Abstract
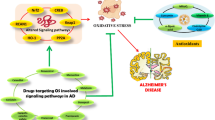
Protein misfolding and aggregation of amyloid beta (Aβ) peptide, as well as formation of neurofibrillary tangles (NFTs) are the signature hallmarks of Alzheimer’s disease (AD) pathology. To prevent this, molecular chaperones come into play as they facilitate the refolding of the misfolded proteins and cell protection under stress. Here, we have evaluated the possible effects of Ginkgo biloba (GBE) against aggregation of the Aβ through activation of heat shock proteins (HSPs) in the Aluminium (Al) induced AD based model. GBE (100 mg/kg body weight) was administered per oral to the female SD rats in conjunction with intraperitoneal (i.p.) injection of Al lactate (10 mg/kg body weight) for six weeks. Pretreated animals were administered GBE for additional two weeks prior to any exposure of Al. GBE administration resulted in decrease in Aβ aggregation, ubiquitin deposition, accompanying a significant decline in APP & Tau protein hyperphosphorylation which can be attributed to activation of Heat shock factor (HSF-1) and upregulation in the protein expression of HSPs. Histopathological investigation studies have also shown the decrease in aggregation of Aβ peptide by GBE administration. Additionally, the decrease in ROS levels and Aβ aggregation by GBE administration prohibited the decline in the neurotransmitter levels and monoamine oxidase levels in hippocampus and cortex. This further caused improvement in learning and memory of the animals. In conclusion, our results indicate that GBE prevents the symptoms of Al induced AD like pathophysiology by upregulating the HSPs levels and decreasing the aggregation load.
Graphic Abstract
















Similar content being viewed by others
Abbreviations
- Al:
-
Aluminium
- ROS:
-
Reactive oxygen species
- DCF:
-
2′7′-Dichlorofluorescceine
- Aβ:
-
Amyloid beta
- FTIR:
-
Fourier transform infrared spectroscopy
- HSPs:
-
Heat shock proteins
- AChE:
-
Acetylcholinesterase
- MWM:
-
Morris water maze
- GBE:
-
Ginkgo biloba extract
References
Laabbar W, Elgot A, Kissani N, Gamrani H (2014) Chronic aluminum intoxication in rat induced both serotonin changes in the dorsal raphe nucleus and alteration of glycoprotein secretion in the subcommissural organ: Immunohistochemical study. Neurosci Lett 577:72–76
Foster HD (2000) How aluminum causes Alzheimer’s disease: the implications for prevention and treatment of Foster’s multiple antagonist hypothesis. J Orthomol Med 15:21–51. https://doi.org/10.1051/meca
Yumoto S, Kakimi S, Ohsaki A, Ishikawa A (2009) Demonstration of aluminum in amyloid fibers in the cores of senile plaques in the brains of patients with Alzheimer’s disease. J Inorg Biochem 103(11):1579–1584
Liaquat L, Sadir S, Batool Z, Tabassum S, Shahzad S, Afzal A, Haider S (2019) Acute aluminum chloride toxicity revisited: Study on DNA damage and histopathological, biochemical and neurochemical alterations in rat brain. Life Sci 217:202–211
Yan R, Vassar R (2014) Targeting the β secretase BACE1 for Alzheimer's disease therapy. Lancet Neurol 13(3):319–329
Miu AC, Andreescu CE (2003) A behavioral and histological study of the effects of long-term exposure of adult rats to aluminum. Intern J Neurosci 113:1197–1211. https://doi.org/10.1080/00207450390232292
Kawahara M, Kato-Negishi M (2011) Link between aluminum and the pathogenesis of Alzheimer's disease: the integration of the aluminum and amyloid cascade hypotheses. Int J Alzheimer’s Dis 2011:276393
Vasudevaraju BP, Govindaraju M, Palanisamy AP, Sambamurti K, Rao KSJ (2008) Molecular toxicity of aluminium in relation to neurodegeneration. Indian J Med Res 128:545–556
Ricchelli F, Drago D, Filippi B, Tognon G, Zatta P (2005) Aluminum-triggered structural modifications and aggregation of β-amyloids. Cell Mol Life Sci 62(15):1724–1733
Yang EY, Guo-Ross SX, Bondy SC (1999) The stabilization of ferrous iron by a toxic β-amyloid fragment and by an aluminum salt. Brain Res 839(2):221–226
Barone E (2016) Editorial (Thematic Issue: Oxidative Stress and Alzheimer Disease: Where Do We Stand?). Curr Alzheimer Res 13:108–111. https://doi.org/10.2174/156720501302160101123849
Shankar GM, Li S, Mehta TH, Garcia-Munoz A, Shepardson NE, Smith I, Brett FM, Farrell MA, Rowan MJ, Lemere CA, Regan CM (2008) Amyloid-β protein dimers isolated directly from Alzheimer's brains impair synaptic plasticity and memory. Nat Med 14(8):837
Praticò D, Uryu K, Sung S, Tang S, Trojanowski JQ, Lee VM (2002) Aluminum modulates brain amyloidosis through oxidative stress in APP transgenic mice. FASEB J 16(9):1138–1140
Rodella LF, Ricci F, Borsani E, Stacchiotti A, Foglio E, Favero G, Rezzani R, Mariani C, Bianchi R (2008) Aluminium exposure induces Alzheimer s disease-like histopathological alterations in mouse brain. Histol Histopathol 23(4):433–439
Kobayashi K, Yumoto S, Nagai H, Hosoyama Y, Imamura M, Masuzawa SI, Koizumi Y, Yamashita H (1990) 26Al tracer experiment by accelerator mass spectrometry and its application to the studies for amyotrophic lateral sclerosis and Alzheimer's disease. I. Proc Jpn Acad Ser B 66(10):189–192
Sherman MY, Goldberg AL (2001) Cellular defenses against unfolded proteins: a cell biologist thinks about neurodegenerative diseases. Neuron 29(1):15–32
Muchowski PJ, Wacker JL (2005) Modulation of neurodegeneration by molecular chaperones. Nat Rev Neurosci 6:11–22. https://doi.org/10.1038/nrn1587
Sreedhar AS, Csermely P (2004) Heat shock proteins in the regulation of apoptosis: new strategies in tumor therapy: a comprehensive review. Pharmacol Ther 101(3):227–257
Stefani M, Dobson CM (2003) Protein aggregation and aggregate toxicity: new insights into protein folding, misfolding diseases and biological evolution. J Mol Med 81:678–699. https://doi.org/10.1007/s00109-003-0464-5
Sood PK, Nahar U, Nehru B (2011) Curcumin attenuates aluminum-induced oxidative stress and mitochondrial dysfunction in rat brain. Neurotox Res 20:351–361. https://doi.org/10.1007/s12640-011-9249-8
Thakur P, Nehru B (2014) Modulatory effects of sodium salicylate on the factors affecting protein aggregation during rotenone induced Parkinson’s disease pathology. Neurochem Int 75:1–10. https://doi.org/10.1016/j.neuint.2014.05.002
Thakur P, Nehru B (2014) Long-term heat shock proteins (HSPs) induction by carbenoxolone improves hallmark features of Parkinson's disease in a rotenone-based model. Neuropharmacology 79:190–200
Schwarzbach C, Vauth C, Roll S, Willich SN, Weinmann S (2010) Effects of Ginkgo biloba in dementia: systematic review and meta-analysis. BMC Geriatr. https://doi.org/10.1186/1471-2318-10-14
DeFeudis FV, Drieu K (2000) Ginkgo biloba extract (EGb 761) and CNS functions basic studies and clinical applications. Curr Drug Targets 1(1):25–58
Li H, Sun X, Yu F, Xu L, Miu J, Xiao P (2018) In silico investigation of the pharmacological mechanisms of beneficial effects of Ginkgo biloba L. on Alzheimer’s Disease. Nutrients 10(5):589
Augustin S, Rimbach G, Augustin K, Schliebs R, Wolffram S, Cermak R (2009) Effect of a short- and long-term treatment with Ginkgo biloba extract on amyloid precursor protein levels in a transgenic mouse model relevant to Alzheimer’s disease. Arch Biochem Biophys 481:177–182. https://doi.org/10.1016/j.abb.2008.10.032
Colciaghi F, Borroni B, Zimmermann M, Bellone C, Longhi A, Padovani A, Cattabeni F, Christen Y, Di Luca M (2004) Amyloid precursor protein metabolism is regulated toward alpha-secretase pathway by Ginkgo biloba extracts. Neurobiol Dis 16:454–460. https://doi.org/10.1016/j.nbd.2004.03.011
Yao ZX, Han Z, Drieu K, Papadopoulos V (2004) Ginkgo biloba extract (Egb 761) inhibits β-amyloid production by lowering free cholesterol levels. J Nutr Biochem 15:749–756. https://doi.org/10.1016/j.jnutbio.2004.06.008
Eckert A (2012) Mitochondrial effects of Ginkgo biloba extract. Int Psychogeriatr 24:18–20. https://doi.org/10.1017/S1041610212000531
Verma S, Ranawat P, Sharma N, Nehru B (2019) Ginkgo biloba attenuates aluminum lactate-induced neurotoxicity in reproductive senescent female rats: behavioral, biochemical, and histopathological study. Environ Sci Pollut Res 18:1–20
Krewski D, Yokel RA, Nieboer E, Borchelt D, Cohen J, Harry J, Kacew S, Lindsay J, Mahfouz AM, Rondeau V (2007) Human health risk assessment for aluminium, aluminium oxide, and aluminium hydroxide. J Toxicol Environ Health Part B 10(S1):1–269
Colomina MT, Peris-Sampedro F (2017) Aluminum and Alzheimer’s disease. In: Aschner M, Costa L (eds) Neurotoxicity of metals. Springer, Cham, pp 183–197
Best TM, Fiebig R, Corr DT, Brickson S, Ji L (1999) Free radical activity, antioxidant enzyme, and glutathione changes with muscle stretch injury in rabbits. J Appl Physiol 87:74–82. https://doi.org/10.1152/jappl.1999.87.1.74
Kapoor M, Sharma N, Sandhir R, Nehru B (2018) Effect of the NADPH oxidase inhibitor apocynin on ischemia-reperfusion hippocampus injury in rat brain. Biomed Pharmacother 97:458–472
Sivakumar S, Sivasubramanian J, Raja B (2012) Aluminium induced structural, metabolic alterations and protective effects of desferrioxamine in the brain tissue of mice: an FTIR study. Spectrochimica Acta Part A 99:252–258
Sivakumar S, Khatiwada CP, Sivasubramanian J, Raja B (2014) Protective effects of deferiprone and desferrioxamine in brain tissue of aluminum intoxicated mice: an FTIR study. Biomed Prevent Nutr 4(1):53–61
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Fischer AH, Jacobson KA, Rose J, Zeller R (2008) Hematoxylin and eosin staining of tissueand cell sections. Cold Spring Harb Protoc 3:4986–4988. https://doi.org/10.1101/pdb.prot4986
Morris R (1984) Developments if a water-maze procedure for studying spatial learning in the rat. J Neurosci Method 11:47–60. https://doi.org/10.1016/0165-0270(84)90007-4
Nehru B, Bhalla P, Garg A (2006) Evidence for centrophenoxine as a protective drug in aluminium induced behavioral and biochemical alteration in rat brain. Mol Cell Biochem 290:33–42. https://doi.org/10.1007/s11010-006-9125-7
Church WH (2005) Column chromatography analysis of brain tissue: an advanced laboratory exercise for neuroscience majors. J Undergraduate Neurosci Edu 3(2):A36
Ellman GL, Courtney KD, Andres V, Featherstone RM (1961) A new and rapid colorimetric determination of Acetylcholinesterase activity. Biochem Pharmacol 7(2):88–90
Gupta D, Kurhe Y, Radhakrishnan M (2014) Antidepressant effects of insulin in streptozotocin induced diabetic mice: modulation of brain serotonin system. Physiol Behav 129:73–78
Baker MJ, Trevisan J, Bassan P, Bhargava R, Butler HJ, Dorling KM, Fielden PR, Fogarty SW, Fullwood NJ, Heys KA, Hughes C (2014) Using Fourier transform IR spectroscopy to analyze biological materials. Nat Protocols 9(8):1771
Whitley D, Goldberg SP, Jordan WD (1999) Heat shock proteins: a review of the molecular chaperones. J Vasc Surg 29(4):748–751
Qu Z, Titus AS, Xuan Z, D’Mello SR (2018) Neuroprotection by heat shock factor-1 (HSF1) and trimerization-deficient mutant identifies novel alterations in gene expression. Sci Rep 8(1):17255
Eisele YS, Monteiro C, Fearns C, Encalada SE, Wiseman RL, Powers ET, Kelly JW (2015) Targeting protein aggregation for the treatment of degenerative diseases. Nature reviews Drug Discov 14(11):759
Xue C, Lin TY, Chang D, Guo Z (2017) Thioflavin T as an amyloid dye: fibril quantification, optimal concentration and effect on aggregation. R Soc Open Sci 4(1):160696
Sharma S, Verma S, Kapoor M, Saini A, Nehru B (2016) Alzheimer’s disease like pathology induced six weeks after aggregated amyloid-beta injection in rats: increased oxidative stress and impaired long-term memory with anxiety-like behavior. Neurol Res 38(9):838–850
Rajamohamedsait HB, Sigurdsson EM (2012) Histological staining of amyloid and pre-amyloid peptides and proteins in mouse tissue. Methods Mol Biol 849:411–424
Maezawa I, Hong HS, Liu R, Wu CY, Cheng RH, Kung MP, Kung HF, Lam KS, Oddo S, LaFerla FM, Jin LW (2008) Congo red and thioflavin-T analogs detect Aβ oligomers. J Neurochem 104(2):457–468
Uchihara T (2007) Silver diagnosis in neuropathology: principles, practice and revised interpretation. Acta Neuropathol 113(5):483–499
Balgoon MJ, Raouf GA, Qusti SY, Ali SS (2015) ATR-IR study of the mechanism of aluminum chloride induced alzheimer’s disease; curative and protective effect of Lipidium sativum water extract on hippocampus rats brain tissue. Int J Med Health Biomed Bioengi Pharma Eng 9(11):782–792
Edmondson DE, Binda C (2018) Monoamine oxidases. In: Harris JR, Boekema E (eds) Membrane protein complexes: structure and function. Springer, Singapore, pp 117–139
Christen Y (2000) Oxidative stress and Alzheimer disease. Am J Clin Nutr 71:621S–629S. https://doi.org/10.1093/ajcn/71.2.621s
Kaur S, Chhabra R, Nehru B (2013) Phytomedicine Ginkgo biloba extract attenuates hippocampal neuronal loss and cognitive dysfunction resulting from trimethyltin in mice. Eur J Integr Med 20:178–186. https://doi.org/10.1016/j.phymed.2012.10.003
Ahlemeyer B, Krieglstein J (2003) Review neuroprotective effects of Ginkgo biloba extract C. Cell Mol Life Sci 60:1779–1792. https://doi.org/10.1007/s00018-003-2324-4
Shi C, Zhao L, Zhu B, Li Q, Yew DT, Yao Z, Xu J (2009) Dosage effects of EGb761 on hydrogen peroxide-induced cell death in SH-SY5Y cells. Chemico-Biol Interact 180(3):389–397
Shi C, Liu J, Wu F, Yew D (2010) Ginkgo biloba extract in Alzheimer’s disease: from action mechanisms to medical practice. Int J Mol Sci 11(1):107–123
Shinoki A, Lang W, Thawornkuno C, Kang HK, Kumagai Y, Okuyama M, Mori H, Kimura A, Ishizuka S, Hara H (2013) A novel mechanism for the promotion of quercetin glycoside absorption by megalo α-1,6-glucosaccharide in the rat small intestine. Food Chem 136:293–296. https://doi.org/10.1016/j.foodchem.2012.08.028
Smith JV, Luo Y (2004) Studies on molecular mechanisms of Ginkgo biloba extract. Appl Microbiol Biotechnol 64:465–472. https://doi.org/10.1007/s00253-003-1527-9
Van Beek TA (2002) Chemical analysis of Ginkgo biloba leaves and extracts. J Chromatogr A 967:21–55. https://doi.org/10.1016/S0021-9673(02)00172-3
Kakimura JI, Kitamura Y, Takata K, Umeki M, Suzuki S, Shibagaki K, Taniguchi T, Nomura Y, Gebicke-Haerter PJ, Smith MA, Perry G, Shimohama S (2002) Microglial activation and amyloid-beta clearance induced by exogenous heat-shock proteins. FASEB J 16:601–603
Kakimura JI, KitamuraY TT, Shimohama S, Gebicke-Haerter PJ (2001) BiP/GRP78-induced production of cytokines and uptake of amyloid-β(1–42) peptide in microglia. Biochem Biophys Res Commun 281:6–10. https://doi.org/10.1006/bbrc.2001.4299
Wan W, Kalionis B, Chen C, Li Y, Xia S, Zhang C, Murthi P, Liu L (2016) EGb761 protects against Aβ1-42 oligomer-induced cell damage via endoplasmic reticulum stress activation andHsp70 protein expression increase in SH-SY5Y cells. Exp Gerontol 75:56–63. https://doi.org/10.1016/j.exger.2016.01.003
Namba T, Katsuno M, Takehara M, Mizushima T, Adachi H, Sobue G, Hoshino T, Murao N, Suzuki T, Matsushima T (2011) Suppression of Alzheimer’s disease-related phenotypes by expression of heat shock protein 70 in mice. J Neurosci 31:5225–5234. https://doi.org/10.1523/jneurosci.5478-10.2011
Yang Y, Turner RS, Gaut JR (1998) The Chaperone BiP/GRP78 binds to amyloid precursor protein and decreases Aβ 40 and Aβ 42 secretion. J Biol Chem 273(40):25552–25555
Maiti P, Manna J, Veleri S, Frautschy S (2014) Molecular chaperone dysfunction in neurodegenerative diseases and effects of curcumin. Biomed Res Int. https://doi.org/10.1155/2014/495091
Zourlidou A, Payne Smith MD, Latchman DS (2004) HSP27 but not HSP70 has a potent protective effect against α-synuclein-induced cell death in mammalian neuronal cells. J Neurochem 88:1439–1448. https://doi.org/10.1046/j.1471-4159.2003.02273.x
Shimura H, Miura-Shimura Y, Kosik KS (2004) Binding of tau to heat shock protein 27 leads to decreased concentration of hyperphosphorylated tau and enhanced cell survival. J Biol Chem 279:17957–17962. https://doi.org/10.1074/jbc.M400351200
Toyran N, Zorlu F, Dönmez G, Öğe K, Severcan F (2004) Chronic hypoperfusion alters the content and structure of proteins and lipids of rat brain homogenates: a Fourier transform infrared spectroscopy study. Eur Biophys J 33(6):549–554
Dzyuba SV, Petrovic AG, Polavarapu PL, He J, Nakanishi K, Berova N (2007) Spectroscopic investigation of Ginkgo biloba terpene trilactones and their interaction with amyloid peptide Aβ(25–35). Spectrochim Acta Part A Mol Biomol Spectrosc 69:1213–1222. https://doi.org/10.1016/j.saa.2007.06.030
Linardaki ZI, Orkoula MG, Kokkosis AG, Lamari FN, Margarity M (2013) Investigation of the neuroprotective action of saffron (Crocus sativus L.) in aluminum-exposed adult mice through behavioral and neurobiochemical assessment. Food Chem Toxicol 52:163–170
Blennow K, Leon MJ, De Zetterberg H (2001) Seminar Alzheimer’s disease. Lancet 368:1–17. https://doi.org/10.1016/S0140-6736(06)69113-7
Hörtnagl H, Potter PE, Hanin I (1987) Effect of cholinergic deficit induced by ethylcholine aziridinium on serotonergic parameters in rat brain. Neuroscience 22(1):203–213
Kumar S (2002) Aluminium-induced changes in the rat brain serotonin system. Food Chem Toxicol 40:1875–1880. https://doi.org/10.1016/S0278-6915(02)00180-1
Durán R, Arufe MC, Arias B, Alfonso M (1995) Effect of domoic acid on brain amino acid levels. Rev Esp Fisiol 51:23–27
Luo Y, Smith JV, Paramasivam V, Burdick A, Curry KJ, Buford JP, Khan I, Netzer WJ, Xu H, Butko P (2002) Inhibition of amyloid-β aggregation and caspase-3 activation by the Ginkgo biloba extract EGb761. Proc Natl Acad Sci 99(19):12197–12202
Gong QH, Wu Q, Huang XN, Sun AS, Shi JS (2005) Protective effects of Ginkgo biloba leaf extract on aluminum-induced brain dysfunction in rats. Life Sci 77:140–148. https://doi.org/10.1016/j.lfs.2004.10.067
Abd-Elhady RM, Elsheikh AM, Khalifa AE (2013) Anti-amnestic properties of Ginkgo biloba extract on impaired memory function induced by aluminum in rats. Int J Dev Neurosci 31:598–607. https://doi.org/10.1016/J.IJDEVNEU.2013.07.006
Acknowledgements
We wish to thank Prof. Suresh Kumar of Department of Statistics for their valuable advice and support in analyzing the data.
Funding
The study was carried out by the funds received by University grants commission-Basic Scientific research (UGC-BSR) to Ms Sonia Verma and DST-PURSE 2017–18, New Delhi to Department of Biophysics, Panjab University.
Author information
Authors and Affiliations
Contributions
SV has carried out all the research work presented in this article. She has analysed all the results of molecular biology and histopathological studies. She has written and edited the scientific article. Prof. BN and Dr. PR has given their valuable advice and support in carrying out this piece of work and in the preparation of this manuscript. Dr. SS has helped the author with his valuable suggestions in the research work and writing the article.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
All the protocols performed were approved by Animal Ethical Committee (IAEC) of Panjab University, Chandigarh, India with approval no. PU/45/99/CPCSEA/IAEC/2018/153. Every effort was made to minimize the number of animals and the distress caused throughout the experiment.
Informed Consent
All authors have agreed to submit the article in its current form.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Verma, S., Sharma, S., Ranawat, P. et al. Modulatory Effects of Ginkgo biloba Against Amyloid Aggregation Through Induction of Heat Shock Proteins in Aluminium Induced Neurotoxicity. Neurochem Res 45, 465–490 (2020). https://doi.org/10.1007/s11064-019-02940-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-019-02940-z