Abstract
Objectives
The factors that contribute to the morphological changes of dental pulp cell–derived microtissues are unknown. Here, we investigated the contraction dynamics of rod-shaped microtissues derived from dental pulp cells and examined the underlying cell signaling pathways.
Methods
Human dental pulp cells were seeded into agarose molds to assemble into rod-shaped microtissues. Resazurin- and tetrazolium-based cytotoxicity assays, Live/Dead staining, and hematoxylin and eosin staining for histological evaluation of rods were performed. Rod contraction was evaluated and measured for a period of 10 days. The role of TGF-β, phosphoinositide 3-kinase (PI3K)/AKT, and mitogen-activated protein kinase (MAPK) signaling pathway was analyzed.
Results
Dental pulp cells readily assembled into rods, maintaining the geometric shape for 48 h. Following this period, they condensed to form stable spheroidal structures that remained vital for 10 days from seeding. Inhibition of phosphoinositide 3-kinase signaling pathway by LY294002 significantly prolonged the diminution in the length of rods formed by dental pulp cells. TGF-β and pharmacological inhibition of TGF-β signaling did not show pronounced effects.
Conclusion
Overall, dental pulp cells readily formed rod-shaped patterns of microtissues which, over a period of time, condensed into more stable spheroidal structures. Hence, technologies like bioprinting, using direct fabrication of microtissues need to consider the contraction dynamics.
Clinical relevance
The field of regenerative endodontology will benefit from our findings as it can be applied as a novel platform to test the impact of pharmacological agents, biomaterials, and regenerative approaches including bioprinting.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ameliorating the stability, survival ability, and functionalities of transplanted cells are the key elements to a successful tissue regeneration technique [1]. Vast literature exists exemplifying the approaches employed for dental pulp regeneration, both in vivo and in vitro [2,3,4]. Scaffold-free schemes using microtissues of various cell types in complex shapes such as spheroids, rods, toroids [5,6,7], and sheets not only facilitate a more in vivo–like environment for the transplanted cells but also avoid issues sprouting from inflammation and slow degradation of the scaffolds [8]. In order to mimic the rod-like shape of the root canal, attempts have been made to fabricate the most suitable cell-seeding system including sheets and spheroids [4, 9]. The rationale behind our research was to check the feasibility of molding dental pulp cells into rod-shaped microtissues and to investigate the potential signaling pathways responsible for regulating their contraction.
The uniqueness in the design of rod microtissues is that it is free of size constraints with respect to the length, unlike the spheroid diameter which is restricted by the diffusion capacity of the capillary network and thus feasible molds for spheroids are limited with regard to the dimensions [5]. Rod microtissues could have the potential to overcome this challenge owing to the feasibility of increasing the length without altering the thickness. Moreover, its closely mimicking cylindrical shape makes it a desirable endodontic graft for regeneration of the dental pulp. Hence, it is imperative to comprehend its contraction dynamics and potential mechanisms responsible for constructing a more stable microtissue model for dental pulp regeneration in vitro.
Literature has shown that self-assembly of microtissues is directed not only by cell surface adhesive forces, but also by cytoskeletal contraction [7]. Transforming growth factor-beta (TGF-β) is considered to be essential for cell chemotaxis, proliferation, differentiation [10, 11], and migration [12] in dental pulp cells (DPC). Based on this, we investigated its impact on the dimensional regulation of DPC rods. In transplanted tissues, mitogen-activated protein kinases (MAPK) and phosphoinositide 3-kinase (PI3K)/AKT cell-signaling pathways play a vital role [1, 13]. Their properties and broad range of interaction with the microenvironment in both dental embryogenesis [14] and in vitro pulp regeneration significantly regulate the self-assembly of cells [15, 16]. Recent studies have shown that PI3K has a role in the leading edge of migrating fibroblasts via F-actin filament branching [17]. There is also evidence that uncoupling of intermediate filaments from focal adhesions compromises the downstream MAPK cascades to ERK1/2 and p38 [14, 15]. Thus, cell migration can be controlled by p38-mediated protrusion and stress fiber formation. Hence, we investigated the potential role of these pathways in regulating the spatio-temporal dimensional alteration of DPC rod microtissues.
To use DPC rod microtissues as a platform for future experiments for in vivo endodontic regenerative medicine, in vitro 3D pulp tissue models for testing dental pharmacokinetics and direct application of rod-shaped large tissue constructs with bioprinting, it is crucial to study its dimensional stability and the potential factors involved in the regulation of geometrical alterations in in vivo–like conditions.
Materials and methods
Isolation and culture of dental pulp cells
Human DPC were harvested in a sterile environment from extracted third molars without pulpitis, with a prior informed consent [16]. Pulp tissue underwent explant cultures to isolate DPC through outgrowth. Cells were cultured in alpha-minimal essential medium (α-MEM, Sigma-Aldrich, St. Louis,MO, USA) supplemented with 10% fetal bovine serum (Gibco, Thermo FischerScientific, MA, USA), penicillin G, streptomycin and amphotericin B (Gibco) at 37 °C, 5% CO2, and 95% atmospheric moisture. The experiments were performed with three donors to take into consideration the donor-dependent variability in response and to rule out bias. The protocol was accepted by the ethics committee of the Medical University of Vienna (631/2007).
Fabrication of rod microtissues
3D rod-shaped microtissue patterns of DPC were created using 3D Petri dishes® embracing the manufacturer’s instructions (Microtissues, Inc., Providence, RI, USA). Nominal dimensions of each 3D culture trough are 2200 μm in length × 800 μm in depth × 400 μm in width. Pouring liquid agarose into flexible 3D Petri dishes® embodying a trough-shaped arrangement formed agarose molds with 24 troughs for constructing DPC rods. The agarose molds were soaked in cell culture medium and positioned into 24-well plates, with one mold per well. Cell suspensions of 480,000 cells in drops of 70 μL were pipetted into each mold as described by the manufacturer instructions. Each well then received 1 mL of cell culture medium and plates were incubated for 24 h.
MTT staining
Rod microtissues of DPC were incubated with 1 mg/mL MTT at 37 °C for 30 min in a 24-well plate after the 24-h incubation period. Formazan formation was observed under light microscope and images were taken [18].
Live/Dead staining
To assess the viability of the self-assembly of the DPC, samples were stained with the Live/Dead Cell Staining Kit (Enzo Life Sciences AG, Lausen, TX, USA) embracing the manufacturer’s guidelines in a 24-well plate following the 24 h incubation period [19]. The vitality of the rod microtissues was analyzed using fluorescence microscopy for green and red with a B-2A filter (excitation filter wavelengths: 450–490 nm), respectively after 24 and 240 h. Vital cells were detected as green while the dead cells as red. Images were taken.
Resazurin-based toxicity assay
Resazurin-based toxicity assay was performed according to the manufacturer’s instructions to assess the cell viability of DPC rod microtissues. Sixty microliters of resazurin dye (Merck, Darmstadt, Germany) were added into each well of the 24-well plate, 24 h after seeding the cells into agarose molds. Following 8 h of incubation at 37 °C, fluorescence was evaluated using a Synergy HTX multi-mode reader (BioTek, Winooski, VT, USA) at a wavelength of 600 nm, using an excitation wavelength of 540 nm (Klara Janjić et al. 2018). The data was calculated relative to the control (only the cell culture medium).
Contraction dynamics of dental pulp cell rod microtissues
Geometrical and morphological alterations in the length and width of the rod microtissues of DPC were measured over a period of 10 days. Cell culture medium was changed every 3 days. Images of the self-assembly of DPC in the agarose mold troughs were taken at 0, 2, 6, 24, 48, 72, 96, 120, and 240 h after seeding at fourfold magnification. Length and width were calculated in millimeters using the Call EZ software.
Histological evaluation
Hematoxylin and eosin (H&E) staining of DPC rod microtissues was performed after a 24-h incubation period using the following protocol: samples were stained for 7 min in Mayer’s hematoxylin and rinsed in distilled water for 30 s. After differentiating with 0.1% HClOH for 20 s, they were rinsed for 10 min in tap water followed by rinsing in distilled water for 30 s. Next, they were stained for 3 min in 0.5% Eosin G (with two droplets of glacial acetic acid) and rinsed in tap water for 10 s, followed by dehydration in 70% EtOH, 96% EtOH, 100% EtOH, and xylene for 2, 2, 10, and 5 min, respectively. Finally, they were permanently embedded.
TGF-β signaling
DPC were incubated with human TGF-β at 5 μg/mL and its inhibitor SB431542 at 10 mM as described above to examine the role of TGF-β on the contraction of their rod-shaped microtissue patterns. The concentration was based on previous publications [20]. Twenty-four hours after incubation, images were taken using fourfold objective and OptoCapture software 2.2. Length and width were calculated in millimeters using Call EZ software. Data are displayed as compared with the untreated cells, referred to control.
PI3/AKT and MAPK signaling
DPC were incubated with the pharmacological inhibitors LY294002 (PI3K-inhibitor; Sigma), SB203580 (p38- inhibitor; Sigma), SP600125 (JNK-inhibitor; Calbiochem, San Diego, CA, USA), and U0126 (ERK-inhibitor; Cell Signaling Technology, Beverly, MA, USA), all at 10 μM as described above, to examine the role of PI3K and MAPK signaling. The concentration was based on previous reports [21]. Twenty-four hours after incubation, images were taken and processed as described above.
Statistical evaluation
Statistical analysis was done with IBM SPSS Statistics Version 24 (IBM Corporation, Armonk, NY, USA), using the ANOVA and the post hoc Dunnett’s test. The level of significance was set at p < 0.05.
Results
Contraction dynamics of dental pulp cell rod microtissues
Rods from all the DPC donors condensed over time (Fig. 1). To quantify the dynamics of rod formation over a time period of 240 h, we measured changes in the length (Fig. 1b) and width (Fig. 2c) of the rod microtissues. The analysis showed that the DPC rod length condensed to 62%, 27%, and 11% of the original length at 6, 24, and 240 h, respectively (p < 0.05). The compensation in the diminution of length was maintained by the width which was 70%, 82%, and 55% of the original width at 6, 24, and 240 h, respectively (p < 0.05). These data highlight the pronounced dimensional changes in the rod microtissue within the first 24 h.
Contraction dynamics of rod microtissues of dental pulp cells. 3D rod microtissue cultures were created using 3D Petri dishes® with dental pulp cells. Images were taken directly after seeding (0 h), at 2 h, 6 h, 24 h, 48 h, 72 h, 96 h, 120 h, and 240 h after seeding. The figure shows representative images of 3 donors (a). The length (b) and width (c) were quantified. Experiments were performed 3 times, with 3 donors and 4 rods per experiment were analyzed. The data points show the length and width relative to 0 h as mean ± standard deviation. p < 0.05
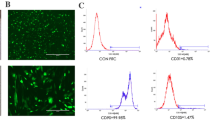
Rod microtissues maintain viability based on Live/Dead staining, MTT staining, histological analysis, and Resazurin-based toxicity assay. To assess the viability of the rod microtissues, the Live/Dead staining (LD) was performed after 24 h, the MTT staining and histological evaluation by hematoxylin and eosin (H&E) staining were performed with rods after 24 h (a). Resazurin-based toxicity assays were done. Experiments were performed 3 times with 3 donors per experiment (b). Bars represent mean ± standard deviation relative to the control
Dental pulp cell rod microtissues maintained viability
To assess the viability of the rod microtissues, the Live/Dead and MTT staining, and the resazurin-based cytotoxicity assays were performed (Fig. 2). The self-assembly of DPC, that is, rods at 24 h, stained with the cell permeable green fluorescent dye, visible as bright green structures, indicating vitality. It was observed that the formazan crystals in the MTT assay could not be dissolved by dimethyl sulfoxide, hence, microscopic images were taken. Staining the cells with tetrazolium dye made the DPC rods appear as dark blue structures, indicating the conversion of the tetrazolium dye into formazan.
To confirm the viability results from Live/Dead and MTT staining, the resazurin-based cytotoxicity assay was performed (Fig. 2a). The data indicated that the DPC rods were vital after 24 h. To explore the histology of the DPC rod microtissues, they were stained with H&E dyes (Fig. 2a). They appeared as cylindrical structures with blue-violet nuclei and red cytoplasm. The resazurin-based cytotoxicity assays showed that the microtissues were able to convert resazurin into resorufin (Fig. 2b). While the rods showed 7584 ± 2258 relative fluorescence units, 1285 ± 256 relative fluorescence units were found in the blank group without cells (negative control). Overall, the data indicate that cells maintained their viability in the rod microtissue.
TGF-β or its inhibitor SB43154 do not prolong the contraction of dental pulp cell rods
DPC rods were incubated with recombinant human TGF-β and the inhibitor of TGF-β, SB43154 for 24 h (Fig. 3). Geometrical measurements and their average displayed that the length of the rods treated with TGF-β was 108% and the width was 95.1% of the control; whereas, for the set of rods treated with SB43154, the length was 96.4% and the width was 107.5% that of control. This minor alteration in the length and width of the rods from the images taken after 24 h indicated that neither of the above played a role in the DPC rod contraction.
Neither TGF-β nor the TGF-β signaling inhibitor SB43154 has a pronounced impact on contraction of dental pulp cell rod microtissues. To investigate the role of TGF-β on the contraction of the rod microtissue formed by dental pulp cells, the cells were incubated with human TGF-β or the TGF-β signaling inhibitor SB431542. After 24 h, images were taken and length (a) and width (b) were calculated. Experiments were performed 3 times with 3 different donors per experiment. Bars represent mean ± standard deviation relative to untreated cells (untreated control)
Inhibitor of PI3K signaling inhibits dental pulp cell rod microtissue contraction
DPC were incubated with the pharmacological inhibitors LY294002 (PI3K-inhibitor), SB203580 (p38-inhibitor), SP600125 (JNK-inhibitor), and UO126 (ERK-inhibitor), all at 10 μM for 24 h, to examine their effect on the rod size diminution (Fig. 4a). It was observed that the inhibitor of PI3K, LY294002, significantly decreased the contraction in length, compared with the other pharmacological inhibitors and control (p < 0.05) (Fig. 4b). The measurements displayed that the average length of the rods treated with LY294002 was 165.8%, with SB203580 was 108.9%, with SP600125 was 105.9%, and with UO126 was 93.9% of the control after 24 h of incubation period. The alteration in length was compensated by the change in width (Fig. 4c) which was 96.8% with LY294002, 99.7% with SB203580, 93.8% with SP600125, and 100.7% with UO126 of the control. The increase in the length and delayed contraction by the influence of LY294002 was significant as compared with control (p < 0.05).
Inhibitor of PI3K signaling affects rod microtissue length. To investigate the role of PI3K/AKT and MAPK signaling, rod microtissues of dental pulp cells were incubated with the pharmacological inhibitors LY294002 (PI3K-inhibitor), SB203580 (p38- inhibitor), SP600125 (JNK-inhibitor), and U0126 (ERK-inhibitor). Experiments were performed 3 times with 3 donors per experiment. After 24 h, images (a) were taken and length (b) and width (c) were calculated. Bars represent mean ± standard deviation relative to untreated cells (untreated control)
Discussion
Building macrotissues from optimally shaped microtissues with lesser limitations of maintaining vascularity and dimensional stability over time still needs to be addressed [22]. Hence, in the present study, we investigated the contraction dynamics in the human DPC rod-shaped self-assembly of microtissues as it can serve as a potential platform for pulp repair and regeneration. It was observed that DPC have a potential to self-assemble into rods that condense over a period of 10 days into spheroid structures but maintain vitality. Introduction of cytokine TGF-β (and its inhibitor) that is known for cell differentiation and migration of DPC did not alter the contraction in these rods, indicating that this autocrine signaling mechanism does not play a major role in this system. On the other hand, the pharmacological inhibitor of PI3K showed a significant delay in the contraction of DPC rod length, revealing a pivotal role of PI3K/AKT pathway in DPC microtissue contraction in in vivo–like conditions.
Explicit conceptualization of the stability, functionality, and survival of the transplanted tissue is indispensable in the field of tissue regeneration as these traits are attenuated in the host environment [23]. To optimize their application in vivo, it is mandatory to look into the dimensional stability of complex-shaped microtissue constructs. Human-derived periodontal ligament and gingival cells have previously been directed into rod-shaped microtissues [24]. Considering this, it was interesting to investigate whether DPC self-assembled into stable rod-shaped terminal structures. Spheroid-shaped microtissues of DPC have been established as terminal structures [25, 26] for endodontic regenerative strategies. Their property of self-aggregation makes intimate cell-cell communication and cell-extracellular matrix interaction possible by forming an in vivo–like extracellular matrix [27]. Measures taken to promote its vascularization in vitro by pre-conditioning with hypoxia is known to promote angiogenesis [19]. Literature regarding similar aspects of rod-shaped DPC microtissues is still vacuous.
With our setting, it was possible to fabricate DPC microtissue rods with an average length of 0.6 mm and width 0.3 mm after 24 h. Rods of all tested DPC donors condensed over time into terminal spheroids. These structures remained vital as displayed MTT staining, resazurin-based cytotoxicity assays, and Live/Dead imaging (Also see supplementary fig. 1). Microtissue rods existed as tissue pellets with a cell density of 6857 cells/ μL firmly adhered to each other in vitro. Thus, it was not possible to dissolve the formazan crystals with DMSO. Hence, we could not quantify the formazan formation with photometer rather confirmed the results for viability with resazurin-based cytotoxicity assays [28]. Our findings are in line with the kinetics from a related research employing normal human fibroblasts and H35 cell line highlighting a steep contraction curve in the length of microtissue rods in the first 6 h after seeding [5]. Advanced in vivo investigation is indispensable as the condensation might be influenced once these microtissues are in contact with dentine and other cells in the transplanted site.
Cytokines and cell-signaling molecules modulate the morphology of transplanted cells in vivo by acting on the cytoskeleton-mediated tension in the 3D tissues [5, 7]. Immense work has been done previously to establish the role of intercellular signaling molecules in the migration of DPC microtissues by applying their pharmacological inhibitors in vitro for instance, Y-27632, inhibitor to Rho-associated kinases [27]. Rho-kinase functions by effectuating cytoskeletal contraction by actomyosin coupling and phosphorylation [29]. Similarly, PI3K is known to cause migration in various mesenchymal stem cells including dental pulp stem cells [1, 30, 31]. Inhibitor of PI3K, LY294002 is known to attenuate ICAM-1 expression, where ICAM-1 is the cellular adhesion molecule of dental pulp–derived cells [32]. Studies with smooth muscle cells have shown that PI3K regulates a protein called PLEKHG3 that selectively binds to new F-actin at the leading edge of migrating fibroblasts [17]. The findings from our experimental set up where LY294002, the pharmacological inhibitor of PI3K, was observed to significantly delay the contraction in the length of DPC microtissues as compared with the untreated cells and other pharmacological inhibitors of MAPK, support the role of PI3K pathway in controlling the contraction dynamics of the microtissues in vitro.
Our findings are relevant for research employing DPC rod microtissues. However, the dental pulp contains a plethora of cells including endothelial and nerve cells which interact differently with the signaling molecules used in the setup. This heterogeneity could lead to variation in reproducibility of therapeutic results. Therefore, further research is required with single cell populations and co-cultures of DPC and endothelial cells or vascular endothelial growth factors to explore their influence on morphogenesis and proliferation of DPC rod microtissues. Design influencing features like posts, cones, and plugs that create tension effectuating the change in self-assembly need to be considered in future experiments [6].
Conclusion
The revelations from our research can be applied in further experiments using dental pulp cell–based 3D microtissues as a platform to test the efficacy of dental pharmacological agents, biomaterials and regenerative approaches, newer assays, and innovative caries management treatment strategies. It is a significant finding for the selection of the correct seeding DPC microtissue constructs in bioprinters.
References
Chen J, Crawford R, Chen C, Xiao Y (2013) The key regulatory roles of the PI3K/Akt signaling pathway in the functionalities of mesenchymal stem cells and applications in tissue regeneration. Tissue Eng Part B Rev 19:516–528. https://doi.org/10.1089/ten.TEB.2012.0672
Janjić K, Cvikl B, Moritz A, Agis H (2016) Dental pulp regeneration. J Stomat Occ Med 8:1–9. https://doi.org/10.1007/s12548-015-0139-1
Müller AS, Janjić K, Lilaj B, Edelmayer M, Agis H (2017) Hypoxia-based strategies for regenerative dentistry-views from the different dental fields. Arch Oral Biol 81:121–130. https://doi.org/10.1016/j.archoralbio.2017.04.029
Dissanayaka WL, Zhu L, Hargreaves KM, Jin L, Zhang C (2014) Scaffold-free prevascularized microtissue spheroids for pulp regeneration. J Dent Res 93:1296–1303. https://doi.org/10.1177/0022034514550040
Dean DM, Napolitano AP, Youssef J, Morgan JR (2007) Rods, tori, and honeycombs: the directed self-assembly of microtissues with prescribed microscale geometries. FASEB J 21:4005–4012. https://doi.org/10.1096/fj.07-8710com
Svoronos AA, Tejavibulya N, Schell JY, Shenoy VB, Morgan JR (2014) Micro-mold design controls the 3D morphological evolution of self-assembling multicellular microtissues. Tissue Eng Part A 20:1134–1144. https://doi.org/10.1089/ten.TEA.2013.0297
Dean DM, Morgan JR (2008) Cytoskeletal-mediated tension modulates the directed self-assembly of microtissues. Tissue Eng Part A 14:1989–1997. https://doi.org/10.1089/ten.tea.2007.0320
Na S, Zhang H, Huang F, Wang W, Ding Y, Li D, Jin Y (2016) Regeneration of dental pulp/dentine complex with a three-dimensional and scaffold-free stem-cell sheet-derived pellet. J Tissue Eng Regen Med 10:261–270. https://doi.org/10.1002/term.1686
Itoh Y, Sasaki JI, Hashimoto M, Katata C, Hayashi M, Imazato S (2018) Pulp regeneration by 3-dimensional dental pulp stem cell constructs. J Dent Res 97:1137–1143. https://doi.org/10.1177/0022034518772260
Niwa T, Yamakoshi Y, Yamazaki H, Karakida T, Chiba R, Hu JC, Nagano T, Yamamoto R, Simmer JP, Margolis HC, Gomi K (2018) The dynamics of TGF-β in dental pulp, odontoblasts and dentin. Sci Rep 8:4450. https://doi.org/10.1038/s41598-018-22823-7
Guzalinuer A, Muhetaer H, Wu H, Paerhati A (2018) Experimental study on the transforming growth factor β3 combined with dental pulp stem cells in early bone integration of implant. Zhonghua Kou Qiang Yi Xue Za Zhi 53:259–263. https://doi.org/10.3760/cma.j.issn.1002-0098.2018.04.009
Melin M, Joffre-Romeas A, Farges JC, Couble ML, Magloire H, Bleicher F (2000) Effects of TGFbeta1 on dental pulp cells in cultured human tooth slices. J Dent Res 79:1689–1696. https://doi.org/10.1177/00220345000790090901
Barone V, Heisenberg C-P (2012) Cell adhesion in embryo morphogenesis. Curr Opin Cell Biol 24:148–153. https://doi.org/10.1016/j.ceb.2011.11.006
Leduc C, Etienne-Manneville S (2015) Intermediate filaments in cell migration and invasion: the unusual suspects. Curr Opin Cell Biol 32:102–112. https://doi.org/10.1016/j.ceb.2015.01.005
Gregor M, Osmanagic-Myers S, Burgstaller G, Wolfram M, Fischer I, Walko G, Resch GP, Jörgl A, Herrmann H, Wiche G (2014) Mechanosensing through focal adhesion-anchored intermediate filaments. FASEB J 28:715–729. https://doi.org/10.1096/fj.13-231829
Janjić K, Lilaj B, Moritz A, Agis H (2018) Formation of spheroids by dental pulp cells in the presence of hypoxia and hypoxia mimetic agents. Int Endod J 51(Suppl 2):e146–e156. https://doi.org/10.1111/iej.12806
Tang DD, Gerlach BD (2017) The roles and regulation of the actin cytoskeleton, intermediate filaments and microtubules in smooth muscle cell migration. Respir Res 18:54. https://doi.org/10.1186/s12931-017-0544-7
Kurzmann C, Janjić K, Shokoohi-Tabrizi H, Edelmayer M, Pensch M, Moritz A, Agis H (2017) Evaluation of resins for stereolithographic 3D-printed surgical guides: the response of L929 cells and human gingival fibroblasts. Biomed Res Int 2017:4057612. https://doi.org/10.1155/2017/4057612
Janjić K, Alhujazy U, Moritz A, Agis H (2018) L-mimosine and hypoxia enhance angiopoietin-like 4 production involving hypoxia-inducible factor-1alpha: insights from monolayer and spheroid cultures of dental pulp-derived cells and tooth slice cultures. Arch Oral Biol 85:172–177. https://doi.org/10.1016/j.archoralbio.2017.10.011
Panahipour L, Stähli A, Haiden N, Gruber R (2018) TGF-β activity in cow milk and fermented milk products: an in vitro bioassay with oral fibroblasts. Arch Oral Biol 95:15–21. https://doi.org/10.1016/j.archoralbio.2018.07.005
Agis H, Stampfl B, Watzek G, Gruber R (2010) Activated platelets increase proliferation and protein synthesis of human dental pulp-derived cells. Int Endod J 43:115–124. https://doi.org/10.1111/j.1365-2591.2009.01650.x
Luo H, Chen M, Wang X, Mei Y, Ye Z, Zhou Y, Tan WS (2014) Fabrication of viable centimeter-sized 3D tissue constructs with microchannel conduits for improved tissue properties through assembly of cell-laden microbeads. J Tissue Eng Regen Med 8:493–504. https://doi.org/10.1002/term.1554
Murry CE, Soonpaa MH, Reinecke H, Nakajima H, Nakajima HO, Rubart M, Pasumarthi KB, Virag JI, Bartelmez SH, Poppa V, Bradford G, Dowell JD, Williams DA, Field LJ (2004) Haematopoietic stem cells do not transdifferentiate into cardiac myocytes in myocardial infarcts. Nature 428:664–668. https://doi.org/10.1038/nature02446
Oberoi G, Janjić K, Müller AS, Schädl B, Andrukhov O, Moritz A, Agis H (2018) Contraction dynamics of rod microtissues of gingiva-derived and periodontal ligament-derived cells. Front Physiol 9:1683. https://doi.org/10.3389/fphys.2018.01683
Janjić K, Edelmayer M, Moritz A, Agis H (2017) L-mimosine and hypoxia can increase angiogenin production in dental pulp-derived cells. BMC Oral Health 17:87. https://doi.org/10.1186/s12903-017-0373-6
Janjić K, Kurzmann C, Moritz A, Agis H (2017) Expression of circadian core clock genes in fibroblasts of human gingiva and periodontal ligament is modulated by L-Mimosine and hypoxia in monolayer and spheroid cultures. Arch Oral Biol 79:95–99. https://doi.org/10.1016/j.archoralbio.2017.03.007
Hsieh H-Y, Young T-H, Yao C-C, Chen Y-J (2018) Aggregation of human dental pulp cells into 3D spheroids enhances their migration ability after reseeding. J Cell Physiol 234:976–986. https://doi.org/10.1002/jcp.26927
Grela E, Ząbek A, Grabowiecka A (2015) Interferences in the optimization of the MTT assay for viability estimation of Proteus mirabilis. Avicenna J Med Biotechnol 7:159–167
Etienne-Manneville S, Hall A (2002) Rho GTPases in cell biology. Nature 420:629–635. https://doi.org/10.1038/nature01148
Li M, Sun X, Ma L, Jin L, Zhang W, Xiao M, Yu Q (2017) SDF-1/CXCR4 axis induces human dental pulp stem cell migration through FAK/PI3K/Akt and GSK3β/β-catenin pathways. Sci Rep 7:40161. https://doi.org/10.1038/srep40161
Zhang M, Jiang F, Zhang X, Wang S, Jin Y, Zhang W, Jiang X (2017) The effects of platelet-derived growth factor-BB on human dental pulp stem cells mediated dentin-pulp complex regeneration. Stem Cells Transl Med 6:2126–2134. https://doi.org/10.1002/sctm.17-0033
Chang M-C, Hung H-P, Lin LD, Shyu YC, Wang TM, Lin HJ, Chan CP, Huang CC, Jeng JH (2015) Effect of interleukin-1β on ICAM-1 expression of dental pulp cells: role of PI3K/Akt, MEK/ERK, and cyclooxygenase. Clin Oral Investig 19:117–126. https://doi.org/10.1007/s00784-014-1227-0
Acknowledgments
We thank Manuela Pensch for the skillful technical assistance.
Funding
Open access funding provided by Medical University of Vienna. The work was supported by the Osteology Foundation (15-184). Anna Müller received the research fellowship “Wissenschaftsstipendium für Waldviertler WissenschaftlerInnen mit sozialer Kompetenz Wissenschaft – solide wie Waldviertler Granit” by the GEA Akademie (Schrems, Austria).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The protocol for cell isolation was accepted by the ethics committee of the Medical University of Vienna (631/2007).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Figure S1
Rods maintain viability for 240 h based on Live/Dead staining. To assess the viability of the microtissue rods, Live/Dead staining was performed after 240 h and images were taken. (JPG 246 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Oberoi, G., Janjić, K., Müller, A.S. et al. Contraction dynamics of dental pulp cell rod microtissues. Clin Oral Invest 24, 631–638 (2020). https://doi.org/10.1007/s00784-019-02917-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02917-w