Abstract
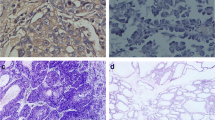
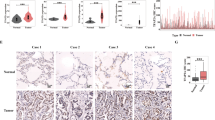
Benign metastasizing leiomyoma (BML) is a rare disease characterized by extrauterine benign leiomyomatosis in patients with a previous or concomitant history of uterine leiomyoma. Currently, there are no specific criteria to predict the metastasizing ability of the uterine leiomyoma and the risk of malignant degeneration of pulmonary BML, and these are the aims of this study. We analyzed 10 uterine (three leiomyomas, four leiomyomas that gave rise to lung BML, three healthy tissues) and 11 pulmonary tissue samples (eight lung BML, three healthy tissues). Interestingly, one of the BML lesions exceptionally evolved into a leiomyosarcoma (case 2). Uterine leiomyoma microvascular density (MVD) was higher in the patients with uterine leiomyomas that gave rise to lung BML, reaching a peak in case 2. Strong positivity for the estrogen (ER) and progesterone (PR) receptors and a low proliferation index (Ki67 < 1%) were discovered both in patients with uterine leiomyoma and in patients with BML. Interestingly, in case 2, the last dedifferentiated leiomyosarcoma showed a weaker ER and PR positivity with a higher proliferation index (Ki67:30%). Regarding the uterine miRNA-126, a trend toward a hypo-expression between uterine leiomyoma and uterine leiomyoma that gave rise to lung BML was discovered, reaching the lowest level in case 2. Considering the pulmonary samples, we observed a higher miRNA-221 and a lower miRNA-126 expression in the leiomyosarcoma. We tried to better elucidate the biological behaviour of this rare disease. The analysis of the miRNA-221 and miRNA-126 could offer new diagnostic, prognostic and therapeutic perspectives.





Similar content being viewed by others
Abbreviations
- BML:
-
Benign metastasizing leiomyoma
- BMLs:
-
Benign metastasizing leiomyomas
- miRNA:
-
MicroRNA
- miRNAs:
-
MicroRNA
- FFPE:
-
Formalin-fixed paraffin-embedded
- EGFL7:
-
Epidermal growth factor-like domain 7
- ER:
-
Estrogen receptor
- PR:
-
Progesterone receptor
- SMA:
-
Smooth muscle actin
- MVD:
-
Microvascular density
- alfa-SMA:
-
Alfa-smooth muscle actin
- MSA:
-
Muscle-specific actin
- CTR:
-
Control group
- MCF-7:
-
Michigan cancer foundation-7
- ERBB2:
-
Erb-B2 receptor tyrosine kinase 2
References
Sapmaz F, Ergin M, Katrancioglu O, Gonlugur T, Gonlugur U, Elagoz S (2008) Benign metastasizing leiomyoma. Lung 186(4):271–273. https://doi.org/10.1007/s00408-008-9084-8
Rao AV, Wilson J, Sylvester K (2008) Pulmonary benign metastasizing leiomyoma following hysterectomy: a clinicopathologic correlation. J Thorac Oncol 3(6):674–676. https://doi.org/10.1097/JTO.0b013e3181757a46
Steiner PE (1939) Metastasizing fibroleiomyoma of the uterus: report of a case and review of the literature. Am J Pathol 15(1):89
Wei WT, Chen PC (2015) Benign metastasizing leiomyoma of the lung: a case report and literature review. Oncol Lett 10(1):307–312
Xiong Y, Ying S, Yichao J, Lei X, Huihua D, Jun W, Zhihong Z, Xing C (2019) Multiple organ benign metastasizing leiomyoma: a case report and literature review. J Obstet Gynaecol Res 45(10):2132–2136. https://doi.org/10.1111/jog.14066
Dutta S, Vo T, Lo WC, Iyer A (2001) Large isolated benign metastasizing leiomyoma of the lung. Ann Thorac Surg 111(2):e147. https://doi.org/10.1016/j.athoracsur.2020.08.093
Ghanema M, Meyera F, Jechorekb D, Schoederb V, Ignatovc A, Fadeld M, Halloula Z (2019) Intravascular (post-hysterectomy) leiomyoma (IVL) as late tumor thrombus within the inferior vena cava (IVC)—a rare case primarily imposing as IVC thrombus originating from left renal vein after former left nephrectomy status. Pathol Res Pract 215(6):152359. https://doi.org/10.1016/j.prp.2019.02.009
Aoki K, Yamamoto T, Terauchi R, Mori T, Shirai T, Kitawaki J (2021) Benign metastasizing leiomyoma in femur and thigh with a history of uterine leiomyoma: a case report and literature review. J Obstet Gynaecol Res 47(2):812–817. https://doi.org/10.1111/jog.14545
Awonuga AO, Shavell VI, Imudia AN, Rotas M, Diamond MP, Puscheck EE (2010) Pathogenesis of benign metastasizing leiomyoma: a review. Obstet Gynecol Surv 65(3):189–195. https://doi.org/10.1097/OGX.0b013e3181d60f93
Rao UN, Finkelstein SD, Jones MW (1999) Comparative immunohistochemical and molecular analysis of uterine and extrauterine leiomyosarcomas. Mod Pathol 12(11):1001–1009
Patton KT, Cheng L, Papavero V et al (2006) Benign metastasizing leiomyoma: clonality, telomere length and clinicopathologic analysis. Mod Pathol 19(1):130–140
Tietze L, Günther K, Hörbe A et al (2000) Benign metastasizing leiomyoma: a cytogenetically balanced but clonal disease. Hum Pathol 31(1):126–128
Nuovo GJ, Schmittgen TD (2008) Benign metastasizing leiomyoma of the lung: clinicopathologic, immunohistochemical, and micro-RNA analyses. Diagn Mol Pathol 17(3):145–150. https://doi.org/10.1097/PDM.0b013e31815aca19
Esteban JM, Allen WM, Schaerf RH (1999) Benign metastasizing leiomyoma of the uterus: histologic and immunohistochemical characterization of primary and metastatic lesions. Arch Pathol Lab Med 123(10):960–962
Ogawa M, Hara M, Ozawa Y et al (2011) Benign metastasizing leiomyoma of the lung with malignant transformation mimicking mediastinal tumor. Clin Imaging 35(5):401–404. https://doi.org/10.1016/j.clinimag.2010.11.003
Song KS, Keum DY, Hwang IS (2017) Malignant transformation of pulmonary benign metastasizing leiomyoma. Korean J Thorac Cardiovasc Surg 50(1):59–63. https://doi.org/10.5090/kjtcs.2017.50.1.59
Ventura L, Gnetti L, Franciosi V et al (2017) Exceptional evolution of benign metastasizing leiomyomas of the lung. J Thorac Oncol 12(1):S1120–S1121. https://doi.org/10.1016/j.jtho.2016.11.1570
Findakly D, Wang J (2020) Molecular profiling of benign metastasizing leiomyoma of the uterus revealing unique novel therapeutic targets. Cureus 12(4):e7701. https://doi.org/10.7759/cureus.7701
Hernández-Plata E, Velázquez-Wong AC, Jiménez-Ramírez C, Fernández-Ramírez F, Galicia-Sánchez LM et al (2019) Identification of genomic copy number variations in lung benign metastasizing leiomyomatosis. Clin Respir J 13(2):105–113. https://doi.org/10.1111/crj.12987
Ambros V (2001) MicroRNAs: tiny regulators with great potential. Cell 107(7):823–826
Ambros V (2004) The functions of animal microRNAs. Nature 431(7006):350–355
Ciafre SA, Galardi S, Mangiola A et al (2005) Extensive modulation of a set of microRNAs in primary glioblastoma. Biochem Biophys Res Commun 334(4):1351–1358
Calin GA, Dumitru CD, Shimizu M et al (2002) Frequent deletions and down-regulation of micro-RNA genes miR15 and miR16 at 13q14 in chronic lymphocytic leukemia. Proc Natl Acad Sci USA 99(24):15524–15529. https://doi.org/10.1073/pnas.242606799
Michael MZ, O’Connor SM, Pellekaan NGV, Young GP, James RJ (2003) Reduced accumulation of specific microRNAs in colorectal neoplasia. Mol Cancer Res 1:882–891
Murakami Y, Yasuda T, Saigo K et al (2005) Comprehensive analysis of microRNA expression patterns in hepatocellular carcinoma and non-tumorous tissues. Oncogene 25(17):2537–2545. https://doi.org/10.1038/sj.onc.1209283
Takamizawa J, Konishi H, Yanagisawa K et al (2004) Reduced expression of the let-7 microRNAs in human lung cancers in association with shortened postoperative survival. Cancer Res. 64(11):3753–3756. https://doi.org/10.1158/0008-5472
Pallante P, Visone R, Ferracin M et al (2006) MicroRNA deregulation in human thyroid papillary carcinomas. Endocr Relat Cancer 13(2):497–508. https://doi.org/10.1677/erc.1.01209
Voorhoeve PM, le Sage C, Schrier M et al (2006) A genetic screen implicates miRNA-372 and miRNA-373 as oncogenes in testicular germ cell tumors. Cell 604:17–46. https://doi.org/10.1007/978-0-387-69116-92
Eder M, Scherr M (2005) MicroRNA and lung cancer. N Engl J Med 352(23):2446–2448. https://doi.org/10.1056/NEJMcibr051201
Lu J, Getz G, Miska EA et al (2005) MicroRNA expression profiles classify human cancers. Nature 435(7043):834–8348. https://doi.org/10.1038/nature03702
Zhang C, Zhang J, Zhang A et al (2010) PUMA is a novel target of miR-221/222 in human epithelial cancers. Int J Oncol 37(6):1621–1626. https://doi.org/10.3892/ijo_00000816
Pineau P, Volinia S, McJunkin K et al (2010) MiR-221 overexpression contributes to liver tumorigenesis. Proc Natl Acad Sci USA 107(1):264–269. https://doi.org/10.1073/pnas.0907904107
Zhao J-J, Lin J, Yang H et al (2008) MicroRNA-221/222 negatively regulates estrogen receptor and is associated with Tamoxifen resistance in breast cancer. J Biol Chem 283(45):31079–31086. https://doi.org/10.1074/jbc.A116.806041
Faeza E, Vinod G, Robert AS, King-Yin LA (2014) MiR-126 in human cancers: clinical roles and current perspectives. Exp Mol Pathol 96(1):98–107. https://doi.org/10.1016/j.yexmp.2013.12.004
Liu B, Peng XC, Zheng XL, Wang J, Qin YW (2009) MiR-126 restoration down-regulate VEGF and inhibit the growth of lung cancer cell lines in vitro and in vivo. Lung Cancer 66:169–175. https://doi.org/10.1016/j.lungcan.2009.01.010
Pfaffl MW, Horgan GW, Dempfle L (2002) Relative expression software tool (REST) for group-wise comparison and statistical analysis of relative expression results in real-time PCR. Nucleic Acids Res 30(9):e36. https://doi.org/10.1093/nar/30.9.e36
Jautzke G, Muller-Ruchholtz E, Thalmann U (1996) Immunohistological detection of estrogen and progesterone receptors in multiple and well differentiated leiomyomatous lung tumors in women with uterine leiomyomas so called benign metastasizing leiomyomas. Pathol Res Pract 192(3):215–223. https://doi.org/10.1016/S0344-0338(96)80224-X
Abell MR, Littler ER (1975) Benign metastasizing uterine leiomyoma. Multi Lymph Nodal Metastases Cancer 36:2206–2213. https://doi.org/10.1002/cncr.2820360938
Canzonieri V, D’Amore ES, Bartoloni G et al (1994) Leiomyomatosis with vascular invasion. A unified pathogenesis regarding leiomyoma with vascular microinvasion, benign metastasizing leiomyoma and intravenous leiomyomatosis. Virchows Arch 425(5):541–545. https://doi.org/10.1007/BF00197559
Nucci MR, Drapkin R, Cin PD et al (2007) Distinctive cytogenetic profile in benign metastasizing leiomyoma: pathogenic implications. Am J Surg Pathol 31:737–743. https://doi.org/10.1097/01.pas.0000213414.15633.4e
Madanecki P, Kapoor N, Bebok Z, Ochocka R, Collawn JF, Bartoszewski R (2013) Regulation of angiogenesis by hypoxia:the role of microRNA. Cell Mol Biol Lett 18(1):47–57. https://doi.org/10.2478/s11658-012-0037-0
Ebrahimi F, Gopalan V, Smith RA, Lam AK (2014) miR-126 in human cancers: clinical roles and current perspectives. Exp Mol Pathol 96(1):98–107. https://doi.org/10.1016/j.yexmp.2013.12.004
Alevizakos M, Kaltsas S, Syrigos KN (2013) The VEGF pathway in lung cancer. Cancer Chemother Pharmacol 72(6):1169–1181. https://doi.org/10.1007/s00280-013-2298-3
Ariazi EA, Ariazi JL, Cordera F, Jordan VC (2006) Estrogen receptors as therapeutic targets in breast cancer. Curr Top Med Chem 6(3):181–202
Zhao JJ, Lin J, Yang H et al (2008) MicroRNA-221/222 negatively regulates estrogen receptor alpha and is associated with tamoxifen resistance in breast cancer. J Biol Chem 283(45):31079–31086. https://doi.org/10.1074/jbc.A116.806041
Miller TE, Ghoshal K, Ramaswamy B et al (2008) MicroRNA-221/222 confers tamoxifen resistance in breast cancer by targeting p27Kip1. J Biol Chem 283(44):29897–29903. https://doi.org/10.1074/jbc.M804612200
Funding
No funding for this work.
Author information
Authors and Affiliations
Contributions
Conception and design: LV, LG and PM. Administrative support: MR and MC. Provision of study materials or patients: LA. Collection and assembly of data: SC and AL. Data analysis and interpretation: LV, LG, MR, PM and GG. Manuscript writing: LV, MS, GM and RM. Final approval of manuscript: MT and PC.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Ethical approval
The study design was approved by the Local Ethics Committees (Comitato Etico dell’Area Vasta Emilia Nord—Protocol Number: LEIO2018-35842).
Informed consent
Consent obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ventura, L., Gnetti, L., Rossi, M. et al. The role of miRNA-221 and miRNA-126 in patients with benign metastasizing leiomyoma of the lung: an overview with new interesting scenarios. Mol Biol Rep 48, 3485–3494 (2021). https://doi.org/10.1007/s11033-021-06322-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-021-06322-z