ABSTRACT
Purpose
Present investigation deals with an extensive approach incorporating in vitro and in vivo experimentation to treat chronic osteomyelitis, using hydroxyapatite porous scaffolds.
Materials and Methods
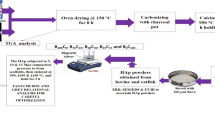
Hydroxyapatite was synthesized in the laboratory by wet chemical method, different porous scaffolds have been fabricated. In vitro studies include variation of porosity with interconnectivity, pore-drug interfacial studies by SEM-EDAX and drug elution studies (by HPLC) both in contact with PBS and SBF at ~37°C. In vivo trials were based on experimental osteomyelitis in rabbit model induced in tibia by Staphylococcus aureus. Characterizations included observation of histopathology, radiology and estimation of drug in both bone and serum for 42 days by HPLC method and subsequent bone-biomaterial interface by SEM.
Results
It was established that lower pore percentage with a distribution of mainly micro-pores were found to be superior over the higher pore percentage both in vitro and in vivo. The criteria was matched with the 50N50H samples which had 50–55% porosity with an average pore size ~110 μm, having higher interconnectivity (10–100 μm), moderately high adsorption efficiency (~50%) when loaded with CFS (drug combinations consisting of irreversible b-lactamase inhibitor and b-lactam antibiotic). CFS release from HAp implants were faster in PBS than SBF. Further, both the results of in vitro and in vivo drug elution after 42 days showed release higher than minimum inhibitory concentration of CFS against Staphylococcus aureus. In vivo studies also proved the superiority of CFS loaded HAp implants than parenteral group based on eradication of infection and new bone formation.
Conclusions
HAp based porous scaffold loaded with CFS and designed porosity (in terms of micro- and macro-porosity, interconnectivity) was found to be an ideal delivery system which could locally, sustainably release the composite antibiotic in reliable manner both in terms of in vitro drug elution behaviour in contact with SBF and in vivo animal trial.












Similar content being viewed by others
Abbreviations
- ASTM:
-
American Society for Testing and Materials
- AUC:
-
Area under the curve
- CFA:
-
Colony-forming unit
- CFS:
-
Combination of CFT and SUL drug
- CFT:
-
Ceftriaxone sodium
- FESEM:
-
Field emission scanning electron microscopy
- FTIR:
-
Fourier-transformed infrared spectroscopy
- HAp:
-
Hydroxyapatite
- HPLC:
-
High performance liquid chromatography
- MIC:
-
Minimum inhibitory concentration
- PBS:
-
Phosphate buffered saline
- PMMA:
-
Poly-methyl methacrylate
- RBC:
-
Red blood cell
- SBF:
-
Simulated body fluid
- SEM-EDAX:
-
Scanning electron microscopy-Energy dispersive analysis of X-ray
- SUL:
-
Sulbactam sodium
- XRD:
-
X-ray diffraction
REFERENCES
Nandi SK, Mukherjee P, Roy S, Kundu B, De DK, Basu D. Local antibiotic delivery systems for the treatment of osteomyelitis—a review. Mater Sci Engg C. 2009;29:2478–85.
Soundrapandian C, Datta S, Sa B. Drug-eluting implants for osteomyelitis. Crit Rev Ther Drug Carrier Syst. 2007;24:493–545.
Rao N, Lipsky BA. Optimising antimicrobial therapy in diabetic foot infections. Drugs. 2007;67:195–214.
Conterno LO, da Silva Filho CR. Antibiotics for treating chronic osteomyelitis in adults. Cochrane Database Syst Rev:CD004439 (2009).
Houghton TJ, Tanaka KS, Kang T, Dietrich E, Lafontaine Y, Delorme D et al. Linking bisphosphonates to the free amino groups in fluoroquinolones: preparation of osteotropic prodrugs for the prevention of osteomyelitis. J Med Chem. 2008;51:6955–69.
Soundrapandian C, Sa B, Datta S. Organic–inorganic composites for bone drug delivery. AAPS PharmSciTech (2009).
Walenkamp GH, Kleijn LL, de Leeuw M. Osteomyelitis treated with gentamicin-PMMA beads: 100 patients followed for 1–12 years. Acta Orthop Scand. 1998;69:518–22.
Neut D, van de Belt H, van Horn JR, van der Mei HC, Busscher HJ. Residual gentamicin-release from antibiotic-loaded polymethylmethacrylate beads after 5 years of implantation. Biomaterials. 2003;24:1829–31.
Kilian O, Hossain H, Flesch I, Sommer U, Nolting H, Chakraborty T et al. Elution kinetics, antimicrobial efficacy, and degradation and microvasculature of a new gentamicin-loaded collagen fleece. J Biomed Mater Res B Appl Biomater. 2009;90:210–22.
Colilla M, Manzano M, Vallet-Regi M. Recent advances in ceramic implants as drug delivery systems for biomedical applications. Int J Nanomedicine. 2008;3:403–14.
Nandi SK, Kundu B, Ghosh SK, Mandal TK, Datta S, De DK et al. Cefuroxime-impregnated calcium phosphates as an implantable delivery system in experimental osteomyelitis. Ceram Int. 2009;35:1367–76.
Bose S, Saha SK. Synthesis and characterization of hydroxyapatite nanopowders by emulsion technique. Chem Mater. 2003;15:4464–9.
Wu Y, Bose S. Nanocrystalline hydroxyapatite: micelle templated synthesis and characterization. Langmuir. 2005;21:3232–4.
Palmer LC, Newcomb CJ, Kaltz SR, Spoerke ED, Stupp SI. Biomimetic systems for hydroxyapatite mineralization inspired by bone and enamel. Chem Rev. 2008;108:4754–83.
Al-Sokanee ZN, Toabi AA, Al-Assadi MJ, Alassadi EA. The drug release study of ceftriaxone from porous hydroxyapatite scaffolds. AAPS PharmSciTech. 2009;10:772–9.
Bose S, Banerjee A, Dasgupta S, Bandyopadhyay A. Synthesis, processing, mechanical and biological property characterization of hydroxyapatite whisker-reinforced hydroxyapatite composites. J Am Ceram Soc. 2009;92:323–30.
Sedrakyan S, Zhou ZY, Perin L, Leach K, Mooney D, Kim TH. Tissue engineering of a small hand phalanx with a porously casted polylactic acid-polyglycolic acid copolymer. Tissue Eng. 2006;12:2675–83.
Yoshikawa H, Tamai N, Murase T, Myoui A. Interconnected porous hydroxyapatite ceramics for bone tissue engineering. J R Soc Interface. 2009;6 Suppl 3:S341–348.
Xue W, Bandyopadhyay A, Bose S. Polycaprolactone coated porous tricalcium phosphate scaffolds for controlled release of protein for tissue engineering. J Biomed Mater Res Part B Appl Biomater. 2009;91:831–8.
Xue W, Bandyopadhyay A, Bose S. Mesoporous calcium silicate for controlled release of bovine serum albumin protein. Acta Biomater. 2009;5:1686–96.
Mastrogiacomo M, Scaglione S, Martinetti R, Dolcini L, Beltrame F, Cancedda R et al. Role of scaffold internal structure on in vivo bone formation in macroporous calcium phosphate bioceramics. Biomaterials. 2006;27:3230–7.
Turco G, Marsich E, Bellomo F, Semeraro S, Donati I, Brun F et al. Alginate/Hydroxyapatite biocomposite for bone ingrowth: a trabecular structure with high and isotropic connectivity. Biomacromolecules. 2009;10:1575–83.
Oudadesse H, Derrien AC, Lucas-Girot A. Statistical experimental design for studies of porosity and compressive strength in composite materials applied as biomaterials. Eur Phys J Appl Phys. 2005;31:217–23.
Chanda A, Singha Oy R, Xue W, Bose S, Bandyopadhyay A. Bone cell-materials interaction on alumina ceramics with different grain sizes. Mater Sci Engg C. 2009;29:1201–6.
Bush K, Mobashery S. How beta-lactamases have driven pharmaceutical drug discovery. From mechanistic knowledge to clinical circumvention. Adv Exp Med Biol. 1998;456:71–98.
Bush K. The impact of beta-lactamases on the development of novel antimicrobial agents. Curr Opin Investig Drugs. 2002;3:1284–90.
Caron F, Gutmann L, Bure A, Pangon B, Vallois JM, Pechinot A et al. Ceftriaxone-sulbactam combination in rabbit endocarditis caused by a strain of Klebsiella pneumoniae producing extended-broad-spectrum TEM-3 beta-lactamase. Antimicrob Agents Chemother. 1990;34:2070–4.
Foulds G, Stankewich JP, Marshall DC, O’Brien MM, Hayes SL, Weidler DJ et al. Pharmacokinetics of sulbactam in humans. Antimicrob Agents Chemother. 1983;23:692–9.
Sinha MK, Sen PS, Basu D, Chattopadhyay S, Basu MK. An improved process for the synthesis of hydroxyapatite powder useful for biomedical applications. In CGCRI (ed.), India, 1998.
Landi E, Tampieri A, Celotti G, Sprio S. Densification behaviour and mechanisms of synthetic hydroxyapatites. J Eur Ceram Soc. 2000;20:2377–87.
D. Basuand M.K. Sinha. A process for the production of improved porous ocular implants and improved porous ocular implants produced thereby. In CGCRI (ed.), India, 2006.
Kokubo T, Kushitani H, Sakka S, Kitsugi T, Yamamuro T. Solutions able to reproduce in vivo surface-structure changes in bioactive glass-ceramic A-W. J Biomed Mater Res. 1990;24:721–34.
Norden CW. Experimental osteomyelitis. I. A description of the model. J Infect Dis. 1970;122:410–8.
Weng W, Baptista JL. Sol-gel derived porous hydroxyapatite coatings. J Mater Sci. 1998;9:159–63.
Choi D, Marra KG, Kumta PN. Chemical synthesis of hydroxyapatite/poly(e-caprolactone) composites. Mater Res Bull. 2004;39:417–32.
Narasaraju TSB, Phebe DE. Some physico-chemical aspects of hydroxylapatite. J Mater Sci. 1996;31:1–21.
Suetsugu Y, Shimoya I, Tanaka J. Configuration of carbonate ions in apatite structure determined by polarized infrared spectroscopy. J Am Ceram Soc. 1998;81:746–8.
Rokusek D, Davitt C, Bandyopadhyay A, Bose S, Hosick HL. Interaction of human osteoblasts with bioinert and bioactive ceramic substrates. J Biomed Mater Res. 2005;75:588–94.
Banerjee A, Bandyopadhyay A, Bose S. Hydroxyapatite nanopowders: synthesis, densification and cell-materials interaction. Mater Sci Engg C. 2007;27:729–35.
Ginebra MP, Traykova T, Planell JA. Calcium phosphate cements as bone drug delivery systems: a review. J Control Release. 2006;113:102–10.
Krajewski A, Ravaglioli A, Roncari E, Pinasco P, Montanari L. Porous ceramic bodies for drug delivery. J Mater Sci. 2000;11:763–71.
Hasegawa M, Sudo A, Komlev VS, Barinov SM, Uchida A. High release of antibiotic from a novel hydroxyapatite with bimodal pore size distribution. J Biomed Mater Res B Appl Biomater. 2004;70:332–9.
Sanchez E, Baro M, Soriano I, Perera A, Evora C. In vivo–in vitro study of biodegradable and osteointegrable gentamicin bone implants. Eur J Pharm Biopharm. 2001;52:151–8.
Tampieri A, Celotti G, Sprio S, Mingazzini C. Characteristics of synthetic hydroxyapatites and attempts to improve their thermal stability. Mater Chem Phys. 2000;64:54–61.
Netz DJ, Sepulveda P, Pandolfelli VC, Spadaro AC, Alencastre JB, Bentley MV et al. Potential use of gelcasting hydroxyapatite porous ceramic as an implantable drug delivery system. Int J Pharm. 2001;213:117–25.
Itokazu M, Yang W, Aoki T, Ohara A, Kato N. Synthesis of antibiotic-loaded interporous hydroxyapatite blocks by vacuum method and in vitro drug release testing. Biomaterials. 1998;19:817–9.
Pham HH, Luo P, Genin F, Dash AK. Synthesis and characterization of hydroxyapatite-ciprofloxacin delivery systems by precipitation and spray drying technique. AAPS PharmSciTech. 2002;3:E1.
Eggli PS, Muller W, Schenk RK. Porous hydroxyapatite and tricalcium phosphate cylinders with two different pore size ranges implanted in the cancellous bone of rabbits. A comparative histomorphometric and histologic study of bony ingrowth and implant substitution. Clin Orthop Relat Res. 1988;232:127–38.
Kuhne JH, Bartl R, Frisch B, Hammer C, Jansson V, Zimmer M. Bone formation in coralline hydroxyapatite. Effects of pore size studied in rabbits. Acta Orthop Scand. 1994;65:246–52.
Rodriguez-Lorenzo LM, Vallet-Regi M, Ferreira JM. Colloidal processing of hydroxyapatite. Biomaterials. 2001;22:1847–52.
Bodhak S, Bose S, Bandyopadhyay A. Role of surface charge and wettability on early stage mineralization and bone cell-materials interactions of polarized hydroxyapatite. Acta Biomater. 2009;5:2178–88.
Bodhak S, Bose S, Bandyopadhyay A. Electrically polarized HAp-coated Ti: in vitro bone cell–material interactions. Acta Biomater. 2010;6:641–51.
Vallet-Regi M, Balas F, Colilla M, Manzano M. Drug confinement and delivery in ceramic implants. Drug Metab Lett. 2007;1:37–40.
Vallet-Regí M, Ruiz-González L, Izquierdo-Barba I, González-Calbet JM. Revisiting silica based ordered mesoporous materials: medical applications. J Mater Chem. 2006;16:26–31.
Lebugle A, Rodrigues A, Bonnevialle P, Voigt JJ, Canal P, Rodriguez F. Study of implantable calcium phosphate systems for the slow release of methotrexate. Biomaterials. 2002;23:3517–22.
Burgos AE, Belchior JC, Sinisterra RD. Controlled release of rhodium (II) carboxylates and their association complexes with cyclodextrins from hydroxyapatite matrix. Biomaterials. 2002;23:2519–26.
Stigter M, Bezemer J, de Groot K, Layrolle P. Incorporation of different antibiotics into carbonated hydroxyapatite coatings on titanium implants, release and antibiotic efficacy. J Control Release. 2004;99:127–37.
Rai B, Teoh SH, Ho KH. An in vitro evaluation of PCL-TCP composites as delivery systems for platelet-rich plasma. J Control Release. 2005;107:330–42.
Higuchi T. Mechanism of sustained-action medication. Theoretical analysis of rate of release of solid drugs dispersed in solid matrices. J Pharm Sci. 1963;52:1145–9.
Joosten U, Joist A, Frebel T, Brandt B, Diederichs S, von Eiff C. Evaluation of an in situ setting injectable calcium phosphate as a new carrier material for gentamicin in the treatment of chronic osteomyelitis: studies in vitro and in vivo. Biomaterials. 2004;25:4287–95.
Korkusuz F, Korkusuz P, Eksioglu F, Gursel I, Hasirci V. In vivo response to biodegradable controlled antibiotic release systems. J Biomed Mater Res. 2001;55:217–28.
Girschick HJ, Zimmer C, Klaus G, Darge K, Dick A, Morbach H. Chronic recurrent multifocal osteomyelitis: what is it and how should it be treated? Nat Clin Pract. 2007;3:733–8.
Shrivastava SM, Saurabh S, Rai D, Dwivedi VK, Chaudhary M. In vitro microbial efficacy of sulbactomax: a novel fixed dose combination of ceftriaxone sulbactam and ceftriaxone alone. Curr Drug Ther. 2009;4:73–7.
Tamai N, Myoui A, Tomita T, Nakase T, Tanaka J, Ochi T et al. Novel hydroxyapatite ceramics with an interconnective porous structure exhibit superior osteoconduction in vivo. J Biomed Mater Res. 2002;59:110–7.
Castro C, Sanchez E, Delgado A, Soriano I, Nunez P, Baro M et al. Ciprofloxacin implants for bone infection. In vitro–in vivo characterization. J Control Release. 2003;93:341–54.
ACKNOWLEDGEMENTS
The authors wish to express their sincere thanks for the financial support by Department of Science and Technology, India [T.1 (7)/TIFA/2006-CGCRI] and the Director, CGCRI, India and Vice Chancellor, West Bengal University of Animal and Fishery Sciences, Kolkata, India for their generous and kind support to this work. All the personnel related to the characterization of the materials are sincerely acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kundu, B., Soundrapandian, C., Nandi, S.K. et al. Development of New Localized Drug Delivery System Based on Ceftriaxone-Sulbactam Composite Drug Impregnated Porous Hydroxyapatite: A Systematic Approach for In Vitro and In Vivo Animal Trial. Pharm Res 27, 1659–1676 (2010). https://doi.org/10.1007/s11095-010-0166-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-010-0166-y