Abstract
Background
Health-related quality of life (HRQOL) is a key concept in pediatric oncology. This systematic review aims to update the conceptual HRQOL model by Anthony et al. (Qual Life Res 23(3):771–789, 2014), covering physical, emotional, social and general HRQOL aspects, and to present a comprehensive overview of age- and disease-specific HRQOL issues in children with cancer.
Methods
Medline, PsychINFO, the Cochrane Database for Systematic Reviews (CDSR), and the COSMIN database were searched (up to 31.12.2020) for publications using patient-reported outcome measures (PROMs) and qualitative studies in children with cancer (8–14-year) or their parents. Items and quotations were extracted and mapped onto the conceptual model for HRQOL in children with cancer mentioned above.
Results
Of 2038 identified studies, 221 were included for data extraction. We identified 96 PROMS with 2641 items and extracted 798 quotations from 45 qualitative studies. Most items and quotations (94.8%) could be mapped onto the conceptual model. However, some adaptations were made and the model was complemented by (sub)domains for ‘treatment burden’, ‘treatment involvement’, and ‘financial issues’. Physical and psychological aspects were more frequently covered than social issues.
Discussion
This review provides a comprehensive overview of HRQOL issues for children with cancer. Our findings mostly support the HRQOL model by Anthony et al. (Qual Life Res 23(3):771–789, 2014), but some adaptations are suggested. This review may be considered a starting point for a refinement of our understanding of HRQOL in children with cancer. Further qualitative research will help to evaluate the comprehensiveness of the HRQOL model and the relevance of the issues it encompasses.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Plain English summary
Due to improved treatment options, more and more children with cancer survive their disease. However, disease and treatment are still burdensome. This does concern children’s physical health, but also their emotional well-being and social life (e.g., family, friends, school). Thus, the focus shifts from survival to children’s health-related quality of life (HRQOL). Several questionnaires—so-called patient-reported outcome measures (PROMs)—have been developed to assess HRQOL from children’s perspective, but they cover different contents. This indicates that there is no consensus about which issues are relevant for HRQOL in children with cancer. In our study, we systematically investigated what existing PROMs assess as well as which issues were discussed in interview studies with children with cancer or their parents. We then compared our findings with an existing model of HRQOL. Our results widely support this previous model, but we suggest some adaptations: We introduced new subdomains for treatment-related emotional burdens (e.g., fear of needles) and treatment involvement (e.g., shared decision-making). Furthermore, we included financial issues, which were not covered within the previous model. While our study gives a very comprehensive overview of what issues are investigated in children with cancer, we cannot make assumptions about which issues are more or less important. Further interview studies with children are needed to learn more about the importance and understandability of the identified issues. With our review, we want to provide a starting point for the further refinement of our understanding of HRQOL in children with cancer.
Background
Children are affected by different types of cancer compared with adults and represent a unique patient population with distinct features in terms of physiological and cognitive development. While survival rates have consistently improved over the last decades [1,2,3], children with cancer still face substantial symptoms and side-effects of the disease and treatment. This may include physical, emotional, and psychosocial, but also school-related aspects of health-related quality of life (HRQOL) [4]. Since most HRQOL aspects are only accessible from the individual's perspective, both the Food and Drug Administration (FDA) and the European Medicines Agency (EMA) recommend the use of patient-reported outcome (PRO) in pediatric oncology [5, 6].
The taskforce for PRO assessment in children and adolescents within the International Society for Pharmacoeconomics and Outcomes Research (ISPOR) has highlighted the importance of age-appropriate assessment [7]: While by the age of 5 years children are able to give basic self-reports, this ability substantially improves by the age of 8 years. From 8 years on, children’s self-report should be considered the most important source of information [8]. However, due to their developmental stage, age-appropriate instruments are needed [8, 9]. At the age of 15, adolescents can complete adult forms [10], but age-specific PROMs are currently being developed to cover the unique challenges at the transition to adulthood [11,12,13,14,15].
Despite the increased awareness of the importance of HRQOL in children with cancer, PROMs are still rarely used in clinical trials [16, 17]. While a generic Standard Set for Pediatric Health Assessment has recently been published [18], no cancer-specific core outcome set has yet been defined. Available HRQOL instruments differ considerably in terms of content [19] and have been criticized for mostly focusing on negative aspects (i.e., impairments instead of functional ability) [20]. While this might be the main focus of clinicians who aim to relieve patients from impairments, children place a high priority on social participation and resources [21]. This might be due to the fact that most questionnaires have either been developed without sufficient patient involvement [22, 23] or developed and validated with adult patients [24]. This is problematic since the involvement of children is a key requirement to ensure content validity of pediatric PRO measures [7].
The most comprehensive conceptual framework for HRQOL in children with cancer so far has been presented by Anthony et al. [25]. In their systematic review, they identified four major HRQOL domains: physical health covers physical functioning and symptoms, while the psychological domain encompasses emotional distress, positive psychological functioning, self-esteem, body image, behavior, and cognitive health. The social domain contains social functioning and relationships, and a general health domain covers the general perception and appraisal of the health status.
The present systematic review builds on the conceptual model of HRQOL in children with cancer provided by Anthony et al. [25] and presents a comprehensive overview of age- and disease-specific HRQOL issues in children with cancer aged 8 to 14 years. To do so, pediatric PROMs as well as qualitative studies with children or their parents are investigated.
Methods
Following the ISPOR guidelines [7], we focused on a specific predefined age-group. The age-range of 8 to 14 years was determined based on cognitive and social aspects as described above. The review forms part of a larger program of work involving the development of a new questionnaire and follows PROM development guidelines by the Quality of Life Group of the European Organization for Research and Treatment of Cancer (EORTC QLG) [26]. The review was not pre-registered since the most commonly used platforms (e.g., PROSPERO) only accepted COVID-19 related registrations at that point in time. Additional information on the data collection (i.e., template data collection forms; data extracted from included studies; data used for all analyses; other materials used in the review) can be requested from the corresponding author. Where applicable, the results were reported in line with the recommendations of the preferred reporting items of systematic reviews and meta-analyses (PRISMA) guidelines [27] (Supplement 1).
Search strategy and study selection
In December 2020, a systematic literature search was conducted in several databases: The strategy (see Table 1) used medical subject headings (MeSH terms) to search MEDLINE via PubMed. For PsycINFO and CDSR the search was based on entry terms of these MeSH terms. Corresponding filters were applied to search the COSMIN database of systematic reviews of outcome measurement instruments. The results on PubMed and PsycINFO were additionally filtered for peer-reviewed manuscripts in English, German, French, or Spanish, to match the language skills of the reviewers.
Studies were selected in a stepwise approach. In each step, teams of at least two reviewers rated eligible papers independently against predefined inclusion and exclusion criteria (see below). First, eligible papers were identified based on their title and abstract by two pairs of reviewers (DR & MR; GR & SS). Second, the full texts of studies identified as relevant by at least one reviewer were re-evaluated in detail by three teams of reviewers [DR & MR; GR & SS; TdR & GP & GA]. The RAYYAN software [28] was used to record these ratings.
Inclusion and exclusion criteria
Quantitative and qualitative publications were included if full-text papers could be accessed and provided information on HRQOL issues of children with cancer at diagnosis or undergoing curative or palliative treatment between the age of 8 to 14 years. Studies assessing parent- or proxy-report alongside self-report by children were accepted. Studies conducted exclusively in parent samples were only included if parents provided qualitative information on the HRQOL of their child diagnosed with cancer. Studies with a broader age-range including older adolescents or younger children were included if they contained children between 8 and 14 years. Reviews were included for descriptive and cross-referencing purposes only.
Studies were excluded if they exclusively (a) investigated healthy or non-cancer samples (mixed samples with cancer patients were included); (b) investigated cancer survivors after treatment completion; (c) consisted of children younger than 8 years (i.e., upper age limit < 8 years); (d) included adolescents and/or adults older than 14 years (i.e., lower age limit > 14 years); or (e) they did not assess HRQOL issues of the children with cancer (e.g., studies focusing on HRQOL of their parents/caregivers, siblings or HCPs; studies relying exclusively on biomarkers, observation- or performance-based clinician reports, or proxy ratings of PROMs). We excluded individual case reports, conference abstracts, and study protocols.
Data extraction
Data were extracted for quantitative and qualitative studies separately. For quantitative studies, a list of PROMs administered to children with cancer was extracted. To ensure that all relevant PROMs were included, the list was cross-checked against a list of 112 measures collected for the development of the ICHOM Standard Set for Pediatric Health Assessment [18]. Subsequently, a comprehensive list of items from all PROMs was extracted [MR]. If the identified studies did not offer sufficient details and no review copy could be found, authors were contacted.
For qualitative studies, a comparable list was extracted, containing direct quotations from children with cancer or corresponding parents [JM]. These quotations consisted of single sentences or short paragraphs representing children’s or parents’ statements in direct speech in order to provide examples for specific subjects discussed in the qualitative studies.
Mapping procedure and analysis
All extracted items and quotations were mapped onto the conceptual model of Anthony et al. [25], using an Excel sheet. Each item/quotation was categorized by two reviewers independently [items: DR & MR; GR & SS; TdR & GP & GA; quotations: JM & MR & DR] as representing a domain, subdomain and identifying concept. In case of conflicts, a third party was consulted, and issues were discussed until consensus was reached. Since some items and quotations could relate to more than one domain, subdomain, or identifying concept, raters were provided with basic mapping rules (Supplement 2) and a list of definitions to optimize interrater reliability. Most definitions were drawn from the Encyclopedia of Quality of Life and Well-Being Research [29]. If items did not fit into the existing model, new identifying concepts or subdomains were formulated. Quantitative analysis was based on descriptive statistics.
Results
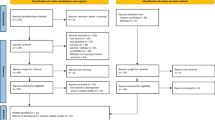
The initial literature search resulted in a total of 2551 hits. After the removal of 83 duplicates, another 2038 studies were excluded based on their title or abstract and 34 studies were excluded because full texts were not accessible. During the full-text screening of the remaining 479 studies, another 213 studies were excluded, resulting in a total of 266 studies which were included in the analysis. Among them were 221 quantitative studies using 96 different PROMs and 45 qualitative studies. For details refer to Fig. 1.
Description of questionnaires administered in quantitative studies
Among the 96 included PROMs, only 19 PROMs were cancer-specific. The most frequently used questionnaires were the PedsQL generic core (in 58/221 studies, 26.2%), PedsQL cancer module (37/221, 16.7%), and the Children's Depression Inventory (CDI; 27/221, 12.2%). The complete list of questionnaires is available in Supplement 3.
About a third of the questionnaires (32/96, 33.3%) assessed multidimensional aspects of HRQOL (i.e., physical and psychosocial factors), while the remaining questionnaires focused solely on either psychological (34/96, 35.4%), physical (26/96, 27.1%), or social factors (4/96, 4.2%).
From all PROMs, a pool of 2,682 individual items was extracted. After excluding conditional, determinant, and open-ended questions, 2,641 items were mapped onto the model of Anthony et al. [25]. As presented in Table 2, almost half of these items were assigned to psychological health-aspects (1239/2641, 46.9%), with most items assessing symptoms of emotional distress. Another third of all items covered physical health (862/2641, 32.6%), while social health (463/2641, 17.2%) accounted for nearly one-fifth. General health perception (73/2641, 2.8%) and financial issues (4/2641, 0.2%) were least frequently assessed.
Description of qualitative studies
Of the 45 qualitative studies, the majority (24/45; 53.3%) focused on more than one domain, while nine studies (9/45, 20.0%) solely focused on physical aspects, eight (8/45, 15.56%) on psychological health, and four studies on social issues. From all qualitative studies, a total of 798 quotations was extracted and mapped onto the conceptual model by Anthony et al. [25]. As shown in Table 2, most quotations were about physical (340/798, 42.6%) and psychological aspects of HRQOL (260/798, 32.6%), while social health (170/798, 21.3%) and general health issues (24/798, 3.0%) were less frequently discussed in the qualitative studies. Only four quotations concerned financial issues (4/798, 0.5%).
Updated conceptual model
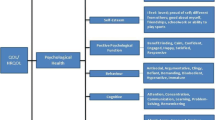
Most of the identified items and quotations (3259/3439; 94.8%) were assigned to one of the domains and subdomains of the conceptual model proposed by Anthony et al. [25]. The remaining 180 items and quotations (180/3439, 5.2%) were assigned to three newly introduced (sub)domains. In the psychological domain, we made a new differentiation between ‘emotional distress’ in general and ‘treatment burden’, which encompasses distress explicitly related to the treatment (e.g., procedural anxiety). Furthermore, we incorporated the previously independent subdomain ‘body image’ as an identifying concept into the ‘self-esteem’ subdomain. Within the social domain, the subdomain ‘treatment involvement’ was added. A new domain for ‘financial issues’ was introduced. An overview of the resulting updated model is presented in Table 2 and Fig. 2. All domains and subdomains are described in more detail in the following paragraphs.
The domain physical health was defined as ‘the extent to which objective physical human states are fulfilled in relation to personal or group perceptions of subjective physical well-being’ [30]. The domain included physical symptoms which were represented by 18 different identifying concepts, such as fatigue, fever, hair loss, or pain. The second subdomain was physical functions, which was represented by 14 identifying concepts, including mobility, physical activity, or physical strength. Most of the issues could be assigned to one of the two subdomains. However, in the case of some issues (e.g., sleep functioning/insomnia or appetite/taste) the wording of the issue informed whether if it was categorized as a symptom or function. To avoid having similar identifying concepts in different subdomains, a consensus was reached among the researchers and issues were assigned to the subdomain they primarily belonged to.
The domain psychological health included a total of six subdomains, namely emotional distress, positive psychological function, self-esteem, treatment burden, cognitive function, and behavior. Most of the items and quotations in this domain could be assigned to the subdomain ‘emotional distress’ (632/1499, 43.6%) which included negative emotional states such as anxiety, depression, stress, sadness, worry, guilt, shame, anger, and envy. While the assignment to this subdomain was clear, the identifying concepts showed a substantial conceptual overlap (e.g., feeling angry, bothered, annoyed, or frustrated).
The newly introduced subdomain ‘treatment burden’ is closely related to emotional distress but covers psychological issues explicitly associated with the treatment. This may include aspects such as procedural anxiety, but also hating to take one's medicine or being bored if the treatment takes a long time. These issues were covered in only six of the identified questionnaires (6/96, 6.3%; SQOLPOP, DISABKIDS DCGM 12/37, PedsQL Child—Transplant, PedsQL Child—SCT, RSQ-PC, USK) and accounted for only 1.9% (24/1239) of items assigned to the psychological domain. In the qualitative studies, however, treatment burden accounted for 15.4% (40/260) of all quotations assigned to the psychological domain and was covered in every fourth study (12/45) [31,32,33,34,35,36,37,38,39,40,41,42]. Children for example told the interviewer that ‘[…] when the nurse told me that I would have to undergo LP, I thought that it is a surgery, so I was really scared’ [38] that they were ‘afraid of unsuccessful treatment’ [42] or ‘fed up […] with medication and chemo[-therapy] I have to undergo’ [34].
The subdomain ‘positive psychological functions’ was defined as abilities to successfully adapt and endure under adverse circumstances as well as efficiently recover from subsequent harmful effects [43]. This subdomain consisted of nine functions and positive emotional states, namely benefit finding, locus of control, feeling calm, confident, engaged, happy, responsive, or satisfied and being religious or having spiritual resources.
The subdomain ‘self-esteem’ was merged with the previously independent subdomain ‘body image’ due to the overlap of content. We defined ‘self-esteem’ as an evaluative aspect of the self-concept that corresponds with an overall view of the self as worthy or unworthy and the assessment of how people feel in relation to their social standing, their physical appearance or their job or school performance [44]. In our review, this included eight identifying concepts, namely feeling different, loved, or proud, feeling good about self or ones’ abilities, friends and school as well as positive feelings about ones’ personal appearance and physical development.
‘Cognitive functions’ included all mental processes to acquire and process knowledge, information, and reasoning [45]. We identified six functions, namely attention, communication, concentration, learning and school-work, problem-solving, and remembering.
In the subdomain ‘behavior’ we included all positive and negative active interactions between the individual and their environment. In the review we were able to identify eight—mainly negative—forms of behavior, namely behaving antisocial/aggressive, argumentative, delinquent, disobedient, hyperactive, or withdrawing. Positive forms of behavior included pro-social behavior and active coping strategies.
The domain ‘social health’ consisted of three subdomains. Social functioning was defined as the ‘ability to achieve personal goals in social interaction while simultaneously maintaining positive relationships’ [46] and included constructs like perceived autonomy and social interactions but also interference with social life due to the disease. Social relationship on the other hand describes the ‘network of social resources that an individual perceives’ [47] and was defined as the quality of social relations with family, parents, siblings but also peers, romantic partners, teachers or others in general.
The third subscale ‘treatment involvement’ was newly introduced to the model based on our findings. This subscale included social and communicative aspects closely related to the treatment, such as information and knowledge about the disease/treatment, involvement in treatment decisions, satisfaction with care but also the quality of relationship with healthcare professionals. Aspects of treatment involvement were covered in 12 questionnaires (12/96, 12.5%; R-PIE, USK, CUIS, QOLCC, LSS-C, CICS, PAC-QOL, PedsQL Child—cancer/transplant module, TQPM, DISABKIDS DCGM, MANE) and accounted for 13.8% (64/463) of items on social health. The focus on this subscale was even more pronounced in qualitative studies: every fourth quotation addressing social health related to treatment involvement (44/170, 25.9%) and the topic was raised in 17 of the 45 (37.8%) qualitative studies [32, 34, 36, 38,39,40,41, 48,49,50,51,52,53,54,55,56,57]. One child, for example, explained the need for information by stating ‘The doctor explains each procedure that I have to undergo, everything that I have to go through. I prefer knowing what's going to happen so that I can prepare myself’ [50]. Children also reported lack of involvement in shared decision-making, for example ‘My mother did [decide when I should train]. Yeah, she decides just about everything’ [36].
The fourth domain ‘general health’ consists of only one subdomain, ‘general health perception’. It covers personal views on patients’ own health, sickness, or HRQOL in the past, present, or future.
A new fifth domain was added to incorporate ‘financial issues’. This was a less frequent issue, only covered in two questionnaires (EORTC QLQ-C30, KIDSCREEN) and two qualitative studies [34, 51]. The EORTC QLQ-C30 item as well as the quotations refer to a financial burden resulting from the condition and/or treatment. The three items of the KIDSCREEN, however, ask whether children have enough money for daily needs and to participate in social activities with peers.
Discussion
The aim of this review was to give a comprehensive overview of HRQOL issues for children aged 8–14 years undergoing treatment for cancer. We collected over 2500 individual items from nearly 100 questionnaires used in quantitative studies as well as almost 800 quotations from qualitative studies. Most items and quotations could be assigned to one of the domains and subdomains of the conceptual model of HRQOL in children with cancer provided by Anthony et al. [25]. Thus, the present review widely supports their HRQOL model. The four major domains physical, emotional, social, and general health as well as most subdomains were maintained. However, based on our results, we suggest complementing and clarifying the model.
Proposed changes to the HRQOL model
Of four proposed changes, two were minor readjustments. We proposed subsuming the previous subdomain ‘body image’ as an identifying concept under the subdomain ‘self-esteem.’ This decision is based on our definition because we regard self-esteem as an evaluative aspect of the self, which also contains feelings towards one’s personal appearance and physical development. Finally, we also identified items and quotations on ‘financial issues,’ which could not be accommodated by the existing model and were therefore assigned to a new, separate domain.
More significant changes were made in the social and psychological domains, where explicitly treatment-related subdomains were introduced. In the psychological domain, a new differentiation was made between general ‘emotional distress’ and ‘treatment burden,’ which covers distress explicitly related to the treatment, as procedural anxiety for instance. One might argue that these aspects could be subsumed under emotional distress and only few questionnaires make this differentiation. However, a large proportion of statements derived from qualitative studies described distress in a direct relation to the treatment). Furthermore, we argue for a specific treatment-related subdomain, as we aim for a model of HRQOL of children undergoing cancer treatment instead of QOL in general.
Within the social domain, we added a subdomain for ‘treatment involvement,’ which covers children’s involvement in shared decision-making, but also their relationships to healthcare-professionals. We considered the healthcare setting as an especially relevant social environment for children with cancer, which is very distinct from other social contexts like family or peers. Communication in this setting has several functions, spanning from sharing information and enabling self-management, to shared decision-making, to sustaining hope, reducing uncertainty, and supporting emotional health [58]. Thus, the quality of social relationships and communication with healthcare providers, is likely to be associated with HRQOL. For example, reduced illness uncertainty has been shown to correlate with improved HRQOL [59]. Therefore, we believe that a specific subdomain for children’s social involvement in healthcare is justified.
Further reflections on the HRQOL model
Beyond that, we faced other challenges and had further discussions on the model, which did not result in adaptations. One problem occurred within the physical domain, as the differentiation between physical symptoms and functions was not always as obvious as expected. In some cases, such as pain, the assignment was relatively clear. However, in the case of other issues such as sleep vs. insomnia the assignment largely depended on the individual wording of the item.
Another discussion came up regarding the subdomain ‘behavior’ within psychological health because behavior in general is not an HRQOL issue, but rather a way to display, communicate, and handle HRQOL issues. Most behaviors described in items or quotations are social behaviors (e.g., to withdraw from others), which can be considered as indicators for social relationships and functioning. Others are expressions of emotions (e.g., aggressive behaviors) or ways to handle psychological burdens (e.g., coping strategies). We decided to maintain this subdomain and its identifying concepts, as they might be relevant or useful for developing proxy-measures which should incorporate observable contents.
Lack of consensus on outcome assessment in children with cancer
Our review also sheds light to a key challenge in HRQOL research in children with cancer. With 96 different PROMs, we have identified a surprisingly large number of PROMs, most of which are not cancer-specific. This might reflect a previously criticized lack of consensus regarding which aspects should be considered essential and thus consistently measured in children with cancer [25, 60]. Recently, Algurén et al. [18] have proposed an Overall Pediatric Health Standard Set (OPH-SS) for children. However, so far, no comparable outcome set has been defined specifically for children with cancer. While generic outcome sets and instruments offer the advantage of comparing the results with healthy children or across different diagnoses, they are not tailored to specific problems children with cancer face. Thus, using generic tools includes the risk of ignoring or overlooking relevant disease-specific HRQOL issues. Furthermore, studies from adult oncology have found generic instruments to be of limited usefulness for the comparison of different cancer treatments, as those measures are not able to detect small changes in HRQOL [61].
The third most commonly used instrument was the CDI [62], a generic instrument assessing depressive symptoms. Even though HRQOL questionnaires contain subscales on emotional health, they may not provide the same depth of information. Less items are available per subscale in multidimensional instruments and a choice must be made which aspects should be included.
To make sure that the final selection of items covers what matters to children, PROM development guidelines require patient involvement in the concept elicitation and cognitive interviews [7, 8, 26, 63, 64]. Nevertheless, children with cancer have rarely been involved in the development of PROMs [22, 23]. Consequently, there is only scarce evidence for the content validity of most available PROMs [23, 65]. Thus, it is questionable whether they cover children’s priorities. For instance, Anthony et al. [21] have shown that social health is underrepresented in existing questionnaires, even though children rate social aspects as most important. In our review, the social domain was also represented by less items and quotations than physical and psychological health.
Strengths, limitations, and outlook
Our review offers an extensive overview of HRQOL issues assessed by PROMs and reported in qualitative studies with children with cancer and their parents. The comprehensiveness can be considered a strength but might also be a limitation. Not only for symptoms and physical functions but also for emotional distress, some identifying concepts show overlapping content. As our review is based on the literature only, we cannot make final statements on the comprehensiveness, relevance, or understandability of the model and its issues from children’s perspective.
For example, we added a domain for ‘financial issues’ that were covered in two PROMs and mentioned in two qualitative studies. However, children might view financial issues as not important or relevant to them or they might not have an understanding of the financial impact of cancer. Thus, it is likely that such issues will not form part of the final EORTC QLG children’s questionnaire which we are currently developing. Questions on finances should perhaps be reserved for caregivers to answer given that they carry more financial responsibilities than children themselves.
We are convinced that, for further refinement of the model, patients, caregivers, and clinical experts should be involved. Thus, we are currently conducting qualitative interviews in an international sample of 8- to 14-year-old cancer patients, their caregivers, and healthcare professionals. In these interviews, participants are invited to describe their understanding of HRQOL before commenting on the comprehensiveness of the updated model as well as the relevance and comprehensibility of all issues.
The selection of included studies was limited by the languages spoken within the reviewers’ team. While we were able to cover studies in English, German, and Spanish and assume that these languages account for the vast majority of scientific literature, we cannot rule out that we could have missed out on information in other languages.
Conclusion
This review presents a comprehensive overview of HRQOL issues derived from quantitative and qualitative studies. While our findings were mostly in line with the previously proposed conceptual model by Anthony et al. [25], we proposed some adaptations. Mainly, we introduced treatment-related subdomains in the social and psychological domains. Further qualitative studies are needed to evaluate the relevance and comprehensibility of all identified HRQOL issues from children’s perspective. This review may be considered a starting point for a refinement of our understanding and concept of HRQOL in children with cancer.
References
Siegel, D. A., King, J., Tai, E., Buchanan, N., Ajani, U. A., & Li, J. (2014). Cancer incidence rates and trends among children and adolescents in the United States, 2001–2009. Pediatrics, 134(4), e945–e955.
Smith, M. A., Altekruse, S. F., Adamson, P. C., Reaman, G. H., & Seibel, N. L. (2014). Declining childhood and adolescent cancer mortality. Cancer, 120(16), 2497–2506.
Howlader, N., Noone, A., Krapcho, M., Miller, D., Brest, A., Yu, M., Ruhl, J., Tatalovich, Z., Mariotto, A., Lewis, D. R., Chen, H. S., Feuer, E. J., Cronin, K. A. (eds) (2021). SEER cancer statistics review, 1975–2018. National Cancer Institute.
National Cancer Institute (NCI) (2015). Children with cancer—A guide for parents. National Institutes of Health.
EMA (2016). Appendix 2 to the guideline on the evaluation of anticancer medicinal products in man: The use of patient-reported outcome (PRO) measures in oncology studies. European Medicines Agency.
FDA (2009). Patient-reported outcome measures: Use in medical product development to support labeling claims. Food and Drug Administration.
Matza, L. S., Patrick, D. L., Riley, A. W., Alexander, J. J., Rajmil, L., Pleil, A. M., Bullinger, M. (2013). Pediatric patient-reported outcome instruments for research to support medical product labeling: Report of the ISPOR PRO good research practices for the assessment of children and adolescents task force. Value Health., 16(4), 461–479.
Arbuckle, R., & Abetz-Webb, L. (2013). “Not just little adults”: Qualitative methods to support the development of pediatric patient-reported outcomes. Patient., 6(3), 143–159.
Coombes, L., Bristowe, K., Ellis-Smith, C., Aworinde, J., Fraser, L. K., Downing, J., Bluebond-Langner, M., Chambers, L., Murtagh, F. E. M., Harding, R. (2021). Enhancing validity, reliability and participation in self-reported health outcome measurement for children and young people: A systematic review of recall period, response scale format, and administration modality. Quality of Life Research, 30(7), 1803–1832.
Withycombe, J. S., McFatrich, M., Pinheiro, L., Hinds, P. S., Keller, F. G., Baker, J. N., Mack, J.W., Sung, L., Waldron, M. K., Reeve, B. B. (2019). The association of age, literacy, and race on completing patient-reported outcome measures in pediatric oncology. Quality of Life Research, 28(7), 1793–1801.
Sodergren, S. C., Husson, O., Robinson, J., Rohde, G. E., Tomaszewska, I. M., Vivat, B., Dyar, R., Darlington, A.S.; on behalf of the EORTC Quality of Life Group (2017). Systematic review of the health-related quality of life issues facing adolescents and young adults with cancer. Quality of Life Research, 26(7), 1659–1672.
Sodergren, S. C., Husson, O., Rohde, G. E., Tomaszewska, I. M., Vivat, B., Yarom, N., Griffiths, H., Darlington, A. S.; on behalf of the EORTC Quality of Life Group (2018). A life put on pause: An exploration of the health-related quality of life issues relevant to adolescents and young adults with cancer. Journal of Adolescent and Young Adult Oncology, 7(4), 453–464.
Sodergren, S. C., Husson, O., Rohde, G. E., Tomaszewska, I. M., Griffiths, H., Pessing, A., Yarom, N., Hooker, L., Din, A., Darlington, A.S.; on behalf of the EORTC Quality of Life Group (2018). Does age matter? A comparison of health-related quality of life issues of adolescents and young adults with cancer. Eur J Cancer Care (Engl)., 27(6), e12980.
Park, C. L., Wortmann, J. H., Hale, A. E., Cho, D., & Blank, T. O. (2014). Assessing quality of life in young adult cancer survivors: Development of the survivorship-related quality of life scale. Quality of Life Research, 23(8), 2213–2224.
Taylor, R. M., Fern, L. A., Solanki, A., Hooker, L., Carluccio, A., Pye, J., Jeans, D., Frere-Smith, T., Gibson, F., Barber, J., Raine, R., Stark, D., Feltbower, R., Pearce, S., Whelan, J.S. (2015). Development and validation of the BRIGHTLIGHT Survey, a patient-reported experience measure for young people with cancer. Health and Quality of Life Outcomes, 13, 107.
Riedl, D., Rothmund, M., Darlington, A. S., Sodergren, S., Crazzolara, R., de Rojas, T.; on behalf of the EORTC Quality of Life Group (2021). Rare use of patient-reported outcomes in childhood cancer clinical trials—A systematic review of clinical trial registries. European Journal of Cancer, 152, 90–99.
Rothmund, M., Lehmann, J., Moser, W., de Rojas, T., Sodergren, S. C., Darlington, A. S., & Riedl, D. (2022). Patient-reported outcomes are under-utilised in evaluating supportive therapies in paediatric oncology—A systematic review of clinical trial registries. Critical Reviews in Oncology/Hematology
Algurén, B., Ramirez, J. P., Salt, M., Sillett, N., Myers, S. N., Alvarez-Cote, A., Butcher, N.J., Caneo, L.F., Cespedes, J.A., Chaplin, J.E., Ng, K.C., García-García, J.J., Hazelzet, J.A., Klassen, A.F., Turquetto, A.L.R., Mew, E.J., Morris, M., Offringa, M., O'Meara, M., Papp, J.M., Rodrigo, C., Switaj, T.L., Valencia Mayer, C., Jenkins, K.J. (2021). Development of an international standard set of patient-centred outcome measures for overall paediatric health: A consensus process. Archives of Disease in Childhood, 106(9), 868–876.
Davis, E., Waters, E., Mackinnon, A., Reddihough, D., Graham, H. K., Mehmet-Radji, O., Boyd, R. (2006). Paediatric quality of life instruments: A review of the impact of the conceptual framework on outcomes. Developmental Medicine and Child Neurology, 48(4), 311–318.
Fayed, N., Schiariti, V., Bostan, C., Cieza, A., & Klassen, A. (2011). Health status and QOL instruments used in childhood cancer research: Deciphering conceptual content using World Health Organization definitions. Quality of Life Research, 20(8), 1247–1258.
Anthony, S. J., Selkirk, E., Sung, L., Klaassen, R. J., Dix, D., & Klassen, A. F. (2017). Quality of life of pediatric oncology patients: Do patient-reported outcome instruments measure what matters to patients? Quality of Life Research, 26(2), 273–281.
Klassen, A. F., Strohm, S. J., Maurice-Stam, H., & Grootenhuis, M. A. (2010). Quality of life questionnaires for children with cancer and childhood cancer survivors: A review of the development of available measures. Supportive Care in Cancer, 18(9), 1207–1217.
Rothmund, M., Meryk, A., Rumpold, G., Crazzolara, R., Sodergren, S. C., Darlington, A.S., Riedl, D. (2022). Lack of evidence for the content validity of patient-reported outcome measures (PROMs) assessing Health-Related Quality of Life (HRQOL) in children with cancer. submitted.
de Rojas, T., Neven, A., Towbin, A. J., Carceller, F., Bautista, F., Riedl, D., Sodergren, S., Darlington, A.S., Fernandez-Teijeiro, A., Moreno, L. (2020). Clinical research tools in pediatric oncology: Challenges and opportunities. Cancer and Metastasis Reviews, 39(1), 149–160.
Anthony, S. J., Selkirk, E., Sung, L., Klaassen, R. J., Dix, D., Scheinemann, K., & Klassen, A. F. (2014). Considering quality of life for children with cancer: A systematic review of patient-reported outcome measures and the development of a conceptual model. Quality of Life Research, 23(3), 771–789.
QLG E. (2021). Guidelines for developing questionnaire modules, 5th edn.
Moher, D., Shamseer, L., Clarke, M., Ghersi, D., Liberati, A., Petticrew, M., Shekelle, P., Stewart, L.A. & PRISMA-P Group (2015). Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Systematic Reviews, 4, 1.
Ouzzani, M., Hammady, H., Fedorowicz, Z., & Elmagarmid, A. (2016). Rayyan-a web and mobile app for systematic reviews. Systematic Reviews, 5(1), 210.
Michalos, A. C. (2014). Encyclopedia of quality of life and well-being research. Springer.
Barnett, A. (2014). Physical QOL. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research. Springer.
Hinds, P. S., Wang, J., Stern, E. D., Macpherson, C. F., Wharton, C. M., Okorosobo, R., Cheng, Y.I., Gross, H.E., Meany, H.J., Jacobs, S. (2017). Voices of children and adolescents on phase 1 or phase 2 cancer trials: A new trial endpoint? Cancer, 123(19), 3799–3806.
Li, H. C. W., Chung, O. K. J., & Chiu, S. Y. (2010). The impact of cancer on children’s physical, emotional, and psychosocial well-being. Cancer Nursing., 33(1), 47–54.
Momani, T. G., Mandrell, B. N., Gattuso, J. S., West, N. K., Taylor, S. L., & Hinds, P. S. (2015). Children’s perspective on health-related quality of life during active treatment for acute lymphoblastic leukemia: An advanced content analysis approach. Cancer Nursing, 38(1), 49–58.
Sibulwa, S., Chansa-Kabali, T., & Hapunda, G. (2019). “Every part of me has changed”-shared lived experiences of adolescents living with cancer in Zambia. Health Psychology Open, 6(1), 2055102919833537.
Sorgen, K. E., & Manne, S. L. (2002). Coping in children with cancer: Examining the goodness-of-fit hypothesis. Children’s Health Care, 31(3), 191–207.
Thorsteinsson, T., Schmiegelow, K., Thing, L. F., Andersen, L. B., Helms, A. S., Ingersgaard, M. V., Lindgren, L.H., Larsen, H.B. (2019). Classmates motivate childhood cancer patients to participate in physical activity during treatment: A qualitative study. European Journal of Cancer Care (England), 28(5), e13121.
Woodgate, R. L. (2008). Feeling states: A new approach to understanding how children and adolescents with cancer experience symptoms. Cancer Nursing, 31(3), 229–238.
Xie, A., Shan, Y., Niu, M. E., Chen, Y., & Wang, X. (2017). Experience and nursing needs of school-age children undergoing lumbar puncture during the treatment of acute lymphoblastic leukaemia: A descriptive and qualitative study. Journal of Clinical Nursing, 26(21–22), 3328–3335.
Tremolada, M., Axia, V., Pillon, M., Scrimin, S., Capello, F., & Zanesco, L. (2005). Parental narratives of quality of life in children with leukemia as associated with the placement of a central venous catheter. Journal of Pain and Symptom Management, 30(6), 544–552.
Han, J., Liu, J. E., Xiao, Q., Zheng, X. L., Ma, Y. H., & Ding, Y. M. (2011). The experiences and feelings of Chinese children living with leukemia: A qualitative study. Cancer Nursing, 34(2), 134–141.
McCaffrey, C. N. (2006). Major stressors and their effects on the well-being of children with cancer. Journal of Pediatric Nursing, 21(1), 59–66.
Nguyen, T. N., Nilsson, S., Hellström, A. L., & Bengtson, A. (2010). Music therapy to reduce pain and anxiety in children with cancer undergoing lumbar puncture: A randomized clinical trial. Journal of Pediatric Oncology Nursing, 27(3), 146–155.
Mitamura, C., Reuman, L., & Tugade, M. (2014). Resilience. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research. Springer.
Wills-Herrera, E. (2014). Self-esteem. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research. Springer.
Kiely, K. M. (2014). Cognitive function. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research. Springer.
Pinquart, M. (2014). Social competence. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research. Springer.
Zhou, E. S. (2014). Social support. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research. Springer.
Ang, S. H., Koh, S. S. L., Lee, X. H. H. T., & Shorey, S. (2018). Experiences of adolescents living with cancer: A descriptive qualitative study. Journal of Child Health Care, 22(4), 532–544.
Gibson, F., Aldiss, S., Taylor, R. M., Maguire, R., McCann, L., Sage, M., Kearney, N (2010). Utilization of the Medical Research Council evaluation framework in the development of technology for symptom management: The ASyMS-YG Study. Cancer Nursing, 33(5), 343–352.
Sposito, A. M., Silva-Rodrigues, F. M., VeC, S., Pfeifer, L. I., de Lima, R. A., & Nascimento, L. C. (2015). Coping strategies used by hospitalized children with cancer undergoing chemotherapy. Journal of Nursing Scholarship, 47(2), 143–151.
Cavicchioli, A. C., Menossi, M. J., & de Lima, R. A. (2007). Cancer in children: The diagnostic itinerary. Revista Latino-Americana de Enfermagem, 15(5), 1025–1032.
Daniel, L. C., Schwartz, L. A., Mindell, J. A., Tucker, C. A., & Barakat, L. P. (2016). Initial validation of the sleep disturbances in pediatric cancer model. Journal of Pediatric Psychology, 41(6), 588–599.
Fleming, C. A., Cohen, J., Murphy, A., Wakefield, C. E., Cohn, R. J., & Naumann, F. L. (2015). Parent feeding interactions and practices during childhood cancer treatment: A qualitative investigation. Appetite, 89, 219–225.
Forgeron, P. A., Finley, G. A., & Arnaout, M. (2006). Pediatric pain prevalence and parents’ attitudes at a cancer hospital in Jordan. Journal of Pain and Symptom Management, 31(5), 440–448.
Griffiths, M., Schweitzer, R., & Yates, P. (2011). Childhood experiences of cancer: An interpretative phenomenological analysis approach. Journal of Pediatric Oncology Nursing, 28(2), 83–92.
Lam, K. K. W., Li, W. H. C., Chung, J. O. K., Ho, K. Y., Xia, W., Cheung, A. T., Chiu, S.Y., Lam, H.S., Chan, G.C.F. (2020). Promoting physical activity among children with cancer through an integrated experiential training programme with coaching: A qualitative study. Patient Education and Counseling, 103(6), 1230–1236.
Kim, H., Zhou, E. S., Chevalier, L., Lun, P., Davidson, R. D., Pariseau, E. M., Long, K.A. (2020). Parental behaviors, emotions at bedtime, and sleep disturbances in children with cancer. Journal of Pediatric Psychology, 45(5), 550–560.
Sisk, B. A., Keenan, M., Schulz, G. L., Kaye, E., Baker, J. N., Mack, J. W., DuBois, J.M. (2022). Interdependent functions of communication with adolescents and young adults in oncology. Pediatric Blood & Cancer, 69(4), e29588.
Fortier, M. A., Batista, M. L., Wahi, A., Kain, A., Strom, S., & Sender, L. S. (2013). Illness uncertainty and quality of life in children with cancer. Journal of Pediatric Hematology/oncology, 35(5), 366–370.
Solans, M., Pane, S., Estrada, M. D., Serra-Sutton, V., Berra, S., Herdman, M., Alonso, J., Rajmil, L. (2008). Health-related quality of life measurement in children and adolescents: A systematic review of generic and disease-specific instruments. Value Health., 11(4), 742–764.
Teckle, P., Peacock, S., McTaggart-Cowan, H., van der Hoek, K., Chia, S., Melosky, B., Gelmon, K. (2011). The ability of cancer-specific and generic preference-based instruments to discriminate across clinical and self-reported measures of cancer severities. Health and Quality of Life Outcomes, 9, 106.
Knight, D., Hensley, V. R., & Waters, B. (1988). Validation of the Children’s Depression Scale and the Children’s Depression Inventory in a prepubertal sample. Journal of Child Psychology and Psychiatry, 29(6), 853–863.
Patrick, D. L., Burke, L. B., Gwaltney, C. J., Leidy, N. K., Martin, M. L., Molsen, E., Ring, L. (2011). Content validity–Establishing and reporting the evidence in newly developed patient-reported outcomes (PRO) instruments for medical product evaluation: ISPOR PRO good research practices task force report: Part 1–Eliciting concepts for a new PRO instrument. Value Health., 14(8), 967–977.
Patrick, D. L., Burke, L. B., Gwaltney, C. J., Leidy, N. K., Martin, M. L., Molsen, E., Ring, L. (2011). Content validity–establishing and reporting the evidence in newly developed patient-reported outcomes (PRO) instruments for medical product evaluation: ISPOR PRO Good Research Practices Task Force report: Part 2—Assessing respondent understanding. Value Health., 14(8), 978–988.
Wayant, C., Manquen, J., Wendelbo, H., Kerr, N., Crow, M., Goodell, J., Tricco, A. C., Mack, J. W., Hellman, C., & Vassar, M. (2021). Identification of evidence for key positive psychological constructs in pediatric and adolescent/young adult patients with cancer: A scoping review. Journal of Adolescent and Young Adult Oncology, 10(3), 247–259.
Funding
Open access funding provided by University of Innsbruck and Medical University of Innsbruck. This study was supported by the European Organisation for Research and Treatment of Cancer Quality of Life Group (EORTC QLG). The Grant (Nos. 002–2020) was awarded to David Riedl and Samantha Sodergren.
Author information
Authors and Affiliations
Consortia
Contributions
MR, SS, TdR, ASD and DR contributed to conceptualization of the review and MR and DR contributed the methodology. Formal analysis and investigation was conducted by MR, DR, SS, GR, TdR GP, GA, and JM. MR and DR wrote the original draft and prepared the manuscript, while SS, GR, ASD, MR and DR reviewed and edited the manuscript. Funding was acquired by SS and DR. SS, AM, ASD and DR supervised the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Rothmund, M., Sodergren, S., Rohde, G. et al. Updating our understanding of health-related quality of life issues in children with cancer: a systematic review of patient-reported outcome measures and qualitative studies. Qual Life Res 32, 965–976 (2023). https://doi.org/10.1007/s11136-022-03259-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-022-03259-z