Ramar K, Rogers R, Schwab RJ, Weaver EM, Weinstein MD, Adult Obstructive Sleep Apnea Task Force of the American Academy of Sleep Medicine (2009) Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J Clin Sleep Med 5:263–276
Skinner MA, Kingshott RN, Jones DR, Homan SD, Taylor DR (2004) Elevated posture for the management of obstructive sleep apnea. Sleep Breath 8:193–200
Jackson M, Collins A, Berlowitz D, Howard M, O’Donoghue F, Barnes M (2015) Efficacy of sleep position modification to treat positional obstructive sleep apnea. Sleep Med 16:545–552
Redolfi S, Arnulf I, Pottier M, Lajou J, Koskas I, Bradley TD, Similowski T (2011) Attenuation of obstructive sleep apnea by compression stockings in subjects with venous insufficiency. Am J Respir Crit Care Med 184:1062–1066
Edwards BA, Sands SA, Eckert DJ, White DP, Butler JP, Owens RL, Malhotra WA (2012) Acetazolamide improves loop gain but not the other physiological traits causing obstructive sleep apnoea. J Physiol 590:1199–1211
Xie A, Teodorescu M, Pegelow DF, Teodorescu MC, Gong Y, Fedie JE, Dempsey JA (1985) Effects of stabilizing or increasing respiratory motor outputs on obstructive sleep apnea. J Appl Physiol 115:22–33
Kirkness JP, Madronio M, Stavrinou R, Wheatley JR, Amis TC (2003) Relationship between surface tension of upper airway lining liquid and upper airway collapsibility during sleep in obstructive sleep apnea hypopnea syndrome. J Appl Physiol 95:1761–1766
Souza FJ, Evangelista AR, Silva JV, Périco GV, Madeira K (2016) Cervical computed tomography in patients with obstructive sleep apnea: influence of head elevation on the assessment of upper airway volume. J Bras Pneumol 42:55–60
Lee CH, Kim DK, Kim SY, Rhee CS, Won TB (2015) Changes in site of obstruction in obstructive sleep apnea patients according to sleep position: a DISE study. Laryngoscope 125:248–254
Redolfi S, Yumino D, Ruttanaumpawan P, Yau B, Su MC, Lam J, Bradley TD (2009) Relationship between overnight rostral fluid shift and obstructive sleep apnea in nonobese men. Am J Respir Crit Care Med 179:241–246
Bignold JJ, Deans-Costi G, Goldsworthy MR, Robertson CA, McEvoy D, Catcheside PG, Mercer JD (2009) Poor long-term patient compliance with the tennis ball technique for treating positional obstructive sleep apnea. J Clin Sleep Med 5:428–430
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research. Dr. Geraldo Lorenzi Filho and Pedro Rodrigues Genta were supported by FAPESP.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Souza, F.J.F., Genta, P.R., de Souza Filho, A.J. et al. The influence of head-of-bed elevation in patients with obstructive sleep apnea. Sleep Breath 21, 815–820 (2017). https://doi.org/10.1007/s11325-017-1524-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1524-3