Abstract
The placenta is essential for a successful pregnancy and healthy intrauterine development in mammals. During human pregnancy, the growth and development of the placenta are inseparable from the rapid proliferation, invasion, and migration of trophoblast cells. Previous reports have shown that the occurrence of many pregnancy disorders may be closely related to the dysfunction of trophoblasts. However, the function regulation of human trophoblast cells in the placenta is poorly understood. Therefore, studying the factors that regulate the function of trophoblast cells is necessary. MicroRNAs (miRNAs) are small, non-coding, single-stranded RNA molecules. Increasing evidence suggests that miRNAs play a crucial role in regulating trophoblast functions. This review outlines the role of miRNAs in regulating the function of trophoblast cells and several common signaling pathways related to miRNA regulation in pregnancy disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The placenta is the first organ for human development and is of great importance for transporting nutrients and oxygen between the mother and fetus [1, 2]. It has been reported that trophoblast cells are the main cells in the placenta [3]. The term “trophoblast” was first used in 1889 to describe the cells that exchange materials between the mother and fetus [4]. So far, trophoblasts have been extensively studied in vivo and in vitro. During human pregnancy, first, human embryonic cells differentiate into two types of cells, namely, inner cell mass (ICM) and trophectoderm (TE). Then, they develop into the embryo and the key part of the placenta, respectively [5]. In the human placenta, TE differentiates into trophoblast stem cells (TSCs), which further differentiate into a type of highly proliferative cell population called cytotrophoblasts (CTBs) [6]. On the one hand, rapidly proliferating CTBs form syncytiotrophoblast (STB) through cell fusion to transport oxygen and nutrients from maternal blood [7, 8]. On the other hand, the rapidly proliferating CTBs break away from the STB layer, invade the maternal endometrium and myometrium, and differentiate into invasive extravillous trophoblast cells (EVTs) [9], which then reshape the artery and widen the diameter to ensure that the fetus has sufficient blood supply [10,11,12,13].
Trophoblast cells have a variety of biological functions, including invasion, proliferation, migration, differentiation, apoptosis, autophagy, pyroptosis, ferroptosis, cellular metabolism, and angiogenesis [14]. Trophoblast cell function maintenance plays a key role in human placenta development. Among them, the proliferation and differentiation of trophoblast cells continue throughout the development of the human placenta [15, 16], and the migration and invasion transfer trophoblast cells to maternal decidua and myometrium and widen the inner diameter of arteries to provide nutritional support for the embryo [17, 18]. In summary, maintaining normal trophoblast cell function is essential for healthy placental development and successful pregnancy. However, so far, the regulatory factors of trophoblast cell function are largely unclear, which limits their application in the treatment of placental abnormalities or pregnancy disorders [19,20,21,22].
The biological function of human placental trophoblasts is a complex process that involves multiple regulatory factors. It has been found that many factors can regulate the growth and development of the placenta by targeting trophoblast cells, such as immune cells [23], transcription factors [24, 25], extracellular matrix components [26], and epigenetic modifications [27]. Among them, epigenetics refers to the heritable changes in gene function that ultimately lead to phenotypic changes without changes in the DNA sequence of the gene [28], and it mainly includes histone modification, DNA methylation, and non-coding RNAs (ncRNAs) [29, 30]. Several lines of evidence suggest that ncRNAs, especially miRNAs, play an important role in regulating trophoblast function [31].
Pregnancy disorders
The placenta not only plays a role during pregnancy but also has a profound impact on the future health of the fetus and mother [3]. Abnormal placenta development is closely related to many pregnancy disorders [32]. It has been reported that pregnancy disorders, such as hypertensive disorders of pregnancy (HDP), intrauterine growth restriction (IUGR), gestational diabetes mellitus (GDM), unexplained stillbirth, and miscarriage account for a large proportion of morbidity and mortality in mothers and newborns [33,34,35]. Among them, HDP is the leading cause of maternal and perinatal death [36, 37]. There are four main forms of HDP: chronic hypertension, gestational hypertension, pre-eclampsia-eclampsia, and chronic hypertension with superimposed pre-eclampsia [37]. Notably, pre-eclampsia (PE) is the most alarming pregnancy disorder [38]. PE is defined as new-onset hypertension with proteinuria and/or end-organ dysfunction after 20 weeks of gestation [39, 40]. Eclampsia is defined as a new-onset generalized tonic–clonic seizure in women with PE and is one of the serious complications of PE [41, 42].
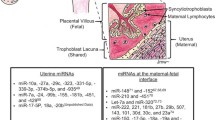
The development of pregnancy disorders is known as a complex process, accompanied by dynamic changes in various cells and molecules in the placenta. During human placental development, the walls of the uterine spiral arteries undergo reactive changes called vascular remodeling. When the free CTBs come into contact with the extracellular matrix, they differentiate into interstitial extravillous trophoblast cells (iEVTs) [43]. When iEVTs invade the arterial lumen, they differentiate into endovascular extravillous trophoblast cells (enEVTs) [44, 45]. Next, enEVTs degrade the media and smooth muscle and replace the endothelium in the maternal arteries to form high-volume, low-resistance vessels to ensure adequate blood flow to the placenta as the fetus grows and progresses during pregnancy (Fig. 1) [28]. Nevertheless, the failure of vascular remodeling can lead to a series of pregnancy disorders, such as PE, GDM, and IUGR [46]. Hence, trophoblast function plays a crucial role in vascular remodeling and contributes to the occurrence and development of pregnancy disorders. Understanding the functional regulation of the trophoblast is of great importance for the prevention and treatment of pregnancy disorders.
Remodeling of normal and abnormal spiral arteries. Extravillous trophoblast cells widen the inner diameter of the artery through invasion and migration, completing the remodeling of the spiral artery. Dysregulation of extravillous trophoblast cell migration and invasion can lead to failure of spiral arterial remodeling and inadequate fetal nutrition. ICM, inner cell mass; CTBs, cytotrophoblasts; STB, syncytiotrophoblast; iEVTs, interstitial extravillous trophoblast cells; enEVTs, extravillous trophoblast cells; NK, natural killer cell; DSC, decidual stromal cells
MiRNAs in placental development and pregnancy disorders
MicroRNAs (miRNAs) are small, endogenous, ncRNA molecules with gene regulatory activities [47, 48], and they play a key role in the regulation of various pathophysiological processes in the human body [49]. During embryonic development, miRNAs regulate multiple stages: gamete development, embryonic development, and placentation [50]. Trophoblasts are the main source of multiple circulating miRNAs in the peripheral blood of pregnant women [51,52,53,54], such as miR-519a-3p, miR-187-5p, miR-204-5p, and miR-449a [23]. Trophoblasts express three miRNA clusters, namely, chromosome 19 miRNA clusters (C19MC), chromosome 14 miRNA clusters (C14MC), and miR-371-3 clusters [48, 53, 55]. Studies have shown that these miRNA clusters are related to the development of the placenta [56], the expression of miRNAs in C14MC gradually decreased during pregnancy, while the expression of C19MC and miR-371-3 cluster members increased significantly [52, 57]. The above evidence suggests that miRNAs may serve as serum markers associated with human pregnancy.
In addition, accumulating studies suggest that the differential expression of various circulating miRNAs during pregnancy is closely related to the occurrence and development of pregnancy disorders, such as PE, GDM, IUGR, and recurrent pregnancy loss (RPL) [58,59,60,61]. Compared with normal pregnant women, the expression profile of circulating miRNA in PE patients has changed, among which the up-regulated miRNAs were miR-125b [62], miR-182-5p [63], miR-210 [64], and miR-125a-5p [65], down-regulated miRNAs are miR-218-5p [66], miR-320a [67], miR-525-5p [68], etc. Furthermore, to date, 32 different types of circulating miRNAs have been identified that are highly differentially expressed in GDM women compared to non-GDM women [69]. Taken together, miRNAs present in the maternal circulation have the potential to provide new diagnostic and therapeutic targets for pregnancy disorders.
MiRNAs regulate the trophoblast cell function in pregnancy disorders
Numerous studies have demonstrated that certain members of the miRNA cluster are involved in regulating the biological function of trophoblast, especially invasion [70,71,72], proliferation [73, 74], migration [75], differentiation [66], apoptosis [14, 72], autophagy [76], pyroptosis [77], ferroptosis [78], cellular metabolism [79, 80], and angiogenesis of trophoblast cell [81, 82].
MiRNAs regulate trophoblast invasion
Placental trophoblasts invade the connective tissue of the mother’s uterus and remodel the uterine spiral arteries, resulting in an increase in the diameter of the spiral artery and ensuring that the placenta can obtain sufficient blood supply [83, 84]. Trophoblasts’ invasion ability abnormally leads to placenta implantation failure, causing a series of pregnancy disorders, such as IUGR, PE, stillbirth, and recurrent miscarriage [17].
It was found that there are several miRNAs in the regulation invasion of trophoblast cells in pregnancy disorders [85, 86], such as miR-218-5p [66], miR-125b [62, 87], miR-182-5p [63], and miR-210 [64], which promote or inhibit the invasion of trophoblast cells by acting on target genes. Transforming growth factor-beta2 (TGF-β2) is a multifunctional polypeptide growth factor that mainly transmits signals through the complex of type I and type II serine and/or threonine receptors and plays an important role in many cellular biological processes, such as cell invasion, proliferation, differentiation, and angiogenesis. In PE placentas, miR-218-5p promoted the invasion of trophoblasts by repressing TGF-β2 expression [66]. Unlike miR-218-5p, miR-125b and miR-182-5p in the trophoblast cells of the placenta of patients with PE are significantly up-regulated [62, 63]. The voltage-gated potassium channel Kv1.1 (KCNA1), as a selective potassium channel protein in the repolarization of the cell membrane, was closely associated with trophoblast invasion. Mechanistic studies have found that miR-125b can prevent the invasion of trophoblasts by targeting KCNA1 [87]. MiR-182-5p inhibited the invasion of placental trophoblasts by down-regulating the Rnd subclass of the Rho family of small guanosine triphosphate (GTP)–binding proteins (RND3) [63]. In PE, it is well established that miR-210 is a widely studied miRNA [88, 89], miR-210 suppresses trophoblast cell invasion by down-regulating multiple target genes expression, such as potassium channel modulatory factor 1 (KCMF1), thrombospondin type-1 domain-containing 7A (THSD7A), the central scaffold protein in the bacterial ISC iron-sulfur (Fe-S) cluster biosynthesis system (ISCU), Jigged 1, and extracellular signal-regulated kinase (ERK) pathway [90, 91].
MiRNAs regulate trophoblast proliferation
Appropriate trophoblast proliferation is essential for normal fetal growth and pregnancy [92]. The proliferation of trophoblasts exists at every stage in the development of the human placenta. CTBs contribute to the rapid growth of the early placenta through high-speed proliferation [93]. The proliferating trophoblast cells merge with one another to form STB, which facilitates the delivery of nutrients and oxygen in the pregnant woman to the uterus. The rapidly proliferating CTBs differentiate to form EVTs, which then invade the uterine artery and reshape the spiral artery to ensure that the fetus has sufficient perfusion [93]. However, if trophoblast proliferation is insufficient, many pregnancy disorders, such as PE, IUGR, spontaneous abortion, and placenta accrete, will inevitably occur [94].
MiRNAs are involved in the bidirectional regulation of trophoblast proliferation [95]. In pregnancy disorders, significant differences exist in the expression profiles of four miRNAs, namely, miR-137, miR-125a-5p, miR-320a, and miR-525-5p. miR-137 was significantly up-regulated in GDM, while protein kinase AMP-activated catalytic subunitα1 (PRKAA1) was down-regulated. Next, miR-137 was found to inhibit trophoblast cell proliferation by targeting the PRKAA1/interleukin-6 (IL-6) axis [96]. In PE, the expression levels of miR-125a-5p up-regulated, whereas miR-320a and miR-525-5p down-regulated [65, 67, 68, 96, 97]. MiR-125a-5p and miR-320a inhibit the proliferation of trophoblasts by targeting vascular endothelial growth factor A (VEGFA) and interleukin-4 (IL-4), respectively [65, 67, 96]. Homeobox D10 (HOXD10) is an important regulator of gene transcription and plays a crucial role in cell proliferation, survival, and invasion. The placenta of PE patients showed low expression of MiR-525-5p and high expression of HOXD10, while inhibition of MiR-52-5p/overexpression of HOXD1 inhibited proliferation and invasion of trophoblasts [68].
MiRNAs regulate trophoblast migration
Proper trophoblast migration is essential for a successful pregnancy [98, 99]. In the human placenta, CTBs migrate into the endometrium and myometrium and transform into EVTs to prepare for the invasion of spiral arteries by trophoblast cells [100]. However, insufficient trophoblast migration results in hypoperfusion of the placenta [101], which may lead to a series of pregnancy disorders [102,103,104,105].
MiRNAs are involved in the regulation of trophoblast migration positively or negatively [90, 106]. Tao found that placental miR-124-3p was significantly up-regulated in PE patients, and miR-124-3p inhibited the migration of trophoblast cells by targeting the placental growth factor (PLGF). PLGF is mainly synthesized by trophoblast cells and plays an important role in promoting placental development [77]. In PE patients, miR-182-5p and miR-125a-5p expression levels were up-regulated, and trophoblast migration was inhibited by targeting RND and VEGFA3, respectively [63, 65, 107,108,109]. In addition, compared with normal placentas, the expression of miR-18b was down-regulated in the placental tissue of PE patients, while the level of its target gene notch homolog protein 2 (Notch2) was increased. When trophoblast cells were transfected with mimics of miR-18b, the expression level of Notch2 decreased and the migration ability of trophoblast cells was enhanced [110].
MiRNAs regulate trophoblast differentiation
The development of the early placenta is under hypoxic conditions, whereas late placental development is carried out under aerobic conditions [111]. During the entire process of placental development, the rapidly proliferating CTBs continue to differentiate into STBs and EVTs to prepare sufficient nutrients and oxygen for the growth and development of the placenta [101, 112, 113]. However, if differentiation is destroyed, serious pregnancy disorders occurred [114].
MiRNAs have been demonstrated to participate in the regulation of trophoblast cell differentiation [115,116,117]. The most common ones are the miR-17–92 cluster and the miR-106a-363 cluster. MiR-17–92 cluster encodes six miRNAs (miR-17, miR-18a, miR-19a, miR-20a, miR-19b-1, and miR-92a-1). The miR-106a-363 cluster also encodes six miRNAs (miR-106a, miR-18b, miR-20b, miR-19b-2, miR-92a-2, and miR-363) [118]. It was found that the miR-17–92 cluster and miR-106a-363 cluster were significantly up-regulated in CTBs while down-regulated in STBs. In PE, up-regulated miR-106a and miR-19b inhibit the differentiation of placental trophoblasts by inhibiting human CYP19A1 (hCYP19A1) and human GCM1 (hGCM1) expression, respectively [118]. hCYP19A1 is closely related to the synthesis of estrogen in pregnant women, which can promote placental angiogenesis and increase uteroplacental blood flow [119,120,121]. Elevated levels of miR-106a and miR-19b can cause insufficient STB cells in maternal blood and decreased angiogenesis of endometrium, leading to pregnancy disorders.
MiRNAs regulate trophoblast apoptosis
Apoptosis is a basic biological phenomenon and a basic measure to maintain the dynamic balance of the number of cells in the body. During the embryonic development stage, excess and mission-completed cells are removed through apoptosis, thereby ensuring the normal development of the embryo. Numerous studies have discovered that proper trophoblast apoptosis is beneficial to fetus growth and development. Insufficient and excessive apoptosis of trophoblast can lead to a series of pregnancy disorders [122, 123].
It was shown that intervention of trophoblast cell apoptosis may be a direction to prevent pregnancy disorders, especially regulating by miRNAs [124]. Pregnancy disorders can occur if trophoblast apoptosis is inhibited, such as PE, GDM, and IUGR. In the placenta of patients with GDM, miR-29b inhibited trophoblast cell apoptosis by targeting the hypoxia-inducible factor 3alpha gene (HIF3A) [77, 125]. HIF3A is a negative regulator of hypoxia-inducible gene expression, which regulates many adaptive responses to low oxygen tension (hypoxia) and has been shown to play a key role in cell metabolism and apoptosis. Moreover, excessive trophoblast apoptosis also brings a series of pregnancy disorders. In PE, one of the most up-regulated miRNAs is miR-30a-3p, which promotes trophoblast apoptosis through the targeted inhibition of insulin-like growth factor 1 (IGF-1) [72, 126]. Compared with normal pregnant women, miR-141 and miR-34a were significantly up-regulated in PE; miR-141 and miR-34a promoted trophoblast apoptosis by targeting C-X-C motif chemokine ligand 12 (CXCL12β) and anti-apoptosis member B-cell CLL/lymphoma 2 (BCL-2) gene expression, respectively [72, 123, 126].
MiRNAs regulate trophoblast autophagy, pyroptosis, and ferroptosis
Autophagy, a type of programmed cell death, is a physiological mechanism for maintaining cellular homeostasis and nutrient cycling. Autophagy plays a crucial role in placenta formation and embryonic development [127]. Moderate trophoblast autophagy is important for maintaining a healthy pregnancy, and inappropriate trophoblast autophagy may interfere with cellular homeostasis and lead to placental abnormalities, which can lead to a range of pregnancy disorders [128]. It was found that in PE, LET-7I inhibits trophoblast autophagy by down-regulating the expression of autophagy-related 4B cysteine peptidase (Atg4B) [129]. Notably, the placenta is not only a conduit for material exchange between mother and baby, but it also provides a physical barrier to microbial invasion. Recently, accumulating studies suggest that intrauterine viral infection is the main cause of pregnancy disorders, such as PE, repeated miscarriages (RM), and IUGR. Studies have found that trophoblast autophagy may play a key role in intrauterine viral infection, and some miRNAs in the C19MC family are involved in the regulation of trophoblast autophagy. In the placenta of patients with intrauterine virus infection, miR517-3p, miR516b-5p, and miR512-3p promote trophoblast autophagy. However, the specific molecular mechanism remains to be further studied [130]. Therefore, excessive autophagy may be an important mechanism of pregnancy disorder induced by intrauterine virus infection.
Pyroptosis is a new type of programmed cell death, which is characterized by dependence on caspases (mainly caspase-1, 4, 5, 11), accompanied by inflammatory factor release [131,132,133]. Excessive inflammation can lead to a variety of pregnancy disorders, such as PE, premature birth, or miscarriage in pregnant women [134]. Downregulated miR-520c-3p inhibits trophoblast pyroptosis by targeting the SET domain containing lysine methyltransferase 7 (SETD7) in placental tissue from PE patients [135]. Unlike miR-520c-3p, miR-124-3p was significantly up-regulated in PE patients, and miR-124-3p promotes trophoblast pyroptosis by inhibiting the expression of PLGF [77].
Ferroptosis is a novel iron-dependent programmed cell death [136]. Ferroptosis plays a crucial role in pregnancy disorders by causing damage to trophoblast cells [136,137,138]. Compared with normal placental tissue, the expression of miR-30b-5p was significantly up-regulated in the placenta of patients with PE, miR-30b-5p induces the expression of Ferroportin1 (an iron exporter) by down-regulating Cys2/glutamate antiporter (system Xc − , SLC7A11), thereby reducing glutathione (GSH) synthesis and increasing iron accumulation, thereby promoting trophoblast ferroptosis. Furthermore, the knockdown of miR-30b-5p slowed the onset of PE in a rat placenta of an eclampsia model [78].
Other functions regulated by miRNAs
The oxygen concentration in the early stage of placental development is relatively low [139], and trophoblast cells mainly synthesize ATP through glycolysis and lactic acid fermentation to maintain the energy supply of tissues [140]. Pieces of evidence show that miRNAs regulate trophoblast metabolism through corresponding targets to adapt to changes in oxygen levels throughout pregnancy [140]. Compared with normal pregnant women, the expression of miR-143 in the placenta of GDM patients is down-regulated, and miR-143 improves mitochondrial function by up-regulating the expression of mitochondrial complexes 1, 2, and 3, which in turn increased trophoblast metabolism to adapt to changes in oxygen levels throughout pregnancy [141]. Mitochondrial dysfunction in the placenta of patients with pregnancy disorders has been reported to be closely associated with uncontrolled oxidative stress (OS). In the placenta of GDM patients, the up-regulated miR-130b-3p contributes to its OS by targeting the inhibition of peroxisome proliferator-activated receptor-gamma co-activator-1alpha (PGC-1α) expression [142]. MiR-199a-5p, which is overexpressed in the placenta of patients with IUGR, may play a role in placental OS and mitochondrial function damage, but the mechanism remains unclear [143].
Placental vascularization is critical for meeting the metabolic demands of a rapidly growing fetus [141]. Delayed or reduced placental vascular development can lead to a variety of pregnancy disorders, such as early embryo arrest (EEA), recurrent spontaneous abortion (RSA), and PE [16]. Early growth response factor 1 (EGR1) is a nuclear transcription factor related to cell proliferation, differentiation, and angiogenesis, which is involved in the regulation of multiple biological functions. In the placenta of EEA patients, up-regulated miR-518b inhibits placental angiogenesis by targeting EGR1 [144]. Compared with normal pregnant rats, overexpressed miR-126 in the placenta of RSA model rats inhibited placental angiogenesis by inhibiting the expression of VEGF. In addition, the down-regulation of miR-126 also resulted in endothelial dysfunction of placental vessels, which further supports the importance of miR-126 in placental vascular development [145,146,147]. In IUGR, it has been found that deletion of the miR-290 cluster in mice leads to disturbance of the labyrinthine vasculature, which in turn inhibits angiogenesis, but the exact mechanism still needs further investigation [74]; this also provides strong evidence that miRNAs are important regulators of placental vascular development. Of note, up to now, there is no evidence that miRNAs are involved in the regulation of trophoblast angiogenesis positively.
Among the ways in which miRNAs regulate the function of trophoblast cells, there are several different ways: one miRNA regulates several biological functions, or one biological function is regulated by multiple miRNAs. For example, miR-124-3p regulates migration, invasion, and apoptosis of trophoblast cells [77]. MiR-182-5p regulates trophoblast migration and invasion [63]. The invasion of trophoblasts may be regulated by multiple miRNAs, such as miR-218-5p, miR-125b, and miR-182-5p [63, 66, 87]. The proliferation of trophoblast cells is regulated by miR-137, miR-320a, miR-125a-5p, and miR-525-5p [65, 67, 68, 96]. These pieces of evidence indicate that the regulation of miRNAs is a complex network in trophoblast cells (Table 1) and miRNAs may be used as specific non-invasive biomarkers and potential targets for the treatment of pregnancy disorders.
Related pathways of miRNA regulation of trophoblast cell function
The activity and function of trophoblasts involve a variety of molecular pathways. MiRNAs play a crucial role in regulating the function of trophoblast by inhibiting or promoting gene expression in related pathways.
TGF-β
TGF-β is a multifunctional cytokine involved in the regulation of various cellular biological functions, such as cell invasion, proliferation, migration, differentiation, apoptosis, and autophagy [148]. TGF-β belongs to the TGF superfamily, which contains more than 30 cytokines, such as Nodal, bone morphogenetic proteins (BMPs), activins/inhibins, growth and differentiation factors (GDFs), inhibins, and anti-Müllerian hormone (AMH) [149]. The TGF-β signaling pathway involves activation of the tetramers that make up type I and type II receptors, which in turn activate and phosphorylate intracellular effectors, namely, Sma- and Mad-related proteins (SMADs) [150, 151]. Numerous studies have demonstrated that the TGF-β pathway plays a key role in regulating the invasion and migration of trophoblast cells [152,153,154]. Multiple cytokines in the TGF-β family are targets of aberrant miRNA expression in pregnancy disorders [150]. Compared with normal pregnant women, the expression of miR-378a-5p was significantly decreased in PE patients; miR-378a-5p promotes trophoblast invasion, proliferation, and migration by targeting Nodal [154, 155]. Up-regulated miR-140-5p in patients with HDP promotes trophoblast invasion and migration by downregulating the activity of the TGF-β/Smad pathway [156]. Activin type IIA receptor (ActRIIA) and activin type IIB receptor (ActRIIB) are target genes that regulate certain key proteins in the TGF-β pathway [157]. It was found that down-regulated miR-195 in the placenta of patients with PE inhibited trophoblast invasion by inhibiting the expressions of ActRIIA and ActRIIB [158]. Taken together, miRNAs can regulate trophoblast function by targeting the TGF-β pathway.
MAPK
Signal molecules related to the mitogen-activated protein kinase (MAPK) pathway are a highly conserved family of protein kinases, which plays a crucial role in signal transmission between cells [150]. The MAPK pathway primarily includes three pathways, namely, classic MAPK, c-Jun amino-terminal kinase (JNK)/p38 MAPK (JNK/p38MAPK), and extracellular signal-regulated kinase 5 (ERK5). Among them, the JNK/p38MAPK pathway is mainly related to inflammation and cell apoptosis, while the ERK pathway is related to cell invasion, proliferation, migration, and differentiation. Studies have discovered that MAPK pathway plays an important role in regulating the biological function of trophoblasts [159], especially in trophoblast cell migration and invasion [160]. Recently, accumulating studies suggest that fibroblast growth factors (FGFs) have many physiological functions. Among them, the most important is activating MAPK to promote the invasion and proliferation of trophoblast cells [161]. In IUGR, fibroblast growth factor 1 (FGF1) is the direct target of miR-210-3p. MiR-210-3p suppresses the invasion of trophoblasts by inhibiting the expression of FGF1 [162]. The adhesion molecule integrin alpha-6 (ITGA6), as a member of the integrin family, can regulate the biological function of trophoblast through MAPK signal pathway. In the placenta of RSA patients, miR-410-5p down-regulated the proliferation, migration, and invasion of trophoblast by inhibiting the expression of ITGA6 [163].
PI3K/AKT
Phosphatidylinositol-3-kinase (PI3K) is a dimer composed of regulatory subunit p85 and catalytic subunit p110. PI3K, which is activated by various extracellular factors, activates protein kinase B (AKT) through phosphorylation, thereby regulating cell biological functions [164]. Many pathophysiological activities are inseparable from the PI3K/AKT pathway. However, this pathway was terminated by tensin homolog (PTEN) [165]. As a phosphatase, PTEN can dephosphorylate Akt and prevent all downstream signaling events regulated by Akt and is a negative regulator of PI3K. Moreover, studies have shown that the different expression levels of PTEN may lead to corresponding changes in cell function, especially cell proliferation [166,167,168,169]. MiRNAs have been demonstrated to participate in the regulation of trophoblast cell functions by targeting PTEN [170]. For example, compared with the normal pregnancy group, the expression of miR-144 in the placenta of PE patients was down-regulated, while the expression of PTEN was up-regulated. MiR-144 promotes trophoblast proliferation by repressing PTEN [171].
Matrix metalloproteinases
Matrix metalloproteinases (MMPS) are a large family, which require Ca2+, Zn2+, and other metal ions as cofactors. Among them, matrix metalloproteinase-2 (MMP-2) and matrix metalloproteinase-9 (MMP-9) play key roles in regulating the function of trophoblast cells [172,173,174], especially during gestational trophoblast cell invasion [175]. MMP-2 and MMP-9 can degrade elastin, collagen, and laminin, so that they can invade the extracellular matrix of uterine decidua, integrate into the wall of the muscular spiral artery, widen the arterial wall, and ensure that the fetus gets enough nutrition. In addition, it is interesting to note that MMP-2 and MMP-9 are direct targets of many miRNAs in pregnancy-related disorders, such as miR-519d-3p, miR-20b, and miR-150-5p [86, 176, 177]. In PE, up-regulated miR-519d-3p and miR-20b target the down-regulation of MMP-2 to inhibit trophoblast migration and invasion [176, 177]. Unlike miR-519d-3p and miR-20b, miR-150-5p, which is upregulated in PE patients, promotes trophoblast invasion by targeting MMP-9 expression [178].
Other pathways
In addition to the pathways discussed above, many other pathways, such as Wnt [179, 180], Notch [181, 182], EphrinB2-EphB4 [183, 184], and endothelial nitric oxide synthase (eNOS), affect the biological function of trophoblast cells. In pregnancy disorders, especially PE and IUGR, multiple dysregulated circulating miRNAs impair the biological function of trophoblast cells by targeting different signaling molecules.
Accumulating evidence suggests that in pregnancy disorders, miRNAs target multiple signaling molecules to regulate the biological functions of trophoblast cells (Fig. 2) [28]. For example, compared with normal pregnant patients, the expression of miR-210 and miR-155 was up-regulated in the placenta of PE patients. miR-210 suppresses trophoblast cell invasion by down-regulating multiple target genes expressions, such as KCMF1, THSD7A, ISCU, and Jigged 1 [90]. Up-regulated miR-155 inhibits trophoblast invasion by targeting Cyclin D1 (CCND1) and eNOS expression [185, 186].
TGF-β pathway, MAPK pathway, and PI3K/AKT pathway. MiRNAs regulate trophoblast biological functions through TGF-β pathway, MAPK pathway, and PI3K/AKT pathway. TGF-β, transforming growth factor β; BMP, bone morphogenetic protein; GDF, growth and differentiation factor; SMAD, Sma- and Mad-related protein; ActRIIA, activin type IIA receptor; ActRIIB, activin type IIB receptor; TGF-βRII, transforming growth factor-beta receptor II; BMPR2, bone morphogenetic protein receptor-2; MAPK, mitogen-activated protein kinase; ERK, extracellular signal-regulated kinase; JNK, c-Jun NH2-terminal kinase; MAP3K, MAPK kinase; MAP2K, MAPK kinase; MLK3, mixed-lineage kinase 3; ASK1, apoptosis signal-regulating kinase 1; MEKK1, MEK kinase 1; PI3K, phosphatidylinositol-3-kinase; AKT, protein kinase B; PTEN, tensin homolog
Furthermore, it is interesting to note that certain proteins in various pathways may interact with one another by activating or inhibiting other pathways. For example, the main components of the IGF-1 signal can activate MAPK pathways and jointly regulate trophoblast cell biological function [187]. Wnt and TGF-β pathways can negatively regulate the expression of MMP-2/9 and down-regulate trophoblast cell invasion [188, 189].
Conclusions and perspectives
This review summarized miRNAs that target corresponding mRNAs and regulate the biological function of trophoblasts in pregnancy disorders, including trophoblast cell invasion, proliferation, migration, differentiation, apoptosis, autophagy, pyroptosis, ferroptosis, cellular metabolism, and angiogenesis through different pathways. Proper function of the trophoblast is essential for embryonic development, while the abnormal function of the trophoblast may lead to pregnancy disorders [190, 191]. Of note, pyroptosis and ferroptosis are the most studied programmed cell death modes in recent years, but few studies have investigated the regulation of miRNAs in pregnancy disorders by regulating pyroptosis and ferroptosis of trophoblast cells. Therefore, plenty of work still needs to be done in determining the types of placental miRNAs and related pathways. At present, although hundreds of different miRNAs are known to be expressed in the placental trophoblast, the pathways by which most miRNAs regulate the biological functions of trophoblast cells remain unclear. Besides, the maternal ability to maintain pregnancy and nurture the fetus also depends on the strong endocrine function of the placenta, and trophoblast cells are the main endocrine cells in the placenta. However, to date, the regulation of miRNAs on the endocrine function of trophoblast cells has not been reported. In summary, these studies indicate that more data are necessary to investigate the mechanisms by which miRNAs regulate the biological and endocrine functions of trophoblast cells.
NcRNAs are a class of non-protein-coding RNAs, which mainly include miRNAs, circulating long non-coding RNAs (lncRNAs), and circular RNAs (circRNAs). Among them, numerous studies have demonstrated that miRNAs regulate the function of trophoblast cells through different targets in pregnancy and thus participate in the occurrence and development of pregnancy disorders, while the application of lncRNAs and circRNAs in the regulation of trophoblast cell function is relatively rare [192]. In addition, miRNAs are specifically expressed according to various tissues, which can be directly collected from maternal blood samples and the content is relatively stable [56, 193]. The above pieces of evidence suggest that miRNAs can serve as ideal non-intrusive biomarkers in pregnancy disorders. Therefore, in-depth exploration of the precise roles of miRNAs in the regulation of trophoblast cells and active promotion of the development of circulating miRNAs as non-invasive biomarkers for pregnancy disorders will help prevent and treat pregnancy disorders in the future.
It is interesting to note that the differential expression of lncRNA and circRNA is closely related to the occurrence and development of pregnancy disorders [190, 191, 194]. For example, so far, lncRNA H19 (H19) is one of the most thoroughly studied lncRNAs [195], and H19 is closely related to the occurrence and development of PE and IUGR [192, 196, 197]. Compared with normal pregnant women, patients with early RSA have 123 differentially expressed circRNAs, of which 78 are up-regulated and 45 are down-regulated, but the specific mechanism remains unclear [191]. Therefore, the differential expression of lncRNAs and circRNAs in pregnancy diseases may be a focus for future pregnancy disorders research.
Recently, accumulating studies suggest that patients with coronavirus disease 2019 (COVID‐19) share many similarities with those with pregnancy disorders. COVID-19 patients are characterized by increased expression of proinflammatory cytokines, such as IL-2, IL6, IL-17, and tumor necrosis factor-alpha (TNFα) [198, 199]. During the development of pregnancy disorders, pro-inflammatory cytokines, such as IL-1β, IL-6, IL-17, and TNFα, are also significantly increased [200, 201]. Moreover, there is an increased incidence of preterm birth and low birth weight in COVID-19-positive pregnant women [202]. In humans, miRNAs can target inflammatory factors to regulate the function of trophoblast cells, and then participate in the occurrence and development of pregnancy disorders [67]. To date, no study has investigated whether miRNAs in COVID-19-positive pregnant women can regulate pregnancy disorders by targeting the expression of related inflammatory factors. Therefore, this research gap may be the focus of future research.
References
Gamage T, et al. The role of DNA methylation in human trophoblast differentiation. Epigenetics. 2018;13(12):1154–73.
Zaga-Clavellina V, et al. Central role of the placenta during viral infection: immuno-competences and miRNA defensive responses. Biochim Biophys Acta Mol Basis Dis. 2021;1867(10):166182.
Turco MY and Moffett A Development of the human placenta. Dev. 2019;146(22). https://doi.org/10.1242/dev.163428.
Pijnenborg R, Vercruysse L. A.A.W. Hubrecht and the naming of the trophoblast. Placenta. 2013;34(4):314–9.
Piliszek A, et al. Cell fate in animal and human blastocysts and the determination of viability. Mol Hum Reprod. 2016;22(10):681–90.
James JL, et al. Can we fix it? Evaluating the potential of placental stem cells for the treatment of pregnancy disorders. Placenta. 2014;35(2):77–84.
Burton GJ, Fowden AL. The placenta: a multifaceted, transient organ. Philos Trans R Soc Lond B Biol Sci. 2015;370(1663):20140066.
Gamage TK, Chamley LW, James JL. Stem cell insights into human trophoblast lineage differentiation. Hum Reprod Update. 2016;23(1):77–103.
Prakobphol A, et al. A role for the L-selectin adhesion system in mediating cytotrophoblast emigration from the placenta. Dev Biol. 2006;298(1):107–17.
Burton GJ, Jauniaux E. What is the placenta? Am J Obstet Gynecol. 2015;213(4 Suppl):S6.e1-S6-8.
Cross JC. Genetic insights into trophoblast differentiation and placental morphogenesis. Semin Cell Dev Biol. 2000;11(2):105–13.
Maltepe E, Fisher SJ. Placenta: the forgotten organ. Annu Rev Cell Dev Biol. 2015;31:523–52.
Apps R, et al. Genome-wide expression profile of first trimester villous and extravillous human trophoblast cells. Placenta. 2011;32(1):33–43.
Hayder H, et al. MicroRNAs: crucial regulators of placental development. Reproduction. 2018;155(6):R259-r271.
Red-Horse K, et al. Trophoblast differentiation during embryo implantation and formation of the maternal-fetal interface. J Clin Invest. 2004;114(6):744–54.
Reynolds LP, Redmer DA. Angiogenesis in the placenta. Biol Reprod. 2001;64(4):1033–40.
Huppertz B. Traditional and new routes of trophoblast invasion and their implications for pregnancy diseases. Int J Mol Sci. 2019;21(1):289.
Burton GJ, et al. Uterine glands provide histiotrophic nutrition for the human fetus during the first trimester of pregnancy. J Clin Endocrinol Metab. 2002;87(6):2954–9.
Mohaupt M. Molecular aspects of preeclampsia. Mol Aspects Med. 2007;28(2):169–91.
Guttmacher AE, Spong CY. The human placenta project: it’s time for real time. Am J Obstet Gynecol. 2015;213(4 Suppl):S3-5.
Nelson DM. How the placenta affects your life, from womb to tomb. Am J Obstet Gynecol. 2015;213(4 Suppl):S12–3.
Liu Y, et al. Single-cell RNA-seq reveals the diversity of trophoblast subtypes and patterns of differentiation in the human placenta. Cell Res. 2018;28(8):819–32.
Li L, et al. miRNAs in decidual NK cells: regulators worthy of attention during pregnancy. Reprod Biol Endocrinol. 2021;19(1):150.
Loregger T, Pollheimer J, Knöfler M. Regulatory transcription factors controlling function and differentiation of human trophoblast—a review. Placenta. 2003;24(Suppl A):S104–10.
Knöfler M, Pollheimer J. IFPA Award in Placentology lecture: molecular regulation of human trophoblast invasion. Placenta. 2012;33(Suppl(2)):S55-62.
Damsky CH, Fitzgerald ML, Fisher SJ. Distribution patterns of extracellular matrix components and adhesion receptors are intricately modulated during first trimester cytotrophoblast differentiation along the invasive pathway, in vivo. J Clin Invest. 1992;89(1):210–22.
Seitz H, et al. A large imprinted microRNA gene cluster at the mouse Dlk1-Gtl2 domain. Genome Res. 2004;14(9):1741–8.
Kohan-Ghadr HR, et al. Potential role of epigenetic mechanisms in regulation of trophoblast differentiation, migration, and invasion in the human placenta. Cell Adh Migr. 2016;10(1–2):126–35.
Halusková J. Epigenetic studies in human diseases. Folia Biol (Praha). 2010;56(3):83–96.
Szyf M. Epigenetics, DNA methylation, and chromatin modifying drugs. Annu Rev Pharmacol Toxicol. 2009;49:243–63.
Lytle JR, Yario TA, Steitz JA. Target mRNAs are repressed as efficiently by microRNA-binding sites in the 5’ UTR as in the 3’ UTR. Proc Natl Acad Sci U S A. 2007;104(23):9667–72.
Smith GC. First-trimester determination of complications of late pregnancy. JAMA. 2010;303(6):561–2.
Brosens I, et al. The “Great Obstetrical Syndromes” are associated with disorders of deep placentation. Am J Obstet Gynecol. 2011;204(3):193–201.
Graham W, et al. Diversity and divergence: the dynamic burden of poor maternal health. Lancet. 2016;388(10056):2164–75.
Chappell LC, et al. Pre-eclampsia. Lancet. 2021;398(10297):341–54.
Gestational Hypertension and Preeclampsia. ACOG Practice Bulletin Summary, Number 222. Obstet Gynecol. 2020;135(6):1492–5.
Wilkerson RG, Ogunbodede AC. Hypertensive disorders of pregnancy. Emerg Med Clin North Am. 2019;37(2):301–16.
Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet Gynecol. 2013;122(5):1122–31.
Uludag SZ, et al. Incidence and outcomes of eclampsia: a single-center 30-year study. Hypertens Pregnancy. 2019;38(2):119–23.
Leeman L, Dresang LT, Fontaine P. Hypertensive disorders of pregnancy. Am Fam Physician. 2016;93(2):121–7.
Bergman L, et al. Investigating maternal brain alterations in preeclampsia: the need for a multidisciplinary effort. Curr Hypertens Rep. 2019;21(9):72.
Magley M, Hinson MR, Haddad LM. Eclampsia (Nursing). 2022 Feb 16. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022.
Kemp B, et al. Invasive depth of extravillous trophoblast correlates with cellular phenotype: a comparison of intra- and extrauterine implantation sites. Histochem Cell Biol. 2002;117(5):401–14.
Espinoza J, et al. Normal and abnormal transformation of the spiral arteries during pregnancy. J Perinat Med. 2006;34(6):447–58.
Anin SA, Vince G, Quenby S. Trophoblast invasion. Hum Fertil (Camb). 2004;7(3):169–74.
Lu S, et al. Effect of 20-hydroxyeicosatetraenoic acid on biological behavior of human villous trophoblasts and uterine vascular smooth muscle cells. Mol Med Rep. 2014;9(5):1889–94.
Lai EC. Micro RNAs are complementary to 3’ UTR sequence motifs that mediate negative post-transcriptional regulation. Nat Genet. 2002;30(4):363–4.
Bartel DP. MicroRNAs: genomics, biogenesis, mechanism, and function. Cell. 2004;116(2):281–97.
Qu K, et al. MicroRNAs: key regulators of endothelial progenitor cell functions. Clin Chim Acta. 2015;448:65–73.
Wilkins-Haug L. Epigenetics and assisted reproduction. Curr Opin Obstet Gynecol. 2009;21(3):201–6.
Donker RB, et al. The expression profile of C19MC microRNAs in primary human trophoblast cells and exosomes. Mol Hum Reprod. 2012;18(8):417–24.
Morales-Prieto DM, et al. MicroRNA expression profiles of trophoblastic cells. Placenta. 2012;33(9):725–34.
Morales-Prieto DM, et al. Elsevier Trophoblast Research Award Lecture: origin, evolution and future of placenta miRNAs. Placenta. 2014;35(Suppl):S39-45.
Yang H, et al. Clinical application of exosomes and circulating microRNAs in the diagnosis of pregnancy complications and foetal abnormalities. J Transl Med. 2020;18(1):32.
Slezak-Prochazka I, et al. MicroRNAs, macrocontrol: regulation of miRNA processing. RNA. 2010;16(6):1087–95.
Morales-Prieto DM, et al. Pregnancy-associated miRNA-clusters. J Reprod Immunol. 2013;97(1):51–61.
Gu Y, et al. Differential miRNA expression profiles between the first and third trimester human placentas. Am J Physiol Endocrinol Metab. 2013;304(8):E836–43.
Aplin JD, et al. Tracking placental development in health and disease. Nat Rev Endocrinol. 2020;16(9):479–94.
Hemmatzadeh M, et al. MicroRNAs: small molecules with a large impact on pre-eclampsia. J Cell Physiol. 2020;235(4):3235–48.
Addo KA, et al. Placental microRNAs: responders to environmental chemicals and mediators of pathophysiology of the human placenta. Toxicol Rep. 2020;7:1046–56.
Chaiwangyen W, et al. PM10 alters trophoblast cell function and modulates miR-125b-5p expression. Biomed Res Int. 2022;2022:3697944.
Yang W, et al. miR-125b enhances IL-8 production in early-onset severe preeclampsia by targeting sphingosine-1-phosphate lyase 1. PLoS ONE. 2016;11(12):e0166940.
Fang YN, et al. Highly expressed miR-182-5p can promote preeclampsia progression by degrading RND3 and inhibiting HTR-8/SVneo cell invasion. Eur Rev Med Pharmacol Sci. 2018;22(20):6583–90.
Zhang Y, et al. Elevated levels of hypoxia-inducible microRNA-210 in pre-eclampsia: new insights into molecular mechanisms for the disease. J Cell Mol Med. 2012;16(2):249–59.
Andraweera PH, et al. Placental expression of VEGF family mRNA in adverse pregnancy outcomes. Placenta. 2012;33(6):467–72.
Brkić J, et al. MicroRNA-218-5p promotes endovascular trophoblast differentiation and spiral artery remodeling. Mol Ther. 2018;26(9):2189–205.
Xie N, Jia Z, Li L. miR-320a upregulation contributes to the development of preeclampsia by inhibiting the growth and invasion of trophoblast cells by targeting interleukin 4. Mol Med Rep. 2019;20(4):3256–64.
Zhang M, et al. Regulatory mechanism of miR-525-5p in over-invasion of trophoblast. J Obstet Gynaecol Res. 2021;47(2):679–88.
Zhu W, et al. Epigenetic alternations of microRNAs and DNA methylation contribute to gestational diabetes mellitus. J Cell Mol Med. 2020;24(23):13899–912.
Xu P, et al. Variations of microRNAs in human placentas and plasma from preeclamptic pregnancy. Hypertension. 2014;63(6):1276–84.
Luo R, et al. MicroRNA-210 contributes to preeclampsia by downregulating potassium channel modulatory factor 1. Hypertension. 2014;64(4):839–45.
Niu ZR, et al. MicroRNA-30a-3p is overexpressed in the placentas of patients with preeclampsia and affects trophoblast invasion and apoptosis by its effects on IGF-1. Am J Obstet Gynecol. 2018;218(2):249.e1-249.e12.
Yan T, et al. MicroRNA-126 regulates EPCs function: implications for a role of miR-126 in preeclampsia. J Cell Biochem. 2013;114(9):2148–59.
Paikari A, et al. The eutheria-specific miR-290 cluster modulates placental growth and maternal-fetal transport. Development. 2017;144(20):3731–43.
Zhang M, et al. Primate-specific miR-515 family members inhibit key genes in human trophoblast differentiation and are upregulated in preeclampsia. Proc Natl Acad Sci U S A. 2016;113(45):E7069-e7076.
Delorme-Axford E, et al. Human placental trophoblasts confer viral resistance to recipient cells. Proc Natl Acad Sci U S A. 2013;110(29):12048–53.
Tao J, et al. MiR-124-3p promotes trophoblast cell HTR-8/SVneo pyroptosis by targeting placental growth factor. Placenta. 2020;101:176–84.
Zhang H, et al. miR-30-5p-mediated ferroptosis of trophoblasts is implicated in the pathogenesis of preeclampsia. Redox Biol. 2020;29:101402.
Muralimanoharan S, et al. MIR-210 modulates mitochondrial respiration in placenta with preeclampsia. Placenta. 2012;33(10):816–23.
Colleoni F, et al. Suppression of mitochondrial electron transport chain function in the hypoxic human placenta: a role for miRNA-210 and protein synthesis inhibition. PLoS ONE. 2013;8(1):e55194.
Zhu Y, et al. MicroRNA-16 inhibits feto-maternal angiogenesis and causes recurrent spontaneous abortion by targeting vascular endothelial growth factor. Sci Rep. 2016;6:35536.
Ji L, et al. MiR-136 contributes to pre-eclampsia through its effects on apoptosis and angiogenesis of mesenchymal stem cells. Placenta. 2017;50:102–9.
Abbas Y, et al. Investigation of human trophoblast invasion in vitro. Hum Reprod Update. 2020;26(4):501–13.
Moser G, et al. Human trophoblast invasion: new and unexpected routes and functions. Histochem Cell Biol. 2018;150(4):361–70.
Doridot L, et al. Trophoblasts, invasion, and microRNA. Front Genet. 2013;4:248.
Yu Y, et al. MicroRNA-204 suppresses trophoblast-like cell invasion by targeting matrix metalloproteinase-9. Biochem Biophys Res Commun. 2015;463(3):285–91.
Li Q, et al. Elevated microRNA-125b inhibits cytotrophoblast invasion and impairs endothelial cell function in preeclampsia. Cell Death Discov. 2020;6:35.
Lv Y, et al. Roles of microRNAs in preeclampsia. J Cell Physiol. 2019;234(2):1052–61.
Kolkova Z, et al. Association of circulating miRNA expression with preeclampsia, its onset, and severity. Diagnostics (Basel). 2021;11(3):476.
Hu XQ, Zhang L. MicroRNAs in uteroplacental vascular dysfunction. Cells. 2019;8(11):1344.
Anton L, et al. miR-210 inhibits trophoblast invasion and is a serum biomarker for preeclampsia. Am J Pathol. 2013;183(5):1437–45.
Sun M, et al. Cyclin G2 is involved in the proliferation of placental trophoblast cells and their interactions with endothelial cells. Med Sci Monit. 2020;26:e926414.
Ali A, et al. The role of LIN28-let-7-ARID3B pathway in placental development. Int J Mol Sci. 2020;21(10):3637.
Liu M, et al. miR-518b enhances human trophoblast cell proliferation through targeting Rap1b and activating Ras-MAPK signal. Front Endocrinol (Lausanne). 2018;9:100.
Arthurs AL, Lumbers ER, Pringle KG. MicroRNA mimics that target the placental renin-angiotensin system inhibit trophoblast proliferation. Mol Hum Reprod. 2019;25(4):218–27.
Lu TM, Lu W, Zhao LJ. MicroRNA-137 affects proliferation and migration of placenta trophoblast cells in preeclampsia by targeting ERRα. Reprod Sci. 2017;24(1):85–96.
Li J, et al. A microRNA signature in gestational diabetes mellitus associated with risk of macrosomia. Cell Physiol Biochem. 2015;37(1):243–52.
Hammer A. Immunological regulation of trophoblast invasion. J Reprod Immunol. 2011;90(1):21–8.
Soares MJ, et al. Adaptive mechanisms controlling uterine spiral artery remodeling during the establishment of pregnancy. Int J Dev Biol. 2014;58(2–4):247–59.
Silva JF, Serakides R. Intrauterine trophoblast migration: a comparative view of humans and rodents. Cell Adh Migr. 2016;10(1–2):88–110.
Tan D, et al. CUL4A enhances human trophoblast migration and is associated with pre-eclampsia. Int J Clin Exp Pathol. 2017;10(10):10544–51.
Tantbirojn P, Crum CP, Parast MM. Pathophysiology of placenta creta: the role of decidua and extravillous trophoblast. Placenta. 2008;29(7):639–45.
Bolze PA, et al. Formalised consensus of the European Organisation for Treatment of Trophoblastic Diseases on management of gestational trophoblastic diseases. Eur J Cancer. 2015;51(13):1725–31.
Smith JM, et al. Are national policies and programs for prevention and management of postpartum hemorrhage and preeclampsia adequate? A key informant survey in 37 countries. Glob Health Sci Pract. 2014;2(3):275–84.
Kaufmann P, Black S, Huppertz B. Endovascular trophoblast invasion: implications for the pathogenesis of intrauterine growth retardation and preeclampsia. Biol Reprod. 2003;69(1):1–7.
Awamleh Z, Gloor GB, Han VKM. Placental microRNAs in pregnancies with early onset intrauterine growth restriction and preeclampsia: potential impact on gene expression and pathophysiology. BMC Med Genomics. 2019;12(1):91.
Nadiminty N, et al. Microarray analysis reveals potential target genes of NF-kappaB2/p52 in LNCaP prostate cancer cells. Prostate. 2010;70(3):276–87.
Paysan L, et al. Rnd3 in cancer: a review of the evidence for tumor promoter or suppressor. Mol Cancer Res. 2016;14(11):1033–44.
Bektic J, et al. Small G-protein RhoE is underexpressed in prostate cancer and induces cell cycle arrest and apoptosis. Prostate. 2005;64(4):332–40.
Yang Z, et al. Extracellular vesicle-derived microRNA-18b ameliorates preeclampsia by enhancing trophoblast proliferation and migration via Notch2/TIM3/mTORC1 axis. J Cell Mol Med. 2021;25(10):4583–95.
Chang CW, Wakeland AK, Parast MM. Trophoblast lineage specification, differentiation and their regulation by oxygen tension. J Endocrinol. 2018;236(1):R43-r56.
James JL, Carter AM, Chamley LW. Human placentation from nidation to 5 weeks of gestation. Part I: what do we know about formative placental development following implantation? Placenta. 2012;33(5):327–34.
Pijnenborg R, Vercruysse L, Hanssens M. The uterine spiral arteries in human pregnancy: facts and controversies. Placenta. 2006;27(9–10):939–58.
Reister F, et al. Macrophage-induced apoptosis limits endovascular trophoblast invasion in the uterine wall of preeclamptic women. Lab Invest. 2001;81(8):1143–52.
Hawkins SM, Buchold GM, Matzuk MM. Minireview: The roles of small RNA pathways in reproductive medicine. Mol Endocrinol. 2011;25(8):1257–79.
Renthal NE, et al. miR-200 family and targets, ZEB1 and ZEB2, modulate uterine quiescence and contractility during pregnancy and labor. Proc Natl Acad Sci U S A. 2010;107(48):20828–33.
Williams KC, et al. MicroRNA-200a serves a key role in the decline of progesterone receptor function leading to term and preterm labor. Proc Natl Acad Sci U S A. 2012;109(19):7529–34.
Kumar P, et al. The c-Myc-regulated microRNA-17~92 (miR-17~92) and miR-106a~363 clusters target hCYP19A1 and hGCM1 to inhibit human trophoblast differentiation. Mol Cell Biol. 2013;33(9):1782–96.
Rosenfeld CR, et al. Effect of estradiol-17beta on blood flow to reproductive and nonreproductive tissues in pregnant ewes. Am J Obstet Gynecol. 1976;124(6):618–29.
Jobe SO, et al. Estradiol-17beta and its cytochrome P450- and catechol-O-methyltransferase-derived metabolites stimulate proliferation in uterine artery endothelial cells: role of estrogen receptor-alpha versus estrogen receptor-beta. Hypertension. 2010;55(4):1005–11.
Kanasaki K, et al. Deficiency in catechol-O-methyltransferase and 2-methoxyoestradiol is associated with pre-eclampsia. Nature. 2008;453(7198):1117–21.
Crocker IP, et al. Differences in apoptotic susceptibility of cytotrophoblasts and syncytiotrophoblasts in normal pregnancy to those complicated with preeclampsia and intrauterine growth restriction. Am J Pathol. 2003;162(2):637–43.
Wu D, et al. Hypoxia-induced microRNA-141 regulates trophoblast apoptosis, invasion, and vascularization by blocking CXCL12β/CXCR2/4 signal transduction. Biomed Pharmacother. 2019;116:108836.
Liu C, et al. MicroRNA-138 targets SP1 to inhibit the proliferation, migration and invasion of hepatocellular carcinoma cells. Oncol Lett. 2018;15(1):1279–86.
Sun DG, et al. The miRNA-29b is downregulated in placenta during gestational diabetes mellitus and may alter placenta development by regulating trophoblast migration and invasion through a HIF3A-dependent mechanism. Front Endocrinol (Lausanne). 2020;11:169.
Guo M, et al. Elevated microRNA-34a contributes to trophoblast cell apoptosis in preeclampsia by targeting BCL-2. J Hum Hypertens. 2017;31(12):815–20.
Kasture V, Sahay A, Joshi S. Cell death mechanisms and their roles in pregnancy related disorders. Adv Protein Chem Struct Biol. 2021;126:195–225.
Lokeswara AW, et al. Preeclampsia: from cellular wellness to inappropriate cell death, and the roles of nutrition. Front Cell Dev Biol. 2021;9:726513.
Xu Y, et al. Let-7i-Induced Atg4B suppression is essential for autophagy of placental trophoblast in preeclampsia. J Cell Physiol. 2017;232(9):2581–9.
Delorme-Axford E, et al. Autophagy as a mechanism of antiviral defense at the maternal-fetal interface. Autophagy. 2013;9(12):2173–4.
Wang Y, et al. Chemotherapy drugs induce pyroptosis through caspase-3 cleavage of a gasdermin. Nature. 2017;547(7661):99–103.
Orning P, et al. Pathogen blockade of TAK1 triggers caspase-8-dependent cleavage of gasdermin D and cell death. Science. 2018;362(6418):1064–9.
Muendlein HI, et al. cFLIP(L) protects macrophages from LPS-induced pyroptosis via inhibition of complex II formation. Science. 2020;367(6484):1379–84.
Park JY, et al. Tendril extract of Cucurbita moschata suppresses NLRP3 inflammasome activation in murine macrophages and human trophoblast cells. Int J Med Sci. 2020;17(8):1006–14.
Liu Z, et al. Melatonin regulates trophoblast pyroptosis, invasion and migration in preeclampsia by inhibiting HtrA1 transcription through the microRNA-520c-3p/SETD7 axis. Am J Reprod Immunol. 2022;87(4):e13523.
Li Y, et al. Ischemia-induced ACSL4 activation contributes to ferroptosis-mediated tissue injury in intestinal ischemia/reperfusion. Cell Death Differ. 2019;26(11):2284–99.
Beharier O, et al. PLA2G6 guards placental trophoblasts against ferroptotic injury. Proc Natl Acad Sci U S A. 2020;117(44):27319–28.
Meihe L, et al. The ferroptosis-NLRP1 inflammasome: the vicious cycle of an adverse pregnancy. Front Cell Dev Biol. 2021;9:707959.
Pringle KG, et al. Beyond oxygen: complex regulation and activity of hypoxia inducible factors in pregnancy. Hum Reprod Update. 2010;16(4):415–31.
Kolahi KS, Valent AM, Thornburg KL. Cytotrophoblast, not syncytiotrophoblast, dominates glycolysis and oxidative phosphorylation in human term placenta. Sci Rep. 2017;7:42941.
Muralimanoharan S, Maloyan A, Myatt L. Mitochondrial function and glucose metabolism in the placenta with gestational diabetes mellitus: role of miR-143. Clin Sci (Lond). 2016;130(11):931–41.
Jiang S, et al. Role of microRNA-130b in placental PGC-1α/TFAM mitochondrial biogenesis pathway. Biochem Biophys Res Commun. 2017;487(3):607–12.
Meng M, et al. Whole genome miRNA profiling revealed miR-199a as potential placental pathogenesis of selective fetal growth restriction in monochorionic twin pregnancies. Placenta. 2020;92:44–53.
Yang W, et al. Increased miRNA-518b inhibits trophoblast migration and angiogenesis by targeting EGR1 in early embryonic arrest†. Biol Reprod. 2019;101(4):664–74.
Herbert SP, Stainier DY. Molecular control of endothelial cell behaviour during blood vessel morphogenesis. Nat Rev Mol Cell Biol. 2011;12(9):551–64.
Nicolau Y, et al. SiRNA silencing of VEGF, IGFs, and their receptors in human retinal microvascular endothelial cells. Am J Transl Res. 2018;10(7):1990–2003.
Li Y, et al. Vascular endothelial growth factor-A (VEGF-A) mediates activin A-induced human trophoblast endothelial-like tube formation. Endocrinol. 2015;156(11):4257–68.
Peng C. The TGF-beta superfamily and its roles in the human ovary and placenta. J Obstet Gynaecol Can. 2003;25(10):834–44.
Marhemati F, et al. Transforming growth factor beta 1 (TGFβ1) polymorphisms and unexplained infertility: a genetic association study. Syst Biol Reprod Med. 2020;66(4):267–80.
Gusar V, et al. MiRNAs regulating oxidative stress: a correlation with Doppler sonography of uteroplacental complex and clinical state assessments of newborns in fetal growth restriction. J Clin Med. 2020;9(10):3227.
Li Y, et al. Roles of TGF-β superfamily proteins in extravillous trophoblast invasion. Trends Endocrinol Metab. 2021;32(3):170–89.
Nadeem L, et al. Nodal signals through activin receptor-like kinase 7 to inhibit trophoblast migration and invasion: implication in the pathogenesis of preeclampsia. Am J Pathol. 2011;178(3):1177–89.
Fu G, et al. MicroRNA-376c impairs transforming growth factor-β and nodal signaling to promote trophoblast cell proliferation and invasion. Hypertension. 2013;61(4):864–72.
Luo L, et al. MicroRNA-378a-5p promotes trophoblast cell survival, migration and invasion by targeting Nodal. J Cell Sci. 2012;125(Pt 13):3124–32.
Massagué J, Chen YG. Controlling TGF-beta signaling. Genes Dev. 2000;14(6):627–44.
Li JY, et al. MiR-140-5p exerts a protective function in pregnancy-induced hypertension via mediating TGF-β/Smad signaling pathway. Hypertens Pregnancy. 2022;41(2):116–25.
Bai Y, et al. Downregulated miR-195 detected in preeclamptic placenta affects trophoblast cell invasion via modulating ActRIIA expression. PLoS ONE. 2012;7(6):e38875.
Wu H, et al. MiR-195 participates in the placental disorder of preeclampsia via targeting activin receptor type-2B in trophoblastic cells. J Hypertens. 2016;34(7):1371–9.
Qiu Q, et al. Both mitogen-activated protein kinase and phosphatidylinositol 3-kinase signalling are required in epidermal growth factor-induced human trophoblast migration. Mol Hum Reprod. 2004;10(9):677–84.
Xia Y, et al. Gene expression network analysis identifies potential targets for prevention of preeclampsia. Int J Gen Med. 2022;15:1023–32.
Yang QE, Giassetti MI, Ealy AD. Fibroblast growth factors activate mitogen-activated protein kinase pathways to promote migration in ovine trophoblast cells. Reproduction. 2011;141(5):707–14.
Li L, et al. miRNA-210-3p regulates trophoblast proliferation and invasiveness through fibroblast growth factor 1 in selective intrauterine growth restriction. J Cell Mol Med. 2019;23(6):4422–33.
Wu S, et al. The miR-410-5p /ITGA6 axis participates in the pathogenesis of recurrent abortion by regulating the biological function of trophoblast. J Reprod Immunol. 2022;152:103647.
Hemmings BA, Restuccia DF. PI3K-PKB/Akt pathway. Cold Spring Harb Perspect Biol. 2012;4(9):a011189.
Tamguney T, Stokoe D. New insights into PTEN. J Cell Sci. 2007;120(Pt 23):4071–9.
Gregorian C, et al. PTEN dosage is essential for neurofibroma development and malignant transformation. Proc Natl Acad Sci U S A. 2009;106(46):19479–84.
Song L, et al. MiR-21 modulates radiosensitivity of cervical cancer through inhibiting autophagy via the PTEN/Akt/HIF-1α feedback loop and the Akt-mTOR signaling pathway. Tumour Biol. 2016;37(9):12161–8.
Wang DD, et al. miR-222 induces adriamycin resistance in breast cancer through PTEN/Akt/p27(kip1) pathway. Tumour Biol. 2016;37(11):15315–24.
Zhu DY, et al. MiR-454 promotes the progression of human non-small cell lung cancer and directly targets PTEN. Biomed Pharmacother. 2016;81:79–85.
Kent LN, et al. FOSL1 is integral to establishing the maternal-fetal interface. Mol Cell Biol. 2011;31(23):4801–13.
Xiao J, et al. miR-144 may regulate the proliferation, migration and invasion of trophoblastic cells through targeting PTEN in preeclampsia. Biomed Pharmacother. 2017;94:341–53.
Isaka K, et al. Expression and activity of matrix metalloproteinase 2 and 9 in human trophoblasts. Placenta. 2003;24(1):53–64.
Staun-Ram E, et al. Expression and importance of matrix metalloproteinase 2 and 9 (MMP-2 and -9) in human trophoblast invasion. Reprod Biol Endocrinol. 2004;2:59.
Zhu J, et al. Dysregulated expression of matrix metalloproteinases and their inhibitors may participate in the pathogenesis of pre-eclampsia and fetal growth restriction. Early Hum Dev. 2014;90(10):657–64.
Anacker J, et al. Human decidua and invasive trophoblasts are rich sources of nearly all human matrix metalloproteinases. Mol Hum Reprod. 2011;17(10):637–52.
Ding J, et al. MiR-519d-3p suppresses invasion and migration of trophoblast cells via targeting MMP-2. PLoS ONE. 2015;10(3):e0120321.
Jin M, et al. MicroRNA-20b inhibits trophoblast cell migration and invasion by targeting MMP-2. Int J Clin Exp Pathol. 2017;10(11):10901–9.
Zeng Y, et al. miR-150-5p mediates extravillous trophoblast cell migration and angiogenesis functions by regulating VEGF and MMP9. Placenta. 2020;93:94–100.
Pollheimer J, et al. Activation of the canonical wingless/T-cell factor signaling pathway promotes invasive differentiation of human trophoblast. Am J Pathol. 2006;168(4):1134–47.
Knöfler M, Pollheimer J. Human placental trophoblast invasion and differentiation: a particular focus on Wnt signaling. Front Genet. 2013;4:190.
Zhao WX, Lin JH. Notch signaling pathway and human placenta. Int J Med Sci. 2012;9(6):447–52.
Haider S, et al. Notch1 controls development of the extravillous trophoblast lineage in the human placenta. Proc Natl Acad Sci U S A. 2016;113(48):E7710-e7719.
Zeng X, et al. EphrinB2-EphB4-RASA1 signaling in human cerebrovascular development and disease. Trends Mol Med. 2019;25(4):265–86.
Dong H, et al. Role of EFNB2/EPHB4 signaling in spiral artery development during pregnancy: an appraisal. Mol Reprod Dev. 2016;83(1):12–8.
Dai Y, et al. MicroRNA-155 inhibits proliferation and migration of human extravillous trophoblast derived HTR-8/SVneo cells via down-regulating cyclin D1. Placenta. 2012;33(10):824–9.
Li X, et al. MicroRNA-155 inhibits migration of trophoblast cells and contributes to the pathogenesis of severe preeclampsia by regulating endothelial nitric oxide synthase. Mol Med Rep. 2014;10(1):550–4.
Siddle K. Signalling by insulin and IGF receptors: supporting acts and new players. J Mol Endocrinol. 2011;47(1):R1-10.
Qiu Q, et al. EGF-induced trophoblast secretion of MMP-9 and TIMP-1 involves activation of both PI3K and MAPK signalling pathways. Reproduction. 2004;128(3):355–63.
Li Y, et al. Activin A increases human trophoblast invasion by inducing SNAIL-mediated MMP2 up-regulation through ALK4. J Clin Endocrinol Metab. 2015;100(11):E1415–27.
Dong L, et al. Circulating CUDR, LSINCT-5 and PTENP1 long noncoding RNAs in sera distinguish patients with gastric cancer from healthy controls. Int J Cancer. 2015;137(5):1128–35.
Yue Y, et al. Sufentanil alleviates pre-eclampsia via silencing microRNA-24-3p to target 11β-hydroxysteroid dehydrogenase type 2. Bioengineered. 2022;13(5):11456–70.
Žarković M, et al. The role of non-coding RNAs in the human placenta. Cells. 2022;11(9):1588.
Tsochandaridis M, et al. Circulating microRNAs as clinical biomarkers in the predictions of pregnancy complications. Biomed Res Int. 2015;2015:294954.
Guglas K, et al. lncRNA in HNSCC: challenges and potential. Contemp Oncol (Pozn). 2017;21(4):259–66.
Yu L, et al. The H19 gene imprinting in normal pregnancy and pre-eclampsia. Placenta. 2009;30(5):443–7.
Lu L, et al. Methylation pattern of H19 exon 1 is closely related to preeclampsia and trophoblast abnormalities. Int J Mol Med. 2014;34(3):765–71.
Tsunoda Y, et al. Expression level of long noncoding RNA H19 of normotensive placentas in late pregnancy relates to the fetal growth restriction. J Obstet Gynaecol Res. 2020;46(7):1025–34.
Mehta P, et al. COVID-19: consider cytokine storm syndromes and immunosuppression. Lancet. 2020;395(10229):1033–4.
Abbas AM, Ahmed OA, Shaltout AS. COVID-19 and maternal pre-eclampsia: a synopsis. Scand J Immunol. 2020;92(3):e12918.
Wang M. The role of IL-37 and IL-38 in obstetrics abnormalities. Front Med (Lausanne). 2021;8:737084.
Donath MY, Shoelson SE. Type 2 diabetes as an inflammatory disease. Nat Rev Immunol. 2011;11(2):98–107.
Jing Y, et al. Potential influence of COVID-19/ACE2 on the female reproductive system. Mol Hum Reprod. 2020;26(6):367–73.
Funding
This study was supported by the Natural Science Foundation of China (No. 81970389) and the Natural Science Foundation of Hunan Province China (Nos. 2021JJ30626, 2022JJ30038, 2022JJ30533) and Scientific Research Project of Hunan Provincial Department of Education (Grant No.18B283).
Author information
Authors and Affiliations
Contributions
ZW conceptualized and designed the original idea. LL performed literature search and analysis and wrote the first draft. YC and CW provided valuable feedback and critically revised the work. LL generated the figures and tables and revised the draft. Supervision was provided by ZC, LX, JM, LH, CY, and ZW. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Lingli Liang, Yanjun Chen, and Chunyan Wu are co-first authors.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liang, L., Chen, Y., Wu, C. et al. MicroRNAs: key regulators of the trophoblast function in pregnancy disorders. J Assist Reprod Genet 40, 3–17 (2023). https://doi.org/10.1007/s10815-022-02677-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-022-02677-9