Abstract
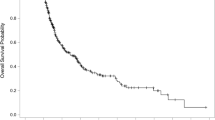
While stereotactic radiosurgery (SRS) has been shown effective in the management of brain metastases, small brain metastases (≤10 mm) can pose unique challenges. Our aim was to investigate the efficacy of SRS in the treatment of small brain metastases, as well as elucidate clinically relevant factors impacting local failure (LF). We utilized a large, single-institution cohort to perform a retrospective analysis of patients with brain metastases up to 1 cm in maximal dimension. Clinical and radiosurgical parameters were investigated for an association with LF and compared using a competing risk model to calculate cumulative incidence functions, with death and whole brain radiotherapy serving as competing risks. 1596 small brain metastases treated with SRS among 424 patients were included. Among these tumors, 33 developed LF during the follow-up period (2.4% at 12 months following SRS). Competing risk analysis demonstrated that LF was dependent on tumor size (0.7% if ≤2 mm and 3.0% if 2–10 mm at 12 months, p = 0.016). Other factors associated with increasing risk of LF were the decreasing margin dose, increasing maximal tumor diameter, volume, and radioresistant tumors (each p < 0.01). 22 tumors (0.78%) developed radiographic radiation necrosis following SRS, and this incidence did not differ by tumor size (≤2 mm and 2–10 mm, p = 0.200). This large analysis confirms that SRS remains an effective modality in treatment of small brain metastases. In light of the excellent local control and relatively low risk of toxicity, patients with small brain metastases who otherwise have a reasonable expected survival should be considered for radiosurgical management.


Similar content being viewed by others
References
National Comprehensive Cancer Network Clinical Practice Guidelines: Central Nervous System Cancers v1.2016. Available via http://www.nccn.org/professionals/physician_gls/pdf/cns.pdf. Accessed 1 Dec 2016
Kocher M, Wittig A, Piroth MD, Treuer H, Seegenschmiedt H, Ruge M, Grosu AL, Guckenberger M (2014) Stereotactic radiosurgery for treatment of brain metastases. A report of the DEGRO Working Group on Stereotactic Radiotherapy. Strahlenther Onkol 190(6):521–532. doi:10.1007/s00066-014-0648-7
Mehta MP, Tsao MN, Whelan TJ, Morris DE, Hayman JA, Flickinger JC, Mills M, Rogers CL, Souhami L (2005) The American Society for Therapeutic Radiology and Oncology (ASTRO) evidence-based review of the role of radiosurgery for brain metastases. Int J Radiat Oncol Biol Phys 63(1):37–46. doi:10.1016/j.ijrobp.2005.05.023
Andrews DW, Scott CB, Sperduto PW, Flanders AE, Gaspar LE, Schell MC, Werner-Wasik M, Demas W, Ryu J, Bahary JP, Souhami L, Rotman M, Mehta MP, Curran WJ Jr (2004) Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet 363(9422):1665–1672. doi:10.1016/s0140-6736(04)16250-8
Trifiletti DM, Sheehan JP, Grover S, Dutta S, Rusthoven CG, Kavanagh BD, Sahgal A, Showalter TN (2017) National trends in radiotherapy for brain metastases at time of diagnosis of non-small cell lung cancer (under review)
Goldberg SB, Gettinger SN, Mahajan A, Chiang AC, Herbst RS, Sznol M, Tsiouris AJ, Cohen J, Vortmeyer A, Jilaveanu L, Yu J, Hegde U, Speaker S, Madura M, Ralabate A, Rivera A, Rowen E, Gerrish H, Yao X, Chiang V, Kluger HM (2016) Pembrolizumab for patients with melanoma or non-small-cell lung cancer and untreated brain metastases: early analysis of a non-randomised, open-label, phase 2 trial. Lancet Oncol. doi:10.1016/s1470-2045(16)30053-5
Dempke WC, Edvardsen K, Lu S, Reinmuth N, Reck M, Inoue A (2015) Brain metastases in NSCLC—are TKIs changing the treatment strategy? Anticancer Res 35(11):5797–5806
Zhu Q, Sun Y, Cui Y, Ye K, Yang C, Yang D, Ma J, Liu X, Yu J, Ge H (2017) Clinical outcome of tyrosine kinase inhibitors alone or combined with radiotherapy for brain metastases from epidermal growth factor receptor (EGFR) mutant non small cell lung cancer (NSCLC). Oncotarget. doi:10.18632/oncotarget.14515
Johnson P, Yang F, Lamichhane N (2016) SU-G-TeP4-10: do small errors matter when treating pituitary adenoma patients using gamma knife? Med Phys 43(6):3687. doi:10.1118/1.4957135
Trifiletti DM, Lee CC, Kano H, Cohen J, Janopaul-Naylor J, Alonso-Basanta M, Lee JY, Simonova G, Liscak R, Wolf A, Kvint S, Grills IS, Johnson M, Liu KD, Lin CJ, Mathieu D, Heroux F, Silva D, Sharma M, Cifarelli CP, Watson CN, Hack JD, Golfinos JG, Kondziolka D, Barnett G, Lunsford LD, Sheehan JP (2016) Stereotactic radiosurgery for brainstem metastases: an International Cooperative Study to define response and toxicity. Int J Radiat Oncol Biol Phys 96(2):280–288. doi:10.1016/j.ijrobp.2016.06.009
Trifiletti DM, Patel N, Lee CC, Romano AM, Sheehan JP (2015) Stereotactic radiosurgery in the treatment of brain metastases from gastrointestinal primaries. J Neurooncol 124(3):439–446. doi:10.1007/s11060-015-1857-3
Snell JW, Sheehan J, Stroila M, Steiner L (2006) Assessment of imaging studies used with radiosurgery: a volumetric algorithm and an estimation of its error. Technical note. J Neurosurg 104(1):157–162. doi:10.3171/jns.2006.104.1.157
Gray B (2014) cmprsk: Subdistribution Analysis of Competing Risks. R package version 2.2-7. Available via https://CRAN.R-project.org/package=cmprsk. Accessed 18 Apr 2016
Scrucca L, Santucci A, Aversa F (2010) Regression modeling of competing risk using R: an in depth guide for clinicians. Bone Marrow Transplant 45(9):1388–1395. doi:10.1038/bmt.2009.359
Chang EL, Wefel JS, Hess KR, Allen PK, Lang FF, Kornguth DG, Arbuckle RB, Swint JM, Shiu AS, Maor MH, Meyers CA (2009) Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: a randomised controlled trial. Lancet Oncol 10(11):1037–1044. doi:10.1016/S1470-2045(09)70263-3
Brown PD, Jaeckle K, Ballman KV, Farace E, Cerhan JH, Anderson SK, Carrero XW, Barker FG 2nd, Deming R, Burri SH, Menard C, Chung C, Stieber VW, Pollock BE, Galanis E, Buckner JC, Asher AL (2016) Effect of radiosurgery alone versus radiosurgery with whole brain radiation therapy on cognitive function in patients with 1 to 3 brain metastases: a randomized clinical trial. JAMA 316(4):401–409. doi:10.1001/jama.2016.9839
Hoffknecht P, Tufman A, Wehler T, Pelzer T, Wiewrodt R, Schutz M, Serke M, Stohlmacher-Williams J, Marten A, Maria Huber R, Dickgreber NJ (2015) Efficacy of the irreversible ErbB family blocker afatinib in epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor (TKI)-pretreated non-small-cell lung cancer patients with brain metastases or leptomeningeal disease. J Thorac Oncol 10(1):156–163. doi:10.1097/jto.0000000000000380
Deng Y, Feng W, Wu J, Chen Z, Tang Y, Zhang H, Liang J, Xian H, Zhang S (2014) The concentration of erlotinib in the cerebrospinal fluid of patients with brain metastasis from non-small-cell lung cancer. Mol Clin Oncol 2(1):116–120. doi:10.3892/mco.2013.190
Zeng YD, Zhang L, Liao H, Liang Y, Xu F, Liu JL, Dinglin XX, Chen LK (2012) Gefitinib alone or with concomitant whole brain radiotherapy for patients with brain metastasis from non-small-cell lung cancer: a retrospective study. Asian Pac J Cancer Prev 13(3):909–914
Costa DB, Shaw AT, Ou SH, Solomon BJ, Riely GJ, Ahn MJ, Zhou C, Shreeve SM, Selaru P, Polli A, Schnell P, Wilner KD, Wiltshire R, Camidge DR, Crino L (2015) Clinical experience with Crizotinib in patients with advanced ALK-rearranged non-small-cell lung cancer and brain metastases. J Clin Oncol 33(17):1881–1888. doi:10.1200/jco.2014.59.0539
Rusthoven CG, Doebele RC (2016) Management of brain metastases in ALK-positive non-small-cell lung cancer. J Clin Oncol 34(24):2814–2819. doi:10.1200/jco.2016.67.2410
Chamberlain MC, Baik CS, Gadi VK, Bhatia S, Chow LQ (2017) Systemic therapy of brain metastases: non-small cell lung cancer, breast cancer, and melanoma. Neuro-Oncology 19(1):i1–i24. doi:10.1093/neuonc/now197
Magnuson WJ, Lester-Coll NH, Wu AJ, Yang TJ, Lockney NA, Gerber NK, Beal K, Amini A, Patil T, Kavanagh BD, Camidge DR, Braunstein SE, Boreta LC, Balasubramanian SK, Ahluwalia MS, Rana NG, Attia A, Gettinger SN, Contessa JN, Yu JB, Chiang VL (2017) Management of brain metastases in Tyrosine kinase inhibitor-naive epidermal growth factor receptor-mutant non-small-cell lung cancer: a retrospective multi-institutional analysis. J Clin Oncol. doi:10.1200/jco.2016.69.7144
Bernstein MB, Krishnan S, Hodge JW, Chang JY (2016) Immunotherapy and stereotactic ablative radiotherapy (ISABR): a curative approach? Nat Rev Clin Oncol. doi:10.1038/nrclinonc.2016.30
Okada H, Weller M, Huang R, Finocchiaro G, Gilbert MR, Wick W, Ellingson BM, Hashimoto N, Pollack IF, Brandes AA, Franceschi E, Herold-Mende C, Nayak L, Panigrahy A, Pope WB, Prins R, Sampson JH, Wen PY, Reardon DA (2015) Immunotherapy response assessment in neuro-oncology: a report of the RANO working group. Lancet Oncol 16(15):e534–e542. doi:10.1016/s1470-2045(15)00088-1
Qian JM, Mahajan A, Yu JB, Tsiouris AJ, Goldberg SB, Kluger HM, Chiang VL (2017) Comparing available criteria for measuring brain metastasis response to immunotherapy. J Neurooncol. doi:10.1007/s11060-017-2398-8
Demaria S, Golden EB, Formenti SC (2015) Role of local radiation therapy in cancer immunotherapy. JAMA Oncol 1(9):1325–1332. doi:10.1001/jamaoncol.2015.2756
Cohen-Inbar O, Shih HH, Xu Z, Schlesinger D, Sheehan JP (2017) The effect of timing of stereotactic radiosurgery treatment of melanoma brain metastases treated with ipilimumab. J Neurosurg. doi:10.3171/2016.9.jns161585
Demaria S, Ng B, Devitt ML, Babb JS, Kawashima N, Liebes L, Formenti SC (2004) Ionizing radiation inhibition of distant untreated tumors (abscopal effect) is immune mediated. Int J Radiat Oncol Biol Phys 58(3):862–870. doi:10.1016/j.ijrobp.2003.09.012
Mohammadi AM, Schroeder JL, Angelov L, Chao ST, Murphy ES, Yu JS, Neyman G, Jia X, Suh JH, Barnett GH, Vogelbaum MA (2016) Impact of the radiosurgery prescription dose on the local control of small (2 cm or smaller) brain metastases. J Neurosurg. doi:10.3171/2016.3.jns153014
Shehata MK, Young B, Reid B, Patchell RA, St Clair W, Sims J, Sanders M, Meigooni A, Mohiuddin M, Regine WF (2004) Stereotatic radiosurgery of 468 brain metastases ≤2 cm: implications for SRS dose and whole brain radiation therapy. Int J Radiat Oncol Biol Phys 59(1):87–93. doi:10.1016/j.ijrobp.2003.10.009
Wolf A, Kvint S, Chachoua A, Pavlick A, Wilson M, Donahue B, Golfinos JG, Silverman J, Kondziolka D (2017) Toward the complete control of brain metastases using surveillance screening and stereotactic radiosurgery. J Neurosurg. doi:10.3171/2016.10.jns161036
Kiess AP, Wolchok JD, Barker CA, Postow MA, Tabar V, Huse JT, Chan TA, Yamada Y, Beal K (2015) Stereotactic radiosurgery for melanoma brain metastases in patients receiving ipilimumab: safety profile and efficacy of combined treatment. Int J Radiat Oncol Biol Phys. doi:10.1016/j.ijrobp.2015.01.004
Xu Z, Schlesinger D, Toulmin S, Rich T, Sheehan J (2012) Impact of triple-negative phenotype on prognosis of patients with breast cancer brain metastases. Int J Radiat Oncol Biol Phys 84(3):612–618. doi:10.1016/j.ijrobp.2011.12.054
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no financial or other conflicts of interest.
Rights and permissions
About this article
Cite this article
Trifiletti, D.M., Hill, C., Cohen-Inbar, O. et al. Stereotactic radiosurgery for small brain metastases and implications regarding management with systemic therapy alone. J Neurooncol 134, 289–296 (2017). https://doi.org/10.1007/s11060-017-2519-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-017-2519-4