Abstract
Objectives
This study aimed at comparing the microtensile bond strength (MTBS) and interfacial adaptation of a modern self-curing and a light-curing restorative bulk-fill composite to a conventional composite applied with the layering technique.
Methods
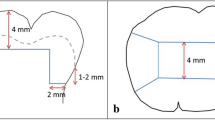
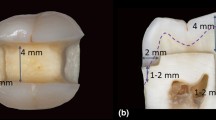
Forty-eight occlusal cavities were divided in three main groups (16/group) based on tested materials: (i) STELA, bulk-fill self-curing restorative (STELA, SDI Ltd.); (ii) 3 M-BULK, bulk-fill composite (Filtek One Bulk-Fill, 3 M Oral Care); and (iii) 3 M-CTR, a conventional composite (Filtek Supreme XTE, 3 M Oral Care). These were used in combination with their adhesives in self-etch (SE) or etch-and-rinse (ER) mode. Specimens stored in artificial saliva (24 h or 12 months) were evaluated for MTBS and fractography. The interfacial analysis was performed through confocal microscopy. ANOVA and Fisher’s LSD post hoc tests were performed with a level of significance of 5%.
Results
All the tested materials applied in ER mode presented (24 h) greater bond strength than in SE mode. Although all materials showed a significant drop in the bond strength after prolonged storage, STELA showed the highest bonding performance and interfaces with few gaps. 3 M-BULK had the lowest bond strength and an interface with several voids and gaps.
Conclusions
All materials were affected by interface degradation and bonding reduction over prolonged aging. However, their use in combination with adhesives applied in ER mode may offer greater immediate bonding performance.
Clinical relevance.
The use of restorative light-curing bulk-fill composites may generate gaps at the bonding interface and voids. STELA may represent a suitable alternative to avoid such issues.





Similar content being viewed by others
References
Sideridou I, Tserki V, Papanastasiou G (2002) Effect of chemical structure on degree of conversion in light-cured dimethacrylate-based dental resins. Biomater 23:1819–1829. https://doi.org/10.1016/s0142-9612(01)00308-8
Ferracane JL (2020) Resin composite-state of the art. Dent Mater 27:29–38. https://doi.org/10.1016/j.dental.2010.10.020
Schneider LF, Cavalcante LM, Silikas N (2010) Shrinkage stresses generated during resin-composite applications: a review. J Dent Biomech 2010:131630. https://doi.org/10.4061/2010/131630
Ferracane JL (2005) Developing a more complete understanding of stresses produced in dental composites during polymerisation. Dent Mater 21:36–42. https://doi.org/10.1016/j.dental.2004.10.004
Cho E, Sadr A, Inai N, Tagami J (2011) Evaluation of resin composite polymerisation by three dimensional micro-CT imaging and nanoindentation. Dent Mater 27:1070–1078. https://doi.org/10.1016/j.dental.2011.07.008
Carvalho RM, Pereira JC, Yoshiyama M, Pashley DH (1996) A review of polymerisation contraction: the influence of stress development versus stress relief. Oper Dent 21:17–24
Versluis A, Douglas WH, Cross M, Sakaguchi RL (1996) Does an incremental filling technique reduce polymerization shrinkage stresses? J Dent Res 75:871–8. https://doi.org/10.1177/00220345960750030301. (Mar)
Rosatto CM, Bicalho AA, Veríssimo C, Bragança GF, Rodrigues MP, Tantbirojn D, Versluis A, Soares CJ (2015) Mechanical properties, shrinkage stress, cuspal strain and fracture resistance of molars restored with bulk-fill composites and incremental filling technique. J Dent 43:1519–1528. https://doi.org/10.1016/j.jdent.2015.09.007
Umer F, Khan FR (2011) Postoperative sensitivity in class V composite restorations: comparing soft start vs. constant curing modes of LED. J Conserv Dent 14:76–79. https://doi.org/10.4103/0972-0707.80738
Yu P, Xu YX, Liu YS (2022) Polymerization shrinkage and shrinkage stress of bulk-fill and non-bulk-fill resin-based composites. J Dent Sci 17:1212–1216. https://doi.org/10.1016/j.jds.2021.12.004
Hansen EK (1986) Effect of cavity depth and application technique on marginal adaptation of resins in dentin cavities. J Dent Res 65:1319–1321. https://doi.org/10.1177/00220345860650110701
Hilton TJ, Schwartz RS, Ferracane JL (1997) Microleakage of four class II resin composite insertion techniques at intraoral temperature. Quintessence Int 28:135–144
Sengupta A, Naka O, Mehta SB, Banerji S (2023) The clinical performance of bulk-fill versus the incremental layered application of direct resin composite restorations: a systematic review. Evid Based Dent 24:143. https://doi.org/10.1038/s41432-023-00905
Fronza BM, Ayres A, Pacheco RR, Rueggeberg FA, Dias C, Giannini M (2017) Characterization of inorganic filler content, mechanical properties, and light transmission of bulk-fill resin composites. Oper Dent 42:445–455. https://doi.org/10.2341/16-024-L
Son SA, Park JK, Seo DG, Ko CC, Kwon YH (2017) How light attenuation and filler content affect the microhardness and polymerisation shrinkage and translucency of bulk-fill composites? Clin Oral Investig 21:559–565. https://doi.org/10.1007/s00784-016-1920-2
Moszner N, Fischer UK, Ganster B, Liska R, Rheinberger V (2008) Benzoyl germanium derivatives as novel visible light photoinitiators for dental materials. Dent Mater 24:901–907. https://doi.org/10.1016/j.dental.2007.11.004
Kaisarly D, Meierhofer D, El Gezawi M, Rösch P, Kunzelmann KH (2021) Effects of flowable liners on the shrinkage vectors of bulk-fill composites. Clin Oral Investig 25:4927–4940. https://doi.org/10.1007/s00784-021-03801-2
Sauro S, Makeeva I, Faus-Matoses V, Foschi F, Giovarruscio M, Maciel Pires P, Martins Moura ME, Almeida Neves A, Faus-Llácer V (2019) Effects of ions-releasing restorative materials on the dentine bonding longevity of modern universal adhesives after load-cycle and prolonged artificial saliva aging. Materials (Basel) 12:722. https://doi.org/10.3390/ma12050722
Oglakci B, Kazak M, Donmez N, Dalkilic EE, Koymen SS (2019) The use of a liner under different bulk-fill resin composites: 3D GAP formation analysis by x-ray microcomputed tomography. J Appl Oral Sci 25(28):e20190042. https://doi.org/10.1590/1678-7757-2019-0042
Burrer P, Par M, Fürer L, Stübi M, Marovic D, Tarle Z, Attin T, Tauböck TT (2023) Effect of polymerization mode on shrinkage kinetics and degree of conversion of dual-curing bulk-fill resin composites. Clin Oral Investig 27:3169–3180. https://doi.org/10.1007/s00784-023-04928-0
Ilie N (2022) Fracture and viscoelastic behavior of novel self-adhesive materials for simplified restoration concepts. J Mech Behav Biomed Mater 125:104970
Braga RR, Ferracane JL (2002) Contraction stress related to degree of conversion and reaction kinetics. J Dent Res 81:114–118
Thadathil Varghese J, Raju R, Farrar P, Prentice L, Prusty BG (2023) Comparative analysis of self-cure and dual cure-dental composites on their physico-mechanical behaviour. Aust Dent J 22. https://doi.org/10.1111/adj.13004
Sauro S, Pashley DH (2016) Strategies to stabilise dentine-bonded interfaces through remineralising operative approaches: state of the art. Int J Adhes Adhes 69:39–57. https://doi.org/10.1016/j.ijadhadh.2016.03.014
Al-Zain AO, Baeesa L, Jassoma E, Alghilan MA, Hariri M, Ismail EH, Münchow EA (2023) Assessment of internal porosities for different placement techniques of bulk-fill resin-based composites: a micro-computed tomography study. Clin Oral Invest. https://doi.org/10.1007/s00784-023-05337-z
Ferracane JL, Hilton TJ (2016) Polymerization stress-is it clinically meaningful? Dent Mater 32:1–10. https://doi.org/10.1016/j.dental.2015.06.020
Maciel Pires P, Ionescu AC, Pérez-Gracia MT, Vezzoli E, Soares IPM, Brambilla E, de Almeida NA, Sauro S (2022) Assessment of the remineralisation induced by contemporary ion-releasing materials in mineral-depleted dentine. Clin Oral Investig 26:6195–6207. https://doi.org/10.1007/s00784-022-04569-9
Pires PM, Neves AA, Makeeva IM, Schwendicke F, Faus-Matoses V, Yoshihara K, Banerjee A, Sauro S (2020) Contemporary restorative ion-releasing materials: current status, interfacial properties and operative approaches. Br Dent J 229:450–458. https://doi.org/10.1038/s41415-020-2169-3
Watson TF, Bartlett DW (1994) Adhesive systems: composites, dentine bonding agents and glass ionomers. Br Dent J 19(176):227–231. https://doi.org/10.1038/sj.bdj.4808410
Lööf J, Svahn F, Jarmar T, Engqvist H, Pameijer CH (2008) A comparative study of the bioactivity of three materials for dental applications. Dent Mater 24(5):653–659. https://doi.org/10.1016/j.dental.2007.06.028
Sauro S, Osorio R, Watson TF, Toledano M (2015) Influence of phosphoproteins’ biomimetic analogs on remineralization of mineral-depleted resin-dentin interfaces created with ion-releasing resin-based systems. Dent Mater 31:759–777. https://doi.org/10.1016/j.dental.2015.03.013
Abuna G, Feitosa VP, Correr AB, Cama G, Giannini M, Sinhoreti MA, Pashley DH, Sauro S (2016) Bonding performance of experimental bioactive/biomimetic self-etch adhesives doped with calcium-phosphate fillers and biomimetic analogs of phosphoproteins. J Dent 52:79–86. https://doi.org/10.1016/j.jdent.2016.07.016
Sofan E, Sofan A, Palaia G, Tenore G, Romeo U, Migliau G (2017) Classification review of dental adhesive systems: from the IV generation to the universal type. Ann Stomatol (Roma) 8:1–17. https://doi.org/10.11138/ads/2017.8.1.001
Maciel Pires P, Dávila-Sánchez A, Faus-Matoses V, Nuñez Martí JM, Lo Muzio L, Sauro S (2022) Bonding performance and ultramorphology of the resin-dentine interface of contemporary universal adhesives. Clin Oral Investig 26(6):4391–4405. https://doi.org/10.1007/s00784-022-04402-3
Hayashi J, Espigares J, Takagaki T, Shimada Y, Tagami J, Numata T, Chan D, Sadr A (2019) Real-time in-depth imaging of gap formation in bulk-fill resin composites. Dent Mater 35(4):585–596. https://doi.org/10.1016/j.dental.2019.01.020
Nie J, Yap AU, Wang XY (2018) Influence of shrinkage and viscosity of flowable composite liners on cervical microleakage of class II restorations: a micro-CT analysis. Oper Dent 43(6):656–664. https://doi.org/10.2341/17-091-L
Hashimoto M (2010) A review–micromorphological evidence of degradation in resin-dentin bonds and potential preventional solutions. J Biomed Mater Res B Appl Biomater 92(1):268–280. https://doi.org/10.1002/jbm.b.31535
Sabatini C, Pashley DH (2014) Mechanisms regulating the degradation of dentin matrices by endogenous dentin proteases and their role in dental adhesion. A Rev Am J Dent 27(4):203–214
Nishitani Y, Yoshiyama M, Wadgaonkar B, Breschi L, Mannello F, Mazzoni A, Carvalho RM, Tjäderhane L, Tay FR, Pashley DH (2006) Activation of gelatinolytic/collagenolytic activity in dentin by self-etching adhesives. Eur J Oral Sci 114(2):160–166. https://doi.org/10.1111/j.1600-0722.2006.00342.x
Tay FR, Pashley DH (2003) Water treeing–a potential mechanism for degradation of dentin adhesives. Am J Dent 16:6–12
Sauro S, Watson TF, Mannocci F, Miyake K, Huffman BP, Tay FR, Pashley DH (2009) Two-photon laser confocal microscopy of micropermeability of resin-dentin bonds made with water or ethanol wet bonding. J Biomed Mater Res B Appl Biomater 90(1):327–337. https://doi.org/10.1002/jbm.b.31290
Spencer P, Wang Y (2002) Adhesive phase separation at the dentin interface under wet bonding conditions. J Biomed Mater Res 62(3):447–456. https://doi.org/10.1002/jbm.10364
Ye Q, Park JG, Topp E, Wang Y, Misra A, Spencer P (2008) In vitro performance of nano-heterogeneous dentin adhesive. J Dent Res 87(9):829–833. https://doi.org/10.1177/154405910808700911
Sauro S, Mannocci F, Toledano M, Osorio R, Thompson I, Watson TF (2009) Influence of the hydrostatic pulpal pressure on droplets formation in current etch-and-rinse and self-etch adhesives: a video rate/TSM microscopy and fluid filtration study. Dent Mater 25(11):1392–1402. https://doi.org/10.1016/j.dental.2009.06.010
De Munck J, Van Landuyt K, Peumans M, Poitevin A, Lambrechts P, Braem M, Van Meerbeek B (2005) A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res 84(2):118–132. https://doi.org/10.1177/154405910508400204
Anchieta RB, Machado LS, Martini AP, Santos PH, Giannini M, Janal M, Tovar N, Sundfeld RH, Rocha EP, Coelho PG (2015) Effect of long-term storage on nanomechanical and morphological properties of dentin-adhesive interfaces. Dent Mater 31(2):141–153. https://doi.org/10.1016/j.dental.2014.11.010
Sauro S, Pashley DH, Montanari M, Chersoni S, Carvalho RM, Toledano M, Osorio R, Tay FR, Prati C (2007) Effect of simulated pulpal pressure on dentin permeability and adhesion of self-etch adhesives. Dent Mater 23(6):705–713. https://doi.org/10.1016/j.dental.2006.06.010
Tay FR, Frankenberger R, Krejci I, Bouillaguet S, Pashley DH, Carvalho RM, Lai CN (2004) Single-bottle adhesives behave as permeable membranes after polymerization I In vivo evidence. J Dent 32(8):611–621. https://doi.org/10.1016/j.jdent.2004.04.006
Davidson CL, de Gee AJ, Feilzer A (1984) The competition between the composite-dentin bond strength and the polymerization contraction stress. J Dent Res 63(12):1396–1399. https://doi.org/10.1177/00220345840630121101
Pashley DH (1991) Dentin bonding: overview of the substrate with respect to adhesive material. J Esthet Dent 3(2):46–50. https://doi.org/10.1111/j.1708-8240.1991.tb00808.x
Perdigão J, Reis A, Loguercio AD (2013) Dentin adhesion and MMPs: a comprehensive review. J Esthet Restor Dent 25(4):219–241. https://doi.org/10.1111/jerd.12016
Sauro S, Osorio R, Watson TF, Toledano M (2012) Assessment of the quality of resin-dentin bonded interfaces: an AFM nano-indentation, μTBS and confocal ultramorphology study. Dent Mater 28(6):622–631. https://doi.org/10.1016/j.dental.2012.02.005
Acknowledgements
All the materials used in this study were regularly purchased from local distributors. The authors also gratefully acknowledge SDI Ltd. (Bayswater, Australia), for a generous donation of STELA Automix restorative and STELA Primer used in this study.
Funding
Paula Maciel Pires was undertaking a post-doctorate exchange program at Cardenal Herrera University during a part of the experimental assay and was supported by a FAPERJ grant from Brazil (E-26/205.718/2022). This study was also supported in part by a grant funded by Generalitat Valenciana (CIAICO/2022/198).
Author information
Authors and Affiliations
Contributions
S.S. and P.M.P. wrote the main manuscript, performed the experimental tests and analysis and interpretation of the results; P.F. contributed to the experimental design; A. A.N. performed the statistical analysis and reviewed the final version of the manuscript; M.L.S. contributed to the experimental design and reviewed the final version of the manuscript; A.F.C. performed part of the experimental tests and reviewed the final version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, human molars used in this study were collected according to the guidelines of the local Ethics Committee (CEEI22/309).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pires, P.M., de Almeida Neves, A., Lukomska-Szymanska, M. et al. Bonding performance and interfacial adaptation of modern bulk-fill restorative composites after aging in artificial saliva: an in vitro study. Clin Oral Invest 28, 132 (2024). https://doi.org/10.1007/s00784-024-05525-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00784-024-05525-5