Abstract
Objectives
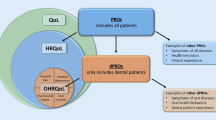
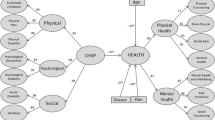
This paper critically examines the different models of oral health aimed at representing oral health-related quality of life (OHRQoL) and explores the extent to which such models changed conceptually to accommodate current theories and empirical knowledge of oral function, impairment and disability.
Methods
A critical synthesis of the existing literature based on a comprehensive yet non-systematic review using Ovid-MEDLINE was performed. Full text of manuscripts available on models of oral health and OHRQoL published in English between 1 January 1950 and 30 June 2013 were identified.
Results
Nineteen manuscripts were identified presenting and discussing various models of oral health and OHRQoL that are predominantly negative and linear. These models are mostly based on sick role-related theories and do not readily accommodate the biopsychosocial theories of oral health. Alternative portrayals have emerged to include positive behaviours and adaptive strategies dynamically, but have yet to influence patient care and the development of subjective OHRQoL indicators.
Conclusion
Despite the multitude of graphical representations of concepts, dental research has remained somewhat ‘linear’ in portraying the consequences of oral diseases as a one-way street. Although the conceptualization of oral health has evolved in the past 30 years, dental research still refers to it as the absence of disease in more than half a dozen models of OHRQoL focused mostly on dysfunction and disability.









Similar content being viewed by others
Notes
Disability can encompass any or all of: impairment of body structure or function; limitation in activities; or restriction in participation. Within limitations and restrictions, disability is seen as a gap between an individual’s capabilities and the demands of the environment. Impairments can occur at the level of organs, tissues and cells, and at the subcellular level [48].
Abbreviations
- CHMS:
-
Canadian Health Measures Survey
- ICF:
-
International Classification of Functioning, Disability and Health
- ICIDH:
-
International Classification of Impairments, Disability and Handicap
- OHRQoL:
-
Oral health-related quality of life
- OHIP:
-
Oral Health Impact Profile
- WHO:
-
World Health Organization
References
Davis, H. B. (1996). The quality of life improvement model: A means to guide practice. Critical Care in Nursing Quarterly, 19, 85–90.
Gift, H. C. (1997). Oral health outcome research—Challenges and opportunities. In G. D. Slade (Ed.), Measuring oral health and quality of life (pp. 25–46). Chapel Hill: University of North Carolina, Dental Ecology.
Cohen, L. K. (1997). The emerging field of oral health related quality of life outcomes research. In G. D. Slade (Ed.), Measuring oral health and quality of life (pp. 1–10). Chapel Hill: University of North Carolina, Dental Ecology.
Brondani, M. A., & MacEntee, M. I. (2007). The concept of validity in the sociodental indicators. Community Dentistry and Oral Epidemiology, 32, 1–7.
Bronfenbrenner, U. (1979). The ecology of human development: Experiments by nature and design. Cambridge, MA: Harvard University Press.
Alvi, S. A. (1997). Ecology of career development in Indonesia: Major macrosystem influences. International Journal of Advanced Counselling, 19, 303–311.
McLaren, L., & Hawe, P. (2005). Ecological perspectives in health research. Journal of Epidemiological Community Health, 59, 6–14.
Guttman, L. (1954). A new approach to factor analysis: The radix. In P. R. Lazarsfeld (Ed.), Mathematical thinking in the social sciences (pp. 258–348). Glencoe, IL: Free Press.
Tracey, T. J., & Rounds, J. (1996). The spherical representation of vocational interests. Journal of Vocational Behaviour, 48, 3–41.
Brondani, M. (2010). Students’ reflective activity within a community-service learning dental module. Journal of Dental Education, 74, 628–636.
VanderVen, K., & Torre, C. A. (1999). A dynamical systems perspective on mediating violence in schools: Emergent roles of child and youth care workers. Child & Youth Care Forum, 28, 411–436.
Shepherd, S. A., & Thomas, I. M. (1982). Marine invertebrates of Southern Australia. Adelaide: South Australian Government Printer.
United States Department of Agriculture. (2011). Available at: http://www.mypyramid.gov/pyramid/index.html. Accessed February 9, 2011.
Hochbaum, G., Sorenson, S., James, R., & Lorig, K. (1992). Theory in health education practice. Health and Education Quarterly, 19, 295–313.
Slade, C. D. (Ed.). (1997). Measuring oral health and quality of life (pp. 3–5). Chapel Hill: University of North Carolina, Dental Ecology.
Locker, D., & Quiñonez, C. (2011). To what extent do oral disorders compromise the quality of life? Community Dentistry and Oral Epidemiology, 39, 3–11.
Brondani, M. A., Bryant, S. R., & MacEntee, M. I. (2007). Elders assessment of an evolving model of oral health. Gerondontology, 24, 189–195.
Levasseur, M., Desrosiers, J., & Tribble, D. S. C. (2007). Comparing the disability creation process and international classification of functioning, disability and health models. Canadian Journal of Occupational Therapy, 74, 233–242.
Capra, F. (1982). The turning point: Science, society and the rising culture. New York: Simon & Schuster Publisher.
Locker, D. (1988). Measuring oral health: A conceptual framework. Community Dental Health, 5, 3–18.
World Health Organization. (1980). International classification of impairments, disabilities and handicaps. Geneva: World Health Organization.
Gray, D. B., & Hendershot, G. E. (2000). The ICIDH-2: Development of new era of outcomes research. Archives of Physical Medical Rehabilitation, 81, S10–S14.
Benyamini, Y., Leventhal, H., & Leventhal, E. A. (2004). Self-rated oral health as an independent predictor of self-rated general health, self-esteem, and life satisfaction. Social Science and Medicine, 59(5), 1109–1116.
Jones, J. A., Kressin, N. R., Miller, D. R., Orner, M. B., Garcia, R. I., & Spiro, A., I. I. I. (2004). Comparison of patient-based oral health outcome measures. Quality of Life Research, 13, 975–985.
Maida, C. A., Marcus, M., Spolsky, V. W., Wang, Y., & Liu, H. (2013). Socio-behavioral predictors of self-reported oral health-related quality of life. Quality of Life Research, 22(3), 559–566.
World Health Organization. (2009). Oral health. Available at: http://www.who.int/topics/oral_health/en. Retrieved September 2, 2009.
Dolan, T. (1993). Identification of appropriate outcomes for an ageing population. Special Care in Dentistry, 13, 35–39.
Locker, D. (1997). Subjective oral health status indicators. In G. D. Slade (Ed.), Measuring oral health and quality of life (pp. 105–112). Chapel Hill: University of North Carolina, Dental Ecology.
Allison, P. J., Locker, D., & Feine, J. S. (1997). Quality of life: A dynamic construct. Social Science and Medicine, 54, 221–230.
Gregory, J., Gibson, B., & Robinson, P. G. (2005). Variation and change in the meaning of oral health related quality of life: A ‘grounded’ systems approach. Social Science and Medicine, 60(8), 1859–1868.
MacEntee, M. I. (2006). An existential model of oral health from evolving views on health, function and disability. Community Dental Health, 23, 5–14.
Adulyanon, S., & Sheiham, A. (1997). Oral impacts on daily performances. In G. D. Slade (Ed.), Measuring oral health and quality of life (pp. 151–160). Chapel Hill: University of North Carolina, Dental Ecology.
Cushing, A. M., Sheiham, A., & Maizels, J. (1986). Developing socio-dental indicators—The social impacts of dental disease. Community Dental Health, 3, 3–17.
Gilbert, G. H., Duncan, R. P., Heft, M. W., Dolan, T. A., & Vogel, W. B. (1998). Multi-dimensionality of oral health in dentate adults. Medical Care, 36, 988–1001.
Broder, H. L., Slade, G., Caine, R., & Reisine, S. (2000). Perceived impact of oral health conditions among minority adolescents. Journal of Public Health Dentistry, 60, 189–192.
Kressin, N., Spiro, A., Bosse, R., Gracia, R., & Kazis, L. (1996). Assessing oral health related quality of life: Findings from a normative aging study. Medical Care, 34, 416–427.
Williams, K. B., Gadbury-Amyot, C. C., Bray, K. K., Manne, D., & Collins, P. (1998). Oral health-related quality of life: A model for dental hygiene. Journal of Dental Hygiene, 72(2), 19–26.
Wilson, I. B., & Cleary, P. D. (1995). Linking clinical variables with health-related quality of life: A conceptual model of patient outcomes. Journal of the American Medical Association, 273, 59–65.
Locker, D., & Gibson, B. (2005). Discrepancies between self-ratings of and satisfaction with oral health in two older adult populations. Community Dentistry and Oral Epidemiology, 33, 280–288.
Laing, R. D. (1971). The politics of the family and other essays. London: Tavistock Publications.
Gerrie, N. F. (1947). Standards of dental care in public health programs for children. American Journal of Public Health, 37, 1317–1321.
McCollum, B. B. (1943). Oral diagnosis. Journal of the American Dental Association, 30, 1218–1233.
Nuttall, N. M., Slade, G. D., Sanders, A. E., Steele, J. G., Allen, P. F., & Lahti, S. (2006). An empirically derived population-response model of the short form of the oral health impact profile. Community Dentistry and Oral Epidemiology, 34, 18–24.
Slade, G. D., & Spencer, A. J. (1994). Development and evaluation of oral health impact profile. Community Dental Health, 11, 3–11.
Brondani, M. (2010). The voice of the elderly in accepting alternative perspectives on oral health. Community Dental Health, 27, 139–144.
Hunt, S. M. (1997). The problem of quality of life. Quality of Life Research, 6, 205–212.
Parsons, T. (1951). The social system (pp. 19–33). New York, NY: Free Press.
World Health Organization. (2001). International classification of functioning, disabilities and health. Geneva: World Health Organization.
Stamm, T. A., Cieza, A., Coenen, M., Machold, K. P., Nell, V. P. K., Smolen, J. S., et al. (2005). Validating the international classification of functioning, disability and health comprehensive core set for rheumatoid arthritis from the patient perspective: A qualitative study. Arthritis and Rheumatism, 53, 431–439.
Üstün, B., Chatterji, S., Rehm, J., Kennedy, C., Prieto, L., & Epping-Jordan, J. (2010). World Health Organization Disability Assessment Schedule II (WHO DAS II): Development, psychometric testing and applications. Geneva: World Health Organization.
Ingstad, B., & Reynolds, W. (1995). Disability and culture. Berkeley: University of California Press.
Ueda, S., & Okawa, Y. (2003). The subjective dimension of functioning and disability: What is it and what is it for? Disability Rehabilitation, 25, 596–601.
MacEntee, M. I., Hole, R., & Stolar, E. (1997). The significance of the mouth in old age. Social Science and Medicine, 45(9), 1449–1458.
Moody, D. L., Sindre, G., Brasethvik, T., & Solvberg, A. (2003). Evaluating the quality of information models: Empirical testing of a conceptual model quality framework. In Proceedings of the 25th international conference on software engineering (pp. 295–305). Portland, Oregon. Available at: http://doi.ieeecomputersociety.org/10.1109/ICSE.2003.1201209. Accessed December 09, 2011.
Finch, H., & Lewis, J. (Eds.). (2003). Focus group. In: Qualitative research practice: A guide for social science students and researchers (pp. 15–45). Thousand Oaks, CA: Sage.
Brondani, M. A., O’Neill, B., Bryant, S. R., & MacEntee, M. I. (2008). Using written vignettes in focus groups among older adults to discuss oral health as a sensitive topic. Qualitative Health Research, 18, 1145–1153.
Green, L. W., & Kreuter, M. M. (Eds.). (1999). Health promotion planning: An educational and ecological approach (3rd ed.). Mountain View: Mayfield.
Potvin, L., Gendron, S., Bilodeau, A., & Chabot, P. (2005). Integrating social theory into public health practice. American Journal of Public Health, 95(4), 591–595.
Statistics Canada. (2012). Oral Health Component of the Canadian Health Measures Survey. 2011. Available at: http://www.hc-sc.gc.ca/ahc-asc/branch-dirgen/fnihb-dgspni/ocdo-bdc/project-eng.php. Accessed July 12, 2012.
Acknowledgments
The authors would like to also express their gratitude to Dr. S. Ross Bryant for his constant encouragement and challenging ideas. A special thanks goes to Jaesung Seo, who was a Master’s Student under the supervision of both authors between 2009 and 2011 and offered a critical review on the concept of oral health and quality of life, as well as validity theory.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brondani, M.A., MacEntee, M.I. Thirty years of portraying oral health through models: what have we accomplished in oral health-related quality of life research?. Qual Life Res 23, 1087–1096 (2014). https://doi.org/10.1007/s11136-013-0541-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-013-0541-3