Abstract
Objectives
The objective of our study was to develop and validate a deep learning approach based on convolutional neural networks (CNNs) for automatic detection of the mandibular third molar (M3) and the mandibular canal (MC) and evaluation of the relationship between them on CBCT.
Materials and methods
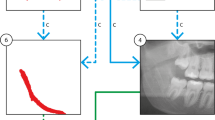
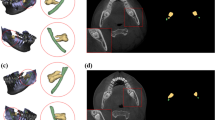
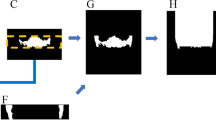
A dataset of 254 CBCT scans with annotations by radiologists was used for the training, the validation, and the test. The proposed approach consisted of two modules: (1) detection and pixel-wise segmentation of M3 and MC based on U-Nets; (2) M3-MC relation classification based on ResNet-34. The performances were evaluated with the test set. The classification performance of our approach was compared with two residents in oral and maxillofacial radiology.
Results
For segmentation performance, the M3 had a mean Dice similarity coefficient (mDSC) of 0.9730 and a mean intersection over union (mIoU) of 0.9606; the MC had a mDSC of 0.9248 and a mIoU of 0.9003. The classification models achieved a mean sensitivity of 90.2%, a mean specificity of 95.0%, and a mean accuracy of 93.3%, which was on par with the residents.
Conclusions
Our approach based on CNNs demonstrated an encouraging performance for the automatic detection and evaluation of the M3 and MC on CBCT.
Clinical relevance
An automated approach based on CNNs for detection and evaluation of M3 and MC on CBCT has been established, which can be utilized to improve diagnostic efficiency and facilitate the precision diagnosis and treatment of M3.





Similar content being viewed by others
References
Gulicher D, Gerlach KL (2001) Sensory impairment of the lingual and inferior alveolar nerves following removal of impacted mandibular third molars. Int J Oral Maxillofac Surg 30:306–312. https://doi.org/10.1054/ijom.2001.0057
Leung YY, Cheung LK (2011) Risk factors of neurosensory deficits in lower third molar surgery: a literature review of prospective studies. Int J Oral Maxillofac Surg 40:1–10. https://doi.org/10.1016/j.ijom.2010.09.005
Ghaeminia H, Meijer GJ, Soehardi A, Borstlap WA, Mulder J, Berge SJ (2009) Position of the impacted third molar in relation to the mandibular canal. Diagnostic accuracy of cone beam computed tomography compared with panoramic radiography. Int J Oral Maxillofac Surg 38:964–971. https://doi.org/10.1016/j.ijom.2009.06.007
Tay AB, Go WS (2004) Effect of exposed inferior alveolar neurovascular bundle during surgical removal of impacted lower third molars. J Oral Maxillofac Surg 62:592–600. https://doi.org/10.1016/j.joms.2003.08.033
Kim JW, Cha IH, Kim SJ, Kim MR (2012) Which risk factors are associated with neurosensory deficits of inferior alveolar nerve after mandibular third molar extraction? J Oral Maxillofac Surg 70:2508–2514. https://doi.org/10.1016/j.joms.2012.06.004
Tantanapornkul W, Okouchi K, Fujiwara Y, Yamashiro M, Maruoka Y, Ohbayashi N, Kurabayashi T (2007) A comparative study of cone-beam computed tomography and conventional panoramic radiography in assessing the topographic relationship between the mandibular canal and impacted third molars. Oral Surg Oral Med Oral Pathol Oral Radiol 103:253–259. https://doi.org/10.1016/j.tripleo.2006.06.060
De VW, Casselman J, Swennen GR (2009) Cone-beam computerized tomography (CBCT) imaging of the oral and maxillofacial region: a systematic review of the literature. Int J Oral Maxillofac Surg 38:609–625. https://doi.org/10.1016/j.ijom.2009.02.028
Patel PS, Shah JS, Dudhia BB, Butala PB, Jani YV, Macwan RS (2020) Comparison of panoramic radiograph and cone beam computed tomography findings for impacted mandibular third molar root and inferior alveolar nerve canal relation. Indian J Dent Res 31:91–102. https://doi.org/10.4103/ijdr.IJDR_540_18
Ghaeminia H, Meijer GJ, Soehardi A, Borstlap WA, Mulder J, Vlijmen OJ, Berge SJ, Maal TJ (2011) The use of cone beam CT for the removal of wisdom teeth changes the surgical approach compared with panoramic radiography: a pilot study. Int J Oral Maxillofac Surg 40:834–839. https://doi.org/10.1016/j.ijom.2011.02.032
Buchanan A, Thachil K, Haggard C, Kalathingal S (2017) Predoctoral and postdoctoral education on cone-beam computed tomography. J Evid Based Dent Pract 17:310–316. https://doi.org/10.1016/j.jebdp.2017.05.002
Rumpa G, Aruna R (2014) Systematic interpretation of CBCT scans: why do it? J Mass Dent Soc 62:68–70
Gulshan V, Peng L, Coram M, Stumpe MC, Wu D, Narayanaswamy A, Venugopalan S, Widner K, Madams T, Cuadros J, Kim R, Raman R, Nelson PC, Mega JL, Webster DR (2016) Development and validation of a deep learning algorithm for detection of diabetic retinopathy in retinal fundus photographs. JAMA 316:2402–2410. https://doi.org/10.1001/jama.2016.17216
Esteva A, Kuprel B, Novoa RA, Ko J, Swetter SM, Blau HM, Thrun S (2017) Dermatologist-level classification of skin cancer with deep neural networks. Nature 542:115–118. https://doi.org/10.1038/nature21056
Hiraiwa T, Ariji Y, Fukuda M, Kise Y, Nakata K, Katsumata A, Fujita H, Ariji E (2019) A deep-learning artificial intelligence system for assessment of root morphology of the mandibular first molar on panoramic radiography. Dentomaxillofac Radiol 48:20180218. https://doi.org/10.1259/dmfr.20180218
Kwak GH, Kwak EJ, Song JM, Park HR, Jung YH, Cho BH, Hui P, Hwang JJ (2020) Automatic mandibular canal detection using a deep convolutional neural network. Sci Rep 10:5711. https://doi.org/10.1038/s41598-020-62586-8
Miki Y, Muramatsu C, Hayashi T, Zhou X, Hara T, Katsumata A, Fujita H (2017) Classification of teeth in cone-beam CT using deep convolutional neural network. Comput Biol Med 80:24–29. https://doi.org/10.1016/j.compbiomed.2016.11.003
Silva G, Oliveira L, Pithon M (2018) Automatic segmenting teeth in X-ray images: Trends, a novel data set, benchmarking and future perspectives. Expert Syst Appl 107:15–31. https://doi.org/10.1016/j.eswa.2018.04.001
Vinayahalingam S, Xi T, Berge S, Maal T, de Jong G (2019) Automated detection of third molars and mandibular nerve by deep learning. Sci Rep 9:9007. https://doi.org/10.1038/s41598-019-45487-3
Casalegno F, Newton T, Daher R, Abdelaziz M, Lodi-Rizzini A, Schürmann F, Krejci I, Markram H (2019) Caries detection with near-infrared transillumination using deep learning. J Dent Res 98:1227–1233. https://doi.org/10.1177/0022034519871884
Lee JH, Kim DH, Jeong SN, Choi SH (2018) Detection and diagnosis of dental caries using a deep learning-based convolutional neural network algorithm. J Dent 77:106–111. https://doi.org/10.1016/j.jdent.2018.07.015
Patil S, Kulkarni V, Bhise A (2019) Algorithmic analysis for dental caries detection using an adaptive neural network architecture. Heliyon 5:e01579. https://doi.org/10.1016/j.heliyon.2019.e01579
Srivastava M, Kumar P, Pradhan L, Varadarajan S (2017) Detection of tooth caries in bitewing radiographs using deep learning. arXiv preprint arXiv:1711.07312. https://arxiv.org/abs/1711.07312
Ekert T, Krois J, Meinhold L, Elhennawy K, Emara R, Golla T, Schwendicke F (2019) Deep learning for the radiographic detection of apical lesions. J Endod 45:917-922.e5. https://doi.org/10.1016/j.joen.2019.03.016
Lee JH, Kim DH, Jeong SN, Choi SH (2018) Diagnosis and prediction of periodontally compromised teeth using a deep learning-based convolutional neural network algorithm. J Periodontal Implant Sci 48:114–123. https://doi.org/10.5051/jpis.2018.48.2.114
Lee JH, Kim DH, Jeong SN (2020) Diagnosis of cystic lesions using panoramic and cone beam computed tomographic images based on deep learning neural network. Oral Dis 26:152–158. https://doi.org/10.1111/odi.13223
Kwon O, Yong TH, Kang SR, Kim JE, Huh KH, Heo MS, Lee SS, Choi SC, Yi WJ (2020) Automatic diagnosis for cysts and tumors of both jaws on panoramic radiographs using a deep convolution neural network. Dentomaxillofac Radiol 49:20200185. https://doi.org/10.1259/dmfr.20200185
Murata M, Ariji Y, Ohashi Y, Kawai T, Fukuda M, Funakoshi T, KiMase Y, Nozawa M, Katsumata A, Fujita H, Ariji E (2019) Deep-learning classification using convolutional neural network for evaluation of maxillary sinusitis on panoramic radiography. Oral Radiol 35:301–307. https://doi.org/10.1007/s11282-018-0363-7
Arık S, Ibragimov B, Xing L (2017) Fully automated quantitative cephalometry using convolutional neural networks. J Med Imaging (Bellingham) 4:014501. https://doi.org/10.1117/1.jmi.4.1.014501
Yu HJ, Cho SR, Kim MJ, Kim WH, Kim JW, Choi J (2020) Automated skeletal classification with lateral cephalometry based on artificial intelligence. J Dent Res 99:249–256. https://doi.org/10.1177/0022034520901715
Jaskari J, Sahlsten J, Järnstedt J, Mehtonen H, Karhu K, Sundqvist O, Hietanen A, Varjonen V, Mattila V, Kaski K (2020) Deep learning method for mandibular canal segmentation in dental cone beam computed tomography volumes. Sci Rep 10:5842. https://doi.org/10.1038/s41598-020-62321-3
Banar N, Bertels J, Laurent F, Boedi RM, De Tobel J, Thevissen P, Vandermeulen D (2020) Towards fully automated third molar development staging in panoramic radiographs. Int J Legal Med 134:1831–1841. https://doi.org/10.1007/s00414-020-02283-3
Merdietio Boedi R, Banar N, De Tobel J, Bertels J, Vandermeulen D, Thevissen PW (2020) Effect of lower third molar segmentations on automated tooth development staging using a convolutional neural network. J Forensic Sci 65:481–486. https://doi.org/10.1111/1556-4029.14182
Vranckx M, Van Gerven A, Willems H, Vandemeulebroucke A, Ferreira Leite A, Politis C, Jacobs R (2020) Artificial intelligence (AI)-driven molar angulation measurements to predict third molar eruption on panoramic radiographs. Int J Environ Res Public Health 17:3716. https://doi.org/10.3390/ijerph17103716
Fukuda M, Ariji Y, Kise Y, Nozawa M, Kuwada C, Funakoshi T, Muramatsu C, Fujita H, Katsumata A, Ariji E (2020) Comparison of 3 deep learning neural networks for classifying the relationship between the mandibular third molar and the mandibular canal on panoramic radiographs. Oral Surg Oral Med Oral Pathol Oral Radiol 130:336–343. https://doi.org/10.1016/j.oooo.2020.04.005
Yoo JH, Yeom HG, Shin WS, Yun JP, Lee JH, Jeong SH, Lim HJ, Lee J, Kim BC (2021) Deep learning based prediction of extraction difficulty for mandibular third molars. Sci Rep 11:1954. https://doi.org/10.1038/s41598-021-81449-4
Orhan K, Bilgir E, Bayrakdar IS, Ezhov M, Gusarev M, Shumilov E (2020) Evaluation of artificial intelligence for detecting impacted third molars on cone-beam computed tomography scans. J Stomatol Oral Maxillofac Surg S2468–7855(20):30303–30307. https://doi.org/10.1016/j.jormas.2020.12.006
Ronneberger O, Fischer P, Brox T (2015) U-net: convolutional networks for biomedical image segmentation. Springer, Cham. https://doi.org/10.1007/978-3-319-24574-4_28
He K, Zhang X, Ren S, Sun J (2016) Deep residual learning for image recognition. In: Proceedings of the IEEE conference on computer vision and pattern recognition, pp 770–778. https://doi.org/10.1109/CVPR.2016.90
Szegedy C, Vanhoucke V, Ioffe S, Shlens J, Wojna Z (2016) Rethinking the inception architecture for computer vision. In: Proceedings of the IEEE conference on computer vision and pattern recognition, pp 2818–2826. https://doi.org/10.1109/CVPR.2016.308
Menon AK, Jayasumana S, Rawat AS, Jain H, Veit A, Kumar S (2020) Long-tail learning via logit adjustment. arXiv preprint arXiv:2007.07314. https://arxiv.org/abs/2007.07314
Taghanaki SA, Zheng Y, Kevin Zhou S, Georgescu B, Sharma P, Xu D, Comaniciu D, Hamarneh G (2019) Combo loss: handling input and output imbalance in multi-organ segmentation. Comput Med Imaging Graph 75:24–33. https://doi.org/10.1016/j.compmedimag.2019.04.005
Kingma DP, Ba J (2014) Adam: a method for stochastic optimization. arXiv preprint arXiv:1412.6980. https://arxiv.org/abs/1412.6980
Dice LR (1945) Measures of the amount of ecologic association between species. Ecology 26:297–302. https://doi.org/10.2307/1932409
Russakovsky O, Deng J, Su H, Krause J, Satheesh S, Ma S, Huang Z, Karpathy A, Khosla A, Bernstein M, BergLi ACFF (2015) Imagenet large scale visual recognition challenge. Int J Comput Vis 115:211–252. https://doi.org/10.1007/s11263-015-0816-y
Matzen LH, Berkhout E (2019) Cone beam CT imaging of the mandibular third molar: a position paper prepared by the European Academy of DentoMaxilloFacial Radiology (EADMFR). Dentomaxillofac Radiol 48(5):20190039. https://doi.org/10.1259/dmfr.20190039
Qi W, Lei J, Liu YN, Li JN, Pan J, Yu GY (2019) Evaluating the risk of post-extraction inferior alveolar nerve injury through the relative position of the lower third molar root and inferior alveolar canal. Int J Oral Maxillofac Surg 48:1577–1583. https://doi.org/10.1016/j.ijom.2019.07.008
Sklavos A, Delpachitra S, Jaunay T, Kumar R, Chandu A (2021) Degree of compression of the inferior alveolar canal on cone-beam computed tomography and outcomes of postoperative nerve injury in mandibular third molar surgery. J Oral Maxillofac Surg 79:974–980. https://doi.org/10.1016/j.joms.2020.12.049
Szalma J, Vajta L, Lovász BV, Kiss C, Soós B, Lempel E (2020) Identification of specific panoramic high-risk signs in impacted third molar cases in which cone beam computed tomography changes the treatment decision. J Oral Maxillofac Surg 78:1061–1070. https://doi.org/10.1016/j.joms.2020.03.012
Mendonça LM, Gaêta-Araujo H, Cruvinel PB, Tosin IW, Azenha MR, Ferraz EP, Oliveira-Santos C, Tirapelli C (2020) Can diagnostic changes caused by cone beam computed tomography alter the clinical decision in impacted lower third molar treatment plan? Dentomaxillofac Radiol 50(4):20200412. https://doi.org/10.1259/dmfr.20200412
Funding
This study was supported by the Program for New Clinical Techniques and Therapies of Peking University School and Hospital of Stomatology (no. PKUSSNCT-19B08).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Institutional Review Board of Peking University School and Hospital of Stomatology and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the Institutional Review Board of Peking University School and Hospital of Stomatology (PKUSSIRB-201949131).
Informed consent
Written informed consent was not required for this study because all the included patients were collected retrospectively. Exemption of informed consent will not affect the rights and health of included patients. The application for free informed consent has been approved by the Institutional Review Board.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, MQ., Xu, ZN., Mao, WY. et al. Deep learning-based evaluation of the relationship between mandibular third molar and mandibular canal on CBCT. Clin Oral Invest 26, 981–991 (2022). https://doi.org/10.1007/s00784-021-04082-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04082-5