Abstract
Despite the increasing demand for artificial intelligence research in medicine, the functionalities of his methods in health emergency remain unclear. Therefore, the authors have conducted this systematic review and a global overview study which aims to identify, analyse, and evaluate the research available on different platforms, and its implementations in healthcare emergencies. The methodology applied for the identification and selection of the scientific studies and the different applications consist of two methods. On the one hand, the PRISMA methodology was carried out in Google Scholar, IEEE Xplore, PubMed ScienceDirect, and Scopus. On the other hand, a review of commercial applications found in the best-known commercial platforms (Android and iOS). A total of 20 studies were included in this review. Most of the included studies were of clinical decisions (n = 4, 20%) or medical services or emergency services (n = 4, 20%). Only 2 were focused on m-health (n = 2, 10%). On the other hand, 12 apps were chosen for full testing on different devices. These apps dealt with pre-hospital medical care (n = 3, 25%) or clinical decision support (n = 3, 25%). In total, half of these apps are based on machine learning based on natural language processing. Machine learning is increasingly applicable to healthcare and offers solutions to improve the efficiency and quality of healthcare. With the emergence of mobile health devices and applications that can use data and assess a patient's real-time health, machine learning is a growing trend in the healthcare industry.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Avoid common mistakes on your manuscript.
Introduction
Nowadays, people are familiar with artificial intelligence and machine learning. These terms are beginning to be present in all facets of the world, whether consciously or unconsciously, as they are linked to computer processes and automated artificial intelligence systems [1].
Artificial intelligence is a field that is composed of computer science methods and reliable datasets. The objective of artificial intelligence is to provide novel and effective methods for problem-solving. It also encompasses sub-fields of machine learning and deep learning, which are frequently mentioned in conjunction with artificial intelligence. These disciplines are comprised of AI algorithms that seek to create expert systems that make predictions or classifications based on input data. The complexity of artificial intelligence systems ranges from simple methods direction for specific tasks to abstract methods that aim to imitate human intelligence using computers.
The applications in everyday life with artificial intelligence and machine learning systems are numerous, and the implementation of these systems, and in particular their growth, is due to the increase in the availability of data that our society is experiencing [2]. These types of artificial intelligence applications take advantage of the large volume of data to extract as much information as possible from it and help to elaborate tasks that require human intelligence, currently transferred to computer systems [3, 4].
The field of artificial intelligence is a set of algorithms that simulates human intelligence embedded in machines, to make them have the same capabilities as human beings [5]. In recent years, interest in AI research has grown exponentially, leading to the development of numerous new applications in a multitude of fields [6]. Figure 1 shows how the number of articles related to this topic is growing more and more as the years go by. From less than 1% in 1998 to almost 3% in 2018 [7].
Growth of IA-related articles between 1998 and 2019 [7]
There are different fields of AI learning. Machine learning and deep learning differ from each other in the way they analyse and manipulate data and are used to train machines to mimic human intelligence and behaviour [8].
Machine learning is a critical field of artificial intelligence that includes statistical methods and algorithms to make predictions using existent data to support the learning process. On the one hand, deep learning is a subfield of machine learning. Deep learning enables the automation of feature extraction to eliminate some processes that have been typically done by human intervention and make it possible to use a high volume of information. On the other hand, these processes need to be manually implemented when using machine learning algorithms.
Machine Learning has been gaining popularity in recent years. It is based on using user-defined algorithms to detect patterns in massive data and make predictions, all autonomously [9]. The purpose of this field of AI is to perform specific tasks without having to be programmed to do so and without having to depend on a rule-based system [10]. On the other hand, deep learning uses artificial neural networks (ANNs) to carry out the ML process, mentioned above, and learn how neurons in the brain work.
The conclusion is that as you go up the level, this information becomes more complex. This learning is called deep learning because of the layered representation model and requires longer periods than ML, due to the multitude of layers of complex computations it must solve [11].
According to the definition provided by the American College of Emergency Physicians, emergency medicine is a medical focused on the diagnosis and treatment of illness or injury. It has a fundamental role to play in society by receiving patients seeking urgent medical care [12]. The practice performed by EM physicians includes the initial assessment, diagnosis, treatment, coordination of care among different physicians, and stabilisation of cases of varying degrees of acuity for any given patient [13].
The use of machine learning and deep learning can help to assess data collected over the past years and provide the information needed to improve emergency medical processes [14]. It can assist in research and medical trials based, for example, on clinical image analysis and classification tasks, thereby automating the process and helping to reduce the workload of medical staff, thus avoiding possible human fatigue that can lead to errors in the important area of healthcare.
Moreover, emergency medicine has been a major focus for study and solution development with the advent of artificial intelligence. Technological advances have brought various tools that have great potential to improve processes and will improve the operational efficiency and quality of healthcare service delivery [14].
There are several studies that support interventions based on artificial intelligence and can match or surpass the expertise of physicians. On the other hand, there are also a multitude of mobile health apps for mobile devices, which offer good options for patient progression, as well as providing patient education materials, receiving personalised guidance and support, data retrieval, and use of self-management interventions should the user need them [15].
Furthermore, this study is necessary to know the current situation in different search platforms and to find out the different utilities that these computer systems are capable of. Currently, proposed methods can perform tasks that would normally require human intelligence, oriented towards the field of medicine.
Methodology
The methodology followed was based on carrying out two different types of systematic reviews:
The first was a review of the literature in articles extracted from different open access scientific search engines for the University of Valladolid. The second review was carried out on different commercial application platforms.
Both reviews were carried out until the end of April 2021, therefore, all articles and applications published later have not been considered in the analysis of the following work.
Literature review
Before beginning to detail the characteristics of the PRISMA-ScR protocol, the articles to be selected must first be obtained, that is why we proceed to specify the search strategy used to find a series of articles. These 3 procedures of the search strategy were carried out successively in each one of the search engines. In this literature review, articles were retrieved from different academic search systems: Google Scholar, IEEE Xplore, PubMed, ScienceDirect and Scopus. The authors have selected these databases for two main points. On the one hand, they cover most of the scientific information in fields such as engineering or telemedicine. On the other hand, these databases have been used by several recent systematic reviews on health informatics [16,17,18,19,20].
In each of these databases, an advanced search is carried out by combining appropriate words and/or expressions, making use of AND and OR connectors. To carry out the research, specifically the Machine Learning analysis in the field of health, the following keywords have been mainly used in combination with each other, although there may be many more combinations, depending on the criteria of each user: (“All Metadata”: machine) AND (“All Metadata”: learning) OR (“All Metadata”: AI) AND (“All Metadata”: health*) AND (“All Metadata”: emergenc*) OR (“All Metadata”: urgenc*).
To minimise this large number of searches and to assist in the selection of suitable items, various filters are applied. The parameters set were as follows:
The date of publication of the article must be between 2011 and the present day.
The language must be English and Spanish only.
The document type criterion. Only documents that are research or systematic review articles will be retained, as they gather information from the most relevant sources.
Appendix A shows schematically the procedure used in the search strategy. The authors used the PRISMA-ScR Protocol. This protocol has 4 phases necessary to perform such a state-of-the-art study. These phases will be carried out in all search systems until the existing results are finalised [21] Fig. 10.
Identification phase: Articles were discarded if, despite including the keywords and filters, they did not go into the subject matter of this research work in depth. To carry out the first round of discarding, the articles obtained were sorted in order of relevance and the title was read. If the article does not have the expected title, it will be discarded.
Selection phase: The documents obtained in the previous phase were screened for duplicate articles. Moreover, the summary of each of the documents is consulted and discarded in case it is not potentially what is expected.
Eligibility phase: In this stage, the article is read individually and in its entirety. Insufficiently informative articles will be discarded. The opinion of the author/authors and their conclusions will be considered, as well as the number of citations the article has.
Inclusion phase: Finally, articles that have not been discarded in the previous phase will be included in this review.
The risk of bias assessment points out the transparency of the results provided by the studies included in a systematic review. Several systematic reviews on related topics available in the literature that has adopted PRISMA methodology do not include the risk of bias [22, 23]. Consequently, this study does not list the risk of bias. Nevertheless, the authors highlight this limitation.
Review of commercial mobile applications
A review of currently available mobile applications is also carried out, to which different search strategies are applied. The collection of mobile apps (mHealth) was carried out in the most popular search systems of the smartphone brands. In this case, the two main and most used app shops have been chosen: App Store used on iOS devices and Google Play used on Android devices [9].
Search terms: The first procedure is similar to the previous review. A set of keywords is chosen that fit the desired search. The set of words was as follows: “mHealth”, “eHealth”, “Machine learning and emergencies”, “Machine learning and health”, “AI and health”, “Al and medicine”, “mHealth and CoreML (for App Store search)” y “mHealth y MLKit (for Google Play search)”. To select the relevant mobile applications; several criteria have been followed:
The main categories will be "medicine" and "health and wellness". Other apps focused in other categories will be discarded.
Apps that have a cost will be discarded.
The rating must be equal to or higher than 2 stars.
The language of the applications must be English and/or Spanish.
The description of each application is read and then downloaded to test each application individually and in full. Apps with insufficient information will be discarded [15]. For applications from the Google Play platform, a Realme 7 5G with Android 10 operating system was used, for applications from the App Store platform, an iPhone 7 with iOS 14.5 operating system (latest update until April 2021) was used.
Appendix B shows the flowchart describing the above-mentioned procedure Fig.11.
Results
In total, 20 potential information articles in the literature review and 12 mobile applications in the review of commercial applications were chosen for the analysis.
Literature review
First, applying the corresponding keywords and filters, a total of 1,583 articles were retrieved through searches in the identified bibliographic databases, as shown in the following Table 1.
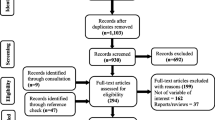
Different criteria were applied to the articles found, discarding 1,478 records whose titles did not meet expectations during the Identification phase. In this selection phase, the summary of each of the 105 documents was consulted, and 74 documents were discarded since, in the opinion of the authors, they were not potentially what was expected.
In total, 31 articles were found for content analysis during the eligibility stage and 11 of them were subsequently eliminated because the information they contained did not focus on healthcare emergencies. Finally, after eliminating several articles with the different criteria mentioned above, 20 articles are included in this systematic review.
The screening process of the included results has been done at least by two reviewers independently. This process has two main stages. On the one hand, the reviewers have read the title and abstract of each study. On the other hand, the reviewers have analysed all the manuscript content. The study is included only with the common consensus of the reviewers.
Figure 2 shows a flow diagram describing the PRISMA-ScR protocol algorithm with numbers.
Figure 3 shows the number of articles from each search engine included in this work.
The Science Direct search engine is the platform where most articles of interest have been selected, followed by IEEE Xplore. Figure 4 shows the number of articles published each year over the last 10 years.
The year 2020 is notable for having 9 articles with information of interest compared to previous years. This is mainly due to research into COVID-19, considered a global health emergency disease, whose need for detection and treatment through machine learning, among others, is of vital importance at present. The included studies are divided into 7 major groups according to the content covered in each of them, as shown in Table 2. These categories have been defined based on the included studies and under the supervision and medical background of the last author. Group 1 includes three studies that focus on methods or systems to support pre-hospital medical care and disease screening. Group 2 includes four works that focus on machine learning-based solutions for clinical decision support. Group 3 presents three research studies that focus on the current pandemic scenario of COVID-19. Group 4 (Emergency medicine) includes 3 review studies focused on health informatics solutions for medical scenarios that require immediate medical attention. Group 5 includes three works that focus on services for enhanced medical scenarios. Group 6 includes two research papers that deal with the applications of mobile computing technologies. Finally, the remaining one study has been categorized as others since cannot be included in any of the before mentioned categories.
Figure 5 represents the distribution of the selected literature concerning the group information represented in Table 2.
Analysis
Table 3 presents the title, date, authors, and main contributions addressed in these articles [14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33].
Performance in the review of commercial mobile applications
Firstly, several searches were conducted on the commercial platforms. The desired keywords were applied and a total of 3,089 applications were retrieved. On the one hand, 2084 results are available in App Store and 1005 in Google Play.
Once the results of the previous table had been obtained, various filters were applied to narrow down the results, resulting in 201 applications, of which the description was read to find the most appropriate thematic applications. A total of 168 were discarded, resulting in 33 applications, which will be subjected to a final criterion. Finally, the 21 less generic applications that did not cover the treatment and/or care of different health emergency diseases were eliminated. Applications with similar functionality to others were also removed, resulting in a total of 12 applications.
Figure 6 also shows graphically the number of applications launched in the different years.
Among the health topics most addressed in this review were clinical decisions, as was the case with the literature review, followed by apps for pre-hospital medical care. Consequently, they have been categorised into 5 groups according to the content covered in each of these apps. The following Table 4 and graph in Fig. 7 shows the categories.
On the other hand, to find out the impact of these apps among users, the ratings of each of them on the two commercial platforms have been studied. Figure 8 below shows graphically the score obtained from 0 to 5 stars.
The highest-rated app on both platforms is Tok Medicine. Followed by Nabta Health and Redivus Health for App Store users. And MDCalc and HealthTap for Google Play users. The AI and ML techniques on which each of these tools are based can also be divided into 4 different groups. The following Table 5 and Fig. 9 show the categories.
The most used technique is ML-based on natural language processing, as most apps have a virtual assistant or use an advanced search that allows the user to use tags and filter content. In this way, the system learns automatically according to the user's preferences and over time will be able to suggest recommendations or searches more in line with the user's needs.
Analysis of the obtained applications
Based on the Core ML [56] model and according to the methodology followed for the selection of each of them, in the following table are 10 apps (out of the 12 existing ones) compatible with the App Store. On the other hand, based on the Kit ML model [57] and the methodology followed for their selection, the following table shows 10 apps (out of the 12 existing ones) compatible with Google Play. The characteristics of the applications included in this systematic review are listed in Appendix C Table 6 [34,35,36,37,38,39,40,41,42,43,44,45].
Discussion
A total of 105 scientific articles from the different databases were examined to find the 20 successful research studies. In total, 35% (7/20) were mainly extracted from the Science Direct platform. These studies were further classified into 7 categories, among which 20% (4/20) for medical and/or emergency service research and another 20% (4/20) for automated systems for clinical decisions.
Secondly, during the commercial review, a total of 201 mobile applications were examined and 12 of them were finally chosen. They were classified into 5 groups, of which 25% (3/12) focus on pre-hospital medical care and another 25% (3/12) on clinical decision support. In addition, 50% (6/12) of them use ML techniques based on natural language processing, as most of the apps make use of virtual assistants or advanced searches so that the system subsequently learns from the user's needs.
Contrasting the articles found in the literature review with the applications from the commercial application review, the search for ML-based mobile applications in the literature review leads to low results compared to the commercial review. Therefore, the authors can conclude that the development of mHealth applications is more economically and commercially motivated than research-driven [58].
Mobile apps can optimise the efficiency of health system services, facilitating the work of healthcare staff, and thus reducing their costs. This model can predict emergency admissions to hospitals and help clinicians accurately monitor the risks faced by patients. Establish measures to avoid unplanned admissions that result in high medical costs [59].
Early prediction and reduction of false alarms. Patients will avoid going to the health centre as, by using ML-based mobile health apps, there will be a more informed patient, who will also follow the indications of the treatment to be followed and, therefore medical collapse can be avoided [59]. This is particularly relevant for pandemic scenarios such as COVID-19. In addition, follow-up is improved as information about these patients will be collected and recorded in the electronic medical record, thus improving the intelligent triage system, and assisting physicians in patient triage. Furthermore, mobile health can reduce the workload for medical staff, allowing them to avoid mental saturation that could lead to vital errors.
Nevertheless, several limitations are still to be solved. The lack of availability of technical means in many of the emergency services is a critical barrier. Still, progress is also needed, as more of these studies and trials need to be analysed before a clear conclusion can be drawn on the effectiveness of this machine learning model [59]. As far as the use of mobile applications is concerned, a complete introduction into society is needed based on several functional criteria, such as coordination and uniformity of all systems accessing the data. Another aspect to be highlighted would be the establishment of security criteria regarding the handling and privacy of such data.
As future work, the authors want to explore a machine learning approach to develop a decision support system to support medical emergency scenarios considering the main advantages and limitations of current systems included in this systematic review.
Conclusions
The emergence of mobile health devices and applications, which can use data and assess a patient's real-time health, lead to a growing trend in machine learning technologies applied to the healthcare industry. The technology can help healthcare experts analyse to identify cases that can lead to improved diagnosis and treatment. On the one hand, this technology will reduce diagnosis times. And speed up immediate patient care. Furthermore, treatments will be optimised and improved. It is expected that, soon, using AI and its subfields, complex algorithmic scoring systems using different variables can be used to predict diagnosis, readmission, and mortality rates. The advantages that machine learning can provide emergency health services play a critical role in improving triage classification and/or diagnosis prediction. Through ML, large-scale analysis is expected to become even more automated than it is today. In the actual pandemic context, the need to analyse data more efficiently arises, whether we are talking about data derived from virus tracking or the analysis of the medical literature that has been generated and collected throughout this review work. The use of AI and ML mechanisms will be the key to efficient global health management [60].
Abbreviations
- AI:
-
Artificial Intelligence
- ANN:
-
Artificial Neural Networks
- COVID-19:
-
Coronavirus Disease 2019
- DL :
-
Deep Learning
- EM :
-
Emergency Medicine
- ML :
-
Machine Learning
- PRISMA-ScR:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews
- WHO:
-
World Health Organization
References
Riedl, M.O.: Human‐centered artificial intelligence and machine learning. 1, (2009).
Wiens, J., Shenoy, E.S.: Machine Learning for Healthcare: On the Verge of a Major Shift in Healthcare Epidemiology. Clin. Infect. Dis. 66, 149–153 (2018). https://doi.org/10.1093/cid/cix731.
Stone, P., Brooks, R., Brynjolfsson, E., Calo, R., Etzioni, O., Hager, G., Hirschberg, J., Kalyanakrishnan, S., Kamar, E., Kraus, S., Leyton-Brown, K., Parkes, D., Press, W., Saxenian, A., Shah, J., Tambe, M., Teller, A.: Artificial Intelligence and life in 2030: the one hundred year study on artificial intelligence. Stanford University (2016).
Alelyani, S., Ibrahim, A.: Internet-of-Things in telemedicine for diabetes management. In: 2018 15th Learning and Technology Conference (L T). pp. 20–23 (2018). https://doi.org/10.1109/LT.2018.8368505.
Dick, S.: Artificial Intelligence. (2019). https://doi.org/10.1162/99608f92.92fe150c.
Hamet, P., Tremblay, J.: Artificial intelligence in medicine. Metabolism. 69, S36–S40 (2017). https://doi.org/10.1016/j.metabol.2017.01.011.
García, J.: Este es el estado actual de la inteligencia artificial a nivel mundial, según el AI Index Report 2019, https://www.xataka.com/inteligencia-artificial/este-estado-actual-inteligencia-artificial-a-nivel-mundial-ai-index-report-2019, last accessed 2021/05/05.
Bini, S.A.: Artificial Intelligence, Machine Learning, Deep Learning, and Cognitive Computing: What Do These Terms Mean and How Will They Impact Health Care? J. Arthroplasty. 33, 2358–2361 (2018). https://doi.org/10.1016/j.arth.2018.02.067.
Char, D.S., Abràmoff, M.D., Feudtner, C.: Identifying Ethical Considerations for Machine Learning Healthcare Applications. Am. J. Bioeth. 20, 7–17 (2020). https://doi.org/10.1080/15265161.2020.1819469.
Descubre los principales beneficios del Machine Learning, https://www.iberdrola.com/innovacion/machine-learning-aprendizaje-automatico, last accessed 2021/05/05.
Deep learning vs. machine learning: ¿qué diferencia hay?, https://www.ionos.es/digitalguide/online-marketing/marketing-para-motores-de-busqueda/deep-learning-vs-machine-learning/, last accessed 2021/05/05.
Sharma, M.: Remote diagnosis, monitoring and intervention for maritime industry workers: need and challenges. Int. Marit. Health. 72, 151–152 (2021). https://doi.org/10.5603/IMH.2021.0029.
Definition of Emergency Medicine, https://www.acep.org/patient-care/policy-statements/definition-of-emergency-medicine/, last accessed 2021/05/07.
Artificial Intelligence and Machine Learning in Emergency Medicine. Biocybern. Biomed. Eng. 41, 156–172 (2021). https://doi.org/10.1016/j.bbe.2020.12.002.
Martínez-Pérez, B., Torre-Díez, I. de la, López-Coronado, M., Herreros-González, J.: Mobile Apps in Cardiology: Review. JMIR MHealth UHealth. 1, e2737 (2013). https://doi.org/10.2196/mhealth.2737.
Castillo-Sánchez, G., Marques, G., Dorronzoro, E., Rivera-Romero, O., Franco-Martín, M., De la Torre-Díez, I.: Suicide Risk Assessment Using Machine Learning and Social Networks: a Scoping Review. J. Med. Syst. 44, 205 (2020). https://doi.org/10.1007/s10916-020-01669-5.
Gupta, A., Katarya, R.: Social media based surveillance systems for healthcare using machine learning: A systematic review. J. Biomed. Inform. 108, 103500 (2020). https://doi.org/10.1016/j.jbi.2020.103500.
Alonso, S.G., Marques, G., Barrachina, I., Garcia-Zapirain, B., Arambarri, J., Salvador, J.C., de la Torre Díez, I.: Telemedicine and e-Health research solutions in literature for combatting COVID-19: a systematic review. Health Technol. 11, 257–266 (2021). https://doi.org/10.1007/s12553-021-00529-7.
Sharma, S., Singh, G., Sharma, M.: A comprehensive review and analysis of supervised-learning and soft computing techniques for stress diagnosis in humans. Comput. Biol. Med. 134, 104450 (2021). https://doi.org/10.1016/j.compbiomed.2021.104450.
Kaur, P., Sharma, M.: Diagnosis of human psychological disorders using supervised learning and nature-inspired computing techniques: a meta-analysis. J. Med. Syst. 43, 204 (2019).
Tricco, A.C., Lillie, E., Zarin, W., O’Brien, K.K., Colquhoun, H., Levac, D., Moher, D., Peters, M.D.J., Horsley, T., Weeks, L., Hempel, S., Akl, E.A., Chang, C., McGowan, J., Stewart, L., Hartling, L., Aldcroft, A., Wilson, M.G., Garritty, C., Lewin, S., Godfrey, C.M., Macdonald, M.T., Langlois, E.V., Soares-Weiser, K., Moriarty, J., Clifford, T., Tunçalp, Ö., Straus, S.E.: PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 169, 467–473 (2018). https://doi.org/10.7326/M18-0850.
Cornet, V.P., Holden, R.J.: Systematic review of smartphone-based passive sensing for health and wellbeing. J. Biomed. Inform. 77, 120–132 (2018). https://doi.org/10.1016/j.jbi.2017.12.008.
Nussbaum, R., Kelly, C., Quinby, E., Mac, A., Parmanto, B., Dicianno, B.E.: Systematic Review of Mobile Health Applications in Rehabilitation. Arch. Phys. Med. Rehabil. 100, 115–127 (2019). https://doi.org/10.1016/j.apmr.2018.07.439.
Baig, M.M., Hua, N., Zhang, E., Robinson, R., Armstrong, D., Whittaker, R., Robinson, T., Mirza, F., Ullah, E.: Machine Learning-based Risk of Hospital Readmissions: Predicting Acute Readmissions within 30 Days of Discharge. In: 2019 41st Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC). pp. 2178–2181 (2019). https://doi.org/10.1109/EMBC.2019.8856646.
Kamruzzaman, M.M.: Architecture of Smart Health Care System Using Artificial Intelligence. In: 2020 IEEE International Conference on Multimedia Expo Workshops (ICMEW). pp. 1–6 (2020). https://doi.org/10.1109/ICMEW46912.2020.9106026.
Paramita, S., Bebartta, H.N.D., Pattanayak, P.: IoT Based Healthcare Monitoring System Using 5G Communication and Machine Learning Models. In: Patgiri, R., Biswas, A., and Roy, P. (eds.) Health Informatics: A Computational Perspective in Healthcare. pp. 159–182. Springer, Singapore (2021). https://doi.org/10.1007/978-981-15-9735-0_9.
Muralitharan, S., Nelson, W., Di, S., McGillion, M., Devereaux, P.J., Barr, N.G., Petch, J.: Machine Learning–Based Early Warning Systems for Clinical Deterioration: Systematic Scoping Review. J. Med. Internet Res. 23, e25187 (2021). https://doi.org/10.2196/25187.
Automatic Clinical Procedure Detection for Emergency Services | IEEE Conference Publication | IEEE Xplore, https://ieeexplore.ieee.org/document/8856281/, last accessed 2021/05/07.
Mun, S.K., Wong, K.H., Lo, S.-C.B., Li, Y., Bayarsaikhan, S.: Artificial Intelligence for the Future Radiology Diagnostic Service. Front. Mol. Biosci. 7, (2021). https://doi.org/10.3389/fmolb.2020.614258.
Schwartz, J.M., Moy, A.J., Rossetti, S.C., Elhadad, N., Cato, K.D.: Clinician involvement in research on machine learning–based predictive clinical decision support for the hospital setting: A scoping review. J. Am. Med. Inform. Assoc. 28, 653–663 (2021). https://doi.org/10.1093/jamia/ocaa296.
Federico, C., Andrea, C., Davide, F., Chiara, D.R., Daniele, C., Eleonora, S., Alessandra, C., Elena, D.V., Giuseppe, B., Massimo, L., Anna, C.: Development, evaluation, and validation of machine learning models for COVID-19 detection based on routine blood tests. medRxiv. 2020.10.02.20205070 (2020). https://doi.org/10.1101/2020.10.02.20205070.
Lalmuanawma, S., Hussain, J., Chhakchhuak, L.: Applications of machine learning and artificial intelligence for Covid-19 (SARS-CoV-2) pandemic: A review. Chaos Solitons Fractals. 139, 110059 (2020). https://doi.org/10.1016/j.chaos.2020.110059.
Waleed Salehi, A., Baglat, P., Gupta, G.: Review on machine and deep learning models for the detection and prediction of Coronavirus. Mater. Today Proc. 33, 3896–3901 (2020). https://doi.org/10.1016/j.matpr.2020.06.245.
Stewart, J., Sprivulis, P., Dwivedi, G.: Artificial intelligence and machine learning in emergency medicine. Emerg. Med. Australas. 30, 870–874 (2018). https://doi.org/10.1111/1742-6723.13145.
Garg, A., Mago, V.: Role of machine learning in medical research: A survey. Comput. Sci. Rev. 40, 100370 (2021). https://doi.org/10.1016/j.cosrev.2021.100370.
Shafaf, N., Malek, H.: Applications of Machine Learning Approaches in Emergency Medicine; a Review Article. Arch. Acad. Emerg. Med. 7, (2019).
Badgujar, S., Pillai, A.S.: Fall Detection for Elderly People using Machine Learning. In: 2020 11th International Conference on Computing, Communication and Networking Technologies (ICCCNT). pp. 1–4 (2020). https://doi.org/10.1109/ICCCNT49239.2020.9225494.
Nuntalid, N., Richards, D.: Poster: Machine Learning for Predicting Emergency Medical Incidents that Need an Air-ambulance. In: 2020 IEEE Symposium on Visual Languages and Human-Centric Computing (VL/HCC). pp. 1–2 (2020). https://doi.org/10.1109/VL/HCC50065.2020.9127266.
Classification of hospital admissions into emergency and elective care: a machine learning approach | SpringerLink, https://link.springer.com/article/10.1007%2Fs10729-017-9423-5, last accessed 2021/05/07.
Machine learning and artificial intelligence in the service of medicine: Necessity or potentiality? - ScienceDirect, https://www.sciencedirect.com/science/article/pii/S2452318620300192?via%3Dihub, last accessed 2021/05/07.
Tripti, N.F., Farhad, A., Iqbal, W., Zaman, H.U.: SaveMe: A Crime Deterrent Personal Safety Android App with a Bluetooth Connected Hardware Switch. In: 2018 9th IEEE Control and System Graduate Research Colloquium (ICSGRC). pp. 23–26 (2018). https://doi.org/10.1109/ICSGRC.2018.8657489.
Naseer Qureshi, K., Din, S., Jeon, G., Piccialli, F.: An accurate and dynamic predictive model for a smart M-Health system using machine learning. Inf. Sci. 538, 486–502 (2020). https://doi.org/10.1016/j.ins.2020.06.025.
Tack, C.: Artificial intelligence and machine learning | applications in musculoskeletal physiotherapy. Musculoskelet. Sci. Pract. 39, 164–169 (2019). https://doi.org/10.1016/j.msksp.2018.11.012.
Mediktor, https://www.mediktor.com/es, last accessed 2021/05/07.
How It Works, https://www.healthtap.com/resources/how-healthtap-works/, last accessed 2021/05/07.
Nabta App, https://nabtahealth.com/our-platform/nabta-app/, last accessed 2021/05/07.
Así es Asistencia COVID-19 la APP del Gobierno para la segunda ola, https://www.moncloa.com/2020/05/08/asistencia-covid-19-app-gobierno/, last accessed 2021/05/07.
Tidda Care, https://tidda.care/odem, last accessed 2021/05/07.
Seeing AI App from Microsoft, https://www.microsoft.com/en-us/ai/seeing-ai, last accessed 2021/05/07.
SKINAPP, https://anapix-medical.com/service/skinapp-standard/, last accessed 2021/05/07.
Helping Medical Professionals Connect, Share and Learn · Medit, https://medit.online/, last accessed 2021/05/07.
Tok Medicine. Espacios digitales para profesionales de la salud, https://tokmedicine.com/home, last accessed 2021/05/07.
MDCalc - Medical calculators, equations, scores, and guidelines, https://www.mdcalc.com/, last accessed 2021/05/07.
+WoundDesk: +WoundDesk - Mobile enhanced Wound Management for Chronic Wounds, https://wounddesk.com, last accessed 2021/05/07.
Redivus Health, https://redivus.com/, last accessed 2021/05/07.
Core ML | Apple Developer Documentation, https://developer.apple.com/documentation/coreml, last accessed 2021/05/07.
ML Kit, https://developers.google.com/ml-kit, last accessed 2021/05/07.
Martínez-Pérez, B., Torre-Díez, I. de la, López-Coronado, M.: Mobile Health Applications for the Most Prevalent Conditions by the World Health Organization: Review and Analysis. J. Med. Internet Res. 15, e2600 (2013). https://doi.org/10.2196/jmir.2600.
Elsevier: Ventajas y asignaturas pendientes de las apps en el sector salud, https://www.elsevier.com/es-es/connect/ehealth/ventajas-y-asignaturas-pendientes-de-las-apps-en-el-sector-salud, last accessed 2021/05/07.
Krittanawong, C.: The rise of artificial intelligence and the uncertain future for physicians. Eur. J. Intern. Med. 48, e13–e14 (2018). https://doi.org/10.1016/j.ejim.2017.06.017.
Acknowledgements
This research has been partially supported by European Commission and the Ministry of Industry, Energy and Tourism under the project AAL-20125036 named BWetake Care: ICTbased Solution for (Self-) Management of Daily Living.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Clinical Systems
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mendo, I.R., Marques, G., de la Torre Díez, I. et al. Machine Learning in Medical Emergencies: a Systematic Review and Analysis. J Med Syst 45, 88 (2021). https://doi.org/10.1007/s10916-021-01762-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10916-021-01762-3