Abstract
Purpose
To (1) prospectively characterize the incidence of decision regret among women considering planned oocyte cryopreservation (planned OC), comparing those who pursued treatment vs those who did not freeze eggs, and (2) to identify baseline predictors for future decision regret.
Methods
A total of 173 women seen in consultation for planned OC were followed prospectively. Surveys were administered at (1) baseline (< 1 week after initial consultation) and (2) follow-up, 6 months after planned OC among participants who froze eggs or 6 months following consultation in the absence of further communication to pursue treatment. The primary outcome was the incidence of moderate-to-severe decision regret, indicated by a Decision Regret Scale score > 25. We also examined predictors of regret.
Results
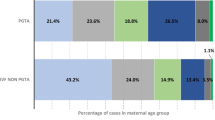
The incidence of moderate-to-severe regret over the decision to freeze eggs was 9% compared to 51% over the decision not to pursue treatment. Among women who froze eggs, adequacy of information at baseline to decide about treatment (aOR 0.16, 95% CI 0.03, 0.87) and emphasis on future parenthood (aOR 0.80, 95% CI 0.66, 0.99) were associated with reduced odds of regret. Forty-six percent of women who froze eggs regretted not doing so earlier. Among women who did not freeze eggs, the primary reasons were financial and time constraints, correlating with increased odds of decision regret in an exploratory analysis.
Conclusions
Among women undergoing planned OC, the incidence of decision regret is low compared to the regret confronting women seen in consultation for planned OC but who do not pursue treatment. Provider counseling is key to offset the regret risk.

Similar content being viewed by others
References
Hamilton BE, Martin JA, Osterman MJ, Curtin SC, Matthews TJ. Births: final data for 2014. National vital statistics reports : from the Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System. 2015;64(12):1-64.
Matthews TJ, Hamilton BE. Delayed childbearing: more women are having their first child later in life. NCHS Data Brief. 2009;21:1–8.
Planned oocyte cryopreservation for women seeking to preserve future reproductive potential: an ethics committee opinion. Fertil Steril. 2018;110(6):1022–8.
Kawwass JF, Crawford S, Hipp HS. Frozen eggs: national autologous oocyte thaw outcomes. Fertil Steril. 2021;116(4):1077–84.
Nasab S, Shah JS, Nurudeen K, Jooya ND, Abdallah ME, Sibai BM. Physicians’ attitudes towards using elective oocyte cryopreservation to accommodate the demands of their career. J Assist Reprod Genet. 2019;36(9):1935–47.
Platts S, Trigg B, Bracewell-Milnes T, Jones BP, Saso S, Parikh J, et al. Exploring women’s attitudes, knowledge, and intentions to use oocyte freezing for non-medical reasons: a systematic review. Acta Obstet Gynecol Scand. 2021;100(3):383–93.
SART. Preliminary national summary report for 2020. https://www.sartcorsonline.com/rptCSR_PublicMultYear.aspx. Accessed 12 April 2022.
ASRM. Mature oocyte cryopreservation: a guideline. Fertil Steril. 2013;99(1):37–43.
Inhorn MC, Birenbaum-Carmeli D, Birger J, Westphal LM, Doyle J, Gleicher N, et al. Elective egg freezing and its underlying socio-demography: a binational analysis with global implications. Reproductive Biol Endocrinol RB&E. 2018;16(1):70.
Göçmen İ, Kılıç A. Egg freezing experiences of women in Turkey: from the social context to the narratives of reproductive ageing and empowerment. Eur J Women’s Stud. 2018;25(2):168–82.
Baldwin K. Conceptualising women’s motivations for social egg freezing and experience of reproductive delay. Sociol Health Illn. 2018;40(5):859–73.
Hammarberg K, Kirkman M, Pritchard N, Hickey M, Peate M, McBain J, et al. Reproductive experiences of women who cryopreserved oocytes for non-medical reasons. Hum Reprod. 2017;32(3):575–81.
Pritchard N, Kirkman M, Hammarberg K, McBain J, Agresta F, Bayly C, et al. Characteristics and circumstances of women in Australia who cryopreserved their oocytes for non-medical indications. J Reprod Infant Psychol. 2017;35(2):108–18.
Baldwin K, Culley L, Hudson N, Mitchell H, Lavery S. Oocyte cryopreservation for social reasons: demographic profile and disposal intentions of UK users. Reprod Biomed Online. 2015;31(2):239–45.
Wafi A, Nekkebroeck J, Blockeel C, De Munck N, Tournaye H, De Vos M. A follow-up survey on the reproductive intentions and experiences of women undergoing planned oocyte cryopreservation. Reprod Biomed Online. 2020;40(2):207–14.
Hodes-Wertz B, Druckenmiller S, Smith M, Noyes N. What do reproductive-age women who undergo oocyte cryopreservation think about the process as a means to preserve fertility? Fertil Steril. 2013;100(5):1343–9.
Baldwin K, Culley L, Hudson N, Mitchell H. Running out of time: exploring women’s motivations for social egg freezing. J Psychosom Obstet Gynaecol. 2019;40(2):166–73.
Seyhan A, Akin OD, Ertaş S, Ata B, Yakin K, Urman B. A survey of women who cryopreserved oocytes for non-medical indications (social fertility preservation). Reprod Sci. 2021;28(8):2216–22.
Gürtin ZB, Morgan L, O’Rourke D, Wang J, Ahuja K. For whom the egg thaws: insights from an analysis of 10 years of frozen egg thaw data from two UK clinics, 2008–2017. J Assist Reprod Genet. 2019;36(6):1069–80.
Jones BP, Kasaven L, L’Heveder A, Jalmbrant M, Green J, Makki M, et al. Perceptions, outcomes, and regret following social egg freezing in the UK; a cross-sectional survey. Acta Obstet Gynecol Scand. 2020;99(3):324–32.
Stoop D, Maes E, Polyzos NP, Verheyen G, Tournaye H, Nekkebroeck J. Does oocyte banking for anticipated gamete exhaustion influence future relational and reproductive choices? A follow-up of bankers and non-bankers. Hum Reprod. 2014;30(2):338–44.
Giannopapa M, Sakellaridi A, Pana A, Velonaki VS. Women electing oocyte cryopreservation: characteristics, information sources, and oocyte disposition: a systematic review. J Midwifery Womens Health. 2022;67(2):178–201.
Blakemore JK, Grifo JA, DeVore SM, Hodes-Wertz B, Berkeley AS. Planned oocyte cryopreservation-10-15-year follow-up: return rates and cycle outcomes. Fertil Steril. 2021;115(6):1511–20.
Cobo A, García-Velasco J, Domingo J, Pellicer A, Remohí J. Elective and onco-fertility preservation: factors related to IVF outcomes. Hum Reprod. 2018;33(12):2222–31.
Brehaut JC, O’Connor AM, Wood TJ, Hack TF, Siminoff L, Gordon E, et al. Validation of a Decision Regret Scale Medical decision making : an. Int J Soc Med Decision Making. 2003;23(4):281–92.
Becerra Pérez MM, Menear M, Brehaut JC, Légaré F. Extent and predictors of decision regret about health care decisions: a systematic review Medical decision making : an. Int J Soc Med Decision Making. 2016;36(6):777–90.
Drost L, Dason ES, Han J, Doshi T, Scheer A, Greenblatt EM, et al. Patients’ and providers’ perspectives on non-urgent egg freezing decision-making: a thematic analysis. BMC Womens Health. 2023;23(1):49.
Peate M, Sandhu S, Braat S, Hart R, Norman R, Parle A, et al. Randomized control trial of a decision aid for women considering elective egg freezing: the Eggsurance study protocol. Womens Health (Lond). 2022;18:17455057221139672.
Greenwood EA, Pasch LA, Hastie J, Cedars MI, Huddleston HG. To freeze or not to freeze: decision regret and satisfaction following elective oocyte cryopreservation. Fertil Steril. 2018;109(6):1097–104.
Gurbuz A, Cil AP, Karakis LS, Abali R, Ceyhan M, Aksakal E, et al. Decision regret and associated factors following oocyte cryopreservation in patients with diminished ovarian reserve and/or age-related fertility decline. J Assist Reprod Genet. 2021;38(6):1469–79.
Pasch LA, Gregorich SE, Katz PK, Millstein SG, Nachtigall RD, Bleil ME, et al. Psychological distress and in vitro fertilization outcome. Fertil Steril. 2012;98(2):459–64.
Newton CR, Sherrard W, Glavac I. The fertility problem inventory: measuring perceived infertility-related stress. Fertil Steril. 1999;72(1):54–62.
Pennebaker JW. Expressive writing in psychological science. Perspect Psychol Sci. 2018;13(2):226–9.
Stoop D, Maes E, Polyzos NP, Verheyen G, Tournaye H, Nekkebroeck J. Does oocyte banking for anticipated gamete exhaustion influence future relational and reproductive choices? A follow-up of bankers and non-bankers. Hum Reprod. 2015;30(2):338–44.
Blakemore JK, Grifo JA, DeVore SM, Hodes-Wertz B, Berkeley AS. Planned oocyte cryopreservation—10–15-year follow-up: return rates and cycle outcomes. Fertil Steril. 2021;115(6):1511–20.
Cascante SD, Blakemore JK, DeVore S, Hodes-Wertz B, Fino ME, Berkeley AS, et al. Fifteen years of autologous oocyte thaw outcomes from a large university-based fertility center. Fertil Steril. 2022;118(1):158–66.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The study funder, EMD Serono, provided renumeration for participant time and effort. The funder provided financial support only and was not involved in the study design, data collection, analysis, or interpretation of study results. EGJ received an investigator-sponsored research grant from the study funder, EMD Serono. LP, AM, RW, JC, MIC, and HGH have nothing to disclose.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jaswa, E.G., Pasch, L.A., McGough, A. et al. Decision regret among women considering planned oocyte cryopreservation: a prospective cohort study. J Assist Reprod Genet 40, 1281–1290 (2023). https://doi.org/10.1007/s10815-023-02789-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-023-02789-w