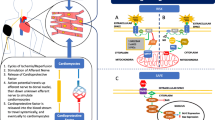
Recent studies have demonstrated that ischemic preconditioning prevents reperfusion-induced endothelial dysfunction. However, the question of the influence of preconditioning on the occurrence of the no-reflow phenomenon remains open. The receptor mechanisms of the cardioprotective and vasoprotective effects of preconditioning are different. The ability of preconditioning to prevent reperfusion-induced endothelial dysfunction is associated with activation of bradykinin B2 receptors and is independent of stimulation of adenosine receptors. The vasoprotective effect of preconditioning is mediated by mechanisms associated with activation of protein kinase C, NO synthase, and cyclooxygenase, the opening of mitochondrial KATP channels, and increases in the antioxidant defense of the heart. Delayed preconditioning also has an endothelium-protecting effect. Triggers for these effects are NO•, O2 •, and peroxynitrite, and endothelial NO synthase may be the end effector is.
Similar content being viewed by others
References
N. A. Zenkov, V. Z. Lankin, and E. B. Men’shchikova, Oxidative Stress: Biochemical and Pathophysiological Aspects [in Russian], MAIK Nauka/Interperiodika, Moscow (2001).
V. A. Kazakov, I. V. Sukhodolo,V. M. Shipulin, and O. N. Ogurkova, “The search for molecular markers of post-operative remodeling of the left ventricle in patients with ischemic cardiomyopathy,” Sib. Med. Zh. (Tomsk), 25, No. 2, 34–37 (2010).
P. F. Litvitskii, V. A. Sandrikov, and E. A. Demurov, Adaptive and Pathogenic Effects of Reperfusion and Reoxygenation of the Myocardium [in Russian], Meditsina, Moscow (1994).
L. N. Maslov, Yu. B. Lishmanov, and N. V. Solenkova, “Adaptation of the myocardium to ischemia. The first phase of ischemic preconditioning,” Usp. Fiziol. Nauk., 37, No. 3, 25–41 (2006).
L. N. Maslov, “New approaches to the prophylaxis and treatment of ischemic and reperfusion damage to the heart in acute myocardial infarction,” Sib. Med. Zh. (Tomsk), 25, No. 2, 17–24 (2010).
V. M. Shipulin, B. N. Kozlov, A. V. Evtushenko, and Yu. Yu. Vecherskii, “Contemporary strategies in the treatment of cardiac failure and heart surgery,” Sib. Med. Zh. (Tomsk), 25, No. 2, 4–12 (2010).
E. Andelova, M. Bartekova, D. Pancza, et. al., “The role of NO in ischemia/reperfusion injury in isolated rat heart,” Gen. Physiol. Biophys., 24, No. 4, 411–426 (2005).
L. Argaud, G. Rioufol. M. Lièvre, et. al., “Preconditioning during coronary angioplasty: no influence of collateral perfusion or the size of the area at risk,” Eur. Heart. J., 25, No. 22, 2019–2025 (2004).
B. Bauer, B. Z. Simkhovich, R. A. Kloner, and K. Przyklenk “Does preconditioning protect the coronary vasculature from subsequent ischemia/reperfusion injury?” Circulation, 88, No. 2, 659–672 (1993).
J. F. Bouchard, J. Chouinard, and D. Lamontagne, “Role of kinins in the endothelial protective effect of ischaemic preconditioning,” Br. J. Pharmacol., 123, No. 3, 413–420 (1998).
J. F. Bouchard, J. Chouinard, and D. Lamontagne, “Participation of prostaglandin E2 in the endothelial protective effect of ischaemic preconditioning in isolated rat heart,” Cardiovasc. Res., 45, No. 2, 418–427 (2000).
B. L. Fubkin, S. T. Shearer, J. Vinten-Johansen, et. al., “Preconditioning during simulated MIDCABG attenuates blood flow defects and neutrophil accumulation,” Ann. Thorac, Surg., 66, No. 3, 726–732 (1998).
M. J. Butler, W. Chan, A. J. Taylor, et. al., “Management of the noreflow phenomenon,” Pharmacol. Ther., 132, No. 1, 72–85 (2011).
S. Chlopicki, M. Lomnicka, and R. H. Gryglewski, “Reversal of the postischaemic suppression of coronary function in perfused guinea pig heart by ischaemic preconditioning,” J. Physiol. Pharmacol., 50, No. 4, 605–615 (1999).
J. C. Cutrn, M. G. Perrelli, B. Cavalieri, et. al., “Microvascular dysfunction induced by reperfusion injury and protective effect of ischemic preconditioning,” Free Radic. Biol. Med., 33, No. 9, 1200–1208 (2002).
I. M. Dauber, K. M. VanBenthuysen, I. F. McMurtry, et. al., “Functional coronary microvascular injury evidence as increased permeability of the brief ischemia and reperfusion,” Circ. Res., 66, No. 4, 986–998 (1990).
I. M. Dauber, E. J. Lesnefsky, K. M. VanBenthuysen, et. al., “Reactive oxygen metabolite scavengers decrease functional coronary microvascular injury due to ischemia-reperfusion,” Am. J. Physiol., 260, No. 1, H42–H49 (1991).
T. Dost, M. V. Cohen, and J. M. Downey, “Redox signalling triggers protection during the reperfusion rather than the ischemic phase of preconditioning,” Basic Res. Cardiol., 103, No. 4, 378–384 (2008).
M. Duda, E. Czarnowska, M. Kurzelewski, et. al., “Ischemic preconditioning prevents endothelial dysfunction, P-selectin expression, and neutrophil adhesion by preventing endothelial and O2 − generation in the post-ischemia guinea-pig heart,” J. Physiol. Pharmacol., 57, No. 4, 553–569 (2006).
M. Duda, A. Konior, E. Klemenska, and A. Beresewicz, “Preconditioning protects endothelium by preventing ET-1-induced activation of NADPH oxidase and xanthine oxidase in post-ischemic heart,” J. Mol. Cell. Cardiol., 42, No. 2, 400–410 (2007).
J. Feng, C. Bianchi, and F. W. Sellke, “Bradykinin preconditioning preserves coronary microvascular reactivity during cardioplegiareperfusion,” Ann. Thorac. Surg., 79, No. 3, 911–916 (2005).
S. Funaro, L. Galiuto, F. Boccalini, et. al., “Determinants of microvascular damage recovery after acute myocardial infarction: results from the acute myocardial infarction contrast imaging (AMICI) multi-centre study,” Eur. J. Echocardiogr., 12, No. 4, 306–312 (2011).
G. J. Gross, S. T. O’Rourke, L. R. Pelc, and D. C. Warltier, “Myocardial and endothelial dysfunction after multiple, brief coronary occlusions: role of oxygen radials,” Am. J. Physiol., 263, No. 6, H1703–H1709 (1992).
S. L. Hale and R. A. Kloner, “Ischemic preconditioning and myocardial hypothermia in rabbits with prolonged coronary artery occlusion,” Am. J. Physiol., 276, No. 6, H2029–H2034 (1999).
T. Hirai, M. Fujita, N. Yoshida, et. al., “Importance of ischemic preconditioning and collateral circulation for left ventricular functional recovery in patients with successful intracoronary thrombolysis for acute myocardial infarction,” Am. Heart J., 126, No. 4, 827–831 (1993).
L. D. Horwitz, D. Kaufman, M. W. Keller, and Y. Kong, “Time course of coronary endothelial healing after injury due to ischemia and reperfusion,” Circulation, 90, No. 5, 2439–2447 (1994).
N. Kaeffer, V. Richard, and C. Thuillez, “Delayed coronary endothelial protection 24 hours after preconditioning: role of free radicals,” Circulation, 96, No. 7, 2311–2316 (1997).
S. J. Kapadia, J. S. Terlato, and A. S. Most, “Presence of a critical coronary artery stenosis does not abolish the protective effect of ischemic preconditioning,” Circulation, 95, No. 5, 1286–1292 (1997).
L. J. Kaplan, C. F. Bellows, H. Blum, et. al., “Ischemic preconditioning preserves end-ischemic ATP, enhancing functional recovery and coronary flow during reperfusion,” J. Surg. Res., 57, No. 1, 179–184 (1994).
M. Kawasuji, M. Ikeda, N. Sakakibara, et. al., “Near-infrared monitoring of myocardial oxygenation during ischemic preconditioning,” Ann. Thorac. Surg., 69, No. 6, 1806–1810 (2000).
Y. D. Kim, J. S. Fomsgaard, K. F. Heim, et. al., “Brief ischemia-reperfusion induces stunning of endothelium in canine coronary artery,” Circulation, 85, No. 4, 1473–1482 (1992).
R. A. Kloner, C. E. Ganote, and R. B. Jennings, “The ‘no-reflow’ phenomenon after temporary coronary occlusion in the dog,” J. Clin. Invest., 54, No. 6, 1496–1508 (1974).
R. A. Kloner, R. E. Rude, N. Carlson, et. al., “Ultrastructural evidence of microvascular damage and myocardial cell injury after coronary artery occlusion: which comes first?” Circulation, 62, No. 5, 945–952 (1980).
R. A. Kloner and K. J. Alker, “The effect of streptokinase on intramyocardial hemorrhage, infarct size, and the no-reflow phenomenon during coronary reperfusion,” Circulation, 70, No. 3, 513–521 (1984).
M. Kurzelewski, E. Czarnowska, M. Maczewski, and A. Beresewicz, “Effect of ischemic preconditioning on endothelial dysfunction and granulocyte adhesion in isolated guinea-pig hearts subjected to ischemia-reperfusion,” J. Physiol. Pharmacol., 50, No. 4, 617–628 (1999).
K. Laude, V. Richard, J. P. Henry, et. al., “Evidence against a role of inducible nitric oxide synthase neuron the endothelial protective effects of delayed preconditioning,” Br. J. Pharmacol., 130, No. 7, 1547–1552 (2000).
K. Laude, C. Tuillez, and V. Richard, “Peroxynitrite triggers a delayed resistance of coronary endothelial cells against ischemia-reperfusion injury,” Am. J. Heart Circ. Physiol., 283, No. 4, H1418–H1423 (2002).
K. Laude, P. Beauchamp, C. Thuillez, and V. Richard, “Endothelial protective effects of preconditioning,” Cardiovasc. Res., 55, No. 3, 466–473 (2002).
K. Laude, J. Favre, C. Thuillez, and V. Richard, “NO produced by endothelial NO synthase is a mediator of delayed preconditioning-induced endothelial protection,” Am. J. Physiol. Heart Circ. Physiol., 284, No. 6, H2053–H2060 (2003).
K. E. Loke and O. L. Woodman, “Preconditioning improves myocardial functional and reflow, but not vascular reactivity, after ischaemia and reperfusion in anaesthetized dogs,” Clin. Exp. Pharmacol. Physiol., 25, No. 7–8, 552–558 (1998).
M. Maczewsk and A. Beresewicz, “The role of adenosine and ATP-sensitive potassium channels in the protection afforded by ischemic preconditioning against the post-ischemic endothelial dysfunction in guinea-pig hearts,” J. Mol. Cell. Cardiol., 30, No. 9, 1735–1747 (1998).
M. Maczewski, M. Duda, W. Pawlak, and A. Beresewicz, “Endothelial protection from reperfusion injury by ischemic preconditioning and diazoxide involves a SOD-like anti-O2 − mechanism,” Physiol. Pharmacol., 55, No. 3, 537–550 (2004).
J. L. Mehta, W. W. Nichols, W. H. Donnelly, et. al., “Impaired canine coronary vasodilator response to acetylcholine and bradykinin after occlusion -reperfusion,” Circulation, 88, No. 1, 223–234 (1993).
M. Miyamae, H. Fujiwara, M. Ikda, et. al., “Preconditioning improves energy metabolism during reperfusion but does not attenuate myocardial stunning in porcine hearts,” Circulation, 88, No. 1, 223–234 (1993).
U. M. Mortensen, B. L. Norgaard, J. E. Nielsen-Kudski, et. al., “A phase of increased ST elevation during coronary occlusion following ischemic preconditioning,” Basic Res. Cardiol., 101, No. 2, 140–148 (2006).
C. A. Murry, R. B. Jennings, and K. A. Reimer, “Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium,” Circulation, 74, No. 5, 1124–1136 (1986).
C. E. Murry, V. J. Richard, R. B. Jennings, and K. A. Reimer, “Myocardial protection is lost before contractile function recovers from ischemic preconditioning,” Am. J. Physiol., 260, No. 3, H796–H804 (1991).
B. Ostadol and F. Kolar, Cardiac Ischemia: From Injury to Protection, Kluwer Academic Press, Boston, Dordrecht, London (1999).
P. Ouyang, L. C. Becker, M. B. Effron, et. al., “Hemodynamic vascular forces contribute to impaired endothelium-dependent vasodilation in reperfused canine epicardial coronary arteries,” J. Am. Coll. Cardiol., 23, No. 5, 1216–1223 (1994).
T. Reffelmann and R. A. Kloner, “Is microvascular protection by cariporide and ischemia preconditioning causally linked to myocardial salvage?” Am. J. Physiol. Heart Circ. Physiol., 284, No. 4, H1134–H1141 (2003).
T. Reffelmann and R. A. Kloner, “The no-reflow phenomenon: A basic mechanism of myocardial ischemia and reperfusion,” Basic Res. Cardiol., 101, No. 5, 359–372 (2006).
K. A. Reimer, C. E. Murry, I. Yamasawa, et. al., “Four brief periods of myocardial ischemia cause no cumulative ATP loss or necrosis,” Am. J. Physiol., 251, No. 6, Part 2, H1306–H1315 (1986).
U. S. Ryan and R. E. Worthington, “Cell-cell contact mechanisms,” Curr. Opin. Immunol., 4, No. 1, 33–37 (1992).
T. Saito, E. Fushimi, T. Abe, et. al., “Augmented contractile response to endothelin and blunted endothelium-dependent relaxation in postischemic reperfused arteries,” Jpn. Circ. J., 56, No. 7, 657–670 (1992).
W. K. Summers and R. L. Jamison, “The no-reflow phenomenon in renal ischemia,” Lab. Invest., 25, No. 6, 635–643 (1971).
S. Takeshima, J. Vaage, and G. Valen, “Preconditioning the globally ischaemic, isolated rat heart: the impact of the preconditioning model on post-ischaemic systolic and diastolic function,” Scand. J. Clin. Lab. Invest., 57, No. 7, 637–646 (1997).
V. H. Thourani, M. Nakamura, I. G. Duarte, et. al., “Ischemic preconditioning attenuates postischemic coronary artery endothelial dysfunction in a model of minimally invasive direct coronary artery bypass grafting,” J. Thorac. Cardiovasc. Surg., 117, No. 2, 383–389 (1999).
M. Tofukuji, C. Metais, J. Li, et. al., “Effects of ischemic preconditioning on myocardial perfusion, function, and microvascular regulation,” Circulation, 98, No. 19, Supplement, II197–II204 (1998).
P. S. Tsao, N. Aoki, D. J. Lefer, et. al., “Time course of endothelial dysfunction and myocardial injury during myocardial ischemia and reperfusion in the cat,” Circulation, 82, No. 4, 1402–1412 (1990).
K. A. VanBenthuysen, I. F. McMurtry, and L. D. Horwitz, “Reperfusion after acute coronary occlusion in dogs impairs endothelium-dependent relaxation to acetylcholine and augments contractile activity in vitro,” J. Clin. Invest., 79, No. 1, 265–274 (1987).
N. Vladic, Z. D. Ge, T. Leucker, et. al., “Decreased tetrahydrobiopterin and disrupted association of Hsp90 with eNOS by hyper-glycemia impair myocardial ischemic preconditioning,” Am. J. Physiol. Heart Circ. Physiol., 301, No. 5, H2130–H2139 (2011).
X. Wu, G. S. Mintz, A. J. Lansky, et. al., “The relationship between attenuated plaque identified by intravascular ultrasound and no-reflow after stenting in acute myocardial infarction: the HORIZONS-AMI (Harmonizing Outcomes with Revascularization and Stents in Acute Myocardial Infarction) trial,” JACC Cardiovasc. Interv., 4, No. 5, 495–502 (2011).
H. Yamagishi, K. Akioka, K. Hirata, et. al., “Effects of preinfarction angina on myocardial injury in patients with acute myocardial infarction: a study with resting 123I-BMIPP and 201Tl myocardial SPECT,” J. Nucl. Med., 41, No. 5, 830–836 (2000).
D. M. Yellon and J. M. Downey, “Preconditioning the myocardium: from cellular physiological to clinical cardiology,” Physiol. Rev., 83, No. 4, 1113–1151 (2003).
J. L. Zhao, Y. J. Yang, S. J. You, et. al., “Beneficial effects of ischemic preconditioning on myocardial no-reflow in a mini-swine model of acute myocardial infarction and reperfusion,” Acta Acad. Med. Sin., 27, No. 4, 486-490 (2005).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Rossiiskii Fiziologicheskii Zhurnal imeni I. M. Sechenova, Vol. 98, No. 4, pp. 433–448, April, 2012.
Rights and permissions
About this article
Cite this article
Maslov, L.N., Lishmanov, Y.B., Oeltgen, P. et al. Effects of Preconditioning on Coronary Perfusion in Cardiac Ischemia and Reperfusion. Neurosci Behav Physi 43, 1039–1048 (2013). https://doi.org/10.1007/s11055-013-9848-3
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-013-9848-3