Abstract
Objective
To investigate the antibacterial and enamel remineralization performances as well as physicochemical properties and biocompatibility of a fluoride-coated clear aligner plastic (FCAP).
Materials and methods
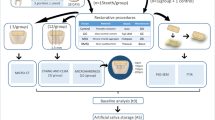
FCAP and normal clear aligner plastic (CAP) was bought from the manufacturer (Angelalign Technology Inc, China). The FCAP was observed under scanning electron microscopy. Its element composition, resistance to separation, contact angle, and protein adhesion performance were characterized. Colony-forming unit (CFU) count and 3-(4,5)-dimethylthiazol(-z-y1)-3,5-diphenyltetrazolium bromide (MTT) assay were used to evaluate the antibacterial ability of Streptococcus mutans. Fluoride release-recharge patterns were obtained. Apatite formation was evaluated after immersing FCAP in artificial saliva. Enamel remineralization capability was evaluated in the demineralization model (immersing samples in demineralization solution for 36 h) and pH cycling model (immersing samples in demineralization solution and remineralization solution in turns for 14 days). Cell Counting Kit-8 (CCK-8) and live/dead cell staining kits were used for cytotoxicity assay.
Results
The FCAP showed uniformly distributed fluoride and did not compromise protein adhesion performance. CFU count (5.47 ± 0.55 for CAP, 3.63 ± 0.38 for FCAP) and MTT assay (0.41 ± 0.025 for CAP, 0.28 ± 0.038) indicated that the FCAP had stronger antibacterial activity compared with normal CAP (P < 0.05 for both evaluations). The FCAP could release fluoride continuously for 14 days and could be recharged after immersing in NaF solution. The FCAP could induce the formation of hydroxyapatite in artificial saliva and could reduce the microhardness decrease, color change, and mineral loss of enamels in both two models (P < 0.05 for all evaluations). CCK-8 and live/dead cell staining analyses showed that the coating did not compromise the biocompatibility of the clear aligner (P > 0.05 for CCK-8 evaluation).
Conclusions
The FCAP had antibacterial, fluoride recharge, and enamel remineralization abilities while it did not compromise physicochemical properties and biocompatibility.
Clinical relevance
The FCAP has the potential to prevent enamel demineralization during clear aligner treatment.








Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
References
Proffit WR, Fields HW, Larson Be, Sarver DM (2018) Contemporary orthodontics. Sixth ed. Mosby, Saint Louis
Weir T (2017) Clear aligners in orthodontic treatment. Aust Dent J 62(Suppl 1):58–62. https://doi.org/10.1111/adj.12480
Schaefer I, Braumann B (2010) Halitosis, Oral health and quality of life during treatment with Invisalign(®) and the effect of a low-dose chlorhexidine solution. J Orofac Orthop 71:430–441. https://doi.org/10.1007/s00056-010-1040-6
Fujiyama K, Honjo T, Suzuki M, Matsuoka S, Deguchi T (2014) Analysis of pain level in cases treated with Invisalign aligner: comparison with fixed edgewise appliance therapy. Prog Orthod 15:64. https://doi.org/10.1186/s40510-014-0064-7
Rosvall MD, Fields HW, Ziuchkovski J, Rosenstiel SF, Johnston WM (2009) Attractiveness, acceptability, and value of orthodontic appliances. Am J Orthod Dentofacial Orthop 135:276.e1–12. https://doi.org/10.1016/j.ajodo.2008.09.020. (discussion 276-277)
Buschang PH, Shaw SG, Ross M, Crosby D, Campbell PM (2014) Comparative time efficiency of aligner therapy and conventional edgewise braces. Angle Orthod 84:391–396. https://doi.org/10.2319/062113-466
Rossini G, Parrini S, Castroflorio T, Deregibus A, Debernardi CL (2015) Efficacy of clear aligners in controlling orthodontic tooth movement: a systematic review. Angle Orthod 85:881–889. https://doi.org/10.2319/061614-436.1
Fang D, Li F, Zhang Y, Bai Y, Wu BM (2020) Changes in mechanical properties, surface morphology, structure, and composition of Invisalign material in the oral environment. Am J Orthod Dentofacial Orthop 157:745–753. https://doi.org/10.1016/j.ajodo.2019.05.023
Moshiri M, Eckhart JE, McShane P, German DS (2013) Consequences of poor oral hygiene during aligner therapy. J Clin Orthod 47:494–498
Julien KC, Buschang PH, Campbell PM (2013) Prevalence of white spot lesion formation during orthodontic treatment. Angle Orthod 83:641–647. https://doi.org/10.2319/071712-584.1
Lucchese A, Gherlone E (2013) Prevalence of white-spot lesions before and during orthodontic treatment with fixed appliances. Eur J Orthod 35:664–668. https://doi.org/10.1093/ejo/cjs070
Wang Q, Ma JB, Wang B, Zhang X, Yin YL, Bai H (2019) Alterations of the oral microbiome in patients treated with the Invisalign system or with fixed appliances. Am J Orthod Dentofacial Orthop 156:633–640. https://doi.org/10.1016/j.ajodo.2018.11.017
Sifakakis I, Papaioannou W, Papadimitriou A, Kloukos D, Papageorgiou SN, Eliades T (2018) Salivary levels of cariogenic bacterial species during orthodontic treatment with thermoplastic aligners or fixed appliances: a prospective cohort study. Prog Orthod 19:25. https://doi.org/10.1186/s40510-018-0230-4
Albhaisi Z, Al-Khateeb SN, Abu Alhaija ES (2020) Enamel demineralization during clear aligner orthodontic treatment compared with fixed appliance therapy, evaluated with quantitative light-induced fluorescence: a randomized clinical trial. Am J Orthod Dentofacial Orthop 157:594–601. https://doi.org/10.1016/j.ajodo.2020.01.004
Borzabadi-Farahani A, Borzabadi E, Lynch E (2014) Nanoparticles in orthodontics, a review of antimicrobial and anti-caries applications. Acta Odontol Scand 72:413–417. https://doi.org/10.3109/00016357.2013.859728
Bącela J, Łabowska MB, Detyna J, Zięty A, Michalak I (2020) Functional coatings for orthodontic archwires-a review. Materials (Basel) 13:3257. https://doi.org/10.3390/ma13153257
Liu Y, Zhang L, Niu LN, Yu T, Xu HHK, Weir MD, Oates TW, Tay FR, Chen JH (2018) Antibacterial and remineralizing orthodontic adhesive containing quaternary ammonium resin monomer and amorphous calcium phosphate nanoparticles. J Dent 72:53–63. https://doi.org/10.1016/j.jdent.2018.03.004
Yu F, Dong Y, Yu HH, Lin PT, Zhang L, Sun X, Liu Y, Xia YN, Huang L, Chen JH (2017) Antibacterial activity and bonding ability of an orthodontic adhesive containing the antibacterial monomer 2-methacryloxylethyl hexadecyl methyl ammonium bromide. Sci Rep 7:41787. https://doi.org/10.1038/srep41787
Ali A, Ismail H, Amin K (2022) Effect of nanosilver mouthwash on prevention of white spot lesions in patients undergoing fixed orthodontic treatment - a randomized double-blind clinical trial. J Dent Sci 17:249–255. https://doi.org/10.1016/j.jds.2021.03.016
Bauer Faria TR, Furletti-Goes VF, Franzini CM, de Aro AA, de Andrade TAM, Sartoratto A, de Menezes CC (2021) Anti-inflammatory and antimicrobial effects of Zingiber officinale mouthwash on patients with fixed orthodontic appliances. Am J Orthod Dentofacial Orthop 159:21–29. https://doi.org/10.1016/j.ajodo.2019.10.025
Flynn LN, Julien K, Noureldin A, Buschang PH (2022) The efficacy of fluoride varnish vs a filled resin sealant for preventing white spot lesions during orthodontic treatment. Angle Orthod 92:204–212. https://doi.org/10.2319/052521-418.1
Poornima P, Krithikadatta J, Ponraj RR, Velmurugan N, Kishen A (2021) Biofilm formation following chitosan-based varnish or chlorhexidine-fluoride varnish application in patients undergoing fixed orthodontic treatment: a double blinded randomised controlled trial. BMC Oral Health 21:465. https://doi.org/10.1186/s12903-021-01805-8
Xie Y, Zhang M, Zhang W, Liu X, Zheng W, Jiang X (2020) Gold nanoclusters-coated orthodontic devices can inhibit the formation of Streptococcus mutans biofilm. ACS Biomater Sci Eng 6:1239–1246. https://doi.org/10.1021/acsbiomaterials.9b01647
Marquis RE (1995) Antimicrobial actions of fluoride for oral bacteria. Can J Microbiol 41:955–964. https://doi.org/10.1139/m95-133
Rošin-Grget K, Peroš K, Sutej I, Bašić K (2013) The cariostatic mechanisms of fluoride. Acta Med Acad 42:179–188. https://doi.org/10.5644/ama2006-124.85
Margolis HC, Moreno EC (1990) Physicochemical perspectives on the cariostatic mechanisms of systemic and topical fluorides. J Dent Res 69:606–613. https://doi.org/10.1177/00220345900690S119. (discussion:634-636)
Zhang N, Melo MA, Chen C, Liu J, Weir MD, Bai Y, Xu HH (2015) Development of a multifunctional adhesive system for prevention of root caries and secondary caries. Dent Mater 31:1119–1131. https://doi.org/10.1016/j.dental.2015.06.010
Kim Y, Son HH, Yi K, Ahn JS, Chang J (2016) Bleaching effects on color, chemical, and mechanical properties of white spot lesions. Oper Dent 41:318–326. https://doi.org/10.2341/15-015-L
Kim Y, Son HH, Yi K, Kim HY, Ahn J, Chang J (2013) The color change in artificial white spot lesions measured using a spectroradiometer. Clin Oral Investig 17:139–146. https://doi.org/10.1007/s00784-012-0680-x
Jansen EE, Meyer-Lueckel H, Esteves-Oliveira M, Wierichs RJ (2021) Do bleaching gels affect the stability of the masking and caries-arresting effects of caries infiltration-in vitro. Clin Oral Investig 25:4011–4021. https://doi.org/10.1007/s00784-020-03732-4
Hua F, Yan J, Zhao S, Yang H, He H (2020) In vitro remineralization of enamel white spot lesions with a carrier-based amorphous calcium phosphate delivery system. Clin Oral Investig 24:2079–2089. https://doi.org/10.1007/s00784-019-03073-x
Niu JY, Yin IX, Wu WKK, Li QL, Mei ML, Chu CH (2021) A novel dual-action antimicrobial peptide for caries management. J Dent 111:103729. https://doi.org/10.1016/j.jdent.2021.103729
Kohda N, Iijima M, Kawaguchi K, Toshima H, Muguruma T, Endo K, Mizoguchi I (2015) Inhibition of enamel demineralization and bond-strength properties of bioactive glass containing 4-META/MMA-TBB-based resin adhesive. Eur J Oral Sci 123:202–207. https://doi.org/10.1111/eos.12187
Zhu Y, Yan J, Mujtaba BM, Li Y, Wei H, Huang S (2021) The dual anti-caries effect of carboxymethyl chitosan nanogel loaded with chimeric lysin ClyR and amorphous calcium phosphate. Eur J Oral Sci 129:e12784. https://doi.org/10.1111/eos.12784
Hua F, Yan J, Zhao S, Yang H, He H (2019) In vitro remineralization of enamel white spot lesions with a carrier-based amorphous calcium phosphate delivery system. Clin Oral Investig 24:2079–2089. https://doi.org/10.1007/s00784-019-03073-x
Zhang J, Boyes V, Festy F, Lynch RJM, Watson TF, Banerjee A (2018) In-vitro subsurface remineralisation of artificial enamel white spot lesions pre-treated with chitosan. Dent Mater 34:1154–1167. https://doi.org/10.1016/j.dental.2018.04.010
Azaripour A, Weusmann J, Mahmoodi B, Peppas D, Gerhold-Ay A, Van Noorden CJ, Willershausen B (2015) Braces versus Invisalign®: gingival parameters and patients’ satisfaction during treatment: a cross-sectional study. BMC Oral Health 15:69. https://doi.org/10.1186/s12903-015-0060-4
Flores-Mir C, Brandelli J, Pacheco-Pereira C (2018) Patient satisfaction and quality of life status after 2 treatment modalities: Invisalign and conventional fixed appliances. Am J Orthod Dentofacial Orthop 154:639–644. https://doi.org/10.1016/j.ajodo.2018.01.013
Abbate GM, Caria MP, Montanari P, Mannu C, Orrù G, Caprioglio A, Levrini L (2015) Periodontal health in teenagers treated with removable aligners and fixed orthodontic appliances. J Orofac Orthop 76:240–250. https://doi.org/10.1007/s00056-015-0285-5
Kotz JC, Treichel PM, Moran MJ (2011) Chemistry and chemical reactivity, 8th edn. CENGAGE Learning, Boston
Lombardo L, Martini M, Cervinara F, Spedicato GA, Oliverio T, Siciliani G (2017) Comparative SEM analysis of nine F22 aligner cleaning strategies. Prog Orthod 18:26. https://doi.org/10.1186/s40510-017-0178-9
Steinberg D, Eyal S (2004) Initial biofilm formation of Streptococcus sobrinus on various orthodontics appliances. J Oral Rehabil 31:1041–1045. https://doi.org/10.1111/j.1365-2842.2004.01350.x
Ambarita AC, Mulyati S, Arahman N, Bilad MR, Shamsuddin N, Ismail NM (2021) Improvement of properties and performances of polyethersulfone ultrafiltration membrane by blending with bio-based dragonbloodin resin. Polymers (Basel) 13:4436. https://doi.org/10.3390/polym13244436
Lee JE, Kim HK (2019) Self-cleanable, waterproof, transparent, and flexible Ag networks covered by hydrophobic polytetrafluoroethylene for multi-functional flexible thin film heaters. Sci Rep 9:16723. https://doi.org/10.1038/s41598-019-53243-w
Sun F, Hung HC, Yan W, Wu K, Shimchuk AA, Gray SD, He W, Huang X, Zhang H (2021) Inhibition of oral biofilm formation by zwitterionic nonfouling coating. J Biomed Mater Res B Appl Biomater 109:1418–1425. https://doi.org/10.1002/jbm.b.34801
Moussa DG, Siqueira WL (2021) Bioinspired caries preventive strategy via customizable pellicles of saliva-derived protein/peptide constructs. Sci Rep 11:17007. https://doi.org/10.1038/s41598-021-96622-y
Chen X, Zhao S, Chu S, Liu S, Yu M, Li J, Gao F, Liu Y (2022) A novel sustained release fluoride strip based poly(propylene carbonate) for preventing caries. Eur J Pharm Sci 171:106128. https://doi.org/10.1016/j.ejps.2022.106128
Qi C, Peng X, Yuan S, Zhang M, Xu X, Cheng X (2022) Evaluation of the antibacterial and anti-inflammatory effects of a natural products-containing toothpaste. Front Cell Infect Microbiol 12:827643. https://doi.org/10.3389/fcimb.2022.827643
Sreenivasan PK, Haraszthy VI, Rayela CC (2021) Antimicrobial effects in oral microenvironments by a novel herbal toothpaste. Contemp Clin Trials Commun 21:100680. https://doi.org/10.1016/j.conctc.2020.100680
Arweiler NB, Müller-Breitenkamp F, Heumann C, Laugisch O, Auschill TM, Action A (2021) Substantivity and anti-plaque effect of different toothpaste slurries - a randomised controlled trial. Oral Health Prev Dent 19:529–536. https://doi.org/10.3290/j.ohpd.b2182977
Lebioda L, Zhang E, Lewinski K, Brewer JM (1993) Fluoride inhibition of yeast enolase: crystal structure of the enolase-Mg(2+)-F(-)-Pi complex at 2.6 A resolution. Proteins 16:219–225. https://doi.org/10.1002/prot.340160302
Thibodeau EA, Keefe TF (1990) pH-dependent fluoride inhibition of catalase activity. Oral Microbiol Immunol 5:328–331. https://doi.org/10.1111/j.1399-302x.1990.tb00435.x
Baykov AA, Dubnova EB, Bakuleva NP, Evtushenko OA, Zhen RG, Rea PA (1993) Differential sensitivity of membrane-associated pyrophosphatases to inhibition by diphosphonates and fluoride delineates two classes of enzyme. FEBS Lett 327:199–202. https://doi.org/10.1016/0014-5793(93)80169-u
Thibodeau EA, Ford CM (1991) Chain formation and de-chaining in Streptococcus sobrinus SL-1. Oral Microbiol Immunol 6:313–315. https://doi.org/10.1111/j.1399-302x.1991.tb00500.x
Belli WA, Buckley DH, Marquis RE (1995) Weak acid effects and fluoride inhibition of glycolysis by Streptococcus mutans GS-5. Can J Microbiol 41:785–791. https://doi.org/10.1139/m95-108
Ahamad I, Bano F, Anwer R, Srivastava P, Kumar R, Fatma T (2021) Antibiofilm activities of biogenic silver nanoparticles against Candida albicans. Front Microbiol 12:741493. https://doi.org/10.3389/fmicb.2021.741493
Zhang L, Weir MD, Chow LC, Antonucci JM, Chen J, Xu HH (2016) Novel rechargeable calcium phosphate dental nanocomposite. Dent Mater 32:285–293. https://doi.org/10.1016/j.dental.2015.11.015
Yi J, Weir MD, Melo MAS, Li T, Lynch CD, Oates TW, Dai Q, Zhao Z, Xu HHK (2019) Novel rechargeable nano-CaF(2) orthodontic cement with high levels of long-term fluoride release. J Dent 90:103214. https://doi.org/10.1016/j.jdent.2019.103214
Al-Eesa NA, Johal A, Hill RG, Wong FSL (2018) Fluoride containing bioactive glass composite for orthodontic adhesives - apatite formation properties. Dent Mater 34:1127–1133. https://doi.org/10.1016/j.dental.2018.04.009
Tanaka T, Kobayashi T, Tamenori Y, Sakanaka A, Kuriki T, Amano A (2019) Phosphoryl oligosaccharides of calcium enhance mineral availability and fluorapatite formation. Arch Oral Biol 101:135–141. https://doi.org/10.1016/j.archoralbio.2019.03.018
Jay E, Rushton M, Grimes R (2012) Migration of fluorine in fluorapatite - a concerted mechanism. J Mater Chem 22:6097–6103. https://doi.org/10.1039/c2jm16235k
Pajor K, Pajchel L, Kolmas J (2019) Hydroxyapatite and fluorapatite in conservative dentistry and oral implantology-a review. Materials (Basel) 12:2683. https://doi.org/10.3390/ma12172683
Ramadoss R, Padmanaban R, Subramanian B (2022) Role of bioglass in enamel remineralization: existing strategies and future prospects-a narrative review. J Biomed Mater Res B Appl Biomater 110:45–66. https://doi.org/10.1002/jbm.b.34904
Arifa MK, Ephraim R, Rajamani T (2019) Recent advances in dental hard tissue remineralization: a review of literature. Int J Clin Pediatr Dent 12:139–144. https://doi.org/10.5005/jp-journals-10005-1603
Al-Nadawi M, Kravitz ND, Hansa I, Makki L, Ferguson DJ, Vaid NR (2021) Effect of clear aligner wear protocol on the efficacy of tooth movement. Angle Orthod 91:157–163. https://doi.org/10.2319/071520-630.1
Júnior NAN, Nunes GP, Gruba AS, Danelon M, da Silva L, de Farias Batista G, Briso ALF, Delbem ACB (2022) Evaluation of bleaching efficacy, microhardness, and trans-amelodentinal diffusion of a novel bleaching agent for an in-office technique containing hexametaphosphate and fluoride. Clin Oral Investig 26:5071–5078. https://doi.org/10.1007/s00784-022-04480-3
Mohanty B, Dadlani D, Mahoney D, Mann AB (2013) Characterizing and identifying incipient carious lesions in dental enamel using micro-Raman spectroscopy. Caries Res 47:27–33. https://doi.org/10.1159/000342432
Xu Y, Xepapadeas AB, Koos B, Geis-Gerstorfer J, Li P, Spintzyk S (2021) Effect of post-rinsing time on the mechanical strength and cytotoxicity of a 3D printed orthodontic splint material. Dent Mater 37:e314-327. https://doi.org/10.1016/j.dental.2021.01.016
Funding
This work was supported by the National Natural Science Foundation of China (No. 81901044), and the Chinese Stomatological Association COS Basic Research Fund (No. COS-B2021-08).
Author information
Authors and Affiliations
Contributions
Yan Jiarong: conceptualization, methodology, formal analysis and writing — original draft; Cao Lingyun: visualization, resources; Luo Ting: visualization, investigation; Qin Danchen: visualization, investigation; Hua Fang: supervision, conceptualization, writing — review and editing; He Hong: supervision, conceptualization, writing — review and editing.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yan, J., Cao, L., Luo, T. et al. In vitro evaluation of a novel fluoride-coated clear aligner with antibacterial and enamel remineralization abilities. Clin Oral Invest 27, 6027–6042 (2023). https://doi.org/10.1007/s00784-023-05216-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-023-05216-7