Abstract
Objectives
This study aimed at evaluating the microtensile bond strength (μTBS) and the resin-dentine ultramorphology (24 h and 10 months ageing) of contemporary universal adhesives applied in self-etch (SE) or etch-and-rinse (ER) mode.
Materials and methods
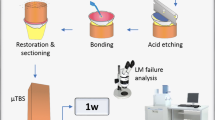
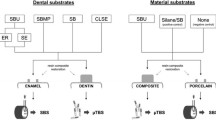
Sixty-four sound human molars were collected and randomly allocated in 4 main experimental groups (n = 16) according to the adhesive system employed and subsequently divided into two subgroups depending on their application mode SE or ER (n = 8): ZipBond X (ZBX-SE; ZBX-ER), Prime and Bond Active (PBA-SE; PBA-ER), Clearfil Universal Bond Quick (CBQ-SE; CBQ-ER) or Scotchbond Universal (SCH-SE; SCH-ER). The specimens were cut into sticks with a cross-sectional area of approximately 0.9 mm2 and subjected to μTBS testing at 24 h or after 10 months of ageing in artificial saliva (AS). Five representative fractured specimens from each group were analysed using field-emission scanning electron microscopy (FE-SEM). Resin-dentine slabs (Ø 0.9mm2) from each experimental group were immersed in Rhodamine B and subsequently analysed using confocal microscopy analysis (CLSM). The μTBS results were analysed using a two-way ANOVA and Newman–Keuls multiple-comparison test (α = 0.05).
Results
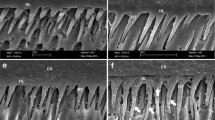
ZBX, PBA and SCH exhibited greater μTBS values than CQB at 24 h in both SE and ER modes (p < 0.05). CQB showed a significant decrease in μTBS values after ageing both when used in SE and ER mode (p < 0.05). ZBX-ER exhibited no significant differences in the μTBS test after ageing (p > 0.05), while a significant drop in μTBS was seen in SCH-ER and APB-ER after 10-month ageing (p < 0.05). Clear signs of degradation were evident in the resin-dentine interface created with CQB regardless of the application mode or the ageing time. In APB-ER and SCH-ER groups, such signs of degradation were evident after ageing in AS. ZBX showed slight dye infiltration both when used in ER and SE mode.
Conclusions
The long-term bonding performance of modern universal adhesives is usually influenced by the adhesive strategy employed; self-etching application should be prioritised during dentine bonding. Moreover, the use of shortened bonding protocols may compromise the quality of the resin-dentine interface and the bonding performance of most modern universal adhesives.
Clinical relevance
The use of etch-and-rinse bonding procedures, as well as “shortened” application protocols should be eluded when using modern universal adhesives in dentine. However, new generation universal adhesives based on innovative chemical formulations may probably allow clinicians to achieve long-term bonding performance with such simplified system also when employed in ER mode.





Similar content being viewed by others
References
Hardan L, Bourgi R, Kharouf N, Mancino D, Zarow M, Jakubowicz N, Haikel Y, Cuevas-Suarez CE (2021) Bond strength of universal adhesives to dentin: a systematic review and meta-analysis. Polymers (Basel) 13.https://doi.org/10.3390/polym13050814
Rosa WL, Piva E, Silva AF (2015) Bond strength of universal adhesives: a systematic review and meta-analysis. J Dent 43:765–776. https://doi.org/10.1016/j.jdent.2015.04.003
Van Meerbeek B, Yoshihara K, Van Landuyt K, Yoshida Y, Peumans M (2020) From Buonocore’s Pioneering Acid-Etch Technique to self-adhering restoratives. A status perspective of rapidly advancing dental adhesive technology. J Adhes Dent 22:7–34. https://doi.org/10.3290/j.jad.a43994
Munoz MA, Luque-Martinez I, Malaquias P, Hass V, Reis A, Campanha NH, Loguercio AD (2015) In vitro longevity of bonding properties of universal adhesives to dentin. Oper Dent 40:282–292. https://doi.org/10.2341/14-055-L
Cuevas-Suarez CE, da Rosa WLO, Lund RG, da Silva AF, Piva E (2019) Bonding performance of universal adhesives: an updated systematic review and meta-analysis. J Adhes Dent 21:7–26. https://doi.org/10.3290/j.jad.a41975
Zanatta RF, Silva TM, Esper M, Bresciani E, Goncalves S, Caneppele T (2019) Bonding performance of simplified adhesive systems in noncarious cervical lesions at 2-year follow-up: a double-blind randomized clinical trial. Oper Dent 44:476–487. https://doi.org/10.2341/18-049-C
de Paris MT, Perdigao J, de Paula E, Coppla F, Hass V, Scheffer RF, Reis A, Loguercio AD (2020) Five-year clinical evaluation of a universal adhesive: a randomized double-blind trial. Dent Mater. https://doi.org/10.1016/j.dental.2020.08.007
Zhang ZY, Tian FC, Niu LN, Ochala K, Chen C, Fu BP, Wang XY, Pashley DH, Tay FR (2016) Defying ageing: an expectation for dentine bonding with universal adhesives? J Dent 45:43–52. https://doi.org/10.1016/j.jdent.2015.11.008
Sauro S, Makeeva I, Faus-Matoses V, Foschi F, Giovarruscio M, Maciel Pires P, Martins Moura ME, Almeida Neves A, Faus-Llacer V (2019) Effects of ions-releasing restorative materials on the dentine bonding longevity of modern universal adhesives after load-cycle and prolonged artificial saliva aging. Materials (Basel) 12.https://doi.org/10.3390/ma12050722
Spencer P, Ye Q, Park J, Topp EM, Misra A, Marangos O, Wang Y, Bohaty BS, Singh V, Sene F, Eslick J, Camarda K, Katz JL (2010) Adhesive/dentin interface: the weak link in the composite restoration. Ann Biomed Eng 38:1989–2003. https://doi.org/10.1007/s10439-010-9969-6
Astvaldsdottir A, Dagerhamn J, van Dijken JW, Naimi-Akbar A, Sandborgh-Englund G, Tranaeus S, Nilsson M (2015) Longevity of posterior resin composite restorations in adults - a systematic review. J Dent 43:934–954. https://doi.org/10.1016/j.jdent.2015.05.001
Demarco FF, Correa MB, Cenci MS, Moraes RR, Opdam NJ (2012) Longevity of posterior composite restorations: not only a matter of materials. Dent Mater 28:87–101. https://doi.org/10.1016/j.dental.2011.09.003
Szesz AL, Pereira GMA, Siqueira FSF, Cardenas AFM, Bandeca MC, Armas-Vega A, Reis A, Loguercio AD (2021) Effect of addition of dimethyl sulfoxide to simplified adhesives on dentin bond durability after three years of water storage. J Adhes Dent 23:159–165. https://doi.org/10.3290/j.jad.b1079585
Pashley DH, Tay FR, Carvalho RM, Rueggeberg FA, Agee KA, Carrilho M, Donnelly A, Garcia-Godoy F (2007) From dry bonding to water-wet bonding to ethanol-wet bonding. A review of the interactions between dentin matrix and solvated resins using a macromodel of the hybrid layer. Am J Dent 20:7–20
Eick JD, Gwinnett AJ, Pashley DH, Robinson SJ (1997) Current concepts on adhesion to dentin. Crit Rev Oral Biol Med 8:306–335. https://doi.org/10.1177/10454411970080030501
Wang Y, Spencer P, Yao X, Brenda B (2007) Effect of solvent content on resin hybridization in wet dentin bonding. J Biomed Mater Res A 82:975–983. https://doi.org/10.1002/jbm.a.31232
Reis A, Carrilho M, Breschi L, Loguercio AD (2013) Overview of clinical alternatives to minimize the degradation of the resin-dentin bonds. Oper Dent 38:E1–E25. https://doi.org/10.2341/12-258-LIT
Loguercio AD, Loeblein F, Cherobin T, Ogliari F, Piva E, Reis A (2009) Effect of solvent removal on adhesive properties of simplified etch-and-rinse systems and on bond strengths to dry and wet dentin. J Adhes Dent 11:213–219
Sauro S, Osorio R, Watson TF, Toledano M (2012) Assessment of the quality of resin-dentin bonded interfaces: an AFM nano-indentation, muTBS and confocal ultramorphology study. Dent Mater 28:622–631. https://doi.org/10.1016/j.dental.2012.02.005
Yiu CK, Pashley EL, Hiraishi N, King NM, Goracci C, Ferrari M, Carvalho RM, Pashley DH, Tay FR (2005) Solvent and water retention in dental adhesive blends after evaporation. Biomaterials 26:6863–6872. https://doi.org/10.1016/j.biomaterials.2005.05.011
Carvalho RM, Mendonca JS, Santiago SL, Silveira RR, Garcia FC, Tay FR, Pashley DH (2003) Effects of HEMA/solvent combinations on bond strength to dentin. J Dent Res 82:597–601. https://doi.org/10.1177/154405910308200805
Luque-Martinez IV, Perdigao J, Munoz MA, Sezinando A, Reis A, Loguercio AD (2014) Effects of solvent evaporation time on immediate adhesive properties of universal adhesives to dentin. Dent Mater 30:1126–1135. https://doi.org/10.1016/j.dental.2014.07.002
Breschi L, Mazzoni A, Ruggeri A, Cadenaro M, Di Lenarda R, De Stefano DE (2008) Dental adhesion review: aging and stability of the bonded interface. Dent Mater 24:90–101. https://doi.org/10.1016/j.dental.2007.02.009
Spagnuolo G, Pires PM, Calarco A, Peluso G, Banerjee A, Rengo S, Elias Boneta AR, Sauro S (2021) An in-vitro study investigating the effect of air-abrasion bioactive glasses on dental adhesion, cytotoxicity and odontogenic gene expression. Dent Mater 37:1734–1750. https://doi.org/10.1016/j.dental.2021.09.004
Feitosa VP, Sauro S, Ogliari FA, Stansbury JW, Carpenter GH, Watson TF, Sinhoreti MA, Correr AB (2014) The role of spacer carbon chain in acidic functional monomers on the physicochemical properties of self-etch dental adhesives. J Dent 42:565–574. https://doi.org/10.1016/j.jdent.2014.02.009
Tezvergil-Mutluay A, Seseogullari-Dirihan R, Feitosa VP, Cama G, Brauer DS, Sauro S (2017) Effects of composites containing bioactive glasses on demineralized dentin. J Dent Res 96:999–1005. https://doi.org/10.1177/0022034517709464
Pashley DH, Tay FR, Breschi L, Tjaderhane L, Carvalho RM, Carrilho M, Tezvergil-Mutluay A (2011) State of the art etch-and-rinse adhesives. Dent Mater 27:1–16. https://doi.org/10.1016/j.dental.2010.10.016
Saikaew P, Matsumoto M, Chowdhury A, Carvalho RM, Sano H (2018) Does shortened application time affect long-term bond strength of universal adhesives to dentin? Oper Dent 43:549–558. https://doi.org/10.2341/17-205-L
Thanatvarakorn O, Prasansuttiporn T, Takahashi M, Thittaweerat S, Foxton RM, Ichinose S, Tagami J, Nakajima M (2016) Effect of scrubbing technique with mild self-etching adhesives on dentin bond strengths and nanoleakage expression. J Adhes Dent 18:197–204. https://doi.org/10.3290/j.jad.a36033
Borges BC, Souza-Junior EJ, Brandt WC, Loguercio AD, Montes MA, Puppin-Rontani RM, Sinhoreti MA (2012) Degree of conversion of simplified contemporary adhesive systems as influenced by extended air-activated or passive solvent volatilization modes. Oper Dent 37:246–252. https://doi.org/10.2341/11-248-L
Cadenaro M, Maravic T, Comba A, Mazzoni A, Fanfoni L, Hilton T, Ferracane J, Breschi L (2019) The role of polymerization in adhesive dentistry. Dent Mater 35:e1–e22. https://doi.org/10.1016/j.dental.2018.11.012
Saikaew P, Chowdhury AF, Fukuyama M, Kakuda S, Carvalho RM, Sano H (2016) The effect of dentine surface preparation and reduced application time of adhesive on bonding strength. J Dent 47:63–70. https://doi.org/10.1016/j.jdent.2016.02.001
Spencer P, Wang Y (2002) Adhesive phase separation at the dentin interface under wet bonding conditions. J Biomed Mater Res 62:447–456. https://doi.org/10.1002/jbm.10364
Feitosa VP, Sauro S, Zenobi W, Silva JC, Abuna G, Van Meerbeek B, Sinhoreti MAC, Correr AB, Yoshihara K (2019) Degradation of adhesive-dentin interfaces created using different bonding strategies after five-year simulated pulpal pressure. J Adhes Dent 21:199–207. https://doi.org/10.3290/j.jad.a42510
Sauro S, Pashley DH, Mannocci F, Tay FR, Pilecki P, Sherriff M, Watson TF (2008) Micropermeability of current self-etching and etch-and-rinse adhesives bonded to deep dentine: a comparison study using a double-staining/confocal microscopy technique. Eur J Oral Sci 116:184–193. https://doi.org/10.1111/j.1600-0722.2007.00518.x
Van Meerbeek B, De Munck J, Mattar D, Van Landuyt K, Lambrechts P (2003) Microtensile bond strengths of an etch & rinse and self-etch adhesive to enamel and dentin as a function of surface treatment. Oper Dent 28:647–660
Hashimoto M, Ohno H, Sano H, Kaga M, Oguchi H (2003) In vitro degradation of resin-dentin bonds analyzed by microtensile bond test, scanning and transmission electron microscopy. Biomaterials 24:3795–3803. https://doi.org/10.1016/s0142-9612(03)00262-x
Tay FR, Pashley DH, Yoshiyama M (2002) Two modes of nanoleakage expression in single-step adhesives. J Dent Res 81:472–476. https://doi.org/10.1177/154405910208100708
Nishitani Y, Yoshiyama M, Wadgaonkar B, Breschi L, Mannello F, Mazzoni A, Carvalho RM, Tjaderhane L, Tay FR, Pashley DH (2006) Activation of gelatinolytic/collagenolytic activity in dentin by self-etching adhesives. Eur J Oral Sci 114:160–166. https://doi.org/10.1111/j.1600-0722.2006.00342.x
Bacelar-Sa R, Sauro S, Abuna G, Vitti R, Nikaido T, Tagami J, Ambrosano GMB, Giannini M (2017) Adhesion evaluation of dentin sealing, micropermeability, and bond strength of current hema-free adhesives to dentin. J Adhes Dent 19:357–364. https://doi.org/10.3290/j.jad.a38866
Van Landuyt KL, De Munck J, Mine A, Cardoso MV, Peumans M, Van Meerbeek B (2010) Filler debonding & subhybrid-layer failures in self-etch adhesives. J Dent Res 89:1045–1050. https://doi.org/10.1177/0022034510375285
De Munck J, Mine A, Poitevin A, Van Ende A, Cardoso MV, Van Landuyt KL, Peumans M, Van Meerbeek B (2012) Meta-analytical review of parameters involved in dentin bonding. J Dent Res 91:351–357. https://doi.org/10.1177/0022034511431251
De Munck J, Van Landuyt K, Peumans M, Poitevin A, Lambrechts P, Braem M, Van Meerbeek B (2005) A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res 84:118–132. https://doi.org/10.1177/154405910508400204
Follak AC, Miotti LL, Lenzi TL, Rocha RO, Soares FZM (2021) Self-etch approach of universal adhesives as an alternative to minimize bond degradation on sound dentin vs caries-affected dentin over time. J Adhes Dent 23:243–252. https://doi.org/10.3290/j.jad.b1367889
Navarra CO, Breschi L, Turco G, Diolosa M, Fontanive L, Manzoli L, Di Lenarda R, Cadenaro M (2012) Degree of conversion of two-step etch-and-rinse adhesives: in situ micro-Raman analysis. J Dent 40:711–717. https://doi.org/10.1016/j.jdent.2012.05.001
Wang R, Shi Y, Li T, Pan Y, Cui Y, Xia W (2017) Adhesive interfacial characteristics and the related bonding performance of four self-etching adhesives with different functional monomers applied to dentin. J Dent 62:72–80. https://doi.org/10.1016/j.jdent.2017.05.010
Hanabusa M, Mine A, Kuboki T, Momoi Y, Van Ende A, Van Meerbeek B, De Munck J (2012) Bonding effectiveness of a new ‘multi-mode’ adhesive to enamel and dentine. J Dent 40:475–484. https://doi.org/10.1016/j.jdent.2012.02.012
Breschi L, Maravic T, Cunha SR, Comba A, Cadenaro M, Tjaderhane L, Pashley DH, Tay FR, Mazzoni A (2018) Dentin bonding systems: from dentin collagen structure to bond preservation and clinical applications. Dent Mater 34:78–96. https://doi.org/10.1016/j.dental.2017.11.005
Ikeda M, Tsubota K, Takamizawa T, Yoshida T, Miyazaki M, Platt JA (2008) Bonding durability of single-step adhesives to previously acid-etched dentin. Oper Dent 33:702–709. https://doi.org/10.2341/08-26
Munoz MA, Luque I, Hass V, Reis A, Loguercio AD, Bombarda NH (2013) Immediate bonding properties of universal adhesives to dentine. J Dent 41:404–411. https://doi.org/10.1016/j.jdent.2013.03.001
Yoshida Y, Yoshihara K, Nagaoka N, Hayakawa S, Torii Y, Ogawa T, Osaka A, Meerbeek BV (2012) Self-assembled nano-layering at the adhesive interface. J Dent Res 91:376–381. https://doi.org/10.1177/0022034512437375
Yoshida Y, Van Meerbeek B, Nakayama Y, Snauwaert J, Hellemans L, Lambrechts P, Vanherle G, Wakasa K (2000) Evidence of chemical bonding at biomaterial-hard tissue interfaces. J Dent Res 79:709–714. https://doi.org/10.1177/00220345000790020301
Marchesi G, Frassetto A, Mazzoni A, Apolonio F, Diolosa M, Cadenaro M, Di Lenarda R, Pashley DH, Tay F, Breschi L (2014) Adhesive performance of a multi-mode adhesive system: 1-year in vitro study. J Dent 42:603–612. https://doi.org/10.1016/j.jdent.2013.12.008
Frassetto A, Breschi L, Turco G, Marchesi G, Di Lenarda R, Tay FR, Pashley DH, Cadenaro M (2016) Mechanisms of degradation of the hybrid layer in adhesive dentistry and therapeutic agents to improve bond durability—a literature review. Dent Mater 32:e41-53. https://doi.org/10.1016/j.dental.2015.11.007
Gutierrez MF, Alegria-Acevedo LF, Mendez-Bauer L, Bermudez J, Davila-Sanchez A, Buvinic S, Hernandez-Moya N, Reis A, Loguercio AD, Farago PV, Martin J, Fernandez E (2019) Biological, mechanical and adhesive properties of universal adhesives containing zinc and copper nanoparticles. J Dent 82:45–55. https://doi.org/10.1016/j.jdent.2019.01.012
Ekambaram MYC, Matinlinna JP (2015) An overview of solvents in resin–dentin bonding. Int J Adhes Adhes 57:22–33. https://doi.org/10.1016/j.ijadhadh.2014.09.007
Reis A, Loguercio AD, Azevedo CL, de Carvalho RM, da Julio SM, Grande RH (2003) Moisture spectrum of demineralized dentin for adhesive systems with different solvent bases. J Adhes Dent 5:183–192
Jacobsen T, Soderholm KJ (1998) Effect of primer solvent, primer agitation, and dentin dryness on shear bond strength to dentin. Am J Dent 11:225–228
Fujita Nakajima K, Nikaido T, Arita A, Hirayama S, Nishiyama N (2018) Demineralization capacity of commercial 10-methacryloyloxydecyl dihydrogen phosphate-based all-in-one adhesive. Dent Mater 34:1555–1565. https://doi.org/10.1016/j.dental.2018.06.027
Teshima M (2018) Effect of the concentration of water in an MDP-based all-in-one adhesive on the efficacy of smear layer removal and on dentin bonding performance. Dent Mater J 37:685–692. https://doi.org/10.4012/dmj.2017-291
Carrilho E, Cardoso M, Marques Ferreira M, Marto CM, Paula A, Coelho AS (2019) 10-MDP based dental adhesives: adhesive interface characterization and adhesive stability—a systematic review. Materials (Basel) 12.https://doi.org/10.3390/ma12050790
Kirihara M, Inoue G, Nikaido T, Ikeda M, Sadr A, Tagami J (2013) Effect of fluoride concentration in adhesives on morphology of acid-base resistant zones. Dent Mater J 32:578–584. https://doi.org/10.4012/dmj.2013-041
Yoshida Y, Yoshihara K, Hayakawa S, Nagaoka N, Okihara T, Matsumoto T, Minagi S, Osaka A, Van Landuyt K, Van Meerbeek B (2012) HEMA inhibits interfacial nano-layering of the functional monomer MDP. J Dent Res 91:1060–1065. https://doi.org/10.1177/0022034512460396
Zhou J, Wurihan SY, Tanaka R, Zhang Z, Zheng K, Li Q, Ikeda S, Gao P, Miyazaki T (2019) Quantitative/qualitative analysis of adhesive-dentin interface in the presence of 10-methacryloyloxydecyl dihydrogen phosphate. J Mech Behav Biomed Mater 92:71–78. https://doi.org/10.1016/j.jmbbm.2018.12.038
Acknowledgements
All the materials used in this study were regularly purchased from local distributors. The authors also gratefully acknowledge SDI Ltd. Bayswater, Victoria, Australia, for a generous donation of the adhesive ZipBond X used in this study. Paula Maciel Pires was undertaking a PhD exchange program at Cardenal Herrera University during a part of the experimental assay and was supported by a CAPES grant from Brazil (grant numbers 88882.424807/2018-01 and 88881.188518/2018-01).
Funding
The research facilities of this study were supported by grants “Ministerio de Ciencia, Innovación y Universidades (PID2020-120346 GB-I00) and Universidad CEU-Cardenal Herrera (Programa FUSP CEU-Santander 2019–2020)” (PI: SS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required. Human molars used in this study were collected according to the guidelines of the local Ethics Committee (CEI20/098).
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maciel Pires, P., Dávila-Sánchez, A., Faus-Matoses, V. et al. Bonding performance and ultramorphology of the resin-dentine interface of contemporary universal adhesives. Clin Oral Invest 26, 4391–4405 (2022). https://doi.org/10.1007/s00784-022-04402-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04402-3