Abstract
Purpose
To examine whether the machine learning (ML) analyses using clinical and pretreatment 2-deoxy-2-[18F]fluoro-d-glucose positron emission tomography ([18F]-FDG-PET)–based radiomic features were useful for predicting prognosis in patients with hypopharyngeal cancer.
Procedures
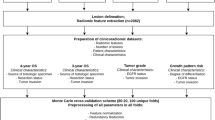
This retrospective study included 100 patients with hypopharyngeal cancer who underwent [18F]-FDG-PET/X-ray computed tomography (CT) before treatment, and these patients were allocated to the training (n=80) and validation (n=20) cohorts. Eight clinical (age, sex, histology, T stage, N stage, M stage, UICC stage, and treatment) and 40 [18F]-FDG-PET–based radiomic features were used to predict disease progression. A feature reduction procedure based on the decrease of the Gini impurity was applied. Six ML algorithms (random forest, neural network, k-nearest neighbors, naïve Bayes, logistic regression, and support vector machine) were compared using the area under the receiver operating characteristic curve (AUC). Progression-free survival (PFS) was assessed using Cox regression analysis.
Results
The five most important features for predicting disease progression were UICC stage, N stage, gray level co-occurrence matrix entropy (GLCM_Entropy), gray level run length matrix run length non-uniformity (GLRLM_RLNU), and T stage. Patients who experienced disease progression displayed significantly higher UICC stage, N stage, GLCM_Entropy, GLRLM_RLNU, and T stage than those without progression (each, p<0.001). In both cohorts, the logistic regression model constructed by these 5 features was the best performing classifier (training: AUC=0.860, accuracy=0.800; validation: AUC=0.803, accuracy=0.700). In the logistic regression model, 5-year PFS was significantly higher in patients with predicted non-progression than those with predicted progression (75.8% vs. 8.3%, p<0.001), and this model was only the independent factor for PFS in multivariate analysis (hazard ratio = 3.22; 95% confidence interval = 1.03–10.11; p=0.045).
Conclusions
The logistic regression model constructed by UICC, T and N stages and pretreatment [18F]-FDG-PET–based radiomic features, GLCM_Entropy, and GLRLM_RLNU may be the most important predictor of prognosis in patients with hypopharyngeal cancer.



Similar content being viewed by others
References
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ (2009) Cancer statistics. CA Cancer J Clin 59:225–249
Kuo P, Chen MM, Decker RH, Yarbrough WG, Judson BL (2014) Hypopharyngeal cancer incidence, treatment, and survival: temporal trends in the United States. Laryngoscope 124:2064–2069
Deschler DG, Day T (2008) TNM Staging of head and neck cancer and neck dissection classification. American Academy of Otolaryngology–Head and Neck Surgery Foundation, Alexandria, pp 10–23
Bar-Ad V, Palmer J, Yang H et al (2014) Current management of locally advanced head and neck cancer: the combination of chemotherapy with locoregional treatments. Semin Oncol 41:798–806
Garneau JC, Bakst RL, Miles BA (2018) Hypopharyngeal cancer: a state of the art review. Oral Oncol 86:244–250
Hamoir M, Schmitz S, Suarez C et al (2018) The current role of salvage surgery in recurrent head and neck squamous cell carcinoma. Cancers (Basel) 10:267
Forastiere AA, Adelstein DJ, Manola J (2013) Induction chemotherapy meta-analysis in head and neck cancer: right answer, wrong question. J Clin Oncol 31:2844–2846
Beitler JJ, Zhang Q, Fu KK et al (2014) Final results of local-regional control and late toxicity of RTOG 9003: a randomized trial of altered fractionation radiation for locally advanced head and neck cancer. Int J Radiat Oncol Biol Phys 89:13–20
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: images are more than pictures, they are data. Radiology 278:563–577
von Schulthess GK, Steinert HC, Hany TF (2006) Integrated PET/CT: current applications and future directions. Radiology 238:405–422
Wong CK, Chan SC, Ng SH et al (2019) Textural features on 18F-FDG PET/CT and dynamic contrast-enhanced MR imaging for predicting treatment response and survival of patients with hypopharyngeal carcinoma. Med (Baltimore) 98:e16608
Chen SW, Shen WC, Lin YC et al (2017) Correlation of pretreatment 18 F-FDG PET tumor textural features with gene expression in pharyngeal cancer and implications for radiotherapy-based treatment outcomes. Eur J Nucl Med Mol Imaging 44:567–580
Erickson BJ, Korfiatis P, Akkus Z, Kline TL (2017) Machine learning for medical imaging. RadioGraphics 37:505–515
Waljee AK, Higgins PD (2010) Machine learning in medicine: a primer for physicians. Am J Gastroenterol 105:1224–1226
Hyun SH, Ahn MS, Koh YW, Lee SJ (2019) A machine-learning approach using PET-based radiomics to predict the histological subtypes of lung cancer. Clin Nucl Med 44:956–960
Nakajo M, Jinguji M, Tani A et al (2021) Application of a machine learning approach for the analysis of clinical and radiomic features of pretreatment [18 F]-FDG PET/CT to Predict Prognosis of Patients with Endometrial Cancer. Mol Imaging Biol 23:756–765
Zhong J, Frood R, Brown P et al (2021) Machine learning-based FDG PET-CT radiomics for outcome prediction in larynx and hypopharynx squamous cell carcinoma. Clin Radiol 76:78.e9–78.e17
Nioche C, Orlhac F, Boughdad S et al (2018) LIFEx: a freeware for radiomic feature calculation in multimodality imaging to accelerate advances in the characterization of tumor heterogeneity. Cancer Res 78:4786–4789
Brown PJ, Zhong J, Frood R et al (2019) Prediction of outcome in anal squamous cell carcinoma using radiomic feature analysis of pre-treatment FDG PET-CT. Eur J Nucl Med Mol Imaging 46:2790–2799
Johnson WE, Li C, Rabinovic A (2007) Adjusting batch effects in microarray expression data using empirical Bayes methods. Biostatistics 8:118–127
Orlhac F, Boughdad S, Philippe C et al (2018) A postreconstruction harmonization method for multicenter radiomic studies in PET. J Nucl Med 59:1321–1328
Koyasu S, Nakamoto Y, Kikuchi M et al (2014) Prognostic value of pretreatment 18F-FDG PET/CT parameters including visual evaluation in patients with head and neck squamous cell carcinoma. AJR Am J Roentgenol 202:851–858
Breiman L (2001) Random forests. Mach Learn 45:5–32
Rahman R, Kodesh A, Levine SZ, Sandin S, Reichenberg A, Schlessinger A (2020) Identification of newborns at risk for autism using electronic medical records and machine learning. Eur Psychiatry 63:e22
Hotta M, Minamimoto R, Miwa K (2019) 11C-methionine-PET for differentiating recurrent brain tumor from radiation necrosis: radiomics approach with random forest classifier. Sci Rep 9:15666
Sian H, Purnami SW (2015) Combine sampling support vector machine for imbalanced data classification. Procedia Comput Sci 72:59–66
Xie Y, Jiang B, Gong E et al (2019) Use of gradient boosting machine learning to predict patient outcome in acute ischemic stroke on the basis of imaging, demographic, and clinical information. AJR Am J Roentgenol 212:44–51
Cook JA, Ranstam J (2016) Overfitting. Br J Surg 103:1814
Demsar J, Curk T, Erjavec A et al (2013) Orange: data mining toolbox in Python. J Mach Learn Res 14:2349–2353
Lausen B, Schumacher M (1992) Maximally selected rank statistics. Biometrics 48:73–85
Ha S, Choi H, Paeng JC, Cheon GJ (2019) Radiomics in oncological PET/CT: A methodological overview. Nucl Med Mol Imaging 53:14–29
Hotta M, Minamimoto R, Gohda Y et al (2021) Prognostic value of 18 F-FDG PET/CT with texture analysis in patients with rectal cancer treated by surgery. Ann Nucl Med 35:843–852
Galloway MM (1975) Texture analysis using gray level run lengths. Comput Graph Image Process 4:172–179
Suzuki K, Yisong C (2018) In: Suzuki K, Chen Y (eds) Artificial intelligence in decision support systems for diagnosis in medical imaging [Internet]. Springer International Publishing, Cham. https://doi.org/10.1007/978-3-319-68843-5
Wachinger C, Reuter M (2016) Domain adaptation for Alzheimer’s disease diagnostics. Neuroimage 139:470–479
Lefebvre JL, Chevalier D, Luboinski B, Kirkpatrick A, Collette L, Sahmoud T (1996) Larynx preservation in pyriform sinus cancer: preliminary results of a European Organization for Research and Treatment of Cancer phase III trial. EORTC Head and Neck Cancer Cooperative Group. J Natl Cancer Inst 88:890–899
Hoffman HT, Karnell LH, Shah JP et al (1997) Hypopharyngeal cancer patient care evaluation. Laryngoscope 107:1005–1017
Hayashi J, Sakata KI, Someya M et al (2012) Analysis and results of Ku and XRCC4 expression in hypopharyngeal cancer tissues treated with chemoradiotherapy. Oncol Lett 4:151–155
Wendt M, Romanitan M, Näsman A et al (2014) Presence of human papillomaviruses and p16 expression in hypopharyngeal cancer. Head Neck 36:107–112
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Consent to Participate
Informed consent was waived by the institutional review board for this retrospective study.
Conflict of Interest
The authors declare that they have no conflict interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information

Supplementary Fig. 1
Kaplan–Meier survival curves for progression-free survival (PFS) in patients with hypopharyngeal cancer using the UICC stage. There were significant differences in 5-year PFS rates (p < 0.001) among the UICC stages. (PNG 86 kb)
ESM 2
(DOCX 53 kb)
Rights and permissions
About this article
Cite this article
Nakajo, M., Kawaji, K., Nagano, H. et al. The Usefulness of Machine Learning–Based Evaluation of Clinical and Pretreatment [18F]-FDG-PET/CT Radiomic Features for Predicting Prognosis in Hypopharyngeal Cancer. Mol Imaging Biol 25, 303–313 (2023). https://doi.org/10.1007/s11307-022-01757-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11307-022-01757-7