Abstract
Children with chronic illness (CI) are at risk for internalizing problems, which reduce their quality of life, hamper treatment, and increase family stress. Accordingly, behavioral interventions are provided at the family level. However, the effects of parental involvement on child outcomes are not consistently beneficial. Therefore, it is relevant to study the working mechanisms. In the present study, we tested child coping and parenting stress as underlying mechanisms of the effect of an intervention for children and an additional group intervention for parents. Data were analyzed from a randomized controlled trial. Families of children with chronic illness (N = 120, child M age = 12.11 years, range 7.98–18.07) participated in a cognitive-behavioral-based group intervention and were randomized in the child-only intervention or parent–child intervention. Primary outcomes were parent- and child-reported internalizing problems, whereas the mediators were the use of child active coping skills and parenting stress. The causal model was tested with multilevel mediation analysis. Active coping skills and parenting stress stood out as significant mediators of the effect of the intervention on parent- and child-reported internalizing behavior (Cohen’s d effect size range 0.29–1.57). When parents were involved in the intervention, children increased their use of active coping skills and parents decreased in parenting stress, which in turn improved child internalizing problems. Knowing that coping skills and parenting stress underlie the benefit of involving parents can be used for optimizing interventions for children with CI and addressing the risk of internalizing problems.
Highlights
-
Parental involvement in interventions for children with chronic illness can be beneficial, however explanations are still unclear.
-
In this randomized efficacy trial, child use of active coping skills and parenting stress appeared significant temporal mediators.
-
Parental involvement supported child coping and diminished parenting stress, which in turn decreased child internalizing problems.
-
Interventions for children with internalizing problems might be optimized by focusing on determined active components.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Chronic illness (CI) affects ~25–40% of children and adolescents (Ullah and Kaelber 2021; Van Cleave et al. 2010). Due to continuous restrictions of activities, painful medical procedures, discomfort, and overall affected lifestyle, at least a quarter of these children develop behavior problems (Glazebrook et al. 2003; Merikangas et al. 2015), especially internalizing ones (Pinquart and Shen 2011). Internalizing problems in children with CI go along not only with low self-esteem (Ferro and Boyle 2015), diminished quality of life (Moreira et al. 2015), or poor adherence to treatment (Hood et al. 2006), but also with psychological burden to the family (Pinquart 2018). Indeed, elevated levels of parenting stress are common among parents of children with CI (Cousino and Hazen 2013). Given the nature of the risks for this population, there is a substantial need for effective evidence-based interventions (Bennett et al. 2015).
One intervention for psychosocial adjustment of children suffering from CI in the Netherlands is “Op Koers” (OK) (in English: “On Track”) (Last et al. 2007). It is a standardized cognitive-behavioral group therapy (CBT) specifically developed for children with any CI. During the intervention, children learn five active coping skills: information seeking, relaxation, social competence, positive thinking, and medical compliance. A randomized control trial (RCT) revealed that OK was efficacious in reducing child internalizing problems and increasing the use of information seeking, positive thinking, and social competence (Scholten et al. 2013). The effects were even more persistent at follow-up if parents followed a parallel intervention “Samen Op Koers” (SOK) (in English: “Together on Track”). This parallel intervention allowed parents to learn about the coping skills for children and the importance of parental support. The benefits of this add-on to regular OK were in line with a meta-analysis showing a significant long-term benefit of parental involvement in CBT intervention for physically healthy children with anxiety disorders (Kreuze et al. 2018). However, other studies did not find any differences in CBT efficacy with and without parental involvement (In-Albon and Schneider 2007; Silverman et al. 2008), suggesting that effects may vary according to the mechanism that such interventions attempt to influence (Lawrence et al. 2021). Therefore, understanding the processes through which the added value of parental involvement in child interventions is achieved is essential. Knowledge of underlying mechanisms may improve the efficacy of interventions for children with CI and their families. In the field of psychological interventions, the process of psychotherapeutic change is under increasing scrutiny (Hofmann and Hayes 2019). Unfortunately, studies focused on the mechanisms of change in child interventions are extremely scarce (Maric et al. 2012). In addition, the majority of the studies on mechanisms of therapeutic change lack the establishment of a timeline between changes in mediators and outcomes (MacKinnon and Fairchild 2009). Hence, results are inconclusive for causality and clinical value.
Parental involvement in CBT for children has been found beneficial in some but not all studies (Kreuze et al. 2018), suggesting variation in findings as a result of different types of parental involvement (Manassis et al. 2014). Parental involvement may have additional value to CBT for children because of three potential benefits: supporting the generalization of skills in daily life, facilitating the continued use of skills beyond the end of therapy, and addressing some parent-related obstacles to treatment success such as parenting cognitions or behaviors (Barmish and Kendall 2005; Compas et al. 2009; Hoagwood 2005). In SOK intervention, parents and children are encouraged to use active coping skills and practice them in real-world settings, especially beyond the end of the therapy. Moreover, parents are supported in their own stress management to encourage positive parenting behaviors. Therefore, parental involvement in SOK intervention may be beneficial compared to child-only intervention, because SOK impacts the use of child coping skills and the level of parenting stress in daily life.
Coping skills have been found to mediate the relation between treatment and changes in depression in adults (Bruijniks et al. 2022). Child use of coping skills in daily life was significantly improved by the intervention (Scholten et al. 2013) as defined by (1) information seeking—asking disease-related questions and informing others about the disease, (2) positive thinking—being able to change negative thoughts into positive ones, and (3) social competence—being open to family and peers about the activities that can or cannot be performed and suggesting appropriate alternatives (Last et al. 2007). Research suggests that the use of active coping skills leads to a better adaptation to the CI (Compas et al. 2012). For instance, the engagement in positive thinking predicted a decrease in depressive symptoms in adolescents with diabetes (Jaser et al. 2017). Because the SOK intervention taught parents to encourage their children to use coping skills in daily life, which is expected to decrease internalizing problems, we expected the increase in active coping skills to mediate the effect of the parent–child intervention compared to child-only intervention on child outcomes.
Parenting stress may also be a candidate as an active component of SOK. Parenting stress is defined as elevated distress linked to the role of being a parent (Abidin 1990). This stress is divided into a child domain, which represents stress related to child behavior and feelings, and a parent domain, which represents stress associated with perceived competence and functionality of parenting (Abidin 1990). SOK may modify the level of parenting stress, especially, parent domain via (1) increased knowledge about the illness and its management, increasing perceived control (Cousino and Hazen 2013), (2) shared experience with other caregivers, resulting in increased perceived social support (Yeh 2003), and (3) encouragement of responding more sensitive and supportive to the child, thereby improving the relationship (Keen et al. 2010). Indeed, a review showed that interventions focused on providing information about children’s illness, emotional support, and improvement of parent–child relationship significantly decreased parenting stress (Golfenshtein et al. 2016). Moreover, the change in parenting stress was found to result in lower internalizing problems in children with CI (Sint Nicolaas 2018). Hence, decreases in the parent domain of parenting stress may mediate the effect of SOK intervention on child internalizing problems compared to OK intervention.
The aim of the present study was to determine whether active coping skills and stress in the parent-domain mediated the effect of the parent–child intervention on child internalizing problems over child-only intervention. The measurement of internalizing problems in children with CI has been discussed in the literature. In general, children with CI appear to report fewer internalizing problems compared to their parents (Pinquart and Shen 2011), but parents may overestimate internalizing problems in their children when they are distressed (Pinquart 2018). Therefore, both parent-reported and self-reported internalizing problem scores were used as outcomes in the current study. Children with CI were randomized to three conditions: child-only intervention (OK), parent–child intervention (SOK), and a waitlist control (Scholten et al. 2013). The present study focused on the first two conditions. The primary outcomes were child- and parent-reported internalizing problems, whereas the mediators were active coping skills (information seeking, positive thinking, and social competence) and parenting stress (parent domain). It was hypothesized that the effect of SOK intervention on child internalizing problems would be mediated by increases in active coping skills and decreases in parenting stress as compared to OK. Expanding this knowledge would not only allow for optimization of the efficacy of interventions for children with CI, but could also set a basis for further development of therapies for other populations and settings.
Methods
Participants and Recruitment
Participants were recruited from outpatient clinics of three academic hospitals, four non-academic hospitals, and two primary schools for children with CI in the Netherlands. Children and parents received an information letter and participation form from their pediatrician. Main inclusion criteria focused on the following: (1) diagnosis of a CI (van der Lee et al. 2007), and (2) age between 8 and 18 years old. Considering the exclusion criteria, the main focus was on the following: (1) severe learning difficulties, and (2) inability to fill out questionnaires independently due to insufficient knowledge of the Dutch language.
A total of 120 participants were included in the study. The age of children ranged from 7.98 to 18.07 years (M = 12.11 years, SD = 2.73, 63% children (7–12 years old), 37% adolescents (≥13 years old)); 47% were girls and 53% were boys. The majority of the children and their primary caregivers (83% mothers, 15% fathers, 2% other) were born in the Netherlands (n = 89; 74%), had a medium to high income (≥€30,500 per year, n = 87; 73%), and lived in a two-parent household (n = 96; 80%). Children were under medical treatment for 45 different illnesses. The three most common ones were: type 1 diabetes (n = 34; 28%), auto-immune diseases (n = 16; 13%), and kidney disease (n = 16; 13%). Based on the Child Behavior Checklist (CBCL; see instruments), 46% of parents and 11% of children reported internalizing baseline problems within the subclinical or clinical range.
Randomization and Procedure
A multicenter randomized controlled trial was designed in line with the Consolidated Standards of Reporting Trials statement (Schulz et al. 2010). This study was approved by the Medical Ethics Committees of the Academic Medical Centre Amsterdam and of the participating hospitals. Additional details of the inclusion criteria, procedures, randomization, and flow-chart were reported by Scholten et al. (2013). Individual participants were randomized per center into three conditions: (1) child only (n = 71), (2) parent–child (n = 49), and (3) waitlist control (n = 74). Randomization was performed per center at three time points (blocks) during the study period. At each timepoint, individuals were randomized across two or three conditions. This resulted in 26 therapy groups (15 child-only and 11 parent–child), divided across 9 centers. In two out of nine centers, the parent–child condition was not organized because of a shortage of therapists needed to organize parallel parent and child groups.
Out of 1134 children and parents who received an information letter, 218 families applied for participation. Twenty-four families were excluded. Informed consent forms were signed by both parents and children of 194 families. For the current study, families in the waitlist condition were excluded resulting in 120 families. Data were collected at baseline, 6-month, and 12-month follow-up. All data were collected online.
Interventions and Therapists
Children in both intervention conditions received the same course of 6 weekly 90 min sessions with the booster session after 6 months. Every therapy group consisted from four to eight participants (M = 5.04, SD = 0.89). Five coping strategies were taught: (1) seeking and giving information about the illness, (2) using relaxation techniques during stressful situations, (3) increasing knowledge of medical compliance, (4) improving social competence, and (5) thinking positively. Due to the differences in the cognitive development and age-related topics, two slightly different versions of the protocol were developed: (1) primary school children (8–12 years old), and (2) secondary school adolescents (12–18 years old) (Last et al. 2007). While the child version mostly focused on drawing, games, relaxation exercises, and role-playing, the adolescent version also included modification of negative thoughts, story-telling, and discussions on being different from other children (Last et al. 2007).
The parent component consisted of 6 weekly 90 min sessions parallel to the child’s sessions. During the intervention, parents were encouraged to be sensitive to children’s needs and to support the use of learned coping skills. Three main goals were highlighted: (1) learning—understanding what skills children learn, (2) observing—being sensitive to children’s thoughts and feelings, and (3) motivating—encouraging children to apply learned coping skills (Scholten et al. 2013). Intervention mainly involved group discussions with other parents, psychoeducation, and homework (e.g., talking with children about their feelings). Previous publications on the efficacy of “Op Koers” report additional details on the interventions (Last et al. 2007; Scholten et al. 2013).
Two qualified psychologists per therapy group carried out the course following a detailed manual. All psychologists (n = 35) were extensively trained in the protocol. Treatment sessions took place in the hospital or school where children were recruited.
Instruments
Child behavior checklist youth self report (CBCL-YSR)
To measure child-reported internalizing problems, the Dutch version of the CBCL-YSR (Verhulst et al. 1997) was used. It is a 119-item 3-point Likert measure indicating behavior problems during the last 6 months. The internalizing factor includes anxious/depressed, withdrawn, and somatic complaints subscales, whereas externalizing factor includes rule-breaking behavior and aggressive behavior subscales. The higher the score, the more behavior problems are indicated. In the present study, the internalizing scale (20 items; raw scores) was used. It yielded good internal consistency with Cronbach’s alpha of 0.88 and 0.90 for 6- and 12-month follow-up, respectively. Items from the somatic complaints subscale were not included, as suggested by Perrin, Stein and Drotar (1991) for children with CI.
Child behavior checklist parent report form (CBCL-PRF)
To determine parent-reported internalizing problems, the Dutch version of the CBCL-PRF (Verhulst et al. 1996) was used. It is a 119-item 3-point Likert measure assessing behavior problems during the last 6 months. The scale has the same internalizing factor with corresponding subscales as the YSR. Raw scores were used; higher scores indicate more behavior problems reported by parents. The internalizing scale (21 items) showed good internal consistency with Cronbach’s alpha of 0.87 for 6- and 12-month follow-up. Items from the somatic complaints subscale were not included.
Questionnaire Op Koers for children (QOK-c)
To assess the use of coping skills in daily life, children reported their active coping skills on the Dutch QOK-c (Last et al. 2007). It is a 28-item 4-point Likert measure focused on five coping skills: positive thinking, relaxation, social competence, information seeking, and medical compliance. For the current study, three subscales were used with acceptable internal consistency at baseline and 6-month follow-up (positive thinking: 3 items, α = 0.53 and α = 0.78; e.g., “When I think about my disease, I think everything will work out fine”; social competence: 6 items, α = 0.73 and α = 0.71; e.g., “I talk with friends about my disease”; and information seeking: 5 items, α = 0.67 and α = 72; e.g., “When I have questions about my disease, I ask my doctor”). Items were averaged per skill resulting in three variables. The higher the score, the more use of active coping skills is identified.
Parenting stress index short form (PSI-SF)
To determine parent-reported parenting stress, the Dutch version of PSI-SF (De Brock et al. 1992) was used. It is a 25-item 6-point Likert measure indicating parents’ perception of the stress regarding the parenting of children. The measure focuses on two subscales: child domain (14 items) and parent domain (11 items). While the child domain represents stress related to child behavior and feelings, the parent domain represents the stress associated with the perceived competence of parenting. In the present study, only the parent domain of parenting stress was used. Higher scores indicate the presence of more parenting stress. In the present study, scores of the parent domain showed good internal consistency with Cronbach’s alpha of α = 0.88 for both baseline and 6-months follow-up.
Data-analyses
The longitudinal design of this study, together with the nested data structure of measurements within participants in therapy groups and centers, required multilevel analysis. To indicate dependency, intraclass correlations were calculated separately for each dependent variable (Snijders and Bosker 1999). Levels were rejected from further analyses if intraclass correlations were smaller than 0.05.
Data were interpreted using intention-to-treat (ITT) principles. To account for temporality (Gaynor 2017), data on coping skills and parenting stress were used from baseline and 6-month follow-up, while data on child internalizing problems were used from 6-month and 12-month follow-up. To increase robustness against deviation from normality, all data were bootstrapped. Indirect effects were tested with the multilevel mediation (MLmed) computational macro in IBM SPSS 24 (Hayes and Rockwood 2020). This model is based on growth curve analyses with random intercepts, and models change in mediators and outcomes based on a covariance structure. In this model, the dependent variable is modeled as the change from 6-month to 12-month follow-up. The model assesses the link between predictor and mediators (path a), mediators and change in outcome (path b), predictor and change in outcome (path c), and predictor and change in outcome via mediators (path c’). The MLmed macro relies upon the SPSS MIXED procedure with a maximum likelihood estimation which is advised for handling missing data in longitudinal trials (Hayes and Rockwood 2020).
Eight models (1 × 4 × 2) were built with intervention (SOK vs. OK) as a predictor, four mediators (three active coping skills and parenting stress), and child- and parent-reported internalizing problems as outcomes. For all the hypotheses, analyses were separately performed for each mediator and for child- and parent-reported internalizing behavior. In all models, time was included as a moderator between predictor and mediator to test effects on change in child internalizing problems over time (slopes). To control for baseline differences, all models included random intercepts.
Mediation effects were interpreted when the standardized indirect effect was significant (Hayes and Rockwood 2020). The 95% confidence intervals (CI) provided basis for evaluating the statistical significance of the indirect effect. Effect sizes were calculated as based on t value and degrees of freedom (df). On the basis of a power β = 0.80 and a longitudinal multilevel design with two conditions, a mean intraclass correlation of 0.62, and a sample size of 120, effect sizes should be moderate to large to detect with an alpha of 0.05 (Pan et al. 2018).
Results
Preliminary Analyses
The flow chart and pre-treatment characteristics of the total sample were reported by Scholten et al. (2013). Despite randomization, significant differences were found between conditions in age and type of center (academic vs. non-academic) (p < 0.05). The parent–child intervention condition was more frequently assigned to older children and provided in the three academic hospitals (p < 0.05) compared to the child-only condition, but no other baseline differences were found for illness severity, gender, ethnicity, income, or single-parent household. Also, no significant baseline differences were found for coping, parenting stress, and internalizing problems. Intraclass correlations indicated no dependency at the level of therapy group or center (ICC < 0.05). Testing age and type of center as covariates in the growth models, both variables were also related to change in child- but not parent-reported internalizing problems (p < 0.05) and were, therefore, included as covariates in the mediation models on child-reported outcomes. In addition, no significant differences were found between groups of primary school children and secondary school adolescents on the change in internalizing problems.
Observed mean scores and standard deviations for all the outcomes and mediators in the ITT sample of child-only and parent–child conditions are presented in Table 1. The efficacy study (Scholten et al. 2013) showed a stronger decrease in child internalizing problems (Cohen’s d = 0.24), and stronger increases in child information seeking (d = 0.30) and social competence (d = 0.31) in the parent–child intervention as compared to the child-only condition. Illness severity and illness type did not moderate the effects.
Indirect Effects
Active coping skills as mediators
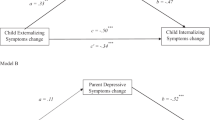
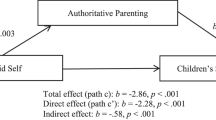
As shown in Fig. 1, significant indirect effects were found for social competence and information seeking for both child- (Z = 2.90, 95% CI [1.08, 5.12]; Z = 2.27, 95% CI [0.45, 3.61], respectively) and parent-reported (Z = 2.55, 95% CI [0.50, 2.79]; Z = 2.20, 95% CI [0.29, 2.41]) internalizing problems. Children in the parent–child condition showed significant increases in social competence (95% CI [0.13, 0.56], d = 0.46) and information seeking (95% CI [0.09, 0.54], d = 0.29) as compared to child-only condition, which in turn resulted in stronger decreases in child- (95% CI [−10.79, −6.37], d = 1.57, 95% CI [−8.57, −3.14], d = 0.90, respectively) and parent-reported (95% CI [−6.23, −2.44], d = 0.77, 95% CI [−5.80, −1.88], d = 0.58) internalizing problems. No significant indirect effects were found of positive thinking on child- or parent-reported internalizing problems (95% CI included zero).
Parenting stress as a mediator
As presented in Fig. 1, a significant indirect effect was found for parenting stress for child- (Z = 1.85, 95% CI [0.11, 2.65]) and parent-reported internalizing problems (Z = 2.09, 95% CI [0.18, 2.83]). Parents in the parent–child condition showed a significantly stronger decrease in parenting stress (95% CI [−7.40, −0.47], d = 0.32) as compared to child-only condition, which in turn resulted in stronger decreases in child- (95% CI [0.13, 0.47], d = 0.69) and parent-reported internalizing problems (95% CI [0.25, 0.48], d = 1.23).
Illness severity, illness type, and center
The models on child-reported internalizing problems were additionally tested including illness severity, illness type, and center (academic vs. non-academic) as covariates. The indirect effects remained significant (95% CI did not include zero).
Discussion
The present study showed that the effect of a parallel parent intervention on child internalizing behavior was mediated by active coping skills and parenting stress, consistent with the study hypothesis. Specifically, SOK resulted in higher increases in the use of child information seeking and social competence as well as a greater decrease in parenting stress during the intervention, which resulted in a higher reduction in child internalizing problems 6–12 months later. Therefore, active coping skills and parenting stress were likely to be part of the underlying mechanisms and explained the added value of the parent–child intervention over the child-only intervention.
Social competence and information seeking stood out as significant mediators of the effect of the intervention on both child- and parent-reported internalizing problems. This was expected as not only children but also parents increased their knowledge about active coping skills and practiced these during the homework assignments. Additional parental involvement in the intervention might have resulted in greater utilization of skills at home, leading to a stronger effect on child internalizing behavior (Compas et al. 2009; Scholten et al. 2013). Surprisingly, positive thinking did not mediate the effect of the intervention. This could be explained by positive thinking being a more internal skill, which is harder to change in such a brief intervention (Malouff and Schutte 2017). This might especially be the case in children with CI, because of the persistence of illness and corresponding limitations in daily life (Snyder et al. 2000). As it could be more challenging to intervene in child positive thinking, parents might have been less likely to practice it with children at home, resulting in a smaller effect on child internalizing behavior.
As expected, parenting stress significantly mediated the effect of SOK on both child- and parent-reported internalizing problems. This is in line with the idea that parent interventions support caregivers in parenting a child with chronic illness (Scholten et al. 2013). Parental involvement in the intervention might have increased confidence in their own parenting as a result of increased knowledge about child’s illness, emotional support among the parents, and improvement of the parent–child relationship (Golfenshtein et al. 2016). Moreover, parents experiencing less parenting stress could be less worried about their own problems and, thus, could be more sensitive as well as responsive to the needs of their child. Consequently, increased availability of the parents could make children more open about their problems to the parents resulting in less internalizing behavior over time (Sint Nicolaas 2018).
The focus on the active components of SOK has expanded the scarce mechanism of change literature in child psychotherapy. Moreover, the comparison between the parent–child intervention and child-only intervention has broadened the knowledge of the added value of parental involvement in interventions for children with CI. The longitudinal design allowed for temporality between the mediators and outcomes, which provided a more accurate interpretation of causality and stronger clinical value. Lastly, we have focused on the high quality of research, emphasizing competent therapists, adequate allocation concealment, ITT principles, multiple imputation, and sufficient sample size.
Regarding limitations, the main one was the lack of objective measures. According to research, children suffering from CI are more prone to underrate their behavior problems, possibly due to suppression of feelings (Jurbergs et al. 2008) or the need to appear as healthy individuals (Huberty et al. 2000). In contrast, parents of children with CI tend to exaggerate child behavior problems, especially internalizing, perhaps due to the influence of their own mental health (Abate et al. 2018; Pinquart and Shen 2011). Moreover, child-reported coping skills represented the subjective perception of the use of the skills by children rather than the actual estimate of the skills used. Therefore, better assessment measures should be developed such as observations of coping in real-life situations. Also, it is essential to note that although the indirect effects were in the expected directions, the effect sizes were small to medium. This may imply that the additional effect of parent involvement parallel to child therapy is small, and that there are also other relevant processes that may explain the beneficial effect of parental involvement, but were challenging to measure. Finally, because some of the randomized therapy groups eventually were not conducted, selection bias may have led to confounding, which was controlled by examining covariates.
More research is also needed on other candidate components of parent–child intervention which were not examined in the current study. For instance, the common components (Wampold 2015) such as therapeutic relationship and the alliance between group members may increase when both parent and child are involved in the intervention (Karver et al. 2006). Moreover, further studies may focus on examining whether parents participating in intervention encourage their children to practice active coping skills in real-world setting, especially beyond the end of the therapy (Barnish & Kendall, 2005).
The present study provided the first evidence of active coping skills and parenting stress being the underlying mechanisms of the parent–child intervention for children with CI. Although replication and extension are necessary, for instance, by increasing the measurement resolution and the length of follow-up, our findings suggest important clinical implications. In the field of child CI, parent–child intervention could be prioritized as a more beneficial treatment option compared to child-only intervention, especially, when the parent–child intervention is focused on increasing child coping skills and reducing parenting stress. Existing interventions for children with CI should also be optimized by explicitly focusing on determined active components. Therefore, the effect of SOK should be increased by a more explicit targeting of parenting stress to act as a buffer to child internalizing problems, which is a goal of an ongoing RCT by Douma and colleagues (2018). Lastly, our findings may set the basis for further development of interventions for other populations of parents with children experiencing high internalizing problems such as children with physical (Brossard-Racine et al. 2012) or developmental disabilities (Graefen et al., 2015).
References
Abate, C., Lippé, S., Bertout, L., Drouin, S., Krajinovic, M., Rondeau, É., & Sultan, S. (2018). Could we use parent report as a valid proxy of child report on anxiety, depression, and distress? A systematic investigation of father–mother–child triads in children successfully treated for leukemia. Pediatric Blood & Cancer, 65(2), e26840.
Abidin, R. R. (1990). Parenting Stress Index (PSI). Charlottesville, VA: Paediatric Psychology Press.
Barmish, A. J., & Kendall, P. C. (2005). Should parents be co-clients in cognitive-behavioral therapy for anxious youth? Journal of Clinical Child and Adolescent Psychology, 34, 569–581.
Bennett, S., Shafran, R., Coughtrey, A., Walker, S., & Heyman, I. (2015). Psychological interventions for mental health disorders in children with chronic physical illness: A systematic review. Archives of Disease in Childhood, 100, 308–316.
De Brock, A. J. L. L., Vermulst, A. A., Gerris, J. R. M., & Abidin, R. R. (1992). NOSI. Nijmeegse ouderlijke stress index. Handleiding experimentele versie. Lisse: Swets & Zeitlinger.
Brossard-Racine, M., Hall, N., Majnemer, A., Shevell, M. I., Law, M., Poulin, C., & Rosenbaum, P. (2012). Behavioral problems in school age children with cerebral palsy. European Journal of Pediatric Neurology, 16(1), 35–41.
Bruijniks, S. J., Meeter, M., Lemmens, L. H., Peeters, F., Cuijpers, P., & Huibers, M. J. (2022). Temporal and specific pathways of change in cognitive behavioral therapy (CBT) and interpersonal psychotherapy (IPT) for depression. Behaviour Research and Therapy, 151, 104010.
Compas, B. E., Forehand, R., Keller, G., Champion, J. E., Rakow, A., & Reeslund, K. L. (2009). Randomized controlled trial of a family cognitive-behavioral preventive intervention for children of depressed parents. Journal of Consulting and Clinical Psychology, 77(6), 1–26.
Compas, B. E., Jaser, S. S., Dunn, M. J., & Rodriguez, E. M. (2012). Coping with chronic illness in childhood and adolescence. Annual Review of Clinical Psychology, 8, 455–480.
Cousino, M. K., & Hazen, R. A. (2013). Parenting stress among caregivers of children with chronic illness: A systematic review. Journal of Pediatric Psychology, 38(8), 809–828.
Douma, M., Scholten, L., Maurice-Stam, H., & Grootenhuis, M. A. (2018). Online cognitive-behavioral based group interventions for adolescents with chronic illness and parents: Study protocol of two multicenter randomized controlled trials. BMC Pediatrics, 18(1), 235.
Ferro, M. A., & Boyle, M. H. (2015). The impact of chronic physical illness, maternal depressive symptoms, family functioning, and self-esteem on symptoms of anxiety and depression in children. Journal of Abnormal Child Psychology, 43(1), 177–187.
Gaynor, S. T. (2017). Temporal precedence in the identification of mediators of change: A brief comment on “Mediators of Change in the Child/Adolescent Multimodal Treatment Study” (Kendall et al., 2016). Journal of Consulting and Clinical Psychology, 85(1), 77–79.
Glazebrook, C., Hollis, C., Heussler, H., Goodman, R., & Coates, L. (2003). Detecting emotional and behavioral problems in pediatric clinics. Child: Care, Health and Development, 29(2), 141–149.
Golfenshtein, N., Srulovici, E., & Deatrick, A. (2016). Interventions for reducing parenting stress in families with pediatric conditions: An integrative review. Journal of Family Nursing, 22(4), 460–492.
Graefen, J., Kohn, J., Wyschkon, A., & Esser, G. (2015). Internalizing problems in children and adolescents with math disability. Zeitschrift für Psychologie, 223(2), 93–101. https://doi.org/10.1027/2151-2604/a000207.
Hayes, A. F., & Rockwood, N. J. (2020). Conditional process analysis: Concepts, computation, and advances in the modeling of the contingencies of mechanisms. American Behavioral Scientist, 64(1), 19–54. https://doi.org/10.1177/0002764219859633.
Hoagwood, K. E. (2005). Family-based services in children’s mental health: A research review and synthesis. Journal of Child Psychology and Psychiatry, 46(7), 690–713.
Hofmann, S. G., & Hayes, S. C. (2019). The future of intervention science: process-based therapy. Clinical Psychological Science, 7(1), 37–50.
Hood, K. K., Huestis, S., Maher, A., Butler, D., Volkening, L., & Laffel, L. M. B. (2006). Depressive symptoms in children and adolescents with type 1 diabetes. Diabetes Care, 29(6), 1389–1391.
Huberty, T. J., Austin, J. K., Harezlak, J., Dunn, D. W., & Ambrosius, W. T. (2000). Informant agreement in behavior ratings for children with epilepsy. Epilepsy and Behavior, 1, 427–435.
In-Albon, T., & Schneider, S. (2007). Psychotherapy of childhood anxiety disorders: a meta-analysis. Psychotherapy and Psychosomatics, 76, 15–24.
Jaser, S. S., Patel, N., Xu, M., Tamborlane, W. V., & Grey, M. (2017). Stress and coping predict adjustment and glycemic control in adolescents with type 1 diabetes. Annals of Behavioral Medicine, 51(1), 30–38.
Jurbergs, N., Russell, G. B., Long, A., & Phipps, S. (2008). Adaptive style and differences in parent and child report of health‐related quality of life in children with cancer. Psycho‐oncology, 17(1), 83–90.
Karver, M. S., Handelsman, J. B., Fields, S., & Bickman, L. (2006). Meta-analysis of therapeutic relationship variables in youth and family therapy: The evidence for different relationship variables in the child and adolescent treatment outcome literature. Clinical Psychology Review, 26(1), 50–65.
Keen, D., Couzens, D., Muspratt, S., & Rodger, S. (2010). The effects of a parent-focused intervention for children with a recent diagnosis of autism spectrum disorder on a parenting stress and competence. Research in Autism Spectrum Disorders, 4, 229–241.
Kreuze, L. J., Pijnenborg, G. H. M., de Jonge, Y. B., & Nauta, M. H. (2018). Cognitive-behavior therapy for children and adolescents with anxiety disorders: A meta-analysis of secondary outcomes. Journal of Anxiety Disorders, 60, 43–57.
Last, B. F., Stam, H., Nieuwenhuizen, A. M. O., & Grootenhuis, M. A. (2007). Positive effects of a psycho-educational group intervention for children with chronic disease: First results. Patient Education and Counseling, 65(1), 101–112.
Lawrence, P. J., Parkinson, M., Jasper, B., Creswell, C., & Halligan, S. L. (2021). Supporting the parents of children and young people with anxiety and depressive disorders is an opportunity not to be missed: a scoping review. The Lancet Psychiatry, 8(10), 909–918.
MacKinnon, D. P., & Fairchild, A. J. (2009). Current directions in mediation analysis. Current Directions in Psychological Science, 18(1), 16–20.
Malouff, J. M., & Schutte, N. S. (2017). Can psychological interventions increase optimism? A meta-analysis. The Journal of Positive Psychology, 12(6), 594–604.
Manassis, K., Lee, T. C., Bennett, K., Zhao, X. Y., Mendlowitz, S., & Wood, J. J. (2014). Types of parental involvement in CBT with anxious youth: A preliminary meta-analysis. Journal of Consulting and Clinical Psychology, 82(6), 1163–1172.
Maric, M., Wiers, R. W., & Prins, P. J. M. (2012). Ten ways to improve the use of statistical mediation analysis in the practice of child and adolescent treatment research. Clinical Child and Family Psychology Review, 15(3), 177–191.
Merikangas, K. R., Calkins, M. E., Burstein, M., He, J. P., Chiavacci, R., Lateef, T., & Gur, R. E. (2015). Comorbidity of physical and mental disorders in the neurodevelopmental genomics cohort study. Pediatrics, 135(4), 927–938.
Moreira, J. M., Soares, C. M. B. M., Teixeira, A. L., Selva, A. C. S., & Kummer, A. M. (2015). Anxiety, depression, resilience and quality of life in children and adolescents with pre-dialysis chronic kidney disease. Pediatric Nephrology, 30(12), 2153–2162.
Pan, H., Liu, S., Miao, D., & Yuan, Y. (2018). Sample size determination for mediation analysis of longitudinal data. BMC Medical Research Methodology, 18(1), 1–11. https://doi.org/10.1186/s12874-018-0473-2.
Perrin, E. C., Stein, R. E. K., & Drotar, D. (1991). Cautions in using the Child Behavior Checklist: Observations based on research about children with a chronic illness. Journal of Pediatric Psychology, 16(4), 411–421.
Pinquart, M. (2018). Parenting stress in caregivers of children with chronic physical condition - A meta-analysis. Stress & Health, 34(2), 197–207.
Pinquart, M., & Shen, Y. (2011). Behavior problems in children and adolescents with chronic physical illness: A meta-analysis. Journal of Pediatric Psychology, 36(9), 1003–1016.
Scholten, L., Willemen, A. M., Last, B., Maurice-Stam, H., van Dijk, E., Ensink, E., & Grootenhuis, M. A. (2013). Efficacy of psychosocial group intervention for children with chronic illness and their parents. Pediatrics, 131(4), 1196–1203.
Schulz, K. F., Altman, D. G., & Moher, D. (2010). CONSORT 2010 Statement: Updated guidelines for reporting parallel group randomised trials. Journal of Clinical Epidemiology, 63, 834–840.
Silverman, W. K., Pina, A. A., & Viswesvaran, C. (2008). Evidence-based psychosocial treatments for phobic and anxiety disorders in children and adolescents. Journal of Clinical Child & Adolescent Psychology, 37, 105–130.
Sint Nicolaas, S. M. (2018). Resilience in pediatric oncology: Family risk and resilience factors and child behavior adjustment (Unpublished doctoral dissertation). Nijmegen, the Netherlands: Radboud University Nijmegen.
Snijders, T. A. B., & Bosker, R. J. (1999). Multilevel analysis: An introduction to basic and advanced multilevel modeling. London: Sage Publications.
Snyder, C. R., Feldman, D. B., Taylor, J. D., Schroeder, L. L., & Adams, III, V. H. (2000). The roles of hopeful thinking in preventing problems and enhancing strengths. Applied and Preventive Psychology, 9(4), 249–269.
Ullah, F., & Kaelber, D. C. (2021). Using large aggregated de-identified electronic health record data to determine the prevalence of common chronic diseases in pediatric patients who visited primary care clinics. Academic Pediatrics, 21(6), 1084–1093. https://doi.org/10.1016/j.acap.2021.05.007.
Van Cleave, J., Gortmaker, S. L., & Perrin, J. M. (2010). Dynamics of obesity and chronic health conditions among children and youth. JAMA, 303(7), 623–630.
Van der Lee, J. H., Mokkink, L. B., Grootenhuis, M. A., Heymans, H. S., & Offringa, M. (2007). Definitions and measurement of chronic health conditions in childhood: A systematic review. JAMA, 297(24), 2741–2751.
Verhulst, F. C., v. d. Ende, J., & Koot, H. M. (1996). Manual for the child behavior check list (CBCL/4-18). Rotterdam: Erasmus University/Department of Child and Adolescent Psychiatry, Sophia Children’s Hospital.
Verhulst, F. C., v. d. Ende, J., & Koot, H. M. (1997). Manual for the youth self-report (YSR). Rotterdam: Erasmus University/Department of Child and Adolescent Psychiatry, Sophia Children’s Hospital.
Wampold, B. E. (2015). How important are the common factors in psychotherapy? An update. World Psychiatry, 14(3), 270–277.
Yeh, C. H. (2003). Psychological distress: testing hypotheses based on Roy’s adaptation model. Nursing Science Quarterly, 16(3), 255–263.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by A.M.W., L.S., and E.K. The first draft of the paper was written by E.K. and all authors commented on previous versions of the paper. All authors read and approved the final paper.
Funding
This work was supported by The Netherlands Organization for Health Research and Development (project no. 15700.2002).
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (include name of committee + reference number) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Willemen, A.M., Kuzminskaite, E., Maurice-Stam, H. et al. The Working Mechanisms of Parental Involvement in Interventions for Children with Chronic Illness. J Child Fam Stud 31, 3037–3046 (2022). https://doi.org/10.1007/s10826-022-02329-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10826-022-02329-7