Abstract
As the seed cells, the immune properties of the mesenchymal stem cells are important for the tissue engineering restoring effect. But the in vivo research model is lacking. In the study, based on a dialyzer pocket model, changes in immunological properties and the differentiation of seeded mesenchymal stem cells (MSCs) in collagen hydrogel were studied in muscle and articular cavity implantation, respectively. The results showed that collagen hydrogel can induce MSCs to form cartilage tissue, followed by alteration of immunological properties. In muscle implantation, relatively low expression of major histocompatibility complex (MHC) molecules and low level of one-way mixed lymphocyte reactions (MLR) on the seeded MSCs were observed, but only a little cartilage tissue formed. In articular cavity implantation, more cartilage tissue formed, but higher MHC expressions and MLR level were found. Results indicated that the immunomodulation and the cartilage formation of the seeded MSCs will be impacted by the scaffold and the environment of the in vivo implanted site. The dialyzer pocket model can be used for the in vivo research for the MSC-based strategy of the tissue engineering, especially for the optimization of the immunomodulation.
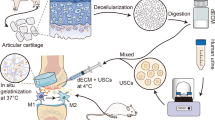
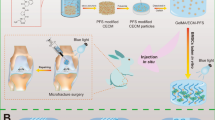
Graphical Abstract






Similar content being viewed by others
References
Steinmetz NJ, Aisenbrey EA, Westbrook KK, Qi HJ, Bryant SJ. Mechanical loading regulates human MSC differentiation in a multi-layer hydrogel for osteochondral tissue engineering. Acta Biomater. 2015;21:142–53.
Lavrentieva A, Hatlapatka T, Neumann A, Weyand B, Kasper C. Potential for osteogenic and chondrogenic differentiation of MSC. Adv Biochem Eng Biotechnol. 2012;129:73–88.
Snyder J, Rin Son A, Hamid Q, Wang C, Lui Y, Sun W. Mesenchymal stem cell printing and process regulated cell properties. Biofabrication. 2015;7:044106.
Zhao CY, Zhu XD, Yuan T, Fan HS, Zhang XD. Fabrication of biomimetic apatite coating on porous titanium and their osteointegration in femurs of dogs. Materials Science & Engineering C-Materials for Biological Applications. 2010;30:98–104.
Zheng L, Fan HS, Sun J, Chen XN, Wang G, Zhang L, Fan YJ, Zhang XD. Chondrogenic differentiation of mesenchymal stem cells induced by collagen-based hydrogel: An in vivo study. J Biomed Mater Res A. 2010;93:783–92.
Mamidi MK, Das AK, Zakaria Z, Bhonde R. Mesenchymal stromal cells for cartilage repair in osteoarthritis. Osteoarthritis Cartilage. 2016;24:1307–16.
Saulnier N, Viguier E, Perrier-Groult E, Chenu C, Pillet E, Roger T, Maddens S, Boulocher C. Intra-articular administration of xenogeneic neonatal Mesenchymal Stromal Cells early after meniscal injury down-regulates metalloproteinase gene expression in synovium and prevents cartilage degradation in a rabbit model of osteoarthritis. Osteoarthritis Cartilage. 2015;23:122–33.
Inoue S, Popp FC, Koehl GE, Piso P, Schlitt HJ, Geissler EK, Dahlke MH. Immunomodulatory effects of mesenchymal stem cells in a rat organ transplant model. Transplantation. 2006;81:1589–95.
Liu H, Kemeny DM, Heng BC, Ouyang HW, Melendez AJ, Cao T. The immunogenicity and immunomodulatory function of osteogenic cells differentiated from mesenchymal stem cells. J Immunol. 2006;176:2864–71.
DelaRosa O, Dalemans W, Lombardo E. Mesenchymal stem cells as therapeutic agents of inflammatory and autoimmune diseases. Curr Opin Biotechnol. 2012;23:978–83.
Bassi EJ, de Almeida DC, Moraes-Vieira PM, Camara NO. Exploring the role of soluble factors associated with immune regulatory properties of mesenchymal stem cells. Stem Cell Rev. 2012;8:329–42.
Klinker MW, Wei CH. Mesenchymal stem cells in the treatment of inflammatory and autoimmune diseases in experimental animal models. World J Stem Cells. 2015;7:556–67.
Doorn J, Moll G, Le Blanc K, van Blitterswijk C, de Boer J. Therapeutic applications of mesenchymal stromal cells: paracrine effects and potential improvements. Tissue Eng Part B Rev. 2012;18:101–15.
Cho KS, Kim YW, Kang MJ, Park HY, Hong SL, Roh HJ. Immunomodulatory Effect of Mesenchymal Stem Cells on T Lymphocyte and Cytokine Expression in Nasal Polyps. Otolaryngol Head Neck Surg. 2014;150:1062–70.
Kitazawa Y, Li XK, Xie L, Zhu P, Kimura H, Takahara S. Bone marrow-derived conventional, but not cloned, mesenchymal stem cells suppress lymphocyte proliferation and prevent graft-versus-host disease in rats. Cell Transplant. 2012;21:581–90.
Park MJ, Shin JS, Kim YH, Hong SH, Yang SH, Shin JY, Kim SY, Kim B, Kim JS, Park CG. Murine mesenchymal stem cells suppress T lymphocyte activation through IL-2 receptor alpha (CD25) cleavage by producing matrix metalloproteinases. Stem Cell Rev. 2011;7:381–93.
Yuan T, Li K, Guo L, Fan H, Zhang X. Modulation of immunological properties of allogeneic mesenchymal stem cells by collagen scaffolds in cartilage tissue engineering. J Biomed Mater Res A. 2011;98:332–41.
Bidarra SJ, Barrias CC, Barbosa MA, Soares R, Amedee J, Granja PL. Phenotypic and proliferative modulation of human mesenchymal stem cells via crosstalk with endothelial cells. Stem Cell Res. 2011;7:186–97.
Yuan T, Luo H, Tan J, Fan H, Zhang X. The effect of stress and tissue fluid microenvironment on allogeneic chondrocytes in vivo and the immunological properties of engineered cartilage. Biomaterials. 2011;32:6017–24.
Zheng L, Sun J, Chen X, Wang G, Jiang B, Fan H, Zhang X. In vivo cartilage engineering with collagen hydrogel and allogenous chondrocytes after diffusion chamber implantation in immunocompetent host. Tissue Eng Part A. 2009;15:2145–53.
Cairns DM, Lee PG, Uchimura T, Seufert CR, Kwon H, Zeng L. The role of muscle cells in regulating cartilage matrix production. J Orthop Res. 2010;28:529–36.
Marwood S, Bowtell JL. Effects of glutamine and hyperoxia on pulmonary oxygen uptake and muscle deoxygenation kinetics. Eur J Appl Physiol. 2007;99:149–61.
Lee RB, Wilkins RJ, Razaq S, Urban JP. The effect of mechanical stress on cartilage energy metabolism. Biorheology. 2002;39:133–43.
Fermor B, Christensen SE, Youn I, Cernanec JM, Davies CM, Weinberg JB. Oxygen, nitric oxide and articular cartilage. Eur Cell Mater. 2007;13:56–65. discussion
Gibson JS, Milner PI, White R, Fairfax TP, Wilkins RJ. Oxygen and reactive oxygen species in articular cartilage: modulators of ionic homeostasis. Pflugers Arch. 2008;455:563–73.
Ng KW, DeFrancis JG, Kugler LE, Kelly TA, Ho MM, O’Conor CJ, Ateshian GA, Hung CT. Amino acids supply in culture media is not a limiting factor in the matrix synthesis of engineered cartilage tissue. Amino Acids. 2008;35:433–8.
Hardmeier R, Redl H, Marlovits S. Effects of mechanical loading on collagen propeptides processing in cartilage repair. J Tissue Eng Regen Med. 2009;4:1–11.
Thakkar S, Ghebes CA, Ahmed M, Kelder C, van Blitterswijk CA, Saris D, Fernandes HA, Moroni L. Mesenchymal stromal cell-derived extracellular matrix influences gene expression of chondrocytes. Biofabrication. 2013;5:025003.
Tortorella D, Gewurz B, Schust D, Furman M, Ploegh H. Down-regulation of MHC class I antigen presentation by HCMV; lessons for tumor immunology. Immunol Invest. 2000;29:97–100.
Chamuleau ME, Ossenkoppele GJ, van de Loosdrecht AA. MHC class II molecules in tumour immunology: prognostic marker and target for immune modulation. Immunobiology. 2006;211:619–25.
Triantafillopoulos IK, Papagelopoulos PJ, Politi PK, Nikiforidis PA. Articular changes in experimentally induced patellar trauma. Knee Surg Sports Traumatol Arthrosc. 2002;10:144–53.
Redman SN, Dowthwaite GP, Thomson BM, Archer CW. The cellular responses of articular cartilage to sharp and blunt trauma. Osteoarthritis Cartilage. 2004;12:106–16.
Acknowledgements
This study is supported by the National Natural Science Foundation of China: 81371685 and 31100692, National key research and development programs of China: 2016YFC1103200.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Yuan, T., Luo, H., Guo, L. et al. In vivo immunological properties research on mesenchymal stem cells based engineering cartilage by a dialyzer pocket model. J Mater Sci: Mater Med 28, 150 (2017). https://doi.org/10.1007/s10856-017-5955-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-017-5955-y