Abstract
Objective
We aimed to develop a tool for virtual orthodontic bracket removal based on deep learning algorithms for feature extraction from bonded teeth and to demonstrate its application in a bracket position assessment scenario.
Materials and methods
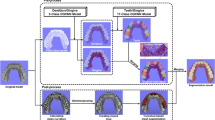
Our segmentation network for virtual bracket removal was trained using dataset A, containing 978 bonded teeth, 20 original teeth, and 20 brackets generated by scanners. The accuracy and segmentation time of the network were tested by dataset B, which included an additional 118 bonded teeth without knowing the original tooth morphology. This tool was then applied for bracket position assessment. The clinical crown center, bracket center, and orientations of separated teeth and brackets were extracted for analyzing the linear distribution and angular deviation of bonded brackets.
Results
This tool performed virtual bracket removal in 2.9 ms per tooth with accuracies of 98.93% and 97.42% (P < 0.01) in datasets A and B, respectively. The tooth surface and bracket characteristics were extracted and used to evaluate the results of manually bonded brackets by 49 orthodontists. Personal preferences for bracket angulation and bracket distribution were displayed graphically and tabularly.
Conclusions
The tool's efficiency and precision are satisfactory, and it can be operated without original tooth data. It can be used to display the bonding deviation in the bracket position assessment scenario.
Clinical significance
With the aid of this tool, unnecessary bracket removal can be avoided when evaluating bracket positions and modifying treatment plans. It has the potential to produce retainers and orthodontic devices prior to tooth debonding.





Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Panayi NC, Tsolakis AI, Athanasiou AE (2020) Digital assessment of direct and virtual indirect bonding of orthodontic brackets: A clinical prospective cross-sectional comparative investigation. Int Orthod 18:714–721. https://doi.org/10.1016/j.ortho.2020.09.007
Marsh K, Weissheimer A, Yin K, Chamberlain-Umanoff A, Tong H, Sameshima GT (2021) Three-dimensional assessment of virtual bracket removal for orthodontic retainers: A prospective clinical study. Am J Orthod Dentofacial Orthop 160:302–311. https://doi.org/10.1016/j.ajodo.2020.09.027
Nakada N, Uchida Y, Inaba M, Kaetsu R, Shimizu N, Namura Y, Motoyoshi M (2021) Pain and removal force associated with bracket debonding: a clinical study. J Appl Oral Sci 29:e20200879. https://doi.org/10.1590/1678-7757-2020-0879
Israel M, Kusnoto B, Evans CA, Begole E (2011) A comparison of traditional and computer-aided bracket placement methods. Angle Orthod 81:828–835. https://doi.org/10.2319/072110-425.1
Duarte MEA, Gribel BF, Spitz A, Artese F, Miguel JAM (2020) Reproducibility of digital indirect bonding technique using three-dimensional (3D) models and 3D-printed transfer trays. Angle Orthod 90:92–99. https://doi.org/10.2319/030919-176.1
Möhlhenrich SC, Alexandridis C, Peters F, Kniha K, Modabber A, Danesh G, Fritz U (2020) Three-dimensional evaluation of bracket placement accuracy and excess bonding adhesive depending on indirect bonding technique and bracket geometry: an in-vitro study. Head Face Med 16:17. https://doi.org/10.1186/s13005-020-00231-5
Faus-Matoses I, Guinot Barona C, Zubizarreta-Macho Á, Paredes-Gallardo V, Faus-Matoses V (2021) A Novel Digital Technique for Measuring the Accuracy of an Indirect Bonding Technique Using Fixed Buccal Multibracket Appliances. J Pers Med 11:932. https://doi.org/10.3390/jpm11090932
Adel SM, Vaid NR, El-Harouni N, Kassem H, Zaher AR (2022) TIP, TORQUE & ROTATIONS: How accurately do digital superimposition software packages quantify tooth movement? Prog Orthod 23:8. https://doi.org/10.1186/s40510-022-00402-x
Adel SM, Vaid NR, El-Harouni N, Kassem H, Zaher AR (2022) Digital model superimpositions: are different software algorithms equally accurate in quantifying linear tooth movements? BMC Oral Health 22:103. https://doi.org/10.1186/s12903-022-02129-x
Adel SM, Vaid NR, El-Harouni N, Kassem H, Park JH, Zaher AR (2023) Quantifying maxillary anterior tooth movement in digital orthodontics: Does the choice of the superimposition software matter? J World Fed Orthod 12:187–196. https://doi.org/10.1016/j.ejwf.2023.07.002
Vollmer S, Mateen BA, Bohner G, Király FJ, Ghani R, Jonsson P, Cumbers S, Jonas A, McAllister KSL, Myles P, Granger D, Birse M, Branson R, Moons KGM, Collins GS, Ioannidis JPA, Holmes C, Hemingway H (2020) Machine learning and artificial intelligence research for patient benefit: 20 critical questions on transparency, replicability, ethics, and effectiveness. Bmj 368:l6927. https://doi.org/10.1136/bmj.l6927
Schwendicke F, Golla T, Dreher M, Krois J (2019) Convolutional neural networks for dental image diagnostics: A scoping review. J Dent 91:103226. https://doi.org/10.1016/j.jdent.2019.103226
Casalegno F, Newton T, Daher R, Abdelaziz M, Lodi-Rizzini A, Schürmann F, Krejci I, Markram H (2019) Caries Detection with Near-Infrared Transillumination Using Deep Learning. J Dent Res 98:1227–1233. https://doi.org/10.1177/0022034519871884
Schwendicke F, Singh T, Lee JH, Gaudin R, Chaurasia A, Wiegand T, Uribe S, Krois J (2021) Artificial intelligence in dental research: Checklist for authors, reviewers, readers. J Dent 107:103610. https://doi.org/10.1016/j.jdent.2021.103610
Jandoo T (2020) WHO guidance for digital health: What it means for researchers. Digit Health 6:2055207619898984. https://doi.org/10.1177/2055207619898984
Leite AF, Gerven AV, Willems H, Beznik T, Lahoud P, Gaêta-Araujo H, Vranckx M, Jacobs R (2021) Artificial intelligence-driven novel tool for tooth detection and segmentation on panoramic radiographs. Clin Oral Investig 25:2257–2267. https://doi.org/10.1007/s00784-020-03544-6
Liu MQ, Xu ZN, Mao WY, Li Y, Zhang XH, Bai HL, Ding P, Fu KY (2022) Deep learning-based evaluation of the relationship between mandibular third molar and mandibular canal on CBCT. Clin Oral Investig 26:981–991. https://doi.org/10.1007/s00784-021-04082-5
Moidu NP, Sharma S, Chawla A, Kumar V, Logani A (2022) Deep learning for categorization of endodontic lesion based on radiographic periapical index scoring system. Clin Oral Investig 26:651–658. https://doi.org/10.1007/s00784-021-04043-y
Wang H, Minnema J, Batenburg KJ, Forouzanfar T, Hu FJ, Wu G (2021) Multiclass CBCT Image Segmentation for Orthodontics with Deep Learning. J Dent Res 100:943–949. https://doi.org/10.1177/00220345211005338
Zhao C, Chen Q, Yu S, Xu C, Li X, Zhang C, Gao L (2020) Effect of interleukin-22 on osteogenic differentiation and the osteoclastogenic response of human periodontal ligament fibroblasts in vitro. J Periodontol 91:1085–1097. https://doi.org/10.1002/jper.19-0470
Takeda S, Mine Y, Yoshimi Y, Ito S, Tanimoto K, Murayama T (2021) Landmark annotation and mandibular lateral deviation analysis of posteroanterior cephalograms using a convolutional neural network. J Dent Sci 16:957–963. https://doi.org/10.1016/j.jds.2020.10.012
Spampinato C, Palazzo S, Giordano D, Aldinucci M, Leonardi R (2017) Deep learning for automated skeletal bone age assessment in X-ray images. Med Image Anal 36:41–51. https://doi.org/10.1016/j.media.2016.10.010
Bichu YM, Hansa I, Bichu AY, Premjani P, Flores-Mir C, Vaid NR (2021) Applications of artificial intelligence and machine learning in orthodontics: a scoping review. Prog Orthod 22:18. https://doi.org/10.1186/s40510-021-00361-9
Schwendicke F, Chaurasia A, Arsiwala L, Lee JH, Elhennawy K, Jost-Brinkmann PG, Demarco F, Krois J (2021) Deep learning for cephalometric landmark detection: systematic review and meta-analysis. Clin Oral Investig 25:4299–4309. https://doi.org/10.1007/s00784-021-03990-w
Xu X, Liu C, Zheng Y (2019) 3D Tooth Segmentation and Labeling Using Deep Convolutional Neural Networks. IEEE Trans Vis Comput Graph 25:2336–2348. https://doi.org/10.1109/tvcg.2018.2839685
Cui Z, Li C, Wang W (2019) ToothNet: automatic tooth instance segmentation and identification from cone beam CT images. 2019 IEEE/CVF Conference on Computer Vision and Pattern Recognition (CVPR), Long Beach, CA, USA, 2019, pp 6361–6370. https://doi.org/10.1109/CVPR.2019.00653
Chan HP, Samala RK, Hadjiiski LM, Zhou C (2020) Deep Learning in Medical Image Analysis. Adv Exp Med Biol 1213:3–21. https://doi.org/10.1007/978-3-030-33128-3_1
Sardarian A, Danaei SM, Shahidi S, Boushehri SG, Geramy A (2014) The effect of vertical bracket positioning on torque and the resultant stress in the periodontal ligament–a finite element study. Prog Orthod 15:50. https://doi.org/10.1186/s40510-014-0050-0
Andrews LF (1979) The straight-wire appliance. Br J Orthod 6:125–143. https://doi.org/10.1179/bjo.6.3.125
Mazzeo F, Marchese E, Assumma V, Sepe J, Perillo L (2013) A new device (FAQ.FIX®) for orthodontic bracket placement in straight wire technique. Prog Orthod 14:23. https://doi.org/10.1186/2196-1042-14-23
Charles RQ, Su H, Kaichun M, Guibas LJ (2017) PointNet: deep learning on point sets for 3D classification and segmentation. 2017 IEEE Conference on Computer Vision and Pattern Recognition (CVPR), Honolulu, HI, USA, 2017, pp 77–85. https://doi.org/10.1109/CVPR.2017.16
Wu TH, Lian C, Lee S, Pastewait M, Piers C, Liu J, Wang F, Wang L, Chiu CY, Wang W, Jackson C, Chao WL, Shen D, Ko CC (2022) Two-Stage Mesh Deep Learning for Automated Tooth Segmentation and Landmark Localization on 3D Intraoral Scans. IEEE Trans Med Imaging 41:3158–3166. https://doi.org/10.1109/tmi.2022.3180343
Besl PJ, McKay ND (1992) A method for registration of 3-D shapes. IEEE Trans Pattern Anal Mach Intell 14:239–256. https://doi.org/10.1109/34.121791
Schwendicke F, Samek W, Krois J (2020) Artificial Intelligence in Dentistry: Chances and Challenges. J Dent Res 99:769–774. https://doi.org/10.1177/0022034520915714
Budd S, Robinson EC, Kainz B (2021) A survey on active learning and human-in-the-loop deep learning for medical image analysis. Med Image Anal 71:102062. https://doi.org/10.1016/j.media.2021.102062
Mangano F, Gandolfi A, Luongo G, Logozzo S (2017) Intraoral scanners in dentistry: a review of the current literature. BMC Oral Health 17:149. https://doi.org/10.1186/s12903-017-0442-x
Liu J, Hao J, Lin H, Pan W, Yang J, Feng Y, Wang G, Li J, Jin Z, Zhao Z, Liu Z (2023) Deep learning-enabled 3D multimodal fusion of cone-beam CT and intraoral mesh scans for clinically applicable tooth-bone reconstruction. Patterns (N Y) 4(9):100825 https://doi.org/10.1016/j.patter.2023.100825
Balki I, Amirabadi A, Levman J, Martel AL, Emersic Z, Meden B, Garcia-Pedrero A, Ramirez SC, Kong D, Moody AR, Tyrrell PN (2019) Sample-Size Determination Methodologies for Machine Learning in Medical Imaging Research: A Systematic Review. Can Assoc Radiol J 70:344–353. https://doi.org/10.1016/j.carj.2019.06.002
Al-Jewair TS, Azarpazhooh A, Suri S, Shah PS (2009) Computer-assisted learning in orthodontic education: a systematic review and meta-analysis. J Dent Educ 73:730–739
Johal A, Bourauel C, Moghanchi S, Dickerson T, Gaudin P, Elliott EL (2022) The Tip and Torque adjustable bracket as a new concept in design. Angle Orthod 92:380–387. https://doi.org/10.2319/061421-474.1
Song J, Kim M (2020) Accuracy on Scanned Images of Full Arch Models with Orthodontic Brackets by Various Intraoral Scanners in the Presence of Artificial Saliva. Biomed Res Int 2020:2920804. https://doi.org/10.1155/2020/2920804
Shin SH, Yu HS, Cha JY, Kwon JS, Hwang CJ (2021) Scanning Accuracy of Bracket Features and Slot Base Angle in Different Bracket Materials by Four Intraoral Scanners: An In Vitro Study. Materials (Basel) 14:365. https://doi.org/10.3390/ma14020365
Koo BC, Chung CH, Vanarsdall RL (1999) Comparison of the accuracy of bracket placement between direct and indirect bonding techniques. Am J Orthod Dentofacial Orthop 116:346–351. https://doi.org/10.1016/s0889-5406(99)70248-9
Park JH, Choi JY, Oh SH, Kim SH (2021) Three-Dimensional Digital Superimposition of Orthodontic Bracket Position by Using a Computer-Aided Transfer Jig System: An Accuracy Analysis. Sensors (Basel) 21:9511. https://doi.org/10.3390/s21175911
Armstrong D, Shen G, Petocz P, Darendeliler MA (2007) A comparison of accuracy in bracket positioning between two techniques–localizing the centre of the clinical crown and measuring the distance from the incisal edge. Eur J Orthod 29:430–436. https://doi.org/10.1093/ejo/cjm037
Balut N, Klapper L, Sandrik J, Bowman D (1992) Variations in bracket placement in the preadjusted orthodontic appliance. Am J Orthod Dentofacial Orthop 102:62–67. https://doi.org/10.1016/0889-5406(92)70015-3
El-Timamy AM, El-Sharaby FA, Eid FH, Mostafa YA (2016) Three-dimensional imaging for indirect-direct bonding. Am J Orthod Dentofacial Orthop 149:928–931. https://doi.org/10.1016/j.ajodo.2015.12.009
Andrews LF (1972) The six keys to normal occlusion. Am J Orthod 62:296–309. https://doi.org/10.1016/s0002-9416(72)90268-0
Silverman E, Cohen M, Gianelly AA, Dietz VS (1972) A universal direct bonding system for both metal and plastic brackets. Am J Orthod 62:236–244. https://doi.org/10.1016/s0002-9416(72)90264-3
Zachrisson BU, Brobakken BO (1978) Clinical comparison of direct versus indirect bonding with different bracket types and adhesives. Am J Orthod 74:62–78. https://doi.org/10.1016/0002-9416(78)90046-5
Nichols DA, Gardner G, Carballeyra AD (2013) Reproducibility of bracket positioning in the indirect bonding technique. Am J Orthod Dentofacial Orthop 144:770–776. https://doi.org/10.1016/j.ajodo.2013.04.023
Xie X, Niu J, Liu X, Chen Z, Tang S, Yu S (2021) A survey on incorporating domain knowledge into deep learning for medical image analysis. Med Image Anal 69:101985. https://doi.org/10.1016/j.media.2021.101985
Hodge TM, Dhopatkar AA, Rock WP, Spary DJ (2004) A randomized clinical trial comparing the accuracy of direct versus indirect bracket placement. J Orthod 31:132–137. https://doi.org/10.1179/146531204225020427
Littlewood SJ, Millett DT, Doubleday B, Bearn DR, Worthington HV (2016) Retention procedures for stabilising tooth position after treatment with orthodontic braces. Cochrane Database Syst Rev 2016:Cd002283. https://doi.org/10.1002/14651858.CD002283.pub4
Funding
This study was funded by the Science and Technology Commission of Shanghai Municipality [Grand numbers 19441906200 and 18441903600], Clinical Research Plan of SHDC [Grand number SHDC2020CR3009A], Shanghai Rising-Star Program [Grand number 19QA1405200], Innovative Research Team of High-Level Local Universities in Shanghai [Grand number SSMU-ZDCX20180902], Young Doctor Collaborative Innovation Team of Ninth People's Hospital Affiliated to Shanghai Jiao Tong University, School of Medicine [Grand number QC2018-02], Innovative Research Team of High-Level Local Universities in Shanghai [SHSMU-ZLCX20212402] and the CSA Clinical Research Fund [CSA-O2020-04] for financial support. Cross Disciplinary Research Fund from Shanghai Ninth People's Hospital, Shanghai Jiao Tong University School of Medicine [JYJC202130].
Author information
Authors and Affiliations
Contributions
LR contributed to conceptualization, methodology, formal analysis, investigation, writing—original draft, and visualization. ZC contributed to validation, formal analysis, investigation, data curation, writing—review & editing, and visualization. CF contributed to conceptualization, methodology, validation, investigation, resources, and writing—review & editing.
YQ contributed to methodology, validation, resources, data curation, and visualization. FD contributed to methodology, software, writing—review & editing, and validation. ON contributed to investigation, and writing—review & editing. JY contributed to investigation and writing—review & editing. GW contributed to investigation and writing—review & editing. XL contributed to validation, writing—review & editing, and supervision. FQ contributed to validation, writing—review & editing, supervision, and project administration.
FB contributed to validation, writing—review & editing, supervision, and funding acquisition.
Corresponding authors
Ethics declarations
Ethics approval
The study was approved by the Independent Ethics Committee of the Shanghai Ninth People’s Hospital affiliated twith Shanghai Jiao Tong University, School of Medicine (SH9H-2021-T360-1).
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Conflict of interests
The authors declare no potential conflicts of interest with respect to the authorship and/or publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Ruomei Li and Cheng Zhu joint first authors.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, R., Zhu, C., Chu, F. et al. Deep learning for virtual orthodontic bracket removal: tool establishment and application. Clin Oral Invest 28, 121 (2024). https://doi.org/10.1007/s00784-023-05440-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00784-023-05440-1