Abstract
Purpose
Glaucoma is a common chronic neurodegenerative disease, which could lead to visual loss. In this study, we aimed to investigate whether fisetin, a natural flavone with anti-inflammatory and antioxidant properties, is able to alleviate glaucoma.
Methods
We employed a DBA/2J mouse model which was treated with or without fisetin. Pattern electroretinogram (P-ERG), visual evoked potentials (VEPs) and intraocular pressure (IOP) were evaluated. Quantitative real-time polymerase chain reaction and enzyme-linked immunosorbent assay (ELISA) were used to measure the expression levels of TNF-α, IL-1β and IL-6. Western blotting was performed to assess the activation of nuclear factor kappa-B (NF-κB).
Results
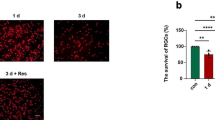
We found that DBA/2J mice treated with fisetin (10-30 mg/kg) showed improved P-ERG and VEP amplitudes and reduced IOP compared to untreated DBA/2J mice. In addition, there were more survived retinal ganglion cells (RGCs) and less activated microglia in fisetin-treated DBA/2J mice than those in untreated mice. Furthermore, secreted protein levels and mRNA levels of TNF-α, IL-1β and IL-6 were significantly repressed by fisetin. The phosphorylated p65 level in the nucleus was dramatically reduced in fisetin-treated mice compared to it in untreated mice. Our results demonstrate that fisetin may exert its function through regulating cytokine productions and inhibiting NF-κB activation in the retina.
Conclusion
In conclusion, fisetin is able to promote the visual functions of DBA/2J mice by inhibiting NF-κB activation.






Similar content being viewed by others
Change history
15 November 2019
The Editor-in-Chief of Documenta Ophthalmologica is publishing an editorial expression of concern for the manuscript "Fisetin rescues retinal functions by suppressing inflammatory response in a DBA/2J mouse model of glaucoma” by Li et al. (2019) [1].
References
Quigley HA, Broman AT (2006) The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol 90:262–267. https://doi.org/10.1136/bjo.2005.081224
Nuschke AC, Farrell SR, Levesque JM, Chauhan BC (2015) Assessment of retinal ganglion cell damage in glaucomatous optic neuropathy: axon transport, injury and soma loss. Exp Eye Res 141:111–124. https://doi.org/10.1016/j.exer.2015.06.006
Howell GR, Macalinao DG, Sousa GL, Walden M, Soto I, Kneeland SC, Barbay JM, King BL, Marchant JK, Hibbs M, Stevens B, Barres BA, Clark AF, Libby RT, John SWM (2011) Molecular clustering identifies complement and endothelin induction as early events in a mouse model of glaucoma. J Clin Investig 121:1429–1444. https://doi.org/10.1172/Jci44646
Nickells RW, Howell GR, Soto I, John SWM (2012) Under pressure: cellular and molecular responses during glaucoma, a common neurodegeneration with axonopathy. Annu Rev Neurosci 35(35):153–179. https://doi.org/10.1146/annurev.neuro.051508.135728
Foster PJ, Buhrmann R, Quigley HA, Johnson GJ (2002) The definition and classification of glaucoma in prevalence surveys. Br J Ophthalmol 86:238–242. https://doi.org/10.1136/bjo.86.2.238
Wax MB, Tezel G, Yang J, Peng G, Patil RV, Agarwal N, Sappington RM, Calkins DJ (2008) Induced autoimmunity to heat shock proteins elicits glaucomatous loss of retinal ganglion cell neurons via activated T-cell-derived fas-ligand. J Neurosci 28:12085–12096. https://doi.org/10.1523/Jneurosci.3200-08.2008
Tezel G, Thornton IL, Tong MG, Luo C, Yang XJ, Cai J, Powell DW, Soltau JB, Liebmann JM, Ritch R (2012) Immunoproteomic analysis of potential serum biomarker candidates in human glaucoma. Invest Ophthalmol Vis Sci 53:8222–8231. https://doi.org/10.1167/iovs.12-10076
Tatton W, Chen D, Chalmers-Redman R, Wheeler L, Nixon R, Tatton N (2003) Hypothesis for a common basis for neuroprotection in glaucoma and Alzheimer’s disease: anti-apoptosis by alpha-2-adrenergic receptor activation. Surv Ophthalmol 48:S25–S37. https://doi.org/10.1016/S0039-6257(03)00005-5
Crish SD, Sappington RM, Inman DM, Horner PJ, Calkins DJ (2010) Distal axonopathy with structural persistence in glaucomatous neurodegeneration. Proc Natl Acad Sci USA 107:5196–5201. https://doi.org/10.1073/pnas.0913141107
Murphy JA, Clarke DB (2006) Target-derived neurotrophins may influence the survival of adult retinal ganglion cells when local neurotrophic support is disrupted: implications for glaucoma. Med Hypotheses 67:1208–1212. https://doi.org/10.1016/j.mehy.2006.04.049
Zhang HF, Lin Y, Li JH, Pober JS, Min W (2007) RIP1-mediated AIP1 phosphorylation at a 14-3-3-binding site is critical for tumor necrosis factor-induced ASK1-JNK/p38 activation. J Biol Chem 282:14788–14796
Wax MB, Tezel G (2009) Immunoregulation of retinal ganglion cell fate in glaucoma. Exp Eye Res 88:825–830. https://doi.org/10.1016/j.exer.2009.02.005
Nakazawa T, Nakazawa C, Matsubara A, Noda K, Hisatomi T, She HC, Michaud N, Hafezi-Moghadam A, Miller JW, Benowitz LI (2006) Tumor necrosis factor-alpha mediates oligodendrocyte death and delayed retinal ganglion cell loss in a mouse model of glaucoma. J Neurosci 26:12633–12641. https://doi.org/10.1523/Jneurosci.2801-06.2006
Lebrun-Julien F, Bertrand MJ, De Backer O, Stellwagen D, Morales CR, Di Polo A, Barker PA (2010) ProNGF induces TNFα-dependent death of retinal ganglion cells through a p75NTR non-cell-autonomous signaling pathway. Proc Natl Acad Sci 107:3817–3822
Funayama T, Ishikawa K, Ohtake Y, Tanino T, Kurosaka D, Kimura I, Suzuki K, Ideta H, Nakamoto K, Yasuda N, Fujimaki T, Murakami A, Asaoka R, Hotta Y, Tanihara H, Kanamoto T, Mishima H, Fukuchi T, Abe H, Iwata T, Shimada N, Kudoh J, Shimizu N, Mashima Y (2004) Variants in optineurin gene and their association with tumor necrosis factor-alpha polymorphisms in Japanese patients with glaucoma. Invest Ophthalmol Vis Sci 45:4359–4367. https://doi.org/10.1167/iovs.03-1403
Pal HC, Athar M, Elmets CA, Afaq F (2015) Fisetin inhibits UVB-induced cutaneous inflammation and activation of PI3 K/AKT/NFκB signaling pathways in SKH-1 hairless mice. Photochem Photobiol 91:225–234
Kim SC, Kang SH, Jeong SJ, Kim SH, Ko HS, Kim SH (2012) Inhibition of c-Jun N-terminal kinase and nuclear factor kappa B pathways mediates fisetin-exerted anti-inflammatory activity in lipopolysaccharide-treated RAW264.7 cells. Immunopharmacol Immunotoxicol 34:645–650. https://doi.org/10.3109/08923973.2011.648270
Chuang JY, Chang PC, Shen YC, Lin CJ, Tsai CF, Chen JH, Yeh WL, Wu LH, Lin HY, Liu YS, Lu DY (2014) Regulatory effects of fisetin on microglial activation. Molecules 19:8820–8839. https://doi.org/10.3390/molecules19078820
Lee JD, Huh JE, Jeon G, Yang HR, Woo HS, Choi DY, Park DS (2009) Flavonol-rich RVHxR from Rhus verniciflua Stokes and its major compound fisetin inhibits inflammation-related cytokines and angiogenic factor in rheumatoid arthritic fibroblast-like synovial cells and in vivo models. Int Immunopharmacol 9:268–276. https://doi.org/10.1016/j.intimp.2008.11.005
Goh FY, Upton N, Guan S, Cheng C, Shanmugam MK, Sethi G, Leung BP, Wong WF (2012) Fisetin, a bioactive flavonol, attenuates allergic airway inflammation through negative regulation of NF-κB. Eur J Pharmacol 679:109–116
Porciatti V, Saleh M, Nagaraju M (2007) The pattern electroretinogram as a tool to monitor progressive retinal ganglion cell dysfunction in the DBA/2J mouse model of glaucoma. Invest Ophthalmol Vis Sci 48:745–751. https://doi.org/10.1167/iovs.06-0733
Gustafson E, Silberschmidt A, Esguerra M, Miller R (2013) Recording and manipulation of the pattern electroretinogram in a mouse eyecup preparation. Investig Ophthalmol Vis Sci 54:6132
Nadal-Nicolas FM, Jimenez-Lopez M, Salinas-Navarro M, Sobrado-Calvo P, Alburquerque-Bejar JJ, Vidal-Sanz M, Agudo-Barriuso M (2012) Whole number, distribution and co-expression of Brn3 transcription factors in retinal ganglion cells of adult albino and pigmented rats. PLoS ONE 7:e49830. https://doi.org/10.1371/journal.pone.0049830
Libby RT, Gould DB, Anderson MG, John SWM (2005) Complex genetics of glaucoma susceptibility. Annu Rev Genom Hum Genet 6:15–44. https://doi.org/10.1146/annurev.genom.6.080604.162209
Anderson MG, Libby RT, Mao M, Cosma IM, Wilson LA, Smith RS, John SWM (2006) Genetic context determines susceptibility to intraocular pressure elevation in a mouse pigmentary glaucoma. BMC Biol 4:20. https://doi.org/10.1186/1741-7007-4-20
Libby RT, Li Y, Savinova OV, Barter J, Smith RS, Nickells RW, John SWM (2005) Susceptibility to neurodegeneration in a glaucoma is modified by Bax gene dosage. PLoS Genet 1:17–26. https://doi.org/10.1371/journal.pgen.0010004
Reichstein D, Ren LZ, Filippopoulos T, Mittag T, Danias J (2007) Apoptotic retinal ganglion cell death in the DBA/2 mouse model of glaucoma. Exp Eye Res 84:13–21. https://doi.org/10.1016/j.exer.2006.08.009
Bosco A, Inman DM, Steele MR, Wu GM, Soto I, Marsh-Armstrong N, Hubbard WC, Calkins DJ, Horner PJ, Vetter ML (2008) Reduced retina microglial activation and improved optic nerve integrity with minocycline treatment in the DBA/2J mouse model of glaucoma. Invest Ophthalmol Vis Sci 49:1437–1446. https://doi.org/10.1167/iovs.07-1337
Neufeld AH (1999) Microglia in the optic nerve head and the region of parapapillary chorioretinal atrophy in glaucoma. Arch Ophthalmol 117:1050–1056
Son JL, Soto I, Oglesby E, Lopez-Roca T, Pease ME, Quigley HA, Marsh-Armstrong N (2010) Glaucomatous optic nerve injury involves early astrocyte reactivity and late oligodendrocyte loss. Glia 58:780–789. https://doi.org/10.1002/glia.20962
Neufeld AH, Liu B (2003) Glaucomatous optic neuropathy: when glia misbehave. Neurosci 9:485–495
Sobrado-Calvo P, Vidal-Sanz M, Villegas-Pérez MP (2007) Rat retinal microglial cells under normal conditions, after optic nerve section, and after optic nerve section and intravitreal injection of trophic factors or macrophage inhibitory factor. J Comp Neurol 501:866–878
Karlstetter M, Ebert S, Langmann T (2010) Microglia in the healthy and degenerating retina: insights from novel mouse models. Immunobiology 215:685–691. https://doi.org/10.1016/j.imbio.2010.05.010
Tezel G, Yang XJ, Yang JJ, Wax MB (2004) Role of tumor necrosis factor receptor-1 in the death of retinal ganglion cells following optic nerve crush injury in mice. Brain Res 996:202–212. https://doi.org/10.1016/j.brainres.2003.10.029
Al-Gayyar M, Elsherbiny N (2013) Contribution of TNF-α to the development of retinal neurodegenerative disorders. Eur Cytokine Netw 24:27–36
Balaiya S, Edwards J, Tillis T, Khetpal V, Chalam KV (2011) Tumor necrosis factor-alpha (TNF-α) levels in aqueous humor of primary open angle glaucoma. Clin Ophthalmol 5:553
Tezel G (2008) TNF-α signaling in glaucomatous neurodegeneration. Prog Brain Res 173:409–421
Wilson GN, Inman DM, Dengler-Crish CM, Smith MA, Crish SD (2015) Early pro-inflammatory cytokine elevations in the DBA/2J mouse model of glaucoma. J Neuroinflammation 12:176
H-l Peng, Huang W-C, S-c Cheng, Liou C-J (2018) Fisetin inhibits the generation of inflammatory mediators in interleukin-1β–induced human lung epithelial cells by suppressing the Nf-κb and Erk1/2 pathways. Int Immunopharmacol 60:202–210
Sahu BD, Kumar JM, Sistla R (2016) Fisetin, a dietary flavonoid, ameliorates experimental colitis in mice: relevance of NF-κB signaling. J Nutr Biochem 28:171–182
Seo S-H, Jeong G-S (2015) Fisetin inhibits TNF-α-induced inflammatory action and hydrogen peroxide-induced oxidative damage in human keratinocyte HaCaT cells through PI3 K/AKT/Nrf-2-mediated heme oxygenase-1 expression. Int Immunopharmacol 29:246–253
Mookherjee S, Banerjee D, Chakraborty S, Banerjee A, Mukhopadhyay I, Sen A, Ray K (2010) Association of IL1A and IL1B loci with primary open angle glaucoma. BMC Med Genet 11:99. https://doi.org/10.1186/1471-2350-11-99
Chidlow G, Wood JPM, Ebneter A, Casson RJ (2012) Interleukin-6 is an efficacious marker of axonal transport disruption during experimental glaucoma and stimulates neuritogenesis in cultured retinal ganglion cells. Neurobiol Dis 48:568–581. https://doi.org/10.1016/j.nbd.2012.07.026
Li GR, Luna C, Liton PB, Navarro I, Epstein DL, Gonzalez P (2007) Sustained stress response after oxidative stress in trabecular meshwork cells. Mol Vis 13:2282–2288
Lebrun-Julien F, Duplan L, Pernet V, Osswald I, Sapieha P, Bourgeois P, Dickson K, Bowie D, Barker PA, Di Polo A (2009) Excitotoxic death of retinal neurons in vivo occurs via a non-cell-autonomous mechanism. J Neurosci 29:5536–5545. https://doi.org/10.1523/Jneurosci.0831-09.2009
Chen C, Yao L, Cui J, Liu B (2018) Fisetin protects against intracerebral hemorrhage-induced neuroinflammation in aged mice. Cerebrovasc Dis 45:154–161. https://doi.org/10.1159/000488117
Sandireddy R, Yerra VG, Komirishetti P, Areti A, Kumar A (2016) Fisetin imparts neuroprotection in experimental diabetic neuropathy by modulating Nrf2 and NF-κB pathways. Cell Mol Neurobiol 36:883–892
Feng G, Z-y Jiang, Sun B, Fu J, T-z Li (2016) Fisetin alleviates lipopolysaccharide-induced acute lung injury via TLR4-mediated NF-κB signaling pathway in rats. Inflammation 39:148–157
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving animal were in accordance with the ethical standards of the institutional and/or national research committee. Animal studies were approved by the People’s Hospital of Rizhao, and all efforts were made to minimize the number of animals used and their suffering.
Statements of human rights
There is no human participation in this study.
Statement on the welfare of animals
All animal experiments were conducted according to the guidelines in our institute and all efforts were made to minimize the nubmer of animals used and their suffering.
Informed consent
Not applicable. There is no human participation in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, L., Qin, J., Fu, T. et al. Fisetin rescues retinal functions by suppressing inflammatory response in a DBA/2J mouse model of glaucoma. Doc Ophthalmol 138, 125–135 (2019). https://doi.org/10.1007/s10633-019-09676-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10633-019-09676-9