Abstract
Purpose
The present study was designed to evaluate the efficacy and safety of a novel, 10% liquid formulation of intravenous immunoglobulin, stabilized with 250 mmol/L l-proline (Privigen®), in patients with primary immunodeficiency disease.
Materials and Methods
Eighty adults and children diagnosed with common variable immunodeficiency or X-linked agammaglobulinemia received intravenous Privigen® infusions (200–888 mg/kg) at 3- or 4-week intervals over a 12-month period, according to their previously established maintenance dose. The primary endpoint was the annual rate of acute serious bacterial infections.
Results
There were six episodes of acute serious bacterial infections, corresponding to an annual rate of 0.08; the annual rate for all infections was 3.55. Mean serum IgG trough levels were between 8.84 and 10.27 g/L. A total of 1,038 infusions were administered, most of them at the maximum rate permitted (8.0 mg kg−1 min−1). Temporally associated adverse events, possibly or probably related to study drug, occurred in 9% of infusions, either during or within 72 h after infusion end.
Conclusion
Privigen® is well tolerated and effective for the treatment of primary immunodeficiency.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The discovery over 50 years ago that immunoglobulin replacement therapy decreased the susceptibility to infection in patients with IgG deficiencies [1] has led to an ongoing effort to develop safer and better formulations of human IgG for the treatment of these patients. Initially, intramuscular human IgG therapy was the only commonly used treatment strategy for replacement therapy [2]. Intravenous immunoglobulin formulations (IVIG) developed in the late 1970s largely replaced intramuscular therapy and were highly effective at preventing infections [3–5]. The replacement of lyophilized IVIG products with ready-to-use liquid formulations has advanced rapidly in the recent years. Liquid IVIG utilization could save time and effort compared with lyophilized products, which require reconstitution.
Privigen® is a 10% liquid preparation of polyvalent human IgG for intravenous administration. Stabilization with l-proline at pH 4.8 is unique in that it minimizes the formation of IgG dimers and preserves IgG functional activity without refrigeration [6–8].
A multicenter, open-label clinical investigation was conducted to evaluate the safety and efficacy of this novel IVIG product in the treatment of primary immunodeficiency diseases (PID).
Materials and Methods
Product
Privigen® (also known as IgPro10, CSL Behring AG, Berne, Switzerland) is a ready-to-use 10% liquid formulation of polyvalent human IgG for intravenous administration that is stable at room temperature for its entire shelf life. In vitro studies showed that Privigen is stable at room temperature up to 36 months, with the content of dimers, aggregates, and fragments (expressed as percent of permitted specification) being, respectively, 53.7%, 8%, and 38.7% at 18 months, 54.5%, 12%, and 47.3% at 24 months, and 55.2%, 18%, and 62.3% at 36 months (data not shown). As with other IVIG preparations, Privigen® is prepared from large donor plasma pools and therefore represents the antibody spectrum present in the donor population [9]. The immunoglobulin Fc and Fab functions are retained. Analysis of six representative lots showed an IgG content of 99.2%, with more than 99.8% being monomers and dimers (typical value for dimers, which are in equilibrium with monomers, is 6%). IgA is present only in trace concentrations (8.6 ± 1.8 μg/mL). Privigen® contains no preservative and has a low sodium content (typically less than or equal to 1 mmol/L) and osmolality (320 ± 9 mOsmol/kg) in the physiological range.
Privigen® is stabilized with the naturally occurring amphiphilic amino acid l-proline (250 mmol/L = 28.8 mg/mL) at a pH of 4.8. The half-life of l-proline in human plasma is in the order of 20 min [10]. This formulation was found to be optimal in preventing IgG denaturation, degradation, or aggregation. Further, the formulation with l-proline limits the excessive in situ formation of idiotype/anti-idiotype dimers, which can precipitate adverse events (AEs), including inflammatory reactions, upon intravenous infusion [8]. It has been observed that clinical tolerance is improved by limiting IgG dimer formation [6, 11].
The IgG fraction from plasma is purified by a combination of cold ethanol fractionation, octanoic acid precipitation, and anion exchange chromatography. The manufacturing process includes two dedicated viral clearance steps (pH 4 incubation and nanofiltration) and two partitioning steps with validated viral clearance characteristics [12, 13].
Study Design
The study was designed as a phase III, open-label, single-arm investigation to evaluate the efficacy and safety of replacement therapy with Privigen® in patients with PID. The study was conducted in accordance with the International Conference on Harmonization Good Clinical Practice guidelines and the Declaration of Helsinki. Informed consent was obtained prior to the conduct of any study-related procedures. All study sites had Institutional Review Board or Independent Ethics Committee approval as required.
Patients were recruited from study sites in the USA and Europe. Men and women between 3 and 69 years of age who had either common variable immunodeficiency (CVID) or X-linked agammaglobulinemia (XLA), as defined by the Pan-American Group for Immunodeficiency and the European Society for Immunodeficiencies [14] were enrolled. Patients were required to have received regular IVIG therapy every 3 to 4 weeks for at least 6 months prior to screening and to have had at least one documented serum IgG trough level of greater than or equal to 4 g/L during this time. Exclusion criteria included previous serious adverse reaction to immunoglobulins or other blood products, selective IgA deficiency or known antibodies to IgA, hyperprolinemia, pregnancy, planning a pregnancy, or breastfeeding.
All patients were to receive a 10% liquid IVIG, Privigen®, at 3- or 4-week intervals over a 12-month period. Each patient’s dose and dosing interval were to be consistent with their prestudy treatment (planned dose of 200–800 mg/kg), which was to remain unchanged throughout the 12-month study period unless there was a medically justified need to change it. Infusions were started at an infusion rate of 0.5 mg kg−1 min−1 and gradually increased to a defined maximum rate at the investigator’s discretion. A maximum infusion rate of 4.0 mg kg−1 min−1 was permitted for the first three infusions and a rate of 8.0 mg kg−1 min−1, for subsequent infusions.
Routine premedication was not permitted. However, any patient who experienced an adverse reaction during or soon after two consecutive infusions was permitted to receive acetaminophen, antihistamines, nonsteroidal anti-inflammatory drugs, or antiemetics at subsequent infusions at the discretion of the investigator. The use of corticosteroids as premedication was not allowed. Other medications taken on a regular basis were continued.
Efficacy and Safety Assessments
The primary study endpoint was the number of acute serious bacterial infections [15] (aSBI), including pneumonia, bacteremia/septicemia, osteomyelitis/septic arthritis, bacterial meningitis, or visceral abscess. All suspected aSBIs were evaluated by a medical expert in consultation with the treating physician according to prespecified essential features for diagnosis set out in the study protocol. Secondary endpoints included the occurrence of any infection, number of days missed from work or school because of illness, number of days hospitalized, days with use of antibiotics, and personal assessment of overall well-being (rated on a five-point scale: 1 = very well, 2 = well, 3 = fair, 4 = poor, 5 = very poor). Information about infections was captured through the reporting of AEs and concomitant medications, respectively. The other secondary endpoints were evaluated via patients’ diaries, which they had to update daily. Blood samples for the determination of IgG trough levels were obtained prior to each infusion.
AEs were defined as any AEs occurring after the start of treatment, regardless of temporal relationship with the infusion, and were tracked during and between infusions. AEs were considered temporally associated with the study drug infusion if they occurred during infusion or within 72 h after the end of infusion, irrespective of any suspected relationship to the study drug. AEs were identified during the infusion by the investigator or study nurse. AE information between infusions was recorded in patient diaries and reviewed at each visit.
l-Proline serum concentrations were measured before and after the first two infusions and prior to the week 12 infusion. Routine chemistry, blood counts, urinalysis, and direct antiglobulin (Coombs’) test were analyzed at the same time points as above and additionally at the completion visit. Postinfusion samples were taken 5 to 20 min after the end of infusions 1 and 2 to evaluate the immediate effect of Privigen® on laboratory parameters. C-reactive protein was measured at various time points during the study. Tests for hepatitis B virus surface antigen (HBsAg), human immunodeficiency virus (HIV), hepatitis C virus (HCV), and B19 virus (B19) were performed before the first infusion and at the completion visit. Vital signs were assessed at screening, before, during, and shortly after each infusion, and at study completion.
Statistical Analysis
The primary efficacy endpoint was the annual rate of aSBIs in the intention-to-treat (ITT) population (all patients who received Privigen®) and in the per-protocol (PP) population (all ITT patients who completed the 12-month study period without major protocol deviations). The objective was to show that the annual rate of aSBIs per patient was less than 1 [15]. Therefore, the null hypothesis that the annual rate of aSBIs was greater or equal to 1 was tested by providing the upper one-sided 97.5% confidence limit of the estimated rate. It was assumed that the number of aSBIs was Poisson-distributed [16]. If the upper one-sided 97.5% confidence limit was less than 1, the null hypothesis was to be rejected.
Secondary efficacy and safety endpoints were analyzed in the ITT population. A major safety point was the proportion of infusions with one or more temporally associated AEs, regardless of causality, the limit for which was set to an upper one-sided 97.5% confidence interval (CI) of less than 40% [15].
Results
Patients
The study was performed at 19 sites in the USA (10), France (3), the UK (2), Germany (2), Belgium (1), and Switzerland (1). Eighty patients received treatment; 72 patients completed the study. Of the eight patients who discontinued, four withdrew consent, three discontinued because of AEs, and one died. Ten patients were excluded from the PP analyses, including the eight patients who discontinued treatment and two patients with other major protocol deviations.
Patient demographics are presented in Table I. More than half of the patients had been diagnosed at least 5 years prior to study enrollment.
Treatment
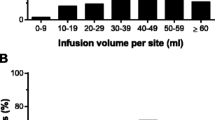
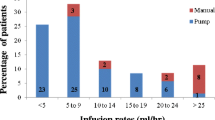
A total of 1,038 infusions were administered throughout the 12-month study, with 16 of the 80 patients (20.0%) receiving treatment according to a 3-week schedule and 64 (80.0%) according to a 4-week schedule. The entire range of individual median doses administered was 200–888 mg/kg. The majority of patients (50 patients, 62.5%) received doses between 300 and 500 mg/kg. The mean doses administered for the 3- or 4-week treatment schedule were similar (457 vs. 451 mg/kg, respectively). Starting with the fourth infusion, 86% of the infusions were given at the maximum permitted rate of 8 mg kg−1 min−1.
Premedication, predominantly diphenhydramine, ibuprofen, and paracetamol/acetaminophen, was administered to 8 (10%) of the 80 patients in the ITT population prior to 51 (4.9%) of the 1,038 infusions. Headache, nausea, and chills were the most frequently cited AEs by patients receiving premedication. Of the 29 patients who had regularly received premedication during the 6 months prior to the study, 24 (82.8%) did not require premedication while being treated with Privigen®. Five patients continued the use of premedication.
Efficacy
During the 12-month study period, there were six episodes of aSBI: three cases of pneumonia and one case each of septic arthritis, osteomyelitis, and an iatrogenic visceral abscess (following bowel perforation as a complication of surgical procedure; Table II). The annual rate of aSBI was 0.08 (upper one-sided 97.5% CI = 0.182) for the ITT population; similar results were found in the PP population (aSBI annual rate = 0.09; upper one-sided 97.5% CI = 0.195). Thus, the primary endpoint was clearly met.
Sixty-six (82.5%) patients experienced 255 episodes of any infection (including aSBIs), which resulted in an annual infection rate of 3.55 per patient. As shown in Table II, the most common infection was sinusitis. The majority of infections were classified as mild or moderate in severity; 16 (6.3%) infections experienced by ten patients were considered severe. Subgroup analyses did not reveal differences in infection rates with respect to different age groups or dose ranges.
Fifty-three (66.3%) patients missed work, school, or daycare or were unable to perform normal activities due to illness, resulting in an average annual rate of 7.94 days per patient. There were five patients who missed greater than or equal to 30 days each, which contributed substantially to the overall rate of days missed. Fifteen patients were hospitalized for a total of 166 days, corresponding to an annual rate of 2.31 days of hospitalization per patient. Of 166 reported days of hospitalization, 116 were attributed to two patients with AEs assessed as not related to the study treatment. The annual rate of antibiotics use was 87.4 days. The patients’ overall feeling of well-being score was classified as “well” on the five-point scale, with a mean of 2.1 ± 0.8 (SD).
Mean serum IgG trough levels ranged from 8.84 to10.27 g/L (Fig. 1) for all infusions. Individual levels remained stable over time and were comparable to prestudy levels.
Mean (±SD) serum IgG trough levels. Time 0 weeks indicates baseline (before the first Privigen® infusion). Mean trough serum IgG levels were approximately 9 to 10 g/L, remaining relatively constant throughout the study. The difference in IgG concentrations between the two schedules was not statistically significant (p = 0.7114)
Safety
The percentage of infusions with temporally associated AEs at least possibly related to therapy was 9%. The percentage of infusions with at least one temporally associated AE was 21%, and thus the main safety endpoint was met. Headache (35 patients, 43.8%), fatigue (13 patients, 16.3%), and nausea (ten patients, 12.5%) were the most frequently reported temporally associated AEs by patients during the 12 months of this study (Table III). The proportion of patients with temporally associated AEs was highest after the first infusion (31 of 80 patients, 38.8%), decreased with subsequent infusions, and stabilized at approximately 18% from infusion 5 on (Fig. 2). There was no dose-dependent increase in the proportion of patients with temporally associated AEs. Twenty of 25 (80.0%) patients receiving a median dose between 200 and less than or equal to 400 mg/kg, 36 of 44 (81.8%) patients receiving 400 to less than or equal to 600 mg/kg, and 8 of 11 (72.7%) patients receiving greater than or equal to 600 mg/kg experienced a temporally associated AE. The figures for the proportion of infusions with temporally associated AEs in the respective dose groups were 19.4%, 21.8%, and 19.9%.
Proportion of infusions with temporally associated AEs (72 h), by infusion. The proportion of patients reporting temporally associated adverse events within 72 h of the infusion decreased with subsequent infusions. Data from both the 3- and 4-week treatment schedules were pooled for this graph, with the number of available observations ranging from 80 (at infusion 1) to 71 (at infusion 13). Infusion 13 was the last infusion for patients on a 4-week schedule; patients on a 3-week schedule received an additional four infusions (infusions 14–17, data not shown)
Seventy-eight (97.5%) patients reported at least one AE during the 1-year study period. Headache was the most frequently reported AE, with 67.5% of patients experiencing 230 events of headache during the 26,198 study days (rate per infusion = 0.22). The majority of the 1,330 AEs were mild (60%) and not related to study treatment (84%).
Nineteen temporally associated AEs occurred during 684 infusions carried out at an infusion rate of 8 mg kg−1 min−1 (2.8% per infusion). This incidence of AEs was similar to the incidence seen in the lowest infusion rate category of less than 4 mg kg−1 min−1: 21 temporally associated AEs in 1,038 infusions or 2.0% per infusion. AEs starting during the infusion were observed in 11.8% of infusions. On just 21 occasions, the infusion rate was adjusted in response to AEs. This represents 2% of all infusions affecting 12 (15%) patients.
During the study, 16 (20%) patients experienced 38 serious AEs. Only in one patient, serious AEs were related to study drug: An 11-year old girl experienced a hypersensitivity reaction during the second infusion for which five serious AEs were reported (hypersensitivity, chills, fatigue, dizziness, and body temperature increased). The patient was withdrawn from the study. One patient was diagnosed with lymphoproliferative disorder approximately 6 months into the study and subsequently died of associated multisystem organ failure. Based on the patient’s history, the investigator determined that death was not related to the study treatment.
Laboratory Parameters
Analysis of laboratory variables also revealed no clinically relevant findings. The direct Coombs’ test changed from negative at baseline to positive in blood samples taken immediately after the first or second infusion in 33 (42.9%) of 77 patients, primarily in patients with blood group A or B. After infusion 1, 24 patients had a positive Coombs’ test; 21 of them were negative prior to infusion 2. There was no relationship between positive Coombs’ tests and the frequency of temporally associated AEs: 25 (75.0%) of the 33 patients with positive Coombs’ result after infusion 1 or 2 experienced temporally associated AEs compared to 36 (81.9%) of 44 patients whose Coombs’ test had been negative. No hemolytic events were detected in association with a positive Coombs’ test. One patient with a number of confounding medical conditions (osteomyelitis, leg amputation) experienced a clinically significant increase in C-reactive protein (48 mg/L). Thirty-eight additional patients experienced minor, transitory C-reactive protein elevation, although none exceeded the upper limit of the normal range (10 mg/L). No positive viral markers (HIV, HCV, B19, or HBsAg) were found at any of the time points tested. The mean l-proline serum concentration prior to infusion 1 was 245 μmol/L. Subsequent preinfusion concentrations had returned to this baseline level. Postinfusion serum levels of l-proline transiently increased to a range from 496 to 3,997 μmol/L (median = 1,927 μmol/L after infusion 1, 1,793 μmol/L after infusion 2).
Discussion
This study demonstrated the efficacy and safety of a novel, proline-stabilized 10% liquid IVIG preparation in patients with CVID and XLA. A survey by the Immune Deficiency Foundation indicated that patients with CVID and agammaglobulinemia together represent approximately 77% of PID patients currently receiving IVIG replacement therapy in the USA and that the 3- or 4-week dose schedule is used in 81% of patients [17]. The doses of Privigen® administered in this study were representative of those used in clinical practice.
An annual aSBI rate below 1 is recognized by the US Food and Drug Administration as indicative of efficacy for IgG substitution [18]. The study met its primary efficacy endpoint with an annual aSBI rate of 0.08. This rate is comparable to the rates recently observed with other IVIG preparations in patients with PID [19–21]. Furthermore, the annual rate of any infection (3.55, including aSBI) reported in this study is consistent with annual infection rates in other published reports [20–22].
The annual rate of days missed from school or work reported herein was 7.94 days, comparable with other studies finding 4.8–6.2 days missed per year [19, 21, 22]. This is in line with statistics reported by the Work Loss Data Institute, which shows that, on average, the typical (nonimmunocompromised) US worker had missed 8.5 days of work in the year 2000 [23]. The annual rate of 2.31 days, for patients in the ITT population, is higher than the mean number of days hospitalized per patient year reported in two recently published studies [19, 21]. This is most likely due to a disproportionate amount of time spent in the hospital by just two patients in this study.
The minimum serum concentration of IgG necessary for protection has not been established in randomized and controlled clinical studies. However, based on clinical experience, a target serum IgG trough level of at least 5 g/L has been proposed in the literature for IVIG therapy, with even further protection achieved at levels of 9 g/L and higher [24–27]. Mean serum IgG trough concentrations remained between 8.84 and 10.27 g/L over the course of this study, comparable to trough levels reported in other recent studies [19–22].
Privigen® was safe and well tolerated, with the majority of AEs assessed as mild. Headache has been the most common AE observed for other IVIG products [7, 14, 21, 22]. This was also the case in the present study. The proportion of infusions with reports of temporally associated AEs (21%) in this study compares favorably with data obtained with two other recently studied liquid IVIG preparations: 24.9% [28] and 29.1% [29]. The proportion of infusions with temporally associated AEs declined with infusion number, consistent with previous observations that first-time use of IVIG or change in IVIG preparation is associated with a higher incidence of AEs [30]. Furthermore, as the later infusions were carried out at high infusion rates, the decline in AE rate is particularly impressive.
Tolerability of IVIG products has been shown to correlate positively with the infusion rate. In the current study, the maximum infusion rate stipulated (8 mg kg−1 min−1) was higher or in the same range than the infusion rate in studies of other IVIG products [19–22]. Most patients received infusions at the maximum allowable infusion rate in our study, and yet infusions were very rarely stopped or interrupted because of AEs. Decreases in infusion rate were required only in 2% of infusions, indicating good tolerability of Privigen® even at relatively high infusion rates.
Due to its short half-life, the serum concentrations of the amino acid stabilizer l-proline returned to baseline levels prior to subsequent infusions, indicating that proline does not accumulate during treatment with Privigen®. The highest Privigen® dose administered in this study, 888 mg/kg, equals 244 mg/kg of l-proline. For comparison, the daily dose of l-proline administered repeatedly for intravenous nutrition in newborn infants amounts to 245 mg/kg l-proline.
Positive Coombs’ results were seen shortly after Privigen® infusions 1 and 2. Most of the patients with positive Coombs’ test after infusion 1 were negative before infusion 2. Transiently positive Coombs’ results may be due to the presence of anti-A and anti-B antibodies in Privigen® coating B and A red blood cells and leading to their rapid clearance between two infusions. Direct Coombs’ test changes from negative at baseline to positive were observed in 46.8% of patients, which is comparable to the rate of 37% reported for another IVIG product [22]. Transiently positive Coombs’ tests are a well-known phenomenon of IVIG treatment in general [31]. The timing of blood sampling and the analyses performed were not designed to detect and fully evaluate laboratory signs of hemolysis; no clinical signs of hemolytic anemia were observed in this study.
Conclusions
The present study met both the efficacy and the safety endpoints. It demonstrates stable IgG trough serum levels, a very low annual aSBI rate, and a low proportion of infusions with temporally associated AEs, which attest to the efficacy and safety of Privigen® treatment in patients requiring regular immunoglobulin replacement therapy. The combination of well-tolerated high infusion rates and convenience of use due to room temperature storage would be potentially advantageous for both patients and healthcare personnel.
References
Bruton OC. Agammaglobulinemia. Pediatrics 1952;9(6):722–8.
Stiehm ER, Vaerman JP, Fudenberg HH. Plasma infusions in immunologic deficiency states: metabolic and therapeutic studies. Blood 1966;28(6):918–37.
Ammann AJ, Ashman RF, Buckley RH, Hardie WR, Krantmann HJ, Nelson J, et al. Use of intravenous gamma-globulin in antibody immunodeficiency: results of a multicenter controlled trial. Clin Immunol Immunopathol. 1982;22(1):60–7. doi:10.1016/0090-1229(82)90022-8.
Cunningham-Rundles C, Siegal FP, Smithwick EM, Lion-Boule A, Cunningham-Rundles S, O’Malley J, et al. Efficacy of intravenous immunoglobulin in primary humoral immunodeficiency disease. Ann Intern Med. 1984;101(4):435–9.
Buckley RH, Schiff RI. The use of intravenous immune globulin in immunodeficiency diseases. N Engl J Med. 1991;325(2):110–7.
Bolli R, Spycher MO, Brügger R, Wüst B, Gennari K. IgG-dimer formation in liquid immunoglobulin preparations is inhibited by nicotinamide and other amphiphilic compounds. J Autoimmun. 1996;96(Suppl 1):96.
Kumar TK, Samuel D, Jayaraman G, Srimathi T, Yu C. The role of proline in the prevention of aggregation during protein folding in vitro. Biochem Mol Biol Int. 1998;46(3):509–17.
Schnorf J, Arnet B, Burek-Kozlowska A, Gennari K, Rohner R, Späth PJ, et al. Laboratory parameters measured during infusion of immunoglobulin preparations for intravenous use and related to tolerability. In: Kazatchkine MD, Morell A, editors. Intravenous immunoglobulin research and therapy. New York: Parthenon; 1996. p. 312–3.
Kazatchkine MD, Kaveri SV. Immunomodulation of autoimmune and inflammatory diseases with intravenous immune globulin. N Engl J Med. 2001;345(10):747–55. doi:10.1056/NEJMra993360.
Druml W, Heinzel G, Kleinberger G. Amino acid kinetics in patients with sepsis. Am J Clin Nutr. 2001;73(5):908–13.
Spycher MO, Bolli R, Hodler G, Gennari K, Hubsch A, Späth P, et al. Well-tolerated liquid intravenous immunoglobulin G preparations (IVIG) have a low immunoglobulin G dimer (IgG-dimer) content. J Autoimmun. 1996;96(Suppl 1):96.
Kempf C, Stucki M, Boschetti N. Pathogen inactivation and removal procedures used in the production of intravenous immunoglobulins. Biologicals 2007;35(1):35–42. doi:10.1016/j.biologicals.2006.01.002.
Stucki M, Boschetti N, Schaefer W, Hostettler T, Kaesermann F, Nowak T, et al. Investigations of prion and virus safety of a new liquid IVIG product. Biologicals 2008;36:239–47. doi:10.1016/j.biologicals.2008.01.004.
Conley ME, Notarangelo LD, Etzioni A. Diagnostic criteria for primary immunodeficiencies. Representing PAGID (Pan-American Group for Immunodeficiency) and ESID (European Society for Immunodeficiencies). Clin Immunol. 1999;93(3):190–7. doi:10.1006/clim.1999.4799.
FDA. Safety, efficacy, and pharmacokinetic studies to support marketing of immune globulin intravenous (human) as replacement therapy for primary humoral immunodeficiency. Draft guidance for Industry. 2005.
Johnson NL, Kotz S. Discrete distributions. New York: Wiley; 1969.
Treatment experiences and preferences of patients with primary immune deficiency diseases. Survey results presented at the Immune Deficiency Foundation Meeting, 20 June 2003. 2003.
Golding B. IGIV clinical endpoints. Committee Update. In Proceedings of the 65th Meeting; 16 March 2000; Silver Spring, MD. 2000.
Berger M, Pinciaro PJ. Safety, efficacy, and pharmacokinetics of Flebogamma 5% [immune globulin intravenous (human)] for replacement therapy in primary immunodeficiency diseases. J Clin Immunol. 2004;24(4):389–96. doi:10.1023/B:JOCI.0000029108.18995.61.
Church JA, Leibl H, Stein MR, Melamed IR, Rubinstein A, Schneider LC, et al. Efficacy, safety and tolerability of a new 10% liquid intravenous immune globulin [IGIV 10%] in patients with primary immunodeficiency. J Clin Immunol. 2006;26(4):388–95. doi:10.1007/s10875-006-9025-3.
Ochs HD, Pinciaro PJ. Octagam 5%, an intravenous IgG product, is efficacious and well tolerated in subjects with primary immunodeficiency diseases. J Clin Immunol. 2004;24(3):309–14. doi:10.1023/B:JOCI.0000025453.23817.3f.
Roifman CM, Schroeder H, Berger M, Sorensen R, Ballow M, Buckley RH, et al. Comparison of the efficacy of IGIV-C, 10% (caprylate/chromatography) and IGIV-SD, 10% as replacement therapy in primary immune deficiency. A randomized double-blind trial. Int Immunopharmacol. 2003;3(9):1325–33. doi:10.1016/S1567-5769(03)00134-6.
Work Loss Data Institute. Official disability guidelines. 2002;6/17(02). http://www.disabilitydurations.com/pr_repmdc.htm.
Stiehm ER. Human intravenous immunoglobulin in primary and secondary antibody deficiencies. Pediatr Infect Dis J. 1997;16(7):696–707. doi:10.1097/00006454-199707000-00012.
Roifman CM, Levison H, Gelfand EW. High-dose versus low-dose intravenous immunoglobulin in hypogammaglobulinaemia and chronic lung disease. Lancet 1987;1(8541):1075–7. doi:10.1016/S0140-6736(87)90494-6.
Ochs HD, Fischer SH, Wedgwood RJ, Wara DW, Cowan MJ, Ammann AJ, et al. Comparison of high-dose and low-dose intravenous immunoglobulin therapy in patients with primary immunodeficiency diseases. Am J Med. 1984;76(3A):78–82. doi:10.1016/0002-9343(84)90324-3.
Eijkhout HW, Der Meer JW, Kallenberg CG, Weening RS, van Dissel JT, Sanders LA, et al. The effect of two different dosages of intravenous immunoglobulin on the incidence of recurrent infections in patients with primary hypogammaglobulinemia. A randomized, double-blind, multicenter crossover trial. Ann Intern Med. 2001;135(3):165–74.
Baxter Healthcare. Gammagard liquid summary basis of approval. Baxter Healthcare; 2004.
Flebogamma 5%, Prescribing Information. Grifols, December 2003.
Brennan VM, Salome-Bentley NJ, Chapel HM. Prospective audit of adverse reactions occurring in 459 primary antibody-deficient patients receiving intravenous immunoglobulin. Clin Exp Immunol. 2003;133(2):247–51. doi:10.1046/j.1365-2249.2003.02199.x.
Pierce LR, Jain N. Risks associated with the use of intravenous immunoglobulin. Transfus Med Rev. 2003;17(4):241–51. doi:10.1016/S0887-7963(03)00038-5.
Acknowledgements
Financial support was provided by CSL Behring, King of Prussia, PA, USA. The authors wish to thank the following persons from CSL Behring AG for their support and successful completion of the study through study management, reviewing the manuscript or measuring l-proline serum concentrations: Martina Weigand, Othmar Zenker, Irmgard Andresen, Kelly Goodwin, Hanspeter Abegglen, Reinhard Bolli, and Michele Baertschi. The statistical support provided by Corinna Miede and Cordula Massion (Accovion GmbH, Germany) is gratefully appreciated. Finally, we want to thank the members of the Data Safety Monitoring Board: Prof. Dr. Louis Aledort, Mount Sinai School of Medicine, New York, USA; Prof. Dr. med. Werner Pichler, Clinic for Rheumatology and Clinical Immunology/Allergology, Inselspital, Bern, Switzerland; and Helmut Sayn, Accovion GmbH, Marburg, Germany.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
The IgPro10 in PID Study Group includes: Michael Borte, Leipzig, Germany; Joseph A. Church, Los Angeles, CA, USA; Marianne Debré, Paris, France; Mary Beth Fasano, Iowa City, IA, USA; John B. Hagan, Rochester, MN, USA; Arthur Helbling, Berne, Switzerland; Alan P. Knutsen, St Louis, MO, USA; Edouard Le Gall, Rennes, France; Isaac Melamed, Thornton, CO, USA; Robert P. Nelson, Indianapolis, IN, USA; Hans-Hartmut Peter, Freiburg, Germany; John W. Sleasman, St Petersburg, FL, USA; Mark R. Stein, North Palm Beach, FL, USA; Hassan Taki, Fort Wayne, IN, USA; Jean-Louis Touraine, Lyon, France; Christiane Vermylen, Bruxelles, Belgium; Richard L. Wasserman, Dallas, TX, USA; David Webster, London, UK; Paul Williams, Cardiff, UK.
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Stein, M.R., Nelson, R.P., Church, J.A. et al. Safety and Efficacy of Privigen®, a Novel 10% Liquid Immunoglobulin Preparation for Intravenous Use, in Patients with Primary Immunodeficiencies. J Clin Immunol 29, 137–144 (2009). https://doi.org/10.1007/s10875-008-9231-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-008-9231-2