Abstract
Comorbidities among US patients with ankylosing spondylitis (AS) are inadequately understood. This study compared the prevalence and incidence of comorbidities between patients with AS and matched controls using national claims databases. Adults enrolled in the MarketScan Commercial and Medicare databases with ≥ 1 inpatient or ≥ 2 non-rule-out outpatient diagnoses of AS between January 1, 2012 and December 31, 2014 were included. Patients had to have ≥ 1 AS diagnosis in 2013; the first AS diagnosis in 2013 was assigned as the index date. Control patients without AS were matched to AS patients on age, geographic region, index calendar year, and sex. Comorbidities were evaluated in AS patients and matched controls during the baseline and follow-up periods (before and after the index date, respectively). Hazard ratios of developing new comorbidities were estimated using Cox proportional hazard models adjusted for patients’ characteristics. A total of 6679 patients with AS were matched to 19,951 control patients. In addition to extra-articular manifestations of AS (inflammatory bowel disease [IBD], psoriasis, uveitis), a higher proportion of AS patients had asthma, cardiovascular disease, depression, dyslipidemia, gastrointestinal ulcers, malignancies, multiple sclerosis, osteoporosis, sleep apnea, and spinal fractures during the baseline period than matched controls. After AS diagnosis, a higher proportion of patients developed newly diagnosed cases of cardiovascular diseases, depression, osteoporosis, spinal fracture, IBD, psoriasis, and uveitis than matched controls. In this real-world, US claims-based study, patients with AS were shown to have significantly more comorbidities than matched controls.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ankylosing spondylitis (AS) is a systemic inflammatory disorder affecting the axial skeleton, peripheral joints, entheses, eyes, skin, and intestines [1,2,3,4,5]. Affecting 0.1 to 1% of the US general population, AS occurs more frequently in men, with a higher prevalence in whites [6,7,8]. The age of onset is typically the late teens through around 40 years. Onset after 50 years of age is unusual; however, delays in diagnosis are known to occur by as much as 8 to 11 years in some individuals [9,10,11].
Patients with AS often have extra-articular manifestations of AS, such as inflammatory bowel disease (IBD; Crohn disease and ulcerative colitis), psoriasis, and uveitis. Several studies, mostly conducted outside the USA, have also shown that patients with AS are at a higher risk of developing hypertension, hyperlipidemia, diabetes, peptic ulcers, headaches, depression, cancer, osteoporosis, and other cardiovascular, pulmonary, renal, and neurological complications compared with the general population [12,13,14,15,16,17,18,19,20,21,22,23,24]. Currently, there are a limited number of studies examining comorbidities in patients with AS in the USA. As rates of comorbidities in the general population are known to differ between the USA and other countries (e.g., obesity, diabetes, smoking), it is unknown if these differences affect comorbidity risk between patients with AS in the USA and those from other countries. This study aimed to examine the real-world comorbidity burden in US patients with AS using large national healthcare claims data and to compare comorbidities in patients with AS with matched control patients without AS.
Methods
Study design and data sources
This retrospective, observational cohort study used medical and pharmacy claims from January 1, 2012 through June 30, 2015, from two large administrative claims databases, the MarketScan® Commercial Claims and Encounters (Commercial) database and the Medicare Supplemental (Medicare) database. These databases include complete longitudinal records of inpatient services, outpatient services, long-term care, and prescription drug claims for commercially insured and Medicare-eligible patients covered under a variety of health plans from patients’ current or former employers. All database records are deidentified in full compliance with US patient confidentiality requirements set forth in the Health Insurance Portability and Accountability Act. Because this study used only deidentified patient records and did not involve the collection, use, or transmittal of individually identifiable data, institutional review board approval to conduct this study was not necessary.
Patient selection
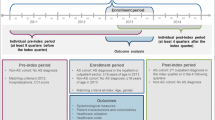
This study included patients aged ≥ 18 years with ≥ 1 inpatient or ≥ 2 non-rule-out outpatient medical claims for AS (International Classification of Diseases, Ninth Revision, Clinical Modification [ICD-9-CM] diagnosis code 720.0) > 30 days apart but within ≤ 365 days of each other between January 1, 2012 and December 31, 2014. Non-rule-out claims were those not related to a diagnostic or rule-out procedure (e.g., laboratory, pathology, or radiology services). Patients with AS were required to have ≥ 1 diagnosis of AS during 2013; the index date was the date of the first observed AS diagnosis in 2013. The year 2013 was chosen because of the availability of medical and pharmacy claims data at the time of analysis. Continuous enrollment with medical and pharmacy benefits for at least 12 months before the index date (baseline period) and 12 months after the index date (follow-up period) was required.
Patients with AS were matched to control patients without AS (general population) at a ratio of up to 5:1 based on age, geographic location, index calendar year, and sex. These matched controls had the same inclusion requirements as the patients with AS except for the diagnosis of AS. Matched controls were assigned the same index dates of their matched patients with AS.
All patients had a variable length follow-up period of ≥ 12 months until the earliest occurrence of inpatient death, end of continuous enrollment, or end of the data availability (June 30, 2015).
Study variables
Patient demographics, including age, sex, geographic region, type of health plan, and duration of follow-up, were recorded on the index date. Comorbidities were identified using diagnosis codes in medical claims, but claims for diagnostic or rule-out procedures (e.g., laboratory, pathology, or radiology services) were excluded to avoid incorrectly identifying patients as having a comorbidity based on the history of testing rather than the test results. The following comorbidities were recorded during the baseline and follow-up periods: cardiovascular conditions (angina, atherosclerosis, cerebrovascular disease/stroke, coronary artery disease, hypertension, myocardial infarction, peripheral vascular disease, venous thromboembolism), IBD (Crohn disease, ulcerative colitis), gastrointestinal ulcers (esophageal, gastric, duodenal, peptic, and gastrojejunal ulcers), malignant neoplasms (malignant solid tumors, hematologic malignancies, and neuroendocrine tumors), asthma, depression, diabetes mellitus, dyslipidemia, multiple sclerosis, osteoporosis, Parkinson disease, psoriasis, sleep apnea, spinal fracture, and uveitis. Deyo-Charlson Comorbidity Index scores were calculated based on the presence of comorbidities during the baseline period. The ICD-9-CM codes used for these conditions are available upon request.
A comorbidity was considered to be newly diagnosed if the diagnosis code for this comorbidity was observed in the follow-up period but not in the baseline period. The incidence rates of comorbidities per 100 patient-years (PY) were calculated for patients with AS and their matched controls during the follow-up period. The incidence rate was calculated as ([number of patients with specific comorbidity/total observation days]/365) × 100. The total number of observation days was accumulated from the index date to the date of the first observed comorbidity for patients who developed a new comorbidity and the entire follow-up period for patients who did not develop a new comorbidity. Patients with comorbidities recorded in the baseline period were excluded from the incidence rate calculation.
Statistical analysis
Bivariate descriptive analyses were conducted on all study variables comparing patients with AS and matched controls. Categorical variables were presented as counts and percentages; continuous variables were summarized with means and standard deviations. When appropriate, the statistical significance of cohort differences in bivariate descriptive statistics used χ2 tests for categorical variables and t tests for differences in continuous variables. The threshold for statistical significance was set a priori to the P value of 0.05.
Hazard ratios (HRs) were estimated using Cox proportional hazard models to assess the difference in the risk of developing a comorbidity between patients with AS and matched controls, overall and stratified by age (< 45 years, ≥ 45 to < 65 years, and ≥ 65 years); HRs were also estimated to assess the difference in the risk of developing a comorbidity between male and female patients with AS. HRs were adjusted for patients’ demographic characteristics (age, sex, health plan type, urban/rural residence, region, index year) and baseline clinical characteristics (Deyo-Charlson comorbidity index, cardiovascular disease, gastrointestinal disorders, malignancies, metabolic syndrome, neurological or psychological conditions, respiratory disease, osteoporosis, uveitis). The threshold for statistical significance was set a priori at 0.05. All analyses were conducted using SAS version 9.4 (SAS Institute Inc.).
Results
A total of 46,265 patients aged ≥ 18 years with ≥ 1 inpatient claim or ≥ 2 outpatient medical claims for AS > 30 days and ≤ 365 days apart were identified between January 1, 2012 and December 31, 2014, in the MarketScan Commercial and Medicare databases. A total of 6834 patients met the criteria for the AS cohort, and 6679 were matched with 19,951 patients without AS (Fig. 1). Patients with AS had a mean (SD) age of 50.8 (13.6) years, and 60.5% were men; matched controls had a mean age of 51.7 (13.4) years, and 60.8% were men. The SD length of follow-up in patients with AS and in matched controls was 739 (139) days and 740 (139) days, respectively (Table 1).
Selection of study cohorts. AS, ankylosing spondylitis. Non–rule-out claims were those not related to a diagnostic or rule-out procedure (e.g., laboratory, pathology, or radiology services). The index date was the date of the first AS diagnosis. Matched controls were assigned the same index date as their matched patient with AS
Patients with AS were shown to have a higher comorbidity burden than matched controls as evidenced by their higher Deyo-Charlson Comorbidity Index score in the baseline period (0.61 [1.15] vs 0.50 [1.14], P < 0.001). In addition, a significantly higher proportion of patients with AS were diagnosed with asthma, cardiovascular diseases, depression, dyslipidemia, gastrointestinal ulcers, malignancies, multiple sclerosis, osteoporosis, sleep apnea, spinal fracture, IBD, psoriasis, and uveitis than matched controls (Table 2). The proportion of patients with peripheral vascular disease, diabetes, and Parkinson disease was similar between patients with AS and matched controls.
Except for diabetes, dyslipidemia, and Parkinson disease, patients with AS had significantly higher incidence rates of all other comorbidities compared with matched controls (Table 3 and Fig. 2). Comorbidities with the highest incidence rates were hypertension, dyslipidemia, and depression (patients with AS—12.98, 13.52, and 6.05 per 100 PYs, respectively; matched controls—10.33, 12.90, and 3.22 per 100 PYs, respectively). The greatest differences in incidence rates were observed in IBD and uveitis; the incidence rates for IBD and uveitis were 8 and 26 times higher, respectively, in patients with AS compared with matched controls. Patients with AS had three to four times higher incidence rates of multiple sclerosis, osteoporosis, and spinal fracture, and approximately two times higher incidence rates of asthma, depression, gastrointestinal ulcers, sleep apnea, and venous thromboembolism, compared with matched controls.
After controlling for patients’ demographic and baseline clinical characteristics, multivariate analyses showed that patients with AS had a significantly higher risk of developing asthma, cardiovascular disease, depression, hypertension, malignancies, osteoporosis, sleep apnea, spinal fracture, IBD (including both Crohn disease and ulcerative colitis) psoriasis, and uveitis compared with matched controls (Table 4). Increased risk of developing cardiovascular disease, depression, hypertension, osteoporosis, spinal fracture, IBD (including Crohn disease), and uveitis in patients with AS were consistent across different age groups (< 45 years, ≥ 45 to < 65 years, and ≥ 65 years). Patients with AS had an increased risk of developing sleep apnea compared with matched controls at all ages except < 45 years of age and had an increased risk of developing malignancies if they were < 65 years of age. Among patients with AS, women were shown to have an increased risk of developing asthma, depression, and osteoporosis compared with men; men were shown to have increased risk of developing cardiovascular disease, dyslipidemia, hypertension, malignancies, sleep apnea, and spinal fracture compared with women.
Discussion
This study demonstrated that in this population of patients with either incident or prevalent AS, a greater proportion of patients with AS had baseline comorbidities compared with matched controls. In addition to a higher rate of extra-articular manifestations of AS (IBD, psoriasis, and uveitis), patients with AS also had significantly higher rates of asthma, cardiovascular disease (including angina, atherosclerosis, cerebrovascular disease/stroke, coronary artery disease, hypertension, myocardial infarction, and venous thromboembolism), depression, gastrointestinal ulcers, osteoporosis, sleep apnea, and spinal fracture. The higher baseline comorbidity burden in patients with AS than in the matched controls is consistent with results from prior studies, with the exception of diabetes, for which rates were found to be statistically similar between patients with AS and matched controls [12,13,14,15,16,17,18,19,20,21]. Although the reasons for this particular lack of association are unclear, the higher prevalence of diabetes in the USA (10.8% of population of ages 20 to 79) than some of the other countries where published AS studies were conducted (e.g., Sweden, 4.7%; China, 9.8%; Japan, 5.7%; Spain, 7.7%) may have obscured the difference in rates of diabetes between patients with AS and matched controls in this study [25]. While the association of AS with cardiovascular disease, IBD, depression, osteoporosis, and uveitis has been well studied, the association of AS with higher rates of sleep apnea, asthma, and malignancies is less established, and additional research is required to further characterize these comorbidities in AS populations.
Although the prevalence of psoriasis at baseline and the incidence of new cases of psoriasis were higher in patients with AS than in matched controls, the overall risk of newly diagnosed psoriasis was lower than expected. We suspect that, in this patient population, psoriasis was diagnosed before the diagnosis of AS, thus making it less likely to be identified as a new comorbidity.
In our study, patients with AS had an increased risk of developing asthma, which is consistent with results of a previous study showing an overall increased risk of asthma in patients with AS compared with the general population; our results are also consistent with the observation of a higher risk of asthma for women with AS than men with AS, with the highest risk being in patients 30 to 49 years of age [26]. This increased risk in younger adults observed in both studies may be due to older patients in general being more likely to already have asthma [27]. The higher rate of asthma in women with AS is likely related to the increased incidence of nonallergic asthma or adult-onset asthma in women overall [27, 28].
Patients with AS in our study were more likely than matched controls to develop malignancies. Previous studies have shown that patients with AS have an increased risk of developing cancer [18, 29]. In addition, a recent systematic review and meta-analysis showed an overall increased risk for malignancy in patients with AS; however, subgroup analyses did not confirm the association to be significant in American or European populations with an increased risk for malignancy of the digestive system, multiple myeloma, and lymphoma [30].
Previous studies have established that patients with AS have an increased risk of spinal fractures, and these fractures can be caused by minimal trauma [31,32,33,34]. Our study also showed that patients with AS had a higher risk of spinal fractures compared with matched controls, and the risk was higher in men with AS than women with AS. Remodeling, fusion, and osteoporosis likely contribute to the increased susceptibility to spinal fractures. Although women in our study had a higher rate of osteoporosis, a previous study has shown that men with AS have more severe radiographic damage than women with AS, which may contribute to the increased risk of spinal fracture in men vs women [35].
This study expanded on evidence from prior studies showing an increased incidence of sleep apnea in patients with AS [36,37,38]. Systemic inflammation has been theorized to contribute to the increased incidence of sleep apnea in patients with AS [36]. Tumor necrosis factor α levels are increased in sleep apnea independent of obesity [39]; however, the literature shows conflicting results on the effect of tumor necrosis factor inhibitors on sleep apnea [36, 40, 41]. In the current study, the risk of sleep apnea was significantly increased in patients with AS aged ≥ 45 years vs matched controls aged ≥ 45 years. Although the risk was also increased in patients with AS vs matched controls aged < 45 years, this difference was not significant.
These findings also support evidence from other published reports on the risk of developing new comorbidities in patients with AS, especially for cardiovascular diseases and depression [15, 17, 20, 42]. The results of this current study are consistent with those from the Swedish National Patient Register, which showed a 50% higher risk of acute coronary syndrome and vascular thromboembolism and a 25% higher risk of stroke in patients with AS compared with the general population [42]. In addition, a study using administrative claims data from the Taiwan National Health Insurance Database showed a > 2-fold increase in the risk of stroke in patients with AS vs a comparison cohort without AS [20]. The percentage of patients with AS newly diagnosed with depression in our study was similar to data from the Skåne Healthcare Register in Sweden, which showed an 80% increased rate of doctor-diagnosed depression in women with AS and a 50% increase in men with AS compared with age- and sex-specific rates of depression in the general population seeking care [17]. Studies of newly diagnosed osteoporosis in patients with AS are lacking, but a systematic literature review of the prevalence of low bone-mineral density found a high overall prevalence of decreased bone density (> 50%) and osteoporosis (13–16%) in patients with newly diagnosed AS (disease duration, < 10 years) [43]. In addition, a cross-sectional analysis of bone-mineral density measurements from 504 Chinese patients with AS showed a higher prevalence of osteoporosis (9.7 vs 0.0%) and osteopenia (57.5 vs 34.9%) compared with matched controls [44]. Although previous studies have shown the increased risk of comorbidities in patients with AS, all these studies were conducted outside of the USA. Our study provides new information and contributes to the existing knowledge about the increased risk of comorbidities in patients with AS and provides important real-world evidence from a US patient population.
This study did not examine the causality of the association between AS and comorbidities. A potential explanation is that patients have shared genetic or environmental risk factors that predispose them to both AS and to the comorbidities. Other possibilities are that AS may increase the risk of the evaluated comorbidities or that AS may be a marker for or consequence of unidentified risk factors that contribute to the risk of both AS and the comorbidities. The higher rates of baseline comorbidities in patients with AS may be evidence of interrelated disease processes or may be associated with treatment; however, associations with treatments were not tested as a part of this research.
The mean age of patients in the study was older than what has been reported in other studies of patients with AS. The patient population in this study included both incident and prevalent AS patients, and the older age may also be due to the inclusion criteria, which required continuous enrollment in an insurance plan for 12 months before and after the index date. Younger patients are more likely to switch jobs and subsequently switch insurance carriers more often [45]. In addition, younger patients may be less likely to have regular visits with healthcare providers, thus having fewer opportunities for a diagnosis of AS or a comorbidity.
Limitations
The limitations of this study are those inherent to any retrospective database analysis. First, in the absence of patient charts or provider attestations, misclassification error is possible when relying on diagnosis coding from administrative claims data, where the extent of under- or overcoding for AS and comorbidities is unknown. In addition, because of the lack of data on body mass index, we were unable to evaluate obesity as a comorbidity or to control for obesity with related comorbidities such as diabetes, sleep apnea, and cardiovascular diseases. Further, we did not evaluate other risk factors that could contribute to the development of comorbidities (e.g., smoking, alcohol consumption, and use of other medications such as nonsteroidal anti-inflammatory drugs). Second, due to the large cohort sizes, small differences between comparator groups may be found to be statistically significant, even though the corresponding interpretation of clinical significance may be questionable. Third, patients with AS may visit healthcare providers more often than matched controls and thus may have more opportunities to be diagnosed with comorbidities. This potential difference in opportunities for diagnosis may result in overestimation of the difference in comorbidity rates between patients with AS and matched controls. Finally, the MarketScan administrative claims databases are convenience samples of individuals, employees, retirees, and their dependents in the USA who had commercial health insurance or Medicare supplemented by other health insurance paid for by a current or former employer; therefore, the results may not be applicable outside of this demographic.
Conclusion
In this real-world, US claims-based study, patients with AS were shown to have significantly more comorbidities than matched controls. Understanding the frequency and risk for these diseases can assist providers with comorbidity screening and patient-management strategies. Furthermore, knowledge of comorbidity risks improves understanding of long-term health prognoses. Use of comprehensive longitudinal real-world data is a promising tool to evaluate the burden of comorbidities in patients with AS. Further research is needed to examine the potential cause and effect relationships between AS and comorbidities.
References
Reveille JD (2006) The genetic basis of ankylosing spondylitis. Curr Opin Rheumatol 18:332–341
Brionez TF, Reveille JD (2008) The contribution of genes outside the major histocompatibility complex to susceptibility to ankylosing spondylitis. Curr Opin Rheumatol 20:384–391
Hanson JA, Mirza S (2000) Predisposition for spinal fracture in ankylosing spondylitis. AJR Am J Roentgenol 174:150
Hunter T (1989) The spinal complications of ankylosing spondylitis. Semin Arthritis Rheum 19:172–182
Sutherland RI, Matheson D (1975) Inflammatory involvement of vertebrae in ankylosing spondylitis. J Rheumatol 2:296–302
Braun J, Bollow M, Remlinger G et al (1998) Prevalence of spondylarthropathies in HLA-B27 positive and negative blood donors. Arthritis Rheum 41:58–67
Trontzas P, Andrianakos A, Miyakis S, Pantelidou K, Vafiadou E, Garantziotou V, Voudouris C, ESORDIG study group (2005) Seronegative spondyloarthropathies in Greece: a population-based study of prevalence, clinical pattern, and management. The ESORDIG study. Clin Rheumatol 24:583–589
De Angelis R, Salaffi F, Grassi W (2007) Prevalence of spondyloarthropathies in an Italian population sample: a regional community-based study. Scand J Rheumatol 36:14–21
Braun J, Sieper J (2007) Ankylosing spondylitis. Lancet 369:1379–1390
Feldtkeller E, Khan MA, van der Heijde D, van der Linden S, Braun J (2003) Age at disease onset and diagnosis delay in HLA-B27 negative vs. positive patients with ankylosing spondylitis. Rheumatol Int 23:61–66
Deodhar A, Mease PJ, Reveille JD, Curtis JR, Chen S, Malhotra K, Pangan AL (2016) Frequency of axial spondyloarthritis diagnosis among patients seen by United States rheumatologists for evaluation of chronic back pain. Arthritis Rheumatol 68:1669–1676
Kang JH, Chen YH, Lin HC (2010) Comorbidity profiles among patients with ankylosing spondylitis: a nationwide population-based study. Ann Rheum Dis 69:1165–1168
Bremander A, Petersson IF, Bergman S, Englund M (2011) Population-based estimates of common comorbidities and cardiovascular disease in ankylosing spondylitis. Arthritis Care Res (Hoboken) 63:550–556
Mercieca C, van der Horst-Bruinsma IE, Borg AA (2014) Pulmonary, renal and neurological comorbidities in patients with ankylosing spondylitis; implications for clinical practice. Curr Rheumatol Rep 16:434
Essers I, Stolwijk C, Boonen A, De Bruin ML, Bazelier MT, de Vries F, van Tubergen A (2016) Ankylosing spondylitis and risk of ischaemic heart disease: a population-based cohort study. Ann Rheum Dis 75:203–209
Chou CH, Lin MC, Peng CL, Wu YC, Sung FC, Kao CH, Liu SH (2014) A nationwide population-based retrospective cohort study: increased risk of acute coronary syndrome in patients with ankylosing spondylitis. Scand J Rheumatol 43:132–136
Meesters JJ, Bremander A, Bergman S, Petersson IF, Turkiewicz A, Englund M (2014) The risk for depression in patients with ankylosing spondylitis: a population-based cohort study. Arthritis Res Ther 16:418
Sun LM, Muo CH, Liang JA, Chang SN, Sung FC, Kao CH (2014) Increased risk of cancer for patients with ankylosing spondylitis: a nationwide population-based retrospective cohort study. Scand J Rheumatol 43:301–306
Chen HH, Yeh SY, Chen HY, Lin CL, Sung FC, Kao CH (2014) Ankylosing spondylitis and other inflammatory spondyloarthritis increase the risk of developing type 2 diabetes in an Asian population. Rheumatol Int 34:265–270
Keller JJ, Hsu JL, Lin SM, Chou CC, Wang LH, Wang J, Bai CH, Chiou HY (2014) Increased risk of stroke among patients with ankylosing spondylitis: a population-based matched-cohort study. Rheumatol Int 34:255–263
Rosenbaum J, Chandran V (2012) Management of comorbidities in ankylosing spondylitis. Am J Med Sci 343:364–366
Castaneda S, Martin-Martinez MA, Gonzalez-Juanatey C et al (2015) Cardiovascular morbidity and associated risk factors in Spanish patients with chronic inflammatory rheumatic diseases attending rheumatology clinics: baseline data of the CARMA project. Semin Arthritis Rheum 44:618–626
Bergman M, Lundholm A (2018) Managing morbidity and treatment-related toxicity in patients with ankylosing spondylitis. Rheumatology (Oxford) 57:419–428. https://doi.org/10.1093/rheumatology/kex292
Stolwijk C, van Tubergen A, Castillo-Ortiz JD, Boonen A (2015) Prevalence of extra-articular manifestations in patients with ankylosing spondylitis: a systematic review and meta-analysis. Ann Rheum Dis 74:65–73
International Diabetes Federation. Diabetes Atlas. Diabetes prevalence (% of population ages 20 to 79). http://www.diabetesatlas.org/across-the-globe.html. Accessed 3 November 2017
Shen TC, Lin CL, Wei CC, Chen CH, Tu CY, Hsia TC, Shih CM, Hsu WH, Sung FC (2015) The risk of asthma in patients with ankylosing spondylitis: a population-based cohort study. PLoS One 10:e0116608
de Nijs SB, Venekamp LN, Bel EH (2013) Adult-onset asthma: is it really different? Eur Respir Rev 22:44–52
Leynaert B, Sunyer J, Garcia-Esteban R, Svanes C, Jarvis D, Cerveri I, Dratva J, Gislason T, Heinrich J, Janson C, Kuenzli N, de Marco R, Omenaas E, Raherison C, Gómez Real F, Wjst M, Zemp E, Zureik M, Burney PGJ, Anto JM, Neukirch F (2012) Gender differences in prevalence, diagnosis and incidence of allergic and non-allergic asthma: a population-based cohort. Thorax 67:625–631
Wang HL, Zhou YM, Zhu GZ, Yang Z, Hua BJ (2017) Malignancy as a comorbidity in rheumatic diseases: a retrospective hospital-based study. Clin Rheumatol 37:81–85. https://doi.org/10.1007/s10067-017-3676-8
Deng C, Li W, Fei Y, Li Y, Zhang F (2016) Risk of malignancy in ankylosing spondylitis: a systematic review and meta-analysis. Sci Rep 6:32063
Alaranta H, Luoto S, Konttinen YT (2002) Traumatic spinal cord injury as a complication to ankylosing spondylitis. An extended report. Clin Exp Rheumatol 20:66–68
Jacobs WB, Fehlings MG (2008) Ankylosing spondylitis and spinal cord injury: origin, incidence, management, and avoidance. Neurosurg Focus 24:E12
Feldtkeller E, Vosse D, Geusens P, van der Linden S (2006) Prevalence and annual incidence of vertebral fractures in patients with ankylosing spondylitis. Rheumatol Int 26:234–239
Leone A, Marino M, Dell'Atti C, Zecchi V, Magarelli N, Colosimo C (2016) Spinal fractures in patients with ankylosing spondylitis. Rheumatol Int 36:1335–1346
Webers C, Essers I, Ramiro S, Stolwijk C, Landewé R, van der Heijde D, van den Bosch F, Dougados M, van Tubergen A (2016) Gender-attributable differences in outcome of ankylosing spondylitis: long-term results from the Outcome in Ankylosing Spondylitis International Study. Rheumatology (Oxford) 55:419–428
Walsh JA, Duffin KC, Crim J, Clegg DO (2012) Lower frequency of obstructive sleep apnea in spondyloarthritis patients taking TNF-inhibitors. J Clin Sleep Med 8:643–648
Solak O, Fidan F, Dündar U, Türel A, Ayçiçek A, Kavuncu V, Unlü M (2009) The prevalence of obstructive sleep apnoea syndrome in ankylosing spondylitis patients. Rheumatology (Oxford) 48:433–435
Erb N, Karokis D, Delamere JP, Cushley MJ, Kitas GD (2003) Obstructive sleep apnoea as a cause of fatigue in ankylosing spondylitis. Ann Rheum Dis 62:183–184
Ciftci TU, Kokturk O, Bukan N, Bilgihan A (2004) The relationship between serum cytokine levels with obesity and obstructive sleep apnea syndrome. Cytokine 28:87–91
In E, Turgut T, Gulkesen A, Yolbas S, Akgol G, Koca SS (2016) Sleep quality is related to disease activity in patients with ankylosing spondylitis: a polysomnographic study. J Clin Rheumatol 22:248–252
Karatas G, Bal A, Yuceege M, Firat H, Gurcay E, Ardic S, Cakci FA (2017) Evaluation of sleep quality in patients with ankylosing spondylitis and efficacy of anti-TNF-alpha therapy on sleep problems: a polisomnographic study. Int J Rheum Dis. https://doi.org/10.1111/1756-185X.13102
Bengtsson K, Forsblad-d'Elia H, Lie E et al (2017) Are ankylosing spondylitis, psoriatic arthritis and undifferentiated spondyloarthritis associated with an increased risk of cardiovascular events? A prospective nationwide population-based cohort study. Arthritis Res Ther 19:102
van der Weijden MA, Claushuis TA, Nazari T, Lems WF, Dijkmans BA, van der Horst-Bruinsma IE (2012) High prevalence of low bone mineral density in patients within 10 years of onset of ankylosing spondylitis: a systematic review. Clin Rheumatol 31:1529–1535
Wang DM, Zeng QY, Chen SB, Gong Y, Hou ZD, Xiao ZY (2015) Prevalence and risk factors of osteoporosis in patients with ankylosing spondylitis: a 5-year follow-up study of 504 cases. Clin Exp Rheumatol 33:465–470
US Department of Labor Bureau of Labor Statistics (2016) Employee Tenure in 2016. USDL-16-1867
Acknowledgments
The authors gratefully acknowledge the important contributions of Aswin Kalyanaraman for his role in the analysis of data, and Jay Margolis, Swathi Malla, and Ellen Riehle for their editorial assistance in the development of the manuscript.
Funding
Support for third-party writing assistance, furnished by Nicola Gillespie, DVM, of Health Interactions, Inc., was provided by Novartis Pharmaceuticals Corporation, East Hanover, NJ.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Authors’ full disclosures
Xue Song and Gilwan Kim are employees of Truven Health Analytics, an IBM Company, which was paid by Novartis in connection with the development of this manuscript. Yujin Park is an employee of Novartis. Jessica Walsh is a paid consultant to Novartis.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Walsh, J.A., Song, X., Kim, G. et al. Evaluation of the comorbidity burden in patients with ankylosing spondylitis using a large US administrative claims data set. Clin Rheumatol 37, 1869–1878 (2018). https://doi.org/10.1007/s10067-018-4086-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-018-4086-2