Abstract
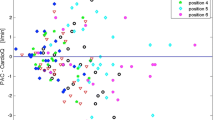
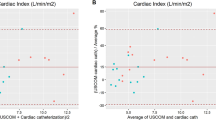
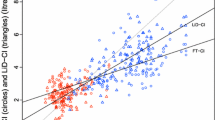
The demise of the pulmonary artery catheter as a gold standard in cardiac output measurement has created the need for new standard. Doppler cardiac output can be measured suprasternally (USCOM) and via the oesophagus (CardioQ). Use in tandem they may provide a reliable trend line of cardiac output changes against which new technologies can be assessed. Data from three similar clinical studies was pooled. Simultaneous USCOM and CardioQ readings, 13 (7–27), were performed every 15–30 min intraoperatively. Within individual patient regression analysis was performed. Data was normalized, CardioQ against USCOM, to eliminate the systematic error component following calibration. Bland–Altman and trend, concordance and polar analysis, were performed on the grouped data. Cardiac output was indexed (CI) to BSA. Data from 53 patients, aged 59 (26–81) years, scheduled for major surgery were included. Within-individual mean (SD) CI was 3.4 (0.6) L min−1 m−2. Correlation was good to excellent in 83 % of cases, R2 > 0.80, and reasonable in 96 %, R2 > 0.60. Percentage error was 38 %, and decreased to 14 % with normalization. The estimated 95 % precision for a single Doppler reading was ±10 %. Concordance rate was 96.6 % (confidence intervals 94.7–99.5 %) and above the >92 % threshold for good trending ability. Polar analysis also confirmed good trending ability. The regression line between Doppler methods was offset with a slope of 0.9, thus CardioQ CI readings increased relative to USCOM. Both Doppler methods trended cardiac output reliably. Used in tandem they provide a new standard to assess cardiac output trending.




Similar content being viewed by others
References
Vincent JL, Rhodes A, Perel A, et al. Clinical review: update on hemodynamic monitoring—a consensus of 16. Crit Care. 2011;15:229.
Critchley LA, Critchley JA. A meta-analysis of studies using bias and precision statistics to compare cardiac output measurement techniques. J Clin Monit Comput. 1999;15:85–91.
Peyton PJ, Chong SW. Minimally invasive measurement of cardiac output during surgery and critical care: a meta-analysis of accuracy and precision. Anesthesiology. 2010;113:1220–35.
Michard F. Thinking outside the (cardiac output) box. Crit Care Med. 2012;40:1361–2.
Preiss David, Fisher Joseph. A measure of confidence in Bland–Altman Analysis for the interchangeability of two methods of measurement. J Clin Monit Comput. 2008;22:257–9.
Olofsen E, Dahan A, Borsboom G, Drummond G. Improvements in the application and reporting of advanced Bland–Altman methods of comparison. J Clin Monit Comput. 2015;29(1):127–39.
Critchley LA, Lee A, Ho AM. A critical review of the ability of continuous cardiac output monitors to measure trends in cardiac output. Anesth Analg. 2010;111:1180–92.
Chong SW, Peyton PJ. A meta-analysis of the accuracy and precision of the ultrasonic cardiac output monitor (USCOM). Anaesthesia. 2012;67:1266–71.
Dark PM, Singer M. The validity of trans-esophageal Doppler ultrasonography as a measure of cardiac output in critically ill adults. Intensive Care Med. 2004;30:2060–6.
Critchley LA, Huang L, Zhang J. Continuous cardiac output monitoring: what do validation studies tell us? Curr Anesthesiol Rep. 2014;4:242–50.
Huang L, Critchley LA. An assessment of two Doppler-based monitors to track cardiac output changes in anaesthetised patients undergoing major surgery. Anaesth Intensive Care. 2014;42:631–9.
Diaper J, Ellenberger C, Villiger Y, Robert J, Inan C, Tschopp JM, Licker M. Comparison of cardiac output as assessed by transesophageal echo-Doppler and transpulmonary thermodilution in patients undergoing thoracic surgery. J Clin Anesth. 2010;22:97–103.
Coats AJS. Doppler ultrasonic measurement of cardiac output: reproducibility and validation. Eur Heart J. 1990;11(Suppl I):49–61.
Lewis JF, Kuo LC, Nelson JG, Liamcher MC, Quinones MA. Pulsed Doppler echocardiographic determination of stroke volume and cardiac output: clinical validation of two new methods using the apical window. Circulation. 1984;70:425–31.
Huang L, Critchley LA, Zhang J. Major upper abdominal surgery alters the calibration of BioReactance cardiac output readings, the NICOM, when comparisons are made against suprasternal and esophageal Doppler intraoperatively. Anesth Analg 2015; (in press).
Critchley LA. Differences between cardio-q and uscom doppler cardiac output readings in high risk surgery patients. Br J Anaesth. 2012;108(Suppl 2):113–114.
Cattermole G, Leung P, Tang C, Smith B, Graham C, Rainer T. A new method to score the quality of USCOM scans. Hong Kong J Emerg Med. 2009;16:288.
Critchley LA, Huang L. USCOM-window to the circulation: utility of supra-sternal Doppler in an elderly anaesthetized patient for a robotic cystectomy. J Clin Monit Comput. 2014;28:83–93.
Bland JM, Altman DG. Agreement between methods of measurement with multiple observations per individual. J Biopharm Stat. 2007;17:571–82.
Perrino AC Jr, O’Connor T, Luther M. Transtracheal Doppler cardiac output monitoring: comparison to thermodilution during noncardiac surgery. Anesth Analg. 1994;78:1060–6.
Axiak Flammer SM, Critchley LA, Weber A, Pirbodaghi T, Brinks H, Vandenberghe S. Reliability of lithium dilution cardiac output in anaesthetized sheep. Br J Anaesth. 2013;111:833–9.
Critchley LA, Yang XX, Lee A. Assessment of trending ability of cardiac output monitors by polar plot methodology. J Cardiothorac Vasc Anesth. 2011;25:536–46.
Critchley LA, Peng ZY, Fok BS, Lee A, Phillips RA. Testing the reliability of a new ultrasonic cardiac output monitor, the USCOM, by using aortic flowprobes in anesthetized dogs. Anesth Analg. 2005;100:748–53.
Phillips RA, Hood SG, Jacobson BM, West MJ, Wan L, May CN. Pulmonary Artery Catheter (PAC) Accuracy and Efficacy compared with flow probe and transcutaneous Doppler (USCOM): an ovine cardiac output validation. Crit Care Res Pract 2012. doi:10.1155/2012/621496.
Singer M, Clarke J, Bennett ED. Continuous hemodynamic monitoring by esophageal Doppler. Crit Care Med. 1989;17(5):447–52
Valtier B, Cholley BP, Belot JP, de la Coussaye JE, Mateo J, Payen DM. Noninvasive monitoring of cardiac output in critically ill patients using transesophageal Doppler. Am J Res Crit Care Med. 1998;158:77–83.
Huang L, Critchley LA. Study to determine the repeatability of supra-sternal Doppler (ultrasound cardiac output monitor) during general anaesthesia: effects of scan quality, flow volume, and increasing age. Br J Anaesth. 2013;111:907–15.
Huang L, Critchley LA, Lok RL, Liu Y. Correlation between supra-sternal Doppler cardiac output (USCOM) measurements and chest radiological features. Anaesthesia. 2013;68:1156–60.
O’Rourke MF, Hashimoto J Mechanical factors in arterial aging: a clinical perspective. J Am Coll Cardiol 2007; 50:1–13. Doppler. Crit Care Med 1989; 17:447–52.
Gan TJ, Soppitt A, Maroof M, et al. Goal-directed intraoperative fluid administration reduces length of hospital stay after major surgery. Anesthesiology. 2002;97:820–6.
Noblett SE, Snowden CP, Shenton BK, Horgan AF. Randomized clinical trial assessing the effect of Doppler-optimized fluid management on outcome after elective colorectal resection. Br J Surg. 2006;93:1069–76.
Marik PE. Obituary: pulmonary artery catheter 1970 to 2013. Ann Intensive Care. 2013;3:38.
Schlöglhofer T, Gilly H, Schima H. Semi-invasive measurement of cardiac output based on pulse contour: a review and analysis. Can J Anaesth. 2014;61:452–79.
Acknowledgments
This work was supported by The Chinese University of Hong Kong through two Direct Grants for Research: Study (2) 2011/12 Project Code 2041689 and study (3) 2012/13 Project Code 4054002.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
An erratum to this article can be found at http://dx.doi.org/10.1007/s10877-015-9775-7.
Rights and permissions
About this article
Cite this article
Li, H., Critchley, L.A.H. & Zhang, J. Does using two Doppler cardiac output monitors in tandem provide a reliable trend line of changes for validation studies?. J Clin Monit Comput 30, 559–567 (2016). https://doi.org/10.1007/s10877-015-9753-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-015-9753-0