Abstract
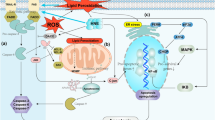
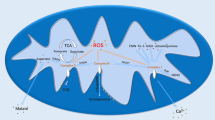
Cerebral ischemic injury is a leading cause of death and long-term disability throughout the world. Peroxisome proliferator-activated receptor gamma (PPAR-ɣ) is a ligand-activated nuclear transcription factor that is a member of the PPAR family. PPAR-ɣ has been shown in several in vitro and in vivo models to prevent post-ischemic inflammation and neuronal damage by negatively controlling the expression of genes modulated by cerebral ischemic injury, indicating a neuroprotective effect during cerebral ischemic injury. A extensive literature review of PubMed, Medline, Bentham, Scopus, and EMBASE (Elsevier) databases was carried out to understand the nature of the extensive work done on the mechanistic role of Peroxisome proliferator activated receptor gamma and its modulation in Cerebral ischemic injury. PPAR-ɣ can interact with specific DNA response elements to control gene transcription and expression when triggered by its ligand. It regulates lipid metabolism, improves insulin sensitivity, modulates antitumor mechanisms, reduces oxidative stress, and inhibits inflammation. This review article provides insights on the current state of research into the neuroprotective effects of PPAR-ɣ in cerebral ischemic injury, as well as the cellular and molecular mechanisms by which these effects are modulated, such as inhibition of inflammation, reduction of oxidative stress, suppression of pro-apoptotic production, modulation of transcription factors, and restoration of injured tissue through neurogenesis and angiogenesis.




Similar content being viewed by others
References
Lee R, Lee M, Wu C, Couto E Silva A et al (2018) Cerebral ischemia and neuroregeneration. Neural Regen Res 13(3):373–385. https://doi.org/10.4103/1673-5374.228711
French BR, Boddepalli RS, Govindarajan R (2016) Acute ischemic stroke: current status and future directions. Mo Med 113(6):480–486
Chugh C (2019) Acute ischemic stroke: management approach. Indian J Crit Care Med 23(2):S140–S146. https://doi.org/10.5005/jp-journals-10071-23192
Rymer MM (2011) Hemorrhagic stroke: intracerebral hemorrhage. Mo Med 108(1):50–54
Boehme AK, Esenwa C, Elkind MS (2017) Stroke risk factors, genetics, and prevention. Circ Res 120(3):472–495. https://doi.org/10.1161/CIRCRESAHA.116.308398
Khan H, Kashyap A, Kaur A et al (2020) Pharmacological postconditioning: a molecular aspect in ischemic injury. J Pharm Pharmacol 72(11):1513–1527. https://doi.org/10.1111/jphp.13336
Grewal AK, Singh N, Singh TG (2019) Neuroprotective effect of pharmacological postconditioning on cerebral ischaemia-reperfusion-induced injury in mice. J Pharm Pharmacol 71(6):956–970. https://doi.org/10.1111/jphp.13073
Donkor ES (2018) Stroke in the 21st century: a snapshot of the burden, epidemiology, and quality of life. Stroke Res Treat. https://doi.org/10.1155/2018/3238165
Tyagi S, Gupta P, Saini AS et al (2011) The peroxisome proliferator-activated receptor: a family of nuclear receptors role in various diseases. J Adv Pharm Technol Res 2(4):236–240. https://doi.org/10.4103/2231-4040.90879
Houseknecht KL, Cole BM, Steele PJ (2002) Peroxisome proliferator-activated receptor gamma (PPARgamma) and its ligands: a review. Domest Anim Endocrinol 22(1):1–23. https://doi.org/10.1016/s0739-7240(01)00117-5
Kroker AJ, Bruning JB (2015) Review of the structural and dynamic mechanisms of PPARγ partial agonism. PPAR Res. https://doi.org/10.1155/2015/816856
Thapa K, Khan H, Sharma U et al (2021) Poly (ADP-ribose) polymerase-1 as a promising drug target for neurodegenerative diseases. Life Science 267:118975. https://doi.org/10.1016/j.lfs.2020.118975
Weikum ER, Liu X, Ortlund EA (2018) The nuclear receptor superfamily: a structural perspective. Protein Sci 27(11):1876–1892. https://doi.org/10.1002/pro.3496
Brunmeir R, Xu F (2018) Functional regulation of PPARs through post-translational modifications. Int J Mol Sci 19(6):1738. https://doi.org/10.3390/ijms19061738
Kim CS, Park WH, Park JY et al (2004) Capsaicin, a spicy component of hot pepper, induces apoptosis by activation of the peroxisome proliferator-activated receptor gamma in HT-29 human colon cancer cells. J Med Food 7(3):267–273. https://doi.org/10.1089/jmf.2004.7.267
Burns KA, Vanden Heuvel JP (2007) Modulation of PPAR activity via phosphorylation. Biochem Biophys Acta 1771(8):952–960. https://doi.org/10.1016/j.bbalip.2007.04.018
Choi JH, Banks AS, Kamenecka TM et al (2011) Antidiabetic actions of a non-agonist PPARγ ligand blocking Cdk5-mediated phosphorylation. Nature 477(7365):477–481. https://doi.org/10.1038/nature10383
Choi SS, Kim ES, Koh M et al (2014) A novel non-agonist peroxisome proliferator-activated receptor γ (PPARγ) ligand UHC1 blocks PPARγ phosphorylation by cyclin-dependent kinase 5 (CDK5) and improves insulin sensitivity. J Biol Chem 289(38):26618–26629. https://doi.org/10.1074/jbc.M114.566794
Rai A, Tripathi S, Kushwaha R et al (2014) CDK5-induced p-PPARγ(Ser 112) downregulates GFAP via PPREs in developing rat brain: effect of metal mixture and troglitazone in astrocytes. Cell Death Dis 5(1):e1033. https://doi.org/10.1038/cddis.2013.514
Ohshima T, Koga H, Shimotohno K (2004) Transcriptional activity of peroxisome proliferator-activated receptor gamma is modulated by SUMO-1 modification. J Biol Chem 279(28):29551–29557. https://doi.org/10.1074/jbc.M403866200
Jennewein C, Kuhn AM, Schmidt MV et al (2008) Sumoylation of peroxisome proliferator-activated receptor gamma by apoptotic cells prevents lipopolysaccharide-induced NCoR removal from kappaB binding sites mediating transrepression of proinflammatory cytokines. J Immunol 181(8):5646–5652. https://doi.org/10.4049/jimmunol.181.8.5646
Waite KJ, Floyd ZE, Arbour-Reily P et al (2001) Interferon-gamma-induced regulation of peroxisome proliferator-activated receptor gamma and STATs in adipocytes. J Biol Chem 276(10):7062–7068. https://doi.org/10.1074/jbc.M007894200
He F, Doucet JA, Stephens JM (2008) Caspase-mediated degradation of PPARgamma proteins in adipocytes. Obesity 16(8):1735–1741. https://doi.org/10.1038/oby.2008.269
Cai W, Yang T, Liu H et al (2018) Peroxisome proliferator-activated receptor γ (PPARγ): a master gatekeeper in CNS injury and repair. Prog Neurobiol 163–164:27–58. https://doi.org/10.1016/j.pneurobio.2017.10.002
Ahmadian M, Suh JM, Hah N et al (2013) PPARγ signaling and metabolism: the good, the bad and the future. Nat Med 19(5):557–566. https://doi.org/10.1038/nm.3159
Song EK, Lee YR, Kim YR et al (2012) NAADP mediates insulin-stimulated glucose uptake and insulin sensitization by PPARγ in adipocytes. Cell Rep 2(6):1607–1619. https://doi.org/10.1016/j.celrep.2012.10.018
Singh S, Singh TG, Rehni AK et al (2021) Reviving mitochondrial bioenergetics: a relevant approach in epilepsy. Mitochondrion 58:213–226. https://doi.org/10.1016/j.mito.2021.03.009
Shimazu T, Inoue I, Araki N et al (2005) A peroxisome proliferator-activated receptor-gamma agonist reduces infarct size in transient but not in permanent ischemia. Stroke 36(2):353–359. https://doi.org/10.1161/01.STR.0000152271.21943.a2
Villapol S (2018) Roles of peroxisome proliferator-activated receptor gamma on brain and peripheral inflammation. Cell Mol Neurobiol 38(1):121–132. https://doi.org/10.1007/s10571-017-0554-5
Mandrekar-Colucci S, Sauerbeck A, Popovich PG et al (2013) PPAR agonists as therapeutics for CNS trauma and neurological diseases. ASN Neuro 5(5):e00129. https://doi.org/10.1042/AN20130030
Moreno S, Farioli-Vecchioli S, Cerù MP (2004) Immunolocalization of peroxisome proliferator-activated receptors and retinoid X receptors in the adult rat CNS. Neuroscience 123(1):131–145. https://doi.org/10.1016/j.neuroscience.2003.08.064
Warden A, Truitt J, Merriman M et al (2016) Localization of PPAR isotypes in the adult mouse and human brain. Sci Rep 6:27618. https://doi.org/10.1038/srep27618b
D’Angelo M, Castelli V, Catanesi M et al (2019) PPARγ and cognitive performance. Int J Mol Sci 20(20):5068. https://doi.org/10.3390/ijms20205068
Ferguson LB, Most D, Blednov YA et al (2014) PPAR agonists regulate brain gene expression: relationship to their effects on ethanol consumption. Neuropharmacology 86:397–407. https://doi.org/10.1016/j.neuropharm.2014.06.024
Bernardo A, Minghetti L (2006) PPAR-gamma agonists as regulators of microglial activation and brain inflammation. Curr Pharm Des 12(1):93–109. https://doi.org/10.2174/138161206780574579
Yu Y, Han Q, Ding X et al (2016) Defining core and penumbra in ischemic stroke: a voxel- and volume-based analysis of whole brain CT perfusion. Sci Rep 6:20932. https://doi.org/10.1038/srep20932
Hillis AE, Baron JC (2015) Editorial: the ischemic penumbra: still the target for stroke therapies? Front Neurol 6:85. https://doi.org/10.3389/fneur.2015.00085
Kapadia R, Yi JH, Vemuganti R (2008) Mechanisms of anti-inflammatory and neuroprotective actions of PPAR-gamma agonists. Front Biosci 13:1813–1826. https://doi.org/10.2741/2802
Prentice H, Modi JP, Wu JY (2015) Mechanisms of neuronal protection against excitotoxicity, endoplasmic reticulum stress, and mitochondrial dysfunction in stroke and neurodegenerative diseases. Oxid Med Cell Longev. https://doi.org/10.1155/2015/964518
Rehni AK, Singh TG, Singh N et al (2010) Tramadol-induced seizurogenic effect: a possible role of opioid-dependent histamine H1 receptor activation-linked mechanism. Naunyn Schmiedebergs Arch Pharmacol 381(1):11–19. https://doi.org/10.1007/s00210-009-0476-y
Liu F, Lu J, Manaenko A et al (2018) Mitochondria in ischemic stroke: new insight and implications. Aging Dis 9(5):924–937. https://doi.org/10.14336/AD.2017.1126
Emerich DF, Dean RL, Bartus RT (2002) The role of leukocytes following cerebral ischemia: pathogenic variable or bystander reaction to emerging infarct? Exp Neurol 173(1):168–181. https://doi.org/10.1006/exnr.2001.7835
Zhang YY, Wang K, Liu YE et al (2019) Identification of key transcription factors associated with cerebral ischemia-reperfusion injury based on gene-set enrichment analysis. Int J Mol Med 43(6):2429–2439. https://doi.org/10.3892/ijmm.2019.4159
Shi H (2009) Hypoxia inducible factor 1 as a therapeutic target in ischemic stroke. Curr Med Chem 16(34):4593–4600. https://doi.org/10.2174/092986709789760779
Liang Z, Wu G, Fan C et al (2016) The emerging role of signal transducer and activator of transcription 3 in cerebral ischemic and hemorrhagic stroke. Prog Neurobiol 137:1–16. https://doi.org/10.1016/j.pneurobio.2015.11.001
Tureyen K, Brooks N, Bowen K et al (2008) Transcription factor early growth response-1 induction mediates inflammatory gene expression and brain damage following transient focal ischemia. J Neurochem 105(4):1313–1324. https://doi.org/10.1111/j.1471-4159.2008.05233.x
Alexander M, Forster C, Sugimoto K et al (2003) Interferon regulatory factor-1 immunoreactivity in neurons and inflammatory cells following ischemic stroke in rodents and humans. Acta Neuropathol 105(5):420–424. https://doi.org/10.1007/s00401-002-0658-x
Lin H, Cheng CF (2018) Activating transcription factor 3, an early cellular adaptive responder in ischemia/reperfusion-induced injury. Tzu-chi Med J 30(2):61–65. https://doi.org/10.4103/tcmj.tcmj_37_18
Sharma VK, Singh TG (2020) CREB: a multifaceted target for Alzheimer’s disease. Curr Alzheimer Res 17(14):1280–1293. https://doi.org/10.2174/1567205018666210218152253
Singh S, Singh TG (2020) Role of nuclear factor kappa B (NF-κB) signalling in neurodegenerative diseases: an mechanistic approach. Curr Neuropharmacol 18(10):918–935. https://doi.org/10.2174/1570159X18666200207120949
Vemuganti R (2008) Therapeutic potential of PPARγ activation in stroke. PPAR Res. https://doi.org/10.1155/2008/461981
Rehni AK, Singh TG (2012) Involvement of CCR-2 chemokine receptor activation in ischemic preconditioning and postconditioning of brain in mice. Cytokine 60(1):83–89. https://doi.org/10.1016/j.cyto.2012.05.009
Wei J, Zhang Y, Jia Q et al (2016) Systematic investigation of transcription factors critical in the protection against cerebral ischemia by Danhong injection. Sci Rep 6:29823. https://doi.org/10.1038/srep29823
Culman J, Zhao Y, Gohlke P et al (2007) PPAR-gamma: therapeutic target for ischemic stroke. Trends Pharmacol Sci 28(5):244–249. https://doi.org/10.1016/j.tips.2007.03.004
Li W, Yang S (2016) Targeting oxidative stress for the treatment of ischemic stroke: Upstream and downstream therapeutic strategies. Brain Circ 2(4):153–163. https://doi.org/10.4103/2394-8108.195279
Khan H, Gupta A, Singh TG et al (2021) Mechanistic insight on the role of leukotriene receptors in ischemic-reperfusion injury. Pharmacol Rep. https://doi.org/10.1007/s43440-021-00258-8
Bordet R, Ouk T, Petrault O et al (2006) PPAR: a new pharmacological target for neuroprotection in stroke and neurodegenerative diseases. Biochem Soc Trans 34(6):1341–1346. https://doi.org/10.1042/BST0341341
Victor NA, Wanderi EW, Gamboa J et al (2006) Altered PPARgamma expression and activation after transient focal ischemia in rats. Eur J Neurosci 24(6):1653–1663. https://doi.org/10.1111/j.1460-9568.2006.05037.x
Stark DT, Bazan NG (2011) Synaptic and extrasynaptic NMDA receptors differentially modulate neuronal cyclooxygenase-2 function, lipid peroxidation, and neuroprotection. J Neurosci 31(39):13710–13721. https://doi.org/10.1523/JNEUROSCI.3544-11.2011
Wang L, Zhang MJ, Li WJ et al (2019) Rosiglitazone protect PC12 cells against oxygen-glucose deprivation/reoxygenation through HMGB1 reduction and DUSP8 upregulation. J Apoplexy Nerv Dis 36:541–545
Yang H, Chen C (2008) Cyclooxygenase-2 in synaptic signaling. Curr Pharm Des 14(14):1443–1451. https://doi.org/10.2174/138161208784480144
Font-Nieves M, Sans-Fons MG, Gorina R et al (2012) Induction of COX-2 enzyme and down-regulation of COX-1 expression by lipopolysaccharide (LPS) control prostaglandin E2 production in astrocytes. J Biol Chem 287(9):6454–6468. https://doi.org/10.1074/jbc.M111.327874
Zhao X, Strong R, Zhang J et al (2009) Neuronal PPARgamma deficiency increases susceptibility to brain damage after cerebral ischemia. J Neurosci 29(19):6186–6195. https://doi.org/10.1523/JNEUROSCI.5857-08.2009
Liu ZJ, Liu W, Liu L et al (2013) Curcumin protects neuron against cerebral ischemia-induced inflammation through improving PPAR-gamma function. Evid Complement Altern Med. https://doi.org/10.1155/2013/470975
Polvani S, Tarocchi M, Galli A (2012) PPARγ and oxidative stress: Con(β) catenating NRF2 and FOXO. PPAR Res. https://doi.org/10.1155/2012/641087
Corona JC, Duchen MR (2016) PPARγ as a therapeutic target to rescue mitochondrial function in neurological disease. Free Radical Biol Med 100:153–163. https://doi.org/10.1016/j.freeradbiomed.2016.06.023
Yu X, Shao XG, Sun H et al (2008) Activation of cerebral peroxisome proliferator-activated receptors gamma exerts neuroprotection by inhibiting oxidative stress following pilocarpine-induced status epilepticus. Brain Res 1200:146–158. https://doi.org/10.1016/j.brainres.2008.01.047
Reddy AT, Lakshmi SP, Banno A et al (2018) Role of GPx3 in PPARγ-induced protection against COPD-associated oxidative stress. Free Radical Biol Med 126:350–357. https://doi.org/10.1016/j.freeradbiomed.2018.08.014
Vanella L, Sanford C, Kim DH et al (2012) Oxidative stress and heme oxygenase-1 regulated human mesenchymal stem cells differentiation. Int J Hypertens. https://doi.org/10.1155/2012/890671
Sharma V, Kaur A, Singh TG (2020) Counteracting role of nuclear factor erythroid 2-related factor 2 pathway in Alzheimer’s disease. Biomed Pharmacother 129:110373. https://doi.org/10.1016/j.biopha.2020.110373
Huang J, Tabbi-Anneni I, Gunda V et al (2010) Transcription factor Nrf2 regulates SHP and lipogenic gene expression in hepatic lipid metabolism. Am J Physiol Gastrointest Liver Physiol 299(6):G1211–G1221. https://doi.org/10.1152/ajpgi.00322.2010
Tabei Y, Murotomi K, Umeno A et al (2017) Antioxidant properties of 5-hydroxy-4-phenyl-butenolide via activation of Nrf2/ARE signaling pathway. Food Chem Toxicol 107(Pt A):129–137. https://doi.org/10.1016/j.fct.2017.06.039
Mahmoud-Awny M, Attia AS, Abd-Ellah MF et al (2015) Mangiferin mitigates gastric ulcer in ischemia/ reperfused rats: involvement of PPAR-γ, NF-κB and Nrf2/HO-1 signaling pathways. PLoS ONE 10(7):e0132497. https://doi.org/10.1371/journal.pone.0132497
Chung SS, Kim M, Youn BS et al (2009) Glutathione peroxidase 3 mediates the antioxidant effect of peroxisome proliferator-activated receptor gamma in human skeletal muscle cells. Mol Cell Biol 29(1):20–30. https://doi.org/10.1128/MCB.00544-08
Alcaraz MJ, Fernández P, Guillén MI (2003) Anti-inflammatory actions of the heme oxygenase-1 pathway. Curr Pharm Des 9(30):2541–2551. https://doi.org/10.2174/1381612033453749
Gong P, Stewart D, Hu B et al (2002) Activation of the mouse heme oxygenase-1 gene by 15-deoxy-Delta(12,14)-prostaglandin J(2) is mediated by the stress response elements and transcription factor Nrf2. Antioxid Redox Signal 4(2):249–257. https://doi.org/10.1089/152308602753666307
Kleinhenz JM, Kleinhenz DJ, You S et al (2009) Disruption of endothelial peroxisome proliferator-activated receptor-gamma reduces vascular nitric oxide production. Am J Physiol 297(5):H1647–H1654. https://doi.org/10.1152/ajpheart.00148.2009
Rehni AK, Singh TG, Kalra R et al (2009) Pharmacological inhibition of inducible nitric oxide synthase attenuates the development of seizures in mice. Nitric Oxide 21(2):120–125. https://doi.org/10.1016/j.niox.2009.06.001
Polikandriotis JA, Mazzella LJ, Rupnow HL et al (2005) Peroxisome proliferator-activated receptor gamma ligands stimulate endothelial nitric oxide production through distinct peroxisome proliferator-activated receptor gamma-dependent mechanisms. Arterioscler Thromb Vasc Biol 25(9):1810–1816. https://doi.org/10.1161/01.ATV.0000177805.65864.d4
Yuen CY, Wong WT, Tian XY et al (2011) Telmisartan inhibits vasoconstriction via PPARγ-dependent expression and activation of endothelial nitric oxide synthase. Cardiovasc Res 90(1):122–129. https://doi.org/10.1093/cvr/cvq392
Febbraio M, Hajjar DP, Silverstein RL (2001) CD36: a class B scavenger receptor involved in angiogenesis, atherosclerosis, inflammation, and lipid metabolism. J Clin Investig 108(6):785–791
Ishii T, Itoh K, Ruiz E et al (2004) Role of Nrf2 in the regulation of CD36 and stress protein expression in murine macrophages: activation by oxidatively modified LDL and 4-hydroxynonenal. Circ Res 94(5):609–616. https://doi.org/10.1161/01.RES.0000119171.44657.45
Pierelli G, Stanzione R, Forte M et al (2017) Uncoupling protein 2: a key player and a potential therapeutic target in vascular diseases. Oxid Med Cell Longev. https://doi.org/10.1155/2017/7348372
Chen YJ, Sheu ML, Tsai KS et al (2013) Advanced glycation end products induce peroxisome proliferator-activated receptor γ down-regulation-related inflammatory signals in human chondrocytes via Toll-like receptor-4 and receptor for advanced glycation end products. PLoS ONE. https://doi.org/10.1371/journal.pone.0066611.e66611
Jiang C, Ting AT, Seed B (1998) PPAR-γ agonists inhibit production of monocyte inflammatory cytokines. Nature 391(6662):82–86. https://doi.org/10.1038/34184
Reddy RC (2008) Immunomodulatory role of PPAR-gamma in alveolar macrophages. J Investig Med 56(2):522–527. https://doi.org/10.2310/JIM.0b013e3181659972
Luo Y, Yin W, Signore AP et al (2006) Neuroprotection against focal ischemic brain injury by the peroxisome proliferator-activated receptor-gamma agonist rosiglitazone. J Neurochem 97(2):435–448. https://doi.org/10.1111/j.1471-4159.2006.03758.x
Glatz T, Stöck I, Nguyen-Ngoc M et al (2010) Peroxisome-proliferator-activated receptors gamma and peroxisome-proliferator-activated receptors beta/delta and the regulation of interleukin 1 receptor antagonist expression by pioglitazone in ischaemic brain. J Hypertens 28(7):1488–1497. https://doi.org/10.1097/HJH.0b013e3283396e4e
Gliem M, Klotz L, van Rooijen N et al (2015) Hyperglycemia and PPARγ antagonistically influence macrophage polarization and infarct healing after ischemic stroke. Stroke 46(10):2935–2942. https://doi.org/10.1161/STROKEAHA.115.010557
Zhang Q, Hu W, Meng B et al (2010) PPARγ agonist rosiglitazone is neuroprotective after traumatic spinal cord injury via anti-inflammatory in adult rats. Neurol Res 32(8):852–859. https://doi.org/10.1179/016164110X12556180206112
Iwanami J, Mogi M, Tsukuda K et al (2010) Low dose of telmisartan prevents ischemic brain damage with peroxisome proliferator-activated receptor-gamma activation in diabetic mice. J Hypertens 28(8):1730–1737. https://doi.org/10.1097/HJH.0b013e32833a551a
Washida K, Ihara M, Nishio K et al (2010) Nonhypotensive dose of telmisartan attenuates cognitive impairment partially due to peroxisome proliferator-activated receptor-gamma activation in mice with chronic cerebral hypoperfusion. Stroke 41(8):1798–1806. https://doi.org/10.1161/STROKEAHA.110.583948
Kumari R, Willing LB, Patel SD et al (2010) The PPAR-gamma agonist, darglitazone, restores acute inflammatory responses to cerebral hypoxia-ischemia in the diabetic ob/ob mouse. J Cereb Blood Flow Metab 30(2):352–360. https://doi.org/10.1038/jcbfm.2009.221
Huang L, Li G, Feng X et al (2015) 15d-PGJ2 reduced microglia activation and alleviated neurological deficit of ischemic reperfusion in diabetic rat model. Biomed Res Int. https://doi.org/10.1155/2015/864509
Pereira MP, Hurtado O, Cárdenas A et al (2005) The nonthiazolidinedione PPARgamma agonist L-796,449 is neuroprotective in experimental stroke. J Neuropathol Exp Neurol 64(9):797–805. https://doi.org/10.1097/01.jnen.0000178852.83680.3c
Han J, Sun L, Xu Y et al (2015) Activation of PPARγ by 12/15-lipoxygenase during cerebral ischemia-reperfusion injury. Int J Mol Med 35(1):195–201. https://doi.org/10.3892/ijmm.2014.1998
Choo J, Lee Y, Yan XJ et al (2015) A novel peroxisome proliferator-activated receptor (PPAR)γ agonist 2-hydroxyethyl 5-chloro-4,5-didehydrojasmonate exerts anti-inflammatory effects in colitis. J Biol Chem 290(42):25609–25619. https://doi.org/10.1074/jbc.M115.673046
Zhuo Y, Zhuo J (2019) Tranilast treatment attenuates cerebral ischemia-reperfusion injury in rats through the inhibition of inflammatory responses mediated by NF-κB and PPARs. Clin Transl Sci 12(2):196–202. https://doi.org/10.1111/cts.12606
Zarubin T, Han J (2005) Activation and signaling of the p38 MAP kinase pathway. Cell Res 15(1):11–18. https://doi.org/10.1038/sj.cr.7290257
Xing B, Xin T, Hunter RL et al (2008) Pioglitazone inhibition of lipopolysaccharide-induced nitric oxide synthase is associated with altered activity of p38 MAP kinase and PI3K/Akt. J Neuroinflamm 5:4. https://doi.org/10.1186/1742-2094-5-4
Ji H, Wang H, Zhang F (2010) PPARγ agonist pioglitazone inhibits microglia inflammation by blocking p38 mitogen-activated protein kinase signaling pathways. Inflamm Res 59(11):921–929. https://doi.org/10.1007/s00011-010-0203-7
Nuwormegbe SA, Sohn JH, Kim SW (2017) A PPAR-gamma agonist rosiglitazone suppresses fibrotic response in human pterygium fibroblasts by modulating the p38 MAPK pathway. Invest Ophthalmol Vis Sci 58(12):5217–5226. https://doi.org/10.1167/iovs.17-22203
Hernandez R, Teruel T, de Alvaro C et al (2004) Rosiglitazone ameliorates insulin resistance in brown adipocytes of Wistar rats by impairing TNF-alpha induction of p38 and p42/p44 mitogen-activated protein kinases. Diabetologia 47(9):1615–1624. https://doi.org/10.1007/s00125-004-1503-7
Liu Y, Chen S, Liu J et al (2020) Telmisartan inhibits oxalate and calcium oxalate crystal-induced epithelial-mesenchymal transformation via PPAR-γ-AKT/STAT3/p38 MAPK-Snail pathway. Life Sci 241:117108. https://doi.org/10.1016/j.lfs.2019.117108
Min KJ, Um HJ, Cho KH et al (2013) Curcumin inhibits oxLDL-induced CD36 expression and foam cell formation through the inhibition of p38 MAPK phosphorylation. Food Chem Toxicol 58:77–85. https://doi.org/10.1016/j.fct.2013.04.008
Liu Q, Wang CY, Liu Z et al (2014) Hydroxysafflor yellow A suppresses liver fibrosis induced by carbon tetrachloride with high-fat diet by regulating PPAR-γ/p38 MAPK signaling. Pharm Biol 52(9):1085–1093. https://doi.org/10.3109/13880209.2013.877491
Ren G, Roberts AI, Shi Y (2011) Adhesion molecules: key players in Mesenchymal stem cell-mediated immunosuppression. Cell Adh Migr 5(1):20–22. https://doi.org/10.4161/cam.5.1.13491
Golias C, Batistatou A, Bablekos G et al (2011) Physiology and pathophysiology of selectins, integrins, and IgSF cell adhesion molecules focusing on inflammation. A paradigm model on infectious endocarditis. Cell Commun Adhes 18(3):19–32. https://doi.org/10.3109/15419061.2011.606381
Wang N, Verna L, Chen NG et al (2002) Constitutive activation of peroxisome proliferator-activated receptor-gamma suppresses pro-inflammatory adhesion molecules in human vascular endothelial cells. J Biol Chem 277(37):34176–34181. https://doi.org/10.1074/jbc.M203436200
Sasaki M, Jordan P, Welbourne T et al (2005) Troglitazone, a PPAR-gamma activator prevents endothelial cell adhesion molecule expression and lymphocyte adhesion mediated by TNF-alpha. BMC Physiol 5(1):3. https://doi.org/10.1186/1472-6793-5-3
Pasceri V, Wu HD, Willerson JT et al (2000) Modulation of vascular inflammation in vitro and in vivo by peroxisome proliferator-activated receptor-gamma activators. Circulation 101(3):235–238. https://doi.org/10.1161/01.cir.101.3.235
Ayumi UO, Yasuo O, Nobuyuki E (2017) The peroxisome proliferator-activated receptor pan-agonist bezafibrate suppresses microvascular inflammatory responses of retinal endothelial cells and vascular endothelial growth factor production in retinal pigmented epithelial cells. Int Immunopharmacol 52:70–76. https://doi.org/10.1016/j.intimp.2017.08.027
Liu T, Zhang L, Joo D et al (2017) NF-κB signaling in inflammation. Signal Transduct Target Ther 2:17023. https://doi.org/10.1038/sigtrans.2017.23
Giridharan S, Srinivasan M (2018) Mechanisms of NF-κB p65 and strategies for therapeutic manipulation. J Inflamm Res 11:407–419. https://doi.org/10.2147/JIR.S140188
Scirpo R, Fiorotto R, Villani A et al (2015) Stimulation of nuclear receptor peroxisome proliferator-activated receptor-γ limits NF-κB-dependent inflammation in mouse cystic fibrosis biliary epithelium. Hepatology 62(5):1551–1562. https://doi.org/10.1002/hep.28000
Kunicka Z, Kurzynska A, Szydlowska A et al (2019) Peroxisome proliferator-activated receptor gamma ligands affect NF-κB and cytokine synthesis in the porcine endometrium-An in vitro study. Am J Reprod Immunol 81(1):e13053. https://doi.org/10.1111/aji.13053
Li Q, Tian Z, Wang M et al (2019) Luteoloside attenuates neuroinflammation in focal cerebral ischemia in rats via regulation of the PPARγ/Nrf2/NF-κB signaling pathway. Int Immunopharmacol 66:309–316. https://doi.org/10.1016/j.intimp.2018.11.044
Rani N, Arya DS (2020) Chrysin rescues rat myocardium from ischemia-reperfusion injury via PPAR-γ/Nrf2 activation. Eur J Pharmacol 883:173389. https://doi.org/10.1016/j.ejphar.2020.173389
Hou Y, Moreau F, Chadee K (2012) PPARγ is an E3 ligase that induces the degradation of NFκB/p65. Nat Commun 3:1300. https://doi.org/10.1038/ncomms2270
Kelley N, Jeltema D, Duan Y et al (2019) The NLRP3 inflammasome: an overview of mechanisms of activation and regulation. Int J Mol Sci 20(13):3328. https://doi.org/10.3390/ijms20133328
Swanson KV, Deng M, Ting JP (2019) The NLRP3 inflammasome: molecular activation and regulation to therapeutics. Nat Rev Immunol 19(8):477–489. https://doi.org/10.1038/s41577-019-0165-0
Song N, Li T (2018) Regulation of NLRP3 inflammasome by phosphorylation. Front Immunol 9:2305. https://doi.org/10.3389/fimmu.2018.02305
Abais JM, XiaM ZY et al (2015) Redox regulation of NLRP3 inflammasomes: ROS as trigger or effector? Antioxid Redox Signal 22(13):1111–1129. https://doi.org/10.1089/ars.2014.5994
Fann DY, Lim YA, Cheng YL et al (2018) Evidence that NF-κB and MAPK signaling promotes NLRP inflammasome activation in neurons following ischemic stroke. Mol Neurobiol 55(2):1082–1096. https://doi.org/10.1007/s12035-017-0394-9
Wang X, Li R, Wang X et al (2015) Umbelliferone ameliorates cerebral ischemia-reperfusion injury via upregulating the PPAR gamma expression and suppressing TXNIP/NLRP3 inflammasome. Neurosci Lett 600:182–187. https://doi.org/10.1016/j.neulet.2015.06.016
Zhang YL, Wang RB, Li WY et al (2017) Pioglitazone ameliorates retinal ischemia/reperfusion injury via suppressing NLRP3 inflammasome activities. Int J Ophthalmol 10(12):1812–1818. https://doi.org/10.18240/ijo.2017.12.04
Mahmoud AM, Hussein OE, Abd El-Twab SM et al (2019) Ferulic acid protects against methotrexate nephrotoxicity via activation of Nrf2/ARE/HO-1 signaling and PPARγ, and suppression of NF-κB/NLRP3 inflammasome axis. Food Funct 10(8):4593–4607. https://doi.org/10.1039/c9fo00114j
Yang CC, Wu CH, Lin TC et al (2021) Inhibitory effect of PPARγ on NLRP3 inflammasome activation. Theranostics 11(5):2424–2441. https://doi.org/10.7150/thno.46873
Pan MG, Xiong Y, Chen F (2013) NFAT gene family in inflammation and cancer. Curr Mol Med 13(4):543–554. https://doi.org/10.2174/1566524011313040007
Liu JO (2009) Calmodulin-dependent phosphatase, kinases, and transcriptional corepressors involved in T-cell activation. Immunol Rev 228(1):184–198. https://doi.org/10.1111/j.1600-065X.2008.00756.x
Kim KD, Srikanth S, Tan YV et al (2014) Calcium signaling via Orai1 is essential for induction of the nuclear orphan receptor pathway to drive Th17 differentiation. J Immunol 192(1):110–122. https://doi.org/10.4049/jimmunol.1302586
Yang XY, Wang LH, Chen T et al (2000) Activation of human T lymphocytes is inhibited by peroxisome proliferator-activated receptor gamma (PPARgamma) agonists PPARgamma co-association with transcription factor NFAT. J Biol Chem 275(7):4541–4544. https://doi.org/10.1074/jbc.275.7.4541
Yao J, Lu Y, Zhi M et al (2017) Dietary n-3 polyunsaturated fatty acids ameliorate Crohn’s disease in rats by modulating the expression of PPAR-γ/NFAT. Mol Med Rep 16(6):8315–8322. https://doi.org/10.3892/mmr.2017.7673
Paintlia AS, Paintlia MK, Singh I et al (2006) IL-4-induced peroxisome proliferator-activated receptor gamma activation inhibits NF-kappaB trans activation in central nervous system (CNS) glial cells and protects oligodendrocyte progenitors under neuroinflammatory disease conditions: implication for CNS-demyelinating diseases. J Immunol 176(7):4385–4398. https://doi.org/10.4049/jimmunol.176.7.4385
Wang X, Yu YY, Lieu S et al (2013) MMP9 regulates the cellular response to inflammation after skeletal injury. Bone 52(1):111–119. https://doi.org/10.1016/j.bone.2012.09.018
Manicone AM, McGuire JK (2008) Matrix metalloproteinases as modulators of inflammation. Semin Cell Dev Biol 19(1):34–41. https://doi.org/10.1016/j.semcdb.2007.07.003
Hetzel M, Walcher D, Grüb M et al (2003) Inhibition of MMP-9 expression by PPARgamma activators in human bronchial epithelial cells. Thorax 58(9):778–783. https://doi.org/10.1136/thorax.58.9.778
Singh HP, Singh TG, Singh R (2020) Attenuation of cisplatin-induced nephrotoxicity by p-coumaric acid through peroxisome proliferator-activated receptor-gamma (PPAR-γ) agonism in male rats. Res J Pharm Technol 13(11):5270–5276. https://doi.org/10.5958/0974-360X.2020.00922.1
Xu L, Liu JT, Li K et al (2019) Genistein inhibits Ang II-induced CRP and MMP-9 generations via the ER-p38/ERK1/2-PPARγ-NF-κB signaling pathway in rat vascular smooth muscle cells. Life Sci 216:140–146. https://doi.org/10.1016/j.lfs.2018.11.036
Xue Q, Yan Y, Zhang R et al (2018) Regulation of iNOS on immune cells and its role in diseases. Int J Mol Sci 19(12):3805. https://doi.org/10.3390/ijms19123805
Rehni AK, Singh TG, Bhateja P et al (2010) Involvement of cyclic adenosine diphosphoribose receptor activation in ischemic preconditioning induced protection in mouse brain. Brain Res 1309:75–82. https://doi.org/10.1016/j.brainres.2009.10.071
Refaie M, El-Hussieny M (2018) Protective effect of pioglitazone on ovarian ischemia reperfusion injury of female rats via modulation of peroxisome proliferator activated receptor gamma and heme-oxygenase 1. Int Immunopharmacol 62:7–14. https://doi.org/10.1016/j.intimp.2018.06.037
Thapa K, Khan H, Singh TG et al (2021) Traumatic brain injury: mechanistic insight on pathophysiology and potential therapeutic targets. J Mol Neurosci. https://doi.org/10.1007/s12031-021-01841-7
Xia P, Pan Y, Zhang F et al (2018) Pioglitazone confers neuroprotection against ischemia-induced pyroptosis due to its inhibitory effects on HMGB-1/RAGE and Rac1/ROS pathway by activating PPAR-ɤ. Cell Physiol Biochem 45(6):2351–2368. https://doi.org/10.1159/000488183
Man SM, Karki R, Kanneganti TD (2017) Molecular mechanisms and functions of pyroptosis, inflammatory caspases and inflammasomes in infectious diseases. Immunol Rev 277(1):61–75. https://doi.org/10.1111/imr.12534
Yang H, Wang H, Andersson U (2020) Targeting inflammation driven by HMGB1. Front Immunol 11:484. https://doi.org/10.3389/fimmu.2020.00484
Kalyan S, Chow AW (2009) Linking innate and adaptive immunity: human Vgamma9Vdelta2 T cells enhance CD40 expression and HMGB-1 secretion. Mediators Inflamm. https://doi.org/10.1155/2009/819408
Sumiyoshi M, Satomi J, Kitazato KT et al (2015) PPARγ-dependent and -independent inhibition of the HMGB1/TLR9 pathway by eicosapentaenoic acid attenuates ischemic brain damage in ovariectomized rats. J Stroke Cerebrovasc Dis 24(6):1187–1195. https://doi.org/10.1016/j.jstrokecerebrovasdis.2015.01.009
Haraguchi T, Takasaki K, Naito T et al (2009) Cerebroprotective action of telmisartan by inhibition of macrophages/microglia expressing HMGB1 via a peroxisome proliferator-activated receptor γ-dependent mechanism. Neurosci Lett 464(3):151–155. https://doi.org/10.1016/j.neulet.2009.08.043
Gao M, Hu Z, Zheng Y et al (2011) Peroxisome proliferator-activated receptor γ agonist troglitazone inhibits high mobility group box 1 expression in endothelial cells via suppressing transcriptional activity of nuclear factor κB and activator protein 1. Shock 36(3):228–234. https://doi.org/10.1097/SHK.0b013e318225b29a
Hwang JS, Kang ES, Ham SA et al (2012) Activation of peroxisome proliferator-activated receptor γ by rosiglitazone inhibits lipopolysaccharide-induced release of high mobility group box 1. Mediators Inflamm. https://doi.org/10.1155/2012/352807
de Los G, Fayos Alonso I, Liang HC, Turner SD et al (2018) The role of activator protein-1 (AP-1) family members in CD30-positive lymphomas. Cancers 10(4):93. https://doi.org/10.3390/cancers10040093
Eckert RL, Adhikary G, Young CA et al (2013) AP1 transcription factors in epidermal differentiation and skin cancer. J Skin Cancer. https://doi.org/10.1155/2013/537028
Xiao P, Liu XW, Zhao NN et al (2018) Correlations of neuronal apoptosis with expressions of c-Fos and c-Jun in rats with post-ischemic reconditioning damage. Eur Rev Med Pharmacol Sci 22(9):2832–2838. https://doi.org/10.26355/eurrev_201805_14984
Ameyar M, Wisniewska M, Weitzman JB (2003) A role for AP-1 in apoptosis: the case for and against. Biochimie 85(8):747–752. https://doi.org/10.1016/j.biochi.2003.09.006
Konstantinopoulos PA, Vandoros GP, Sotiropoulou-Bonikou G et al (2007) NF-kappaB/PPAR gamma and/or AP-1/PPAR gamma “on/off” switches and induction of CBP in colon adenocarcinomas: correlation with COX-2 expression. Int J Colorectal Dis 22(1):57–68. https://doi.org/10.1007/s00384-006-0112-y
Zhang Y, Wang C, Jia ZL et al (2020) Isoniazid promotes the anti-inflammatory response in zebrafish associated with regulation of the PPARγ/NF-κB/AP-1 pathway. Chem Biol Interact 316:108928. https://doi.org/10.1016/j.cbi.2019.108928
Mittal M, Siddiqui MR, Tran K et al (2014) Reactive oxygen species in inflammation and tissue injury. Antioxid Redox Signal 20(7):1126–1167. https://doi.org/10.1089/ars.2012.5149
Zhang Y, Hu L, Cui Y et al (2014) Roles of PPARγ/NF-κB signaling pathway in the pathogenesis of intrahepatic cholestasis of pregnancy. PLoS ONE 9(1):e87343. https://doi.org/10.1371/journal.pone.0087343
Bright JJ, Kanakasabai S, Chearwae W et al (2008) PPAR regulation of inflammatory signaling in CNS diseases. PPAR Res. https://doi.org/10.1155/2008/658520
Li M, Li Z, Sun X et al (2010) Heme oxygenase-1/p21WAF1 mediates peroxisome proliferator-activated receptor-gamma signaling inhibition of proliferation of rat pulmonary artery smooth muscle cells. FEBS J 277(6):1543–1550. https://doi.org/10.1111/j.1742-4658.2010.07581.x
Linares I, Farrokhi K, Echeverri J et al (2018) PPAR-gamma activation is associated with reduced liver ischemia-reperfusion injury and altered tissue-resident macrophages polarization in a mouse model. PLoS ONE 13(4):e0195212. https://doi.org/10.1371/journal.pone.0195212
Xiang S, Chen K, Xu L et al (2020) Bergenin exerts hepatoprotective effects by inhibiting the release of inflammatory factors, apoptosis and autophagy via the PPAR-γ pathway. Drug Des Dev Ther 14:129–143. https://doi.org/10.2147/DDDT.S229063
Chen Y, Liu S, Chen G (2019) Aggravation of cerebral ischemia/reperfusion injury by peroxisome proliferator-activated receptor-gamma deficiency via endoplasmic reticulum stress. Med Sci Monit 25:7518–7526. https://doi.org/10.12659/MSM.915914
Morales J, Li L, Fattah FJ et al (2014) Review of poly (ADP-ribose) polymerase (PARP) mechanisms of action and rationale for targeting in cancer and other diseases. Crit Rev Eukaryot Gene Expr 24(1):15–28. https://doi.org/10.1615/critreveukaryotgeneexpr.2013006875
Wu J, Tsai H, Cheung W et al (2016) PPARγ ameliorates neuronal apoptosis and ischemic brain injury via suppressing NF-κB-driven p22phox transcription. Mol Neurobiol 53:3626–3645. https://doi.org/10.1007/s12035-015-9294-z
Wu JS, Kao MH, Tsai HD et al (2018) Clinacanthus nutans mitigates neuronal apoptosis and ischemic brain damage through augmenting the C/EBPβ-Driven PPAR-γ transcription. Mol Neurobiol 55(7):5425–5438. https://doi.org/10.1007/s12035-017-0776-z
Ormerod BK, Hanft SJ, Asokan A et al (2013) PPARγ activation prevents impairments in spatial memory and neurogenesis following transient illness. Brain Behav Immun 29:28–38. https://doi.org/10.1016/j.bbi.2012.10.017
Reisman M, Adams KT (2014) Stem cell therapy: a look at current research, regulations, and remaining hurdles. P & T 39(12):846–857
Rajkovic O, Potjewyd G, Pinteaux E (2018) Regenerative medicine therapies for targeting neuroinflammation after stroke. Front Neurol 9:734. https://doi.org/10.3389/fneur.2018.00734
Quintanilla RA, Utreras E, Cabezas-Opazo FA (2014) Role of PPAR γ in the differentiation and function of neurons. PPAR Res. https://doi.org/10.1155/2014/768594
Cimini A, Cerù MP (2008) Emerging roles of peroxisome proliferator-activated receptors (PPARs) in the regulation of neural stem cells proliferation and differentiation. Stem Cell Rev 4(4):293–303. https://doi.org/10.1007/s12015-008-9024-2
Wada K, Nakajima A, Katayama K et al (2006) Peroxisome proliferator-activated receptor gamma-mediated regulation of neural stem cell proliferation and differentiation. J Biol Chem 281(18):12673–12681. https://doi.org/10.1074/jbc.M513786200
Xi Y, Zhang Y, Zhu S et al (2020) PPAR-mediated toxicology and applied pharmacology. Cells 9(2):352. https://doi.org/10.3390/cells9020352
Simons M, Nave KA (2015) Oligodendrocytes: myelination and axonal support. Cold Spring Harb Perspect Biol 8(1):a020479. https://doi.org/10.1101/cshperspect.a020479
Roth AD, Leisewitz AV, Jung JE et al (2003) PPAR gamma activators induce growth arrest and process extension in B12 oligodendrocyte-like cells and terminal differentiation of cultured oligodendrocytes. J Neurosci Res 72(4):425–435. https://doi.org/10.1002/jnr.10596
Wan Ibrahim WN, Tofighi R, Onishchenko N et al (2013) Perfluorooctane sulfonate induces neuronal and oligodendrocytic differentiation in neural stem cells and alters the expression of PPARγ in vitro and in vivo. Toxicol Appl Pharmacol 269(1):51–60. https://doi.org/10.1016/j.taap.2013.03.003
Yuan J, Ge H, Liu W et al (2017) M2 microglia promotes neurogenesis and oligodendrogenesis from neural stem/progenitor cells via the PPARγ signaling pathway. Oncotarget 8(12):19855–19865. https://doi.org/10.18632/oncotarget.15774
Morales-Garcia JA, Luna-Medina R, Alfaro-Cervello C et al (2011) Peroxisome proliferator-activated receptor γ ligands regulate neural stem cell proliferation and differentiation in vitro and in vivo. Glia 59(2):293–307. https://doi.org/10.1002/glia.21101
Esposito G, Scuderi C, Valenza M et al (2011) Cannabidiol reduces Aβ-induced neuroinflammation and promotes hippocampal neurogenesis through PPARγ involvement. PLoS ONE 6(12):e28668. https://doi.org/10.1371/journal.pone.0028668
Li L, Gan H, Jin H et al (2021) Astragaloside IV promotes microglia/macrophages M2 polarization and enhances neurogenesis and angiogenesis through PPARγ pathway after cerebral ischemia/reperfusion injury in rats. Int Immunopharmacol 92:107335. https://doi.org/10.1016/j.intimp.2020.107335
Kinouchi T, Kitazato KT, Shimada K et al (2018) Treatment with the PPARγ agonist pioglitazone in the early post-ischemia phase inhibits pro-inflammatory responses and promotes neurogenesis via the activation of innate- and bone marrow-derived stem cells in rats. Transl Stroke Res 9(3):306–316. https://doi.org/10.1007/s12975-017-0577-8
Li Y, Ren T, Xu L et al (2019) Propane-2-sulfonic acid octadec-9-enyl-amide, a novel peroxisome proliferator-activated receptors α and γ dual agonist, enhances hippocampal neurogenesis and neuroplasticity in rats with cerebral ischaemia. NeuroReport 30(18):1299–1306. https://doi.org/10.1097/WNR.0000000000001360
Font MA, Arboix A, Krupinski J (2010) Angiogenesis, neurogenesis and neuroplasticity in ischemic stroke. Curr Cardiol Rev 6(3):238–244. https://doi.org/10.2174/157340310791658802
Kotlinowski J, Jozkowicz A (2016) PPAR gamma and angiogenesis: endothelial cells perspective. J Diabetes Res. https://doi.org/10.1155/2016/8492353
de Oliveira Bristot VJ, de Bem Alves AC, Cardoso LR et al (2019) The role of PGC-1α/UCP2 signaling in the beneficial effects of physical exercise on the brain. Front Neurosci 13:292. https://doi.org/10.3389/fnins.2019.00292
Puigserver P, Spiegelman BM (2003) Peroxisome proliferator-activated receptor-gamma coactivator 1 alpha (PGC-1 alpha): transcriptional coactivator and metabolic regulator. Endocr Rev 24(1):78–90. https://doi.org/10.1210/er.2002-0012
Chu K, Lee ST, Koo JS et al (2006) Peroxisome proliferator-activated receptor-gamma-agonist, rosiglitazone, promotes angiogenesis after focal cerebral ischemia. Brain Res 1093(1):208–218. https://doi.org/10.1016/j.brainres.2006.03.114
Huang PH, Sata M, Nishimatsu H et al (2008) Pioglitazone ameliorates endothelial dysfunction and restores ischemia-induced angiogenesis in diabetic mice. Biomed Pharmacother 62(1):46–52. https://doi.org/10.1016/j.biopha.2007.06.014
Biscetti F, Straface G, Arena V et al (2009) Pioglitazone enhances collateral blood flow in ischemic hindlimb of diabetic mice through an Akt-dependent VEGF-mediated mechanism, regardless of PPARgamma stimulation. Cardiovasc Diabetol 8:49. https://doi.org/10.1186/1475-2840-8-49
Annabi B, Lord-Dufour S, Vézina A et al (2012) Resveratrol targeting of carcinogen-induced brain endothelial cell inflammation biomarkers MMP-9 and COX-2 is Sirt1-independent. Drug Target Insights 6:1–11. https://doi.org/10.4137/DTI.S9442
Grewal AK, Singh N, Singh TG (2019) Effects of resveratrol postconditioning on cerebral ischemia in mice: role of the sirtuin-1 pathway. Can J Physiol Pharmacol 97(11):1094–1101. https://doi.org/10.1139/cjpp-2019-0188
Biscetti F, Pecorini G, Arena V et al (2013) Cilostazol improves the response to ischemia in diabetic mice by a mechanism dependent on PPARγ. Mol Cell Endocrinol 381(1–2):80–87. https://doi.org/10.1016/j.mce.2013.07.011
Seok H, Lee M, Shin E et al (2019) Low-dose pioglitazone can ameliorate learning and memory impairment in a mouse model of dementia by increasing LRP1 expression in the hippocampus. Sci Rep 9:4414. https://doi.org/10.1038/s41598-019-40736-x
Rinwa P, Kaur B, Jaggi AS et al (2010) Involvement of PPAR-gamma in curcumin-mediated beneficial effects in experimental dementia. Naunyn-Schmied Arch Pharmacol 381:529–539. https://doi.org/10.1007/s00210-010-0511-z
McTigue DM, Tripathi R, Wei P et al (2007) The PPAR gamma agonist Pioglitazone improves anatomical and locomotor recovery after rodent spinal cord injury. Exp Neurol 205(2):396–406. https://doi.org/10.1016/j.expneurol.2007.02.009
Ma Y, Sullivan JC, Schreihofer DA (2010) Dietary genistein and equol (4’, 7 isoflavandiol) reduce oxidative stress and protect rats against focal cerebral ischemia. Am J Physiol 299(3):R871–R877. https://doi.org/10.1152/ajpregu.00031.2010
Rehni AK, Singh TG, Kakkar T et al (2011) Involvement of src-kinase activation in ischemic preconditioning induced protection of mouse brain. Life Sci 88(19–20):825–829. https://doi.org/10.1016/j.lfs.2011.02.024
Magi S, Piccirillo S, Amoroso S et al (2019) Excitatory amino acid transporters (EAATs): glutamate transport and beyond. Int J Mol Sci 20(22):5674. https://doi.org/10.3390/ijms20225674
Liu AJ, Hu YY, Li WB et al (2011) Cerebral ischemic pre-conditioning enhances the binding characteristics and glutamate uptake of glial glutamate transporter-1 in hippocampal CA1 subfield of rats. J Neurochem 119(1):202–209. https://doi.org/10.1111/j.1471-4159.2011.07396.x
Zhao CC, Jiang MY, Zhang LY et al (2019) Peroxisome proliferator-activated receptor gamma participates in the acquisition of brain ischemic tolerance induced by ischemic preconditioning via glial glutamate transporter 1 in vivo and in vitro. J Neurochem 151(5):608–625. https://doi.org/10.1111/jnc.14824
Kawahara K, Yanoma J, Tanaka M et al (2004) Nitric oxide produced during ischemia is toxic but crucial to preconditioning-induced ischemic tolerance of neurons in culture. Neurochem Res 29(4):797–804. https://doi.org/10.1023/b:nere.0000018853.30131.4d
Dirnagl U, Becker K, Meisel A (2009) Preconditioning and tolerance against cerebral ischaemia: from experimental strategies to clinical use. Lancet Neurol 8(4):398–412. https://doi.org/10.1016/S1474-4422(09)70054-7
Blanco M, Moro MA, Dávalos A et al (2005) Increased plasma levels of 15-deoxyDelta prostaglandin J2 are associated with good outcome in acute atherothrombotic ischemic stroke. Stroke 36(6):1189–1194. https://doi.org/10.1161/01.STR.0000166054.55993.e5
Romera C, Hurtado O, Mallolas J et al (2007) Ischemic preconditioning reveals that GLT1/EAAT2 glutamate transporter is a novel PPARgamma target gene involved in neuroprotection. J Cerebr Blood Flow Metab 27(7):1327–1338. https://doi.org/10.1038/sj.jcbfm.9600438
Wynne AM, Mocanu MM, Yellon DM (2005) Pioglitazone mimics preconditioning in the isolated perfused rat heart: a role for the prosurvival kinases PI3K and P42/44MAPK. J Cardiovasc Pharmacol 46(6):817–822. https://doi.org/10.1097/01.fjc.0000188365.07635.57
Moolman JA, Hartley S, Van Wyk J et al (2006) Inhibition of myocardial apoptosis by ischaemic and beta-adrenergic preconditioning is dependent on p38 MAPK. Cardiovasc Drugs Ther 20(1):13–25. https://doi.org/10.1007/s10557-006-6257-7
Li J, Lang MJ, Mao XB et al (2008) Antiapoptosis and mitochondrial effect of pioglitazone preconditioning in the ischemic/reperfused heart of rat. Cardiovasc Drugs Ther 22(4):283–291. https://doi.org/10.1007/s10557-008-6115-x
Ren Y, Wang C, Xu J et al (2019) Cafestol and kahweol: a review on their bioactivities and pharmacological properties. Int J Mol Sci 20(17):4238. https://doi.org/10.3390/ijms20174238
Caiozzi G, Wong BS, Ricketts ML (2012) Dietary modification of metabolic pathways via nuclear hormone receptors. Cell Biochem Funct 30(7):531–551. https://doi.org/10.1002/cbf.2842
Ji J, Wu L, Feng J et al (2020) Cafestol preconditioning attenuates apoptosis and autophagy during hepatic ischemia-reperfusion injury by inhibiting ERK/PPARγ pathway. Int Immunopharmacol 84:106529. https://doi.org/10.1016/j.intimp.2020.106529
Zeng Y, Xie K, Dong H et al (2012) Hyperbaric oxygen preconditioning protects cortical neurons against oxygen-glucose deprivation injury: role of peroxisome proliferator-activated receptor-gamma. Brain Res 1452:140–150. https://doi.org/10.1016/j.brainres.2012.02.063
Bassaganya-Riera J, Reynolds K, Martino-Catt S et al (2004) Activation of PPAR gamma and delta by conjugated linoleic acid mediates protection from experimental inflammatory bowel disease. Gastroenterology 127(3):777–791. https://doi.org/10.1053/j.gastro.2004.06.049
Słowikowski BK, Drzewiecka H, Malesza M et al (2020) The influence of conjugated linoleic acid on the expression of peroxisome proliferator-activated receptor-γ and selected apoptotic genes in non-small cell lung cancer. Mol Cell Biochem 466(1–2):65–82. https://doi.org/10.1007/s11010-020-03689-8
Chambrier C, Bastard JP, Rieusset J et al (2002) Eicosapentaenoic acid induces mRNA expression of peroxisome proliferator-activated receptor gamma. Obes Res 10(6):518–525. https://doi.org/10.1038/oby.2002.70
Zirpoli H, Chang CL, Carpentier YA et al (2020) Novel approaches for omega-3 fatty acid therapeutics: chronic versus acute administration to protect heart, brain, and spinal cord. Annu Rev Nutr 40:161–187. https://doi.org/10.1146/annurev-nutr-082018-124539
Abdelrahman M, Sivarajah A, Thiemermann C (2005) Beneficial effects of PPAR-gamma ligands in ischemia-reperfusion injury, inflammation and shock. Cardiovasc Res 65(4):772–781. https://doi.org/10.1016/j.cardiores.2004.12.008
Itoh T, Fairall L, Amin K et al (2008) Structural basis for the activation of PPARgamma by oxidized fatty acids. Nat Struct Mol Biol 15(9):924–931. https://doi.org/10.1038/nsmb.1474
Bazan NG (2009) Cellular and molecular events mediated by docosahexaenoic acid-derived neuroprotectin D1 signaling in photoreceptor cell survival and brain protection. Prostaglandins Leukot Essent Fatty Acids 81(2–3):205–211. https://doi.org/10.1016/j.plefa.2009.05.024
Zhao Y, Calon F, Julien C et al (2011) Docosahexaenoic acid-derived neuroprotectin D1 induces neuronal survival via secretase- and PPARγ-mediated mechanisms in Alzheimer’s disease models. PLoS ONE 6(1):e15816. https://doi.org/10.1371/journal.pone.0015816
Bazan NG (2012) Neuroinflammation and proteostasis are modulated by endogenously biosynthesized neuroprotectin D1. Mol Neurobiol 46(1):221–226. https://doi.org/10.1007/s12035-012-8322-5
Belayev L, Freitas RS, Marcell SJ et al (2017) Chapter 52—lipid mediators. In: Caplan LR, Biller J, Leary MC, Lo EH, Thomas AJ, Yenari M, Zhang JH (eds) Primer on cerebrovascular diseases, 2nd edn. Academic Press, London, pp 256–260
Liao Z, Dong J, Wu W et al (2012) Resolvin D1 attenuates inflammation in lipopolysaccharide-induced acute lung injury through a process involving the PPARγ/NF-κB pathway. Respir Res 13(1):110. https://doi.org/10.1186/1465-9921-13-110
Saito T, Hasegawa-Moriyama M, Kurimoto T et al (2015) Resolution of inflammation by resolvin D1 is essential for peroxisome proliferator-activated receptor-γ-mediated analgesia during postincisional pain development in Type 2 diabetes. Anesthesiology 123(6):1420–1434. https://doi.org/10.1097/ALN.0000000000000892
Villacorta L, Zhang J, Garcia-Barrio MT et al (2007) Nitro-linoleic acid inhibits vascular smooth muscle cell proliferation via the Keap1/Nrf2 signaling pathway. Am J Physiol 293(1):770–776. https://doi.org/10.1152/ajpheart.00261.2007
Panati K, Subramani PA, Reddy MM et al (2019) The nitrated fatty acid, 10-nitrooleate inhibits the neutrophil chemotaxis via peroxisome proliferator-activated receptor gamma in CLP-induced sepsis in mice. Int Immunopharmacol 72:159–165. https://doi.org/10.1016/j.intimp.2019.04.001
Nie H, Xue X, Li J et al (2015) Nitro-oleic acid attenuates OGD/R-triggered apoptosis in renal tubular cells via inhibition of Bax mitochondrial translocation in a PPAR-γ-dependent manner. Cell Physiol Biochem 35(3):1201–1218. https://doi.org/10.1159/000373944
Mazidi M, Karimi E, Meydani M et al (2016) Potential effects of curcumin on peroxisome proliferator-activated receptor-γ in vitro and in vivo. World J Methodol 6(1):112–117. https://doi.org/10.5662/wjm.v6.i1.112
Choi JH, Jin SW, Choi CY et al (2017) Capsaicin inhibits dimethylnitrosamine-induced hepatic fibrosis by inhibiting the TGF-β1/Smad pathway via peroxisome proliferator-activated receptor gamma activation. J Agric Food Chem 65(2):317–326. https://doi.org/10.1021/acs.jafc.6b04805
Robich MP, Osipov RM, Chu LM et al (2011) Resveratrol modifies risk factors for coronary artery disease in swine with metabolic syndrome and myocardial ischemia. Eur J Pharmacol 664(1–3):45–53. https://doi.org/10.1016/j.ejphar.2011.04.059
Aires V, Brassart B, Carlier A et al (2014) A role for peroxisome proliferator-activated receptor gamma in resveratrol-induced colon cancer cell apoptosis. Mol Nutr Food Res 58(9):1785–1794. https://doi.org/10.1002/mnfr.201300962
Calleri E, Pochetti G, Dossou K et al (2014) Resveratrol and its metabolites bind to PPARs. ChemBioChem 15(8):1154–1160. https://doi.org/10.1002/cbic.201300754
Park JW, Jang YH, Kim JM et al (2009) Green tea polyphenol (-)-epigallocatechin gallate reduces neuronal cell damage and up-regulation of MMP-9 activity in hippocampal CA1 and CA2 areas following transient global cerebral ischemia. J Neurosci Res 87(2):567–575. https://doi.org/10.1002/jnr.21847
Wang S, Wang J, Wei H et al (2020) Genistein attenuates acute cerebral ischemic damage by inhibiting the NLRP3 inflammasome in reproductively senescent mice. Front Aging Neurosci 12:153. https://doi.org/10.3389/fnagi.2020.00153
Xiong D, Deng Y, Huang B et al (2016) Icariin attenuates cerebral ischemia-reperfusion injury through inhibition of inflammatory response mediated by NF-κB, PPARα and PPARγ in rats. Int Immunopharmacol 30:157–162. https://doi.org/10.1016/j.intimp.2015.11.035
Ban K, Sprunt JM, Martin S et al (2011) Glutamine activates peroxisome proliferator-activated receptor-γ in intestinal epithelial cells via 15-S-HETE and 13-OXO-ODE: a novel mechanism. Am J Physiol Gastrointest Liver Physiol 301(3):G547–G554. https://doi.org/10.1152/ajpgi.00174.2011
Wang AL, Niu Q, Shi N et al (2015) Glutamine ameliorates intestinal ischemia-reperfusion injury in rats by activating the Nrf2/Are signaling pathway. Int J Clin Exp Pathol 8(7):7896–7904
Berni Canani R, Di Costanzo M, Leone L (2012) The epigenetic effects of butyrate: potential therapeutic implications for clinical practice. Clin Epigenet 4(1):4. https://doi.org/10.1186/1868-7083-4-4
Takaki K, Mitsuyama K, Tsuruta O et al (2006) Attenuation of experimental colonic injury by thiazolidinedione agents. Inflamm Res 55(1):10–15. https://doi.org/10.1007/s00011-005-0002-8
Dworzanski T, Celinski K, Korolczuk A et al (2010) Influence of the peroxisome proliferator-activated receptor gamma (PPAR-γ) agonist, rosiglitazone and antagonist, biphenol-A-diglicydyl ether (BADGE) on the course of inflammation in the experimental model of colitis in rats. J Physiol Pharmacol 61(6):683–693
Zingarelli B, Sheehan M, Hake PW et al (2003) Peroxisome proliferator activator receptor-gamma ligands, 15-deoxy-Delta(12,14)-prostaglandin J2 and ciglitazone, reduce systemic inflammation in polymicrobial sepsis by modulation of signal transduction pathways. J Immunol 171(12):6827–6837. https://doi.org/10.4049/jimmunol.171.12.6827
Ryu S, Kim DS, Lee MW et al (2018) Anti-leukemic effects of PPARγ ligands. Cancer Lett 418:10–19. https://doi.org/10.1016/j.canlet.2018.01.020
Murray JR, de la Vega L, Hayes JD et al (2019) Induction of the antioxidant response by the transcription factor NRF2 increases bioactivation of the mutagenic air pollutant 3-nitrobenzanthrone in human lung cells. Chem Res Toxicol 32(12):2538–2551. https://doi.org/10.1021/acs.chemrestox.9b00399
Wang YY, Yang YX, Zhe H et al (2014) Bardoxolone methyl (CDDO-Me) as a therapeutic agent: an update on its pharmacokinetic and pharmacodynamic properties. Drug Des Dev Ther 8:2075–2088. https://doi.org/10.2147/DDDT.S68872
Monsalve FA, Pyarasani RD, Delgado-Lopez F et al (2013) Peroxisome proliferator-activated receptor targets for the treatment of metabolic diseases. Mediators Inflamm. https://doi.org/10.1155/2013/549627
Ribeiro Filho HV, Bernardi Videira N, Bridi AV et al (2018) Screening for PPAR non-agonist ligands followed by characterization of a hit, AM-879, with additional no-adipogenic and cdk5-mediated phosphorylation inhibition properties. Front Endocrinol 9:11. https://doi.org/10.3389/fendo.2018.00011
Birrell MA, Patel HJ, McCluskie K et al (2004) PPAR-gamma agonists as therapy for diseases involving airway neutrophilia. Eur Respir J 24(1):18–23. https://doi.org/10.1183/09031936.04.00098303
Perrotta C, Pellegrino P, Moroni E et al (2015) Five-aminosalicylic Acid: an update for the reappraisal of an old drug. Gastroenterol Res Pract. https://doi.org/10.1155/2015/456895
Yousefipour Z, Chug N, Marek K et al (2017) Contribution of PPARγ in modulation of acrolein-induced inflammatory signaling in gp91phox knock-out mice. Biochem Cell Biol 95(4):482–490. https://doi.org/10.1139/bcb-2016-0198
Kurebayashi S, Xu X, Ishii S et al (2005) A novel thiazolidinedione MCC-555 down-regulates tumor necrosis factor-alpha-induced expression of vascular cell adhesion molecule-1 in vascular endothelial cells. Atherosclerosis 182(1):71–77. https://doi.org/10.1016/j.atherosclerosis.2005.02.004
Sharma S, Sowjanya A, Kumari M et al (2006) Biochemical mechanism of insulin sensitization, lipid modulation and anti-atherogenic potential of PPAR alpha/gamma dual agonist: ragaglitazar. Life Sci 80(3):235–244. https://doi.org/10.1016/j.lfs.2006.09.009
Massaro M, Scoditti E, Pellegrino M et al (2016) Therapeutic potential of the dual peroxisome proliferator activated receptor (PPAR)α/γ agonist aleglitazar in attenuating TNF-α-mediated inflammation and insulin resistance in human adipocytes. Pharmacol Res 107:125–136. https://doi.org/10.1016/j.phrs.2016.02.027
Wang Y, Yang YS, Tang XC et al (2011) T33, a novel peroxisome proliferator-activated receptor γ/α agonist, exerts neuroprotective action via its anti-inflammatory activities. Acta Pharmacol Sin 32(9):1100–1108. https://doi.org/10.1038/aps.2011.69
Zhang H, You L, Zhao M (2019) Rosiglitazone attenuates paraquat-induced lung fibrosis in rats in a PPAR gamma-dependent manner. Eur J Pharmacol 851:133–143. https://doi.org/10.1016/j.ejphar.2019.02.037
Rieusset J, Touri F, Michalik L et al (2002) A new selective peroxisome proliferator-activated receptor gamma antagonist with antiobesity and antidiabetic activity. Mol Endocrinol (Baltimore, Md) 16(11):2628–2644. https://doi.org/10.1210/me.2002-0036
Yu L, Su X, Li S et al (2020) Microglia and their promising role in ischemic brain injuries: an update. Front Cell Neurosci 14:211. https://doi.org/10.3389/fncel.2020.00211
Hong SJ, Choi SC, Ahn CM et al (2011) Telmisartan reduces neointima volume and pulse wave velocity 8 months after zotarolimus-eluting stent implantation in hypertensive type 2 diabetic patients. Heart (British Cardiac Society) 97(17):1425–1432. https://doi.org/10.1136/hrt.2011.225193
Acknowledgements
The authors are grateful to the Chitkara College of Pharmacy, Chitkara University, Rajpura, Patiala, Punjab, India for providing the necessary facilities to carry out the research work.
Author information
Authors and Affiliations
Contributions
Conceptualization: Conceived and designed the experiments: TGS. Analyzed the data: AM, HKK Wrote the manuscript: AM, NG. Visualization: HKK. Editing of the Manuscript: TGS. Critically reviewed the article: TGS. Supervision: TGS. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
There are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mannan, A., Garg, N., Singh, T.G. et al. Peroxisome Proliferator-Activated Receptor-Gamma (PPAR-ɣ): Molecular Effects and Its Importance as a Novel Therapeutic Target for Cerebral Ischemic Injury. Neurochem Res 46, 2800–2831 (2021). https://doi.org/10.1007/s11064-021-03402-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-021-03402-1