Abstract
Introduction
Sleep disorder is a common and unpleasant symptom in patients with chronic kidney disease (CKD), bringing a heavy burden on the patients and families. As a non-pharmacological therapy, exercise interventions are widely recommended for CKD patients. However, whether exercise can improve overall sleep quality in such a population remains ambiguous. The systematic review and meta-analysis aimed to evaluate the effect of exercise interventions on sleep quality in CKD patients.
Methods
PubMed, Embase, Web of Science, Cochrane Central Register of Controlled Trials, and ClinicalTrials.gov were searched from inception to April 22, 2022. A randomized controlled trial (RCT) added an exercise intervention to conventional treatment/usual care to assess the effect on sleep quality in CKD patients. Two authors independently selected literature, extracted data, assessed the risk of bias using the Cochrane risk of bias tool 2, and assessed the certainty of the evidence using the Grading of Recommendations, Assessment, Development, and Evaluation. The outcome was analyzed using a random-effect model using the Hartung-Knapp-Sidik-Jonkman method as a standardized mean difference (SMD). Additional statistical analysis includes the Egger regression test, subgroup analysis, sensitivity analysis, and meta-regression.
Results
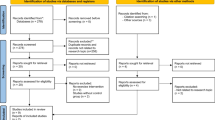
Nineteen articles (20 RCTs) enrolling 989 patients with CKD were included. The pooled SMD suggested favorably associated exercise interventions (SMD − 0.16; 95% CI − 0.62 to 0.31; very low evidence) with substantial heterogeneity (I2 = 87%). Subgroup analyses demonstrated that SMD for sleep quality favored moderate intensity and aerobic exercise, no matter the time, but not statistically significant. Meta-regression showed that the effect size of exercise interventions on sleep quality was not associated with the total sample size, the proportion of males, duration of intervention, mean age, and exercise volume but was associated with baseline sleep scores. In addition, there may be an exercise threshold for the effect of exercise on sleep in CKD patients (i.e., 80 min/week).
Conclusion
This systematic review and meta-analysis suggest that exercise interventions may be associated with improved sleep quality in patients with CKD. However, high heterogeneity and a small effect size limit this result. More studies and standardized reporting of exercise intervention characteristics should be conducted in the future to strengthen the most convincing evidence in this field.


Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this article and its additional files.
Abbreviations
- CKD:
-
Chronic kidney disease
- SMD:
-
Standardized mean difference
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analyses
- CENTRAL:
-
Cochrane central register of controlled trials
- MeSH:
-
Medical subject heading
- RCT:
-
Randomized controlled trial
- PSQI:
-
Pittsburgh sleep quality index
- ESS:
-
Epworth sleepiness scale
- KDQOL-SF™:
-
Kidney-disease quality of life-short form
- PSG:
-
Polysomnography
- MD:
-
Mean differences
- GRADE:
-
Grading of recommendations, assessment, development, and evaluation
- CERT:
-
Consensus on exercise reporting template
References
Yang C, Gao B, Zhao X, Su Z, Sun X, Wang HY, Zhang P, Wang R, Liu J, Tang W et al (2020) Executive summary for China kidney disease network (CK-NET) 2016 annual data report. Kidney Int 98(6):1419–1423. https://doi.org/10.1016/j.kint.2020.09.003
Webster AC, Nagler EV, Morton RL, Masson P (2017) Chronic kidney disease. Lancet 389(10075):1238–1252. https://doi.org/10.1016/S0140-6736(16)32064-5
Iliescu EA, Yeates KE, Holland DC (2004) Quality of sleep in patients with chronic kidney disease. Nephrol Dial Transplant 19(1):95–99. https://doi.org/10.1093/ndt/gfg423
Chu G, Choi P, McDonald VM (2018) Sleep disturbance and sleep-disordered breathing in hemodialysis patients. Semin Dial 31(1):48–58. https://doi.org/10.1111/sdi.12617
Nigam G, Camacho M, Chang ET, Riaz M (2018) Exploring sleep disorders in patients with chronic kidney disease. Nat Sci Sleep 10:35–43. https://doi.org/10.2147/nss.S125839
Agarwal R, Light RP (2011) Sleep and activity in chronic kidney disease: a longitudinal study. Clin J Am Soc Nephrol 6(6):1258–1265. https://doi.org/10.2215/cjn.10581110
Cheng E, Evangelidis N, Guha C, Hanson CS, Unruh M, Wilkie M, Schell J, Hecking M, Gonzalez AM, Ju A et al (2021) Patient experiences of sleep in dialysis: systematic review of qualitative studies. Sleep Med 80:66–76. https://doi.org/10.1016/j.sleep.2021.01.019
Ng ESY, Wong PY, Kamaruddin ATH, Lim CTS, Chan YM (2020) Poor sleep quality, depression and social support are determinants of serum phosphate level among hemodialysis patients in Malaysia. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph17145144
Park S, Lee S, Kim Y, Lee Y, Kang MW, Kim K, Kim YC, Han SS, Lee H, Lee JP et al (2020) Short or long sleep duration and CKD: a Mendelian randomization study. J Am Soc Nephrol 31(12):2937–2947. https://doi.org/10.1681/asn.2020050666
Lee HJ, Kwak N, Kim YC, Choi SM, Lee J, Park YS, Lee CH, Lee SM, Yoo CG, Cho J (2021) Impact of sleep duration on mortality and quality of life in chronic kidney disease: results from the 2007–2015 KNHANES. Am J Nephrol 52(5):396–403. https://doi.org/10.1159/000516096
Jhamb M, Ran X, Abdalla H, Roumelioti ME, Hou S, Davis H, Patel SR, Yabes J, Unruh M (2020) Association of sleep apnea with mortality in patients with advanced kidney disease. Clin J Am Soc Nephrol 15(2):182–190. https://doi.org/10.2215/cjn.07880719
Kutner NG, Zhang R, Huang Y, Bliwise DL (2007) Association of sleep difficulty with kidney disease quality of life cognitive function score reported by patients who recently started dialysis. Clin J Am Soc Nephrol 2(2):284–289. https://doi.org/10.2215/cjn.03000906
Lubas MM, Ware JC, Szklo-Coxe M (2019) Sleep apnea and kidney transplant outcomes: findings from a 20-year (1997–2017) historical cohort study. Sleep Med 63:151–158. https://doi.org/10.1016/j.sleep.2019.05.014
Nguyen T, Polyakova B, Cerenzio J, Ramilo JR (2021) Diphenhydramine use in end-stage kidney disease. Am J Ther 28(2):e232–e237. https://doi.org/10.1097/mjt.0000000000001057
Molnar MZ, Novak M, Mucsi I (2006) Management of restless legs syndrome in patients on dialysis. Drugs 66(5):607–624. https://doi.org/10.2165/00003495-200666050-00003
Dashti-Khavidaki S, Chamani N, Khalili H, Hajhossein Talasaz A, Ahmadi F, Lessan-Pezeshki M, Ghaeli P, Dalili S, Alimadadi A (2011) Comparing effects of clonazepam and zolpidem on sleep quality of patients on maintenance hemodialysis. Iran J Kidney Dis 5(6):404–409
Amiri S, Hasani J, Satkin M (2021) Effect of exercise training on improving sleep disturbances: a systematic review and meta-analysis of randomized control trials. Sleep Med 84:205–218. https://doi.org/10.1016/j.sleep.2021.05.013
Xie Y, Liu S, Chen XJ, Yu HH, Yang Y, Wang W (2021) Effects of exercise on sleep quality and insomnia in adults: a systematic review and meta-analysis of randomized controlled trials. Front Psychiatry 12:664499. https://doi.org/10.3389/fpsyt.2021.664499
Song YY, Hu RJ, Diao YS, Chen L, Jiang XL (2018) Effects of exercise training on restless legs syndrome, depression, sleep quality, and fatigue among hemodialysis patients: a systematic review and meta-analysis. J Pain Symptom Manage 55(4):1184–1195. https://doi.org/10.1016/j.jpainsymman.2017.12.472
Natale P, Ruospo M, Saglimbene VM, Palmer SC, Strippoli GF (2019) Interventions for improving sleep quality in people with chronic kidney disease. Cochrane Database Syst Rev 5(5):CD012625. https://doi.org/10.1002/14651858.CD012625.pub2
Aoike DT, Baria F, Kamimura MA, Ammirati A, Cuppari L (2018) Home-based versus center-based aerobic exercise on cardiopulmonary performance, physical function, quality of life and quality of sleep of overweight patients with chronic kidney disease. Clin Exp Nephrol 22(1):87–98. https://doi.org/10.1007/s10157-017-1429-2
Cho JH, Lee JY, Lee S, Park H, Choi SW, Kim JC (2018) Effect of intradialytic exercise on daily physical activity and sleep quality in maintenance hemodialysis patients. Int Urol Nephrol 50(4):745–754. https://doi.org/10.1007/s11255-018-1796-y
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4(1):1. https://doi.org/10.1186/2046-4053-4-1
Hargrove N, El Tobgy N, Zhou O, Pinder M, Plant B, Askin N, Bieber L, Collister D, Whitlock R, Tangri N et al (2021) Effect of aerobic exercise on dialysis-related symptoms in individuals undergoing maintenance hemodialysis: a systematic review and meta-analysis of clinical trials. Clin J Am Soc Nephrol 16(4):560–574. https://doi.org/10.2215/cjn.15080920
Yang B, Xu J, Xue Q, Wei T, Xu J, Ye C, Mei C, Mao Z (2015) Non-pharmacological interventions for improving sleep quality in patients on dialysis: systematic review and meta-analysis. Sleep Med Rev 23:68–82. https://doi.org/10.1016/j.smrv.2014.11.005
Guo Y, Qiu P, Liu T (2014) Tai Ji Quan: an overview of its history, health benefits, and cultural value. J Sport Health Sci 3(1):3–8. https://doi.org/10.1016/j.jshs.2013.10.004
Martin-Alemañy G, Valdez-Ortiz R, Olvera-Soto G, Gomez-Guerrero I, Aguire-Esquivel G, Cantu-Quintanilla G, Lopez-Alvarenga JC, Miranda-Alatriste P, Espinosa-Cuevas A (2016) The effects of resistance exercise and oral nutritional supplementation during hemodialysis on indicators of nutritional status and quality of life. Nephrol Dial Transplant 31(10):1712–1720. https://doi.org/10.1093/ndt/gfw297
Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh sleep quality index: a new instrument for psychiatric practice and research. Psychiatry Res 28(2):193–213
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Hays RD, Kallich JD, Mapes DL, Coons SJ, Carter WB (1994) Development of the kidney disease quality of life (KDQOL) instrument. Qual Life Res 3(5):329–338. https://doi.org/10.1007/bf00451725
Berry RB, Brooks R, Gamaldo C, Harding SM, Lloyd RM, Quan SF, Troester MT, Vaughn BV (2017) AASM scoring manual updates for 2017 (Version 2.4). J Clin Sleep Med 13(5):665–666. https://doi.org/10.5664/jcsm.6576
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng H-Y, Corbett MS, Eldridge SM et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898. https://doi.org/10.1136/bmj.l4898
Pellizzaro CO, Thomé FS, Veronese FV (2013) Effect of peripheral and respiratory muscle training on the functional capacity of hemodialysis patients. Ren Fail 35(2):189–197. https://doi.org/10.3109/0886022x.2012.745727
Poorsaadet L, Soltani P, Ghassami K, Kohansal B, Ahmadlou M (2018) The effects of aerobic exercise on cognitive performance and sleep quality haemodialysis patients. Aust Med J 11(5):278–285
Paluchamy T, Vaidyanathan R (2018) Effectiveness of intradialytic exercise on dialysis adequacy, physiological parameters, biochemical markers and quality of life—a pilot study. Saudi J Kidney Dis Transpl 29(4):902–910. https://doi.org/10.4103/1319-2442.239661
Greenwood SA, Koufaki P, Macdonald JH, Bhandari S, Burton JO, Dasgupta I, Farrington K, Ford I, Kalra PA, Kean S et al (2021) Randomized trial-prescription of intradialytic exercise to improve quality of life in patients receiving hemodialysis. Kidney Int Rep 6(8):2159–2170. https://doi.org/10.1016/j.ekir.2021.05.034
Giannaki CD, Sakkas GK, Karatzaferi C, Hadjigeorgiou GM, Lavdas E, Kyriakides T, Koutedakis Y, Stefanidis I (2013) Effect of exercise training and dopamine agonists in patients with uremic restless legs syndrome: a six-month randomized, partially double-blind, placebo-controlled comparative study. BMC Nephrol 14:194. https://doi.org/10.1186/1471-2369-14-194
Deeks JJ, Higgins JPT, Altman DG (eds) (2022) Chapter 10: analysing data and undertaking meta-analyses. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). Cochrane. https://training.cochrane.org/handbook
Cristini J, Weiss M, De Las HB, Medina-Rincón A, Dagher A, Postuma RB, Huber R, Doyon J, Rosa-Neto P, Carrier J et al (2021) The effects of exercise on sleep quality in persons with Parkinson’s disease: a systematic review with meta-analysis. Sleep Med Rev 55:101384. https://doi.org/10.1016/j.smrv.2020.101384
Amini E, Goudarzi I, Masoudi R, Ahmadi A, Momeni A (2016) Effect of progressive muscle relaxation and aerobic exercise on anxiety, sleep quality, and fatigue in patients with chronic renal failure undergoing hemodialysis. Int J Pharm Clin Res 8(12):1634–1639
Amirtha Santhi S, Samson R, Srikanth, Pethuru D (2018) Effectiveness of physical activity on depression, anxiety, stress and quality of life of patients on hemodialysis. Biomed Res (India) 29(9):1885–1890
Aoike DT, Baria F, Kamimura MA, Ammirati A, de Mello MT, Cuppari L (2015) Impact of home-based aerobic exercise on the physical capacity of overweight patients with chronic kidney disease. Int Urol Nephrol 47(2):359–367. https://doi.org/10.1007/s11255-014-0894-8
Maynard LG, de Menezes DL, Lião NS, de Jesus EM, Andrade NLS, Santos JCD, da Silva Júnior WM, Bastos KA, Barreto Filho JAS (2019) Effects of exercise training combined with virtual reality in functionality and health-related quality of life of patients on hemodialysis. Games Health J 8(5):339–348. https://doi.org/10.1089/g4h.2018.0066
Pereira ABN, Santana LL, Rocha LB, Cunha KDC, Rocha LSO, Santos MCS, Normando VMF, Torres DDC, Rocha RSB (2022) Physical exercise affects quality of life and cardiac autonomic modulation in patients with chronic kidney failure submitted to hemodialysis: a randomized clinical trial. Percept Mot Skills. https://doi.org/10.1177/00315125221085811
Sakkas GK, Hadjigeorgiou GM, Karatzaferi C, Maridaki MD, Giannaki CD, Mertens PR, Rountas C, Vlychou M, Liakopoulos V, Stefanidis I (2008) Intradialytic aerobic exercise training ameliorates symptoms of restless legs syndrome and improves functional capacity in patients on hemodialysis: a pilot study. Asaio j 54(2):185–190. https://doi.org/10.1097/MAT.0b013e3181641b07
Uchiyama K, Adachi K, Muraoka K, Nakayama T, Oshida T, Yasuda M, Hishikawa A, Minakuchi H, Miyashita K, Tokuyama H et al (2021) Home-based aerobic exercise and resistance training for severe chronic kidney disease: a randomized controlled trial. J Cachexia Sarcopenia Muscle 12(6):1789–1802. https://doi.org/10.1002/jcsm.12775
Uchiyama K, Washida N, Morimoto K, Muraoka K, Kasai T, Yamaki K, Miyashita K, Wakino S, Itoh H (2019) Home-based aerobic exercise and resistance training in peritoneal dialysis patients: a randomized controlled trial. Sci Rep 9(1):2632. https://doi.org/10.1038/s41598-019-39074-9
Wu Y, He Q, Yin X, He Q, Cao S, Ying G (2014) Effect of individualized exercise during maintenance haemodialysis on exercise capacity and health-related quality of life in patients with uraemia. J Int Med Res 42(3):718–727. https://doi.org/10.1177/0300060513509037
Higgins JPT, Li T, Deeks JJ (eds) (2022) Chapter 6: choosing effect measures and computing estimates of effect. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) Cochrane handbook for systematic reviews of interventions version 6.3 (updated February 2022). Cochrane. https://training.cochrane.org/handbook
Baggetta R, D’Arrigo G, Torino C, ElHafeez SA, Manfredini F, Mallamaci F, Zoccali C, Tripepi G (2018) Effect of a home based, low intensity, physical exercise program in older adults dialysis patients: a secondary analysis of the EXCITE trial. BMC Geriatr 18(1):248. https://doi.org/10.1186/s12877-018-0938-5
Manfredini F, Mallamaci F, D’Arrigo G, Baggetta R, Bolignano D, Torino C, Lamberti N, Bertoli S, Ciurlino D, Rocca-Rey L et al (2017) Exercise in patients on dialysis: a multicenter, randomized clinical trial. J Am Soc Nephrol 28(4):1259–1268. https://doi.org/10.1681/asn.2016030378
Van Craenenbroeck AH, Van Craenenbroeck EM, Van Ackeren K, Vrints CJ, Conraads VM, Verpooten GA, Kouidi E, Couttenye MM (2015) Effect of moderate aerobic exercise training on endothelial function and arterial stiffness in CKD stages 3–4: a randomized controlled trial. Am J Kidney Dis 66(2):285–296. https://doi.org/10.1053/j.ajkd.2015.03.015
Norton K, Norton L, Sadgrove D (2010) Position statement on physical activity and exercise intensity terminology. J Sci Med Sport 13(5):496–502. https://doi.org/10.1016/j.jsams.2009.09.008
Jayedi A, Emadi A, Shab-Bidar S (2022) Dose-dependent effect of supervised aerobic exercise on HbA(1c) in patients with type 2 diabetes: a meta-analysis of randomized controlled trials. Sports Med. https://doi.org/10.1007/s40279-022-01673-4
IntHout J, Ioannidis JP, Borm GF (2014) The Hartung-Knapp-Sidik-Jonkman method for random effects meta-analysis is straightforward and considerably outperforms the standard DerSimonian-Laird method. BMC Med Res Methodol 14:25. https://doi.org/10.1186/1471-2288-14-25
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634. https://doi.org/10.1136/bmj.315.7109.629
Sterne J, Harbord R (2004) Funnel plots in meta-analysis. Stata J 4:127–141. https://doi.org/10.1177/1536867X0400400204
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558. https://doi.org/10.1002/sim.1186
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Harbord R, Higgins J (2008) Meta-regression in Stata. Stata J 8:493–519. https://doi.org/10.1177/1536867X0800800403
Balbim GM, Falck RS, Barha CK, Starkey SY, Bullock A, Davis JC, Liu-Ambrose T (2022) Effects of exercise training on the cognitive function of older adults with different types of dementia: a systematic review and meta-analysis. Br J Sports Med. https://doi.org/10.1136/bjsports-2021-104955 (Online ahead of print)
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, Schünemann HJ (2008) GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ 336(7650):924–926. https://doi.org/10.1136/bmj.39489.470347.AD
Afshar R, Emany A, Saremi A, Shavandi N, Sanavi S (2011) Effects of intradialytic aerobic training on sleep quality in hemodialysis patients. Iran J Kidney Dis 5(2):119–123
Giannaki CD, Hadjigeorgiou GM, Karatzaferi C, Maridaki MD, Koutedakis Y, Founta P, Tsianas N, Stefanidis I, Sakkas GK (2013) A single-blind randomized controlled trial to evaluate the effect of 6 months of progressive aerobic exercise training in patients with uraemic restless legs syndrome. Nephrol Dial Transplant 28(11):2834–2840. https://doi.org/10.1093/ndt/gft288
Hernández Sánchez S, Carrero JJ, Morales JS, Ruiz JR (2021) Effects of a resistance training program in kidney transplant recipients: a randomized controlled trial. Scand J Med Sci Sports 31(2):473–479. https://doi.org/10.1111/sms.13853
Yurtkuran M, Alp A, Yurtkuran M, Dilek K (2007) A modified yoga-based exercise program in hemodialysis patients: a randomized controlled study. Complement Ther Med 15(3):164–171. https://doi.org/10.1016/j.ctim.2006.06.008
La Forge R (2005) Aligning mind and body. ACSM’s Health Fitness J 9:7–14. https://doi.org/10.1097/00135124-200509000-00006
Stillman CM, Esteban-Cornejo I, Brown B, Bender CM, Erickson KI (2020) Effects of exercise on brain and cognition across age groups and health states. Trends Neurosci 43(7):533–543. https://doi.org/10.1016/j.tins.2020.04.010
Frimpong E, Mograss M, Zvionow T, Dang-Vu TT (2021) The effects of evening high-intensity exercise on sleep in healthy adults: a systematic review and meta-analysis. Sleep Med Rev 60:101535. https://doi.org/10.1016/j.smrv.2021.101535
Slade SC, Dionne CE, Underwood M, Buchbinder R (2016) Consensus on exercise reporting template (CERT): explanation and elaboration statement. Br J Sports Med 50(23):1428–1437. https://doi.org/10.1136/bjsports-2016-096651
Baker LA, March DS, Wilkinson TJ, Billany RE, Bishop NC, Castle EM, Chilcot J, Davies MD, Graham-Brown MPM, Greenwood SA et al (2022) Clinical practice guideline exercise and lifestyle in chronic kidney disease. BMC Nephrol 23(1):75. https://doi.org/10.1186/s12882-021-02618-1
Smart NA, Williams AD, Levinger I, Selig S, Howden E, Coombes JS, Fassett RG (2013) Exercise & sports science Australia (ESSA) position statement on exercise and chronic kidney disease. J Sci Med Sport 16(5):406–411. https://doi.org/10.1016/j.jsams.2013.01.005
Sadeh A (2011) The role and validity of actigraphy in sleep medicine: an update. Sleep Med Rev 15(4):259–267. https://doi.org/10.1016/j.smrv.2010.10.001
Howden EJ, Lawley JS, Esler M, Levine BD (2017) Potential role of endurance training in altering renal sympathetic nerve activity in CKD? Auton Neurosci 204:74–80. https://doi.org/10.1016/j.autneu.2016.11.002
Fuhro MI, Dorneles GP, Andrade FP, Romão PRT, Peres A, Monteiro MB (2018) Acute exercise during hemodialysis prevents the decrease in natural killer cells in patients with chronic kidney disease: a pilot study. Int Urol Nephrol 50(3):527–534. https://doi.org/10.1007/s11255-017-1747-z
Greenwood SA, Lindup H, Taylor K, Koufaki P, Rush R, Macdougall IC, Mercer TH (2012) Evaluation of a pragmatic exercise rehabilitation programme in chronic kidney disease. Nephrol Dial Transplant 27(Suppl 3):iii126-134. https://doi.org/10.1093/ndt/gfs272
Acknowledgements
We are grateful to Professor Tiansong Zhang for guiding my study.
Funding
This study is supported by Longhua Hospital Shanghai University of Traditional Chinese Medicine (Grant number: Y21026).
Author information
Authors and Affiliations
Contributions
Conceptualization: LH, WW. Methodology: FZ, YZ. Writing-original draft: FZ, HW. Writing-review and editing: HZ, WZ.
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no competing interests exist.
Ethical approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, F., Wang, H., Huang, L. et al. Effect of exercise interventions for sleep quality in patients with chronic kidney disease: a systematic review and meta-analysis. Int Urol Nephrol 55, 1193–1204 (2023). https://doi.org/10.1007/s11255-022-03413-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-022-03413-z