Abstract
To enhance the effect of anti-influenza-virus agent treatment, the effect of combined administration of oseltamivir phosphate and hochu-ekki-to (Japanese traditional herbal medicine, HET) on early viral clearance was examined. Senescence-accelerated mice were given HET in drinking water for 2 weeks, followed by intranasal infection with influenza A virus strain PR8. After 4 hours of infection, oseltamivir was administered orally for 5 days. The viral loads in the lungs of the group receiving combined treatment were dramatically lower when compared with the viral loads in the lungs of the group receiving oseltamivir alone. HET significantly increased the induction of IL-1β and TNF-α in the lungs of PR8-infected mice and stimulated alveolar macrophage phagocytosis. From these results, we conclude that these functions may be responsible the increased effect on viral load reduction. Here, we show that the combined administration of oseltamivir and HET is very useful for influenza treatment in senescence-accelerated mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Influenza is a worldwide epidemic that causes substantial morbidity and mortality. There is the possibility of an influenza pandemic caused by a new type of influenza virus [1–3]. A triple reassortant of swine, avian and human viruses caused a pandemic in 2009 [4–6]. There is the increasing possibility for avian influenza virus (H5N1 to mutate) into a new type that can affect humans [7–11]. It is therefore necessary to prepare for the prevention of not only seasonal influenza but also pandemic influenza. Measures taken against a possible influenza pandemic include the stockpiling of anti-influenza virus drugs, such as oseltamivir and zanamivir—known as neuraminidase inhibitors [12–15]. Additionally, new neuraminidase inhibitor drugs have been developed [16–18]. However, many influenza virus strains have developed resistance to amantadine and rimantadine, which are M2 proton channel blockers, and these drugs are no longer recommended for the treatment of influenza [19, 20]. Oseltamivir-resistant viruses have also been found in recent years [21–23]. Urgent action is required to prevent the emergence of further drug-resistant influenza viruses.
Oseltamivir can reduce influenza symptoms if administered during the early stages of infection [14]. In adults, the virus levels in the body decrease with a reduction in fever [24, 25]. However, the duration of virus shedding in children and immunocompromised people is prolonged even after they become afebrile [26–29]. This long-term virus shedding following neuraminidase inhibitor treatment increases the risk of the emergence of drug-resistant mutations [30, 31]. It is assumed that the same phenomenon is also present in elderly patients who have compromised immune systems.
In this study, we considered whether the combined administration of anti-influenza drugs and immune-stimulating Japanese traditional herbal medicine could reduce the viral load in elderly patients more rapidly than antiviral drugs alone. To this end, we focused on HET (“Bu-Zhong-Yi-Qi-Tang” in Chinese, TJ-41), Japanese traditional herbal medicine (Kampo), well known as a tonic. It has been used for the treatment of patients who have chronic diseases, tuberculosis, appetite loss, and gastroptosis. The various immunostimulatory activities of HET have been reported as follows: enhancement of IFN-γ production [32], activation of macrophages [33], enhancement of natural killer cell activity [34], and stimulation of the mucosal immune system [35, 36]. The anti-infectious activities of HET have been demonstrated against influenza virus [37], Candida [38], cytomegalovirus [39], herpes simplex virus type-1 [40], Listeria monocytogenes [32], and rhinovirus [41].
SAMP1 is an accelerated senescence-prone strain of mouse with a short life span, and shows an early, age-related functional decline in its immune system [42–45]. In this study, we adopted the concomitant therapy of oseltamivir and HET with the aim of controlling the emergence of drug-resistant influenza viruses after treatment with antiviral drugs using a senescence-accelerated mouse model.
Materials and methods
Kampo formulation and antiviral drugs
A spray-dried extract preparation of HET medicine was kindly supplied by Tsumura & Co. (Tokyo, Japan). HET consists of Astragali Radix (4.0 g), Atractylodis lanceae Rhizoma (4.0 g), Ginseng Radix (4.0 g), Angelicae Radix (3.0 g), Bupleuri Radix (2.0 g), Zizyphi Fructus (2.0 g), Aurantii nobilis pericarpium (2.0 g), Glycyrrhizae Radix (1.5 g), Cimicifugae Rhizoma (1.0 g), and Zingiberis Rhizoma (0.5 g). We used oseltamivir phosphate (Tamiflu, Roche Laboratories Inc., Basel, Switzerland) as the antiviral drug.
Cells and virus
Madin-Darby canine kidney cells (MDCK) were purchased from Dainippon Sumitomo Pharma Co., Ltd., and grown in Dulbecco’s modified Eagle’s minimum essential medium (DMEM) (Nissui Pharmaceutical Co. Ltd., Tokyo, Japan) supplemented with glutamine (30 mg/ml), penicillin (100 units/ml), streptomycin (100 μg/ml), sodium bicarbonate (3.7 g/L) and 4 % fetal bovine serum. Cells were maintained at 37 °C in an atmosphere of 5 % CO2.
The influenza A virus used in this study was a mouse-adapted A/Puerto Rico/8/34(H1N1) (PR8) strain. It was kindly supplied by Dr. Hasegawa of the Influenza Virus Research Center, National Institute of Infectious Diseases. Virus stock was propagated in the allantoic cavity of 10-day-old embryonated chicken eggs at 37 °C for 48 h. The allantoic fluids were harvested and centrifuged at 15,000×g at 4 °C for 20 min. The clarified supernatant was aliquoted, filtered and stored at −80 °C until use. The viral titer was assayed by a plaque-forming method using MDCK cells.
Plaque assay
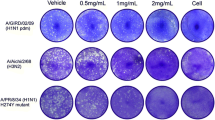
A confluent monolayer of MDCK cells in a 6-well plate was washed twice with serum-free DMEM (SF DMEM), followed by infection with 100 μl of virus suspension in a tenfold serial dilution. After incubation at 37 °C for 1 h with tilting every 10 min, unabsorbed inoculum was removed, and infected cells were overlaid with 4 ml of agar DMEM (SF DMEM containing 0.8 % agarose, 0.2 % albumin and 2.5 μg of trypsin per ml). The plate was incubated at 37 °C in an atmosphere of 5 % CO2 for 2 days. For plaque counting, cells were fixed with 5 % glutaraldehyde solution for 2 h, the agarose medium was removed, and the cells were stained with 1 % crystal violet.
Mice
BALB/c, C57BL/6, senescence-accelerated mouse prone 1 (SAMP1), and control mouse (SAMR1) were purchased from Japan SLC, Inc. All experiments were approved by the institutional ethics committee and carried out in agreement with the ‘Guide for the Care and Use of Laboratory Animals’.
Medication and infection
HET was dissolved in drinking water administered to mice at 6 mg/ml and autoclaved at 121 °C for 15 min. Kampo administration was performed during the entire experimental period. Two weeks after starting Kampo medication, mice were lightly anesthetized by an intraperitoneal injection of pentobarbital sodium at a dose of 50 mg per kg and infected intranasally with 30 μl of the viral suspension containing 20 PFU of PR8. After 4 hours of infection, oseltamivir phosphate, dissolved in water at a concentration of 0.1 mg/200 μL, was administered by oral gavage twice daily for 5 days.
At the time of PR8 infection, 10- to 12-week-old females (SAMP1 and SAMR1) or 8-week-old females (BALB/c) were used. At 2, 4 and 8 days postinfection (dpi), mice were sacrificed by an intraperitoneal injection with excess pentobarbital sodium, and their lungs were harvested. Lung tissue was homogenized with 1 ml of PBS(−) and centrifuged at 9,000×g at 4 °C for 2 min. Supernatants were analyzed for viral titers and cytokine levels.
Cytokine quantification
Cytokine levels in lung homogenates were determined using ELISA kits (eBioscience, Inc., San Diego, CA, USA for TNF-α, IL-1β, IL-6, IL-12 p70, IFN-γ, and CCL2; or R&D Systems, Inc., Minneapolis, MN, USA for IL-17, IFN-α, and IFN-β).
Phagocytosis assay of alveolar macrophages (AM)
Mice were killed with an overdose of pentobarbital sodium, and bronchoalveolar lavage (BAL) was performed by washing three times with 1 ml of Hanks’ balanced salt solution (HBSS). After the BAL fluid was centrifuged at 280×g for 5 min, the cell pellet was washed twice with HBSS. For AMs, only large cells were counted and adjusted to 2.0 × 106 cells/ml with HBSS containing 20 mM HEPES.
Phagocytosis assays was performed using a Luminol Bead Assay kit (Kamakura Techno-Science Inc, Kamakura, Kanagawa, Japan). Briefly, 100 μl of cell suspensions were pre-warmed at 37 °C for 2 min and then mixed with pre-warmed 10 μl of Luminol-bound microbeads. The mixtures were incubated at 37 °C for 15 min. Active oxygen reacted to the phagocytosed microbeads within phagosomes. Chemiluminescence was then generated from microbeads. The signal intensity was quantified in a luminometer (Lumat LB9507, Berthold Technologies GmbH & Co KG, Bad Wildbad, German).
Statistical analysis
Statistical significance of viral load, body weight, cytokine induction, and phagocytosis were calculated using an unpaired two-tailed Student’s t-test. Correlations between the viral load and cytokine production were analyzed by calculating Pearson correlation coefficients. Levels of significance are represented as follows: *, P < 0.05; **, P < 0.01. Survival rates were compared using a log-rank test.
Results
Virus titers in lungs of SAMP1 mice and SAMR1 mice
The susceptibility of mice to influenza viruses depends on both the strain of mouse and the strain of influenza virus [46]. The PR8 virus was initially isolated from a human and subsequently adapted to mice. It is a commonly used strain employed for experimental influenza A virus infections in mice. We measured the 50 % lethal dose (LD50) of PR8 on BALB/c, C57BL/6, SAMP1, and SAMR1 mice. The most resistant strain among these mice was C57BL/6 (LD50 = 48.7 PFU), followed by BALB/c (LD50 = 21.8 PFU). SAMR1 and SAMP1 mice were equivalent to or somewhat more susceptible (LD50 = 19.1 PFU, 13.1 PFU, respectively) than BALB/c, but the difference between these two strains was not confirmed because of their low LD50 titer. Viral titers in the lungs of PR8-infected SAMP1 mice were significantly higher than those of SAMR1 mice (Fig. 1). This result suggests that SAMP1 mice are more susceptible and viral clearance from the body is delayed when compared with SAMR1 mice. The results also indicate that SAMP1 mice may have defects in their innate immune system. Therefore, SAMP1 mice are the better experimental animal model of a compromised immune system associated with aging.
Virus clearance was prolonged in SAMP1 mice compared with SAMR1 mice. SAMP1 mice and SAMR1 mice were infected intranasally with PR8 at 20 PFU/30 μl. At 2 (3 mice), 4 (3 mice), 6 (3 mice), and 8 (5 mice) dpi, mice were sacrificed, lungs were homogenized, and viral titers of the supernatant were determined using a plaque assay. Statistical significance was calculated using an unpaired two-tailed Student’s t-test. Levels of significance are represented as follows: *, P < 0.05; **, P < 0.01
SAMP1 mice and SAMR1 mice were inoculated intranasally with PR8 at 20 PFU/30 μl. Virus titers in lung homogenates were assayed. The virus titers in both SAMP1 mice and SAMR1 mice reached a maximum level at 4 dpi. While the virus titer was maintained at a high level until 6 dpi and decreased at 8 dpi in SAMP1 mice, the titer had begun to decrease significantly at 6 dpi in SAMR1 mice. Virus titers in SAMP1 were significantly higher than those in SAMR1 mice at 6 and 8 dpi (Fig. 1). These results indicate that SAMP1 mice are inferior to SAMR1 mice with regard to PR8 clearance from the body.
Effects of medication on the survival rate of PR8-infected SAMP1 mice
SAMP1 mice were divided into four groups. Group 1 was medicated with a combination of oseltamivir and HET (combination group); group 2 was medicated with only HET (HET group); group 3 was medicated with only oseltamivir (oseltamivir group); and group 4 received mock medication with drinking water (control group).
Two weeks after the start of HET administration, all mice were infected with PR8 at 20 PFU/30 μl, and survival rates were compared among the groups. Mice in the combination group and the oseltamivir group all survived. In the HET group, mice began to die at 10 dpi, and the final survival rate was 70.0 %. In the control group, mice began to die at 8 dpi, and the final survival rate was 57.1 %. The survival rates of the combination group and the oseltamivir group were significantly higher than that of the control group. However, there was no statistically significant difference in survival rates between the HET group and the control group or among the combination group, the HET group, and the oseltamivir group (Fig. 2). These results suggest that administration of HET alone is not effective against lethal PR8 infection in SAMP1 mice.
Administration of HET alone did not have a strong effect on preventing PR8 infection in SAMP1 mice. SAMP1 mice were divided into four groups as follows: combined administration of oseltamivir and HET group (Combination, filled square, 10 mice); HET stand-alone administration group (HET, filled circle, 10 mice); oseltamivir stand-alone administration group (Oseltamivir, open square, 10 mice); and non-medication group (Control, open circle, 7 mice). HET was administered in drinking water at 6 mg/ml for 2 weeks before and during infection. After 4 hours of infection, oseltamivir phosphate was administered by oral gavage at a dosage of 0.1 mg/200 μL twice daily for 5 days. Control-group mice were given water instead of oseltamivir in the same manner. PR8 infection was performed intranasally at 20 PFU/30 μl for all groups. Survival rates were compared using a log-rank test. Levels of significance are represented as follows: *, P < 0.05
Viral loads in lungs of SAMP1 mice medicated with oseltamivir and HET
SAMP1 mice were divided into four groups: the combination group, the HET group, the oseltamivir group, and the control group. Mice were infected with PR8 and sacrificed at 2, 5, and 8 dpi. Their lungs were analyzed for viral loads and cytokine levels.
The viral loads of the control group were in 2.8 × 106 PFU/ml, 5.8 × 106 PFU/ml, and 1.1 × 106 PFU/ml at 2, 5, and 8 dpi, respectively. Those of the HET group were 3.7 × 105 PFU/ml, 3.0 × 106 PFU/ml, and 6.8 × 105 PFU/ml at 2, 5, and 8 dpi, respectively. Those of the oseltamivir group were 4.5 × 104 PFU/ml, 2.7 × 105 PFU/ml, and 1.5 × 104 PFU/ml at 2, 5, and 8 dpi, respectively. Those of the combination group were 2.8 × 104 PFU/ml, 8.0 × 104 PFU/ml, and 37 PFU/ml at 2, 5, and 8 dpi, respectively (Fig. 3). Oseltamivir treatment resulted in a moderate decrease in the viral load (to 1.6 %, 4.8 %, and 1.3 % of the control at 2, 5, and 8 dpi, respectively). HET treatment resulted in a slight decrease in the viral load (to 13.3 %, 51.6 %, and 60.8 % of the control at 2, 5, and 8 dpi, respectively). In contrast, combined administration of oseltamivir and HET resulted in a considerable decrease in the viral load (to 1.0 %, 1.4 %, and 0.0033 % of the control at 2, 5, and 8 dpi, respectively). The combined treatment resulted in much lower amounts of virus compared with oseltamivir treatment alone at 8 dpi. Three independent experiments produced similar results.
These results suggest that concomitant treatment with oseltamivir and HET results in increased PR8 clearance.
Cytokine production in the lungs of mice infected with PR8
IL-12, IL-1β, and TNF-α levels in the HET group were significantly higher than those in the other three groups at 2 dpi, but there was no significant difference at 5 and 8 dpi (Fig. 4a-c). IL-6 levels in the oseltamivir group and the combination group were significantly lower than those in the other two groups at 2 and 5 dpi (Fig. 4d). IL-6 levels were elevated depending on the amount of virus present in the lungs (Fig. 4d). These observations demonstrate that the induction of IL-6 was strongly enhanced through stimulation by the propagated virus; however, because of this, it could not be clarified whether HET influenced the induction of IL-6. IFN-γ induction was significantly lower in the combination group compared with the HET group at 2 and 5 dpi and was also significantly lower in the oseltamivir group compared with the HET group at 2 dpi. IFN-γ levels showed a dramatic increase at 8 dpi in all four groups (Fig. 4e). IFN-γ may play an important role in PR8 infection; however, we could not verify a supplementary effect of HET on production of this cytokine.
Combined administration of oseltamivir and HET resulted in an increased effect on the reduction of the virus in the lungs. SAMP1 mice were medicated with oseltamivir and/or HET, followed by PR8 infection in the same manner as shown in Fig. 2, with the combined administration of oseltamivir and HET group (Combination, filled square); HET stand-alone administration group (HET, filled circle); oseltamivir stand-alone administration group (Oseltamivir, open square); and non-medication group (Control, open circle). At the dpis indicated, lungs were harvested and homogenized, and the virus titers of their supernatants were assayed using the plaque method (3 mice per group). Statistical significance was calculated using an unpaired two-tailed Student’s t-test. Levels of significance are represented as follows: **, P < 0.01
IFN-α production was only observed in the HET group and the control group at 5 dpi. The level of induction in these groups was similar (data not shown). IFN-β production levels were low. No noteworthy differences were observed among the four groups (Fig. 4f), which meant we were unable to confirm the effect of HET on production of this cytokine.
These findings indicate that HET stimulates the induction of IL-12, IL-1β, and TNF-α in the lungs at the early stage of PR8 infection.
Effect of HET on phagocytic activity of alveolar macrophages (AMs)
Mice in the HET group and the control group were either infected with PR8 or not infected. At 3 dpi, AMs were harvested by BAL, and their phagocytic ability was measured. Phagocytosis in the HET group was 2.4 times higher than in the control group in infected mice, showing a significant difference (Fig. 5a). Phagocytosis in the HET group was 1.9 times higher than that in the control group in uninfected mice (Fig. 5b).
HET treatment induced the activity of IL-12, IL-1β, and TNF-α at the early stage of PR8 infection. The experiment was performed as described in Fig. 3. Supernatants of homogenized lungs were examined by ELISA for induction of cytokines. Statistical significance was calculated using an unpaired two-tailed Student’s t-test. Levels of significance are represented as follows: *, P < 0.05; **, P < 0.01
Discussion
From our survival analysis data, we observed that administration of oseltamivir alone seemed to be sufficient for protection against PR8 (Fig. 2). Oseltamivir does, however, have some disadvantages; for example, the time period within which this medication is efficacious is limited, and it must be administered within 36 hours of the appearance of symptoms [14, 47]. Also, oseltamivir is not effective against any influenza-like illness caused by agents other than influenza type A and B viruses. There is also the threat of emergence of resistance mutations [30, 31, 48]. To compensate for these disadvantages, the concomitant administration of oseltamivir and a complementary drug is deemed to be a desirable treatment.
Our results suggest that administration of HET alone contributes to an improvement in the survival rates of mice following PR8 infection (Fig. 2), and it seemed to reduce the viral titer to some degree (Fig. 3), which is consistent with the results of our survival rate studies. Previous researchers have reported that HET could stimulate the mucosal immune system of the upper respiratory tract [35, 36], that HET exerted its inhibitory effect on influenza virus infection via an enhancement of the host immune responses in the researchers’ experimental murine system [37], and that HET helped elderly people increase their immunological capacity [49]. From these previous reports, we assume that the virus-reducing effect of HET in our experiments resulted from its immunostimulatory activity. The effect strongly assisted in viral clearance when given together with oseltamivir. HET also has the advantage of being able to be administered routinely without causing side effects. These results suggested, and we expected, that HET therefore had the potential to compensate for the disadvantages of the antiviral agent.
HET treatment enhanced phagocytosis in AMs harvested from both uninfected and PR8-infected SAMP1 mice. Mice of the HET stand-alone administration group (HET) and the non-medication group (Control) were infected intranasally with PR8 at 20 PFU/30 μl (a) or not infected (b). Mice were sacrificed at 3 dpi, and the AMs were harvested from BAL fluid. Phagocytic ability was assayed using a Luminol Bead Assay kit (4 mice per respective group). Statistical significance was calculated using an unpaired two-tailed Student’s t-test. Levels of significance are represented as follows: *, P < 0.05
Viral infection in the combination group was nearly eliminated from the lungs at 8 dpi (Fig. 3), when the acquired immunity of the mice was not yet very active. Therefore, it is likely that the innate immune response, which had been activated by HET treatment, contributed to this dramatic viral reduction. In the innate immune response, virus-specific molecules are recognized as pathogen-associated molecular patterns by pattern recognition receptors. Consequently, signals are transmitted to the nucleus, followed by the production of inflammatory cytokines (for example, IL-12, IL-1β, TNF-α, IL-6, and IFN-γ) and type 1 interferons (IFN-α and IFN-β), which are important for viral clearance. For this reason, we measured the production of these cytokines in the lungs of PR8-infected mice that were either medicated or not medicated with oseltamivir and/or HET to investigate the mechanisms of the increased antiviral effect.
We took particular note of IL-12, IL-1β, and TNF-α in the control group and the HET group. HET induced the production of these three cytokines at 2 dpi (Fig. 4a-c). We suspected that this elevation in inflammatory cytokines was related to a decrease in viral titers in the lung at 2 dpi (Figs. 3, 4a–c). To confirm our hypothesis, we plotted the values on a graph, with cytokine levels on the x-axis and the viral load on the y-axis, from individual mice from the HET group and the control group at 2 dpi from data obtained from the experiments detailed in Fig. 3 and Fig. 4. Data from the combination group and oseltamivir group were omitted to exclude any possible influence from oseltamivir on the viral load. We then investigated the possible correlation between the viral load and cytokine levels. We found a strong negative correlation between the viral load and the levels of IL-12, IL-1β, or TNF-α. Their correlation coefficients were −0.89 (P = 0.018), −0.76 (P = 0.082), and −0.97 (P = 0.001), respectively (Fig. 6a–c).
Production of IL-12, IL-1β, and TNF-α were inversely proportional to the viral load in the lungs. The viral load (y-axis) and cytokine production of IL-12, IL-1β, or TNF-α (x-axis) of the same individual mouse were plotted. Each marker indicates each individual mouse. Data were obtained from the HET stand-alone administration group and the non-medication group at 2 dpi (3 mice per group). Correlations between the viral load and cytokine production were analyzed by calculating Pearson correlation coefficients. Levels of significance are represented as follows: **, P < 0.01
Previous studies have demonstrated that IL-12, IL-1β, and TNF-α play a critical role in promoting innate immunity during influenza virus infection [50, 51]. We therefore assumed that HET contributed to a reduction in the viral load by elevating the production of these cytokines at the early stages of infection, thereby assisting in suppressing the explosive viral growth that normally follows. As an alternative, it is possible that the negative correlation observed resulted from the activation of AMs rather than directly involving the effects of these cytokines. This could be because these cytokines are produced by macrophages [52, 53]. We suggest that AMs became more active through HET stimulation, and this resulted in an elevation of the antiviral effect and cytokine production of AMs in response to PR8 infection.
To confirm whether HET activated AMs, we performed a phagocytosis assays. The results suggested that HET treatment increased the phagocytic activity of the AMs. This function became more recognizable especially during influenza virus infection (Fig. 5). From these results, it is suggested that HET has an immunostimulatory effect on AMs of SAMP1 mice in the early stages of PR8 infection. AMs play an important role in the prevention of influenza virus infection, as reported in other studies [54, 55]. We conclude that HET induces the activation of AMs, which results in a reduction in the viral load in the lungs in the early phase of the infection. Analysis of the viral load revealed that treatment with HET alone would be unlikely to prevent serious influenza virus infection because of its weak effect; however, the combined administration of oseltamivir and HET has a powerful increased effect against even serious influenza virus infections (Fig. 3).
Combination therapy cleared almost all viral infection from the lungs at 8 dpi. In contrast, administration of oseltamivir alone did not remove the virus at that same time point (Fig. 3). Our findings indicate that combined treatment with oseltamivir and HET promotes early clearance of influenza virus in SAMP1 mice. Early viral clearance has several advantages: First, it promotes improvement of symptoms. Second, it reduces the emergence of drug-resistant strains, because long-term virus shedding following neuraminidase inhibitor treatment increases the risk of the emergence of drug-resistant mutations [30, 31]. Third, it prevents the spread of infection. A previous investigation has demonstrated that fever duration was significantly shorter in patients treated with neuraminidase inhibitors than in untreated patients. However, the duration of virus shedding in patients treated with neuraminidase inhibitors was not significantly shorter than that in untreated patients. Therefore, on return to their communities after the alleviation of their clinical symptoms, it is still possible that they will spread influenza virus to healthy individuals [27].
The results from this study suggest that the combined administration of oseltamivir and HET is a potentially beneficial therapy, based on empirical data using a senescence-accelerated mouse model.
References
Webster RG, Wright SM, Castrucci MR, Bean WJ, Kawaoka Y (1993) Influenza–a model of an emerging virus disease. Intervirology 35(1–4):16–25
Webby RJ, Webster RG (2003) Are we ready for pandemic influenza? Science 302:1519–1522
Morse SS, Mazet JA, Daszak P et al (2012) Prediction and prevention of the next pandemic zoonosis. Lancet 380:1956–1965
Garten RJ, Davis CT, Cox NJ et al (2009) Antigenic and genetic characteristics of swine-origin 2009 A(H1N1) influenza viruses circulating in humans. Science 325(5937):197–201
Cheng VC, To KK, Tse H, Hung IF, Yuen KY (2012) Two years after pandemic influenza A/2009/H1N1: what have we learned? Clin Microbiol Rev 25(2):223–263
Dawood FS, Iuliano AD, Widdowson MA et al (2012) Estimated global mortality associated with the first 12 months of 2009 pandemic influenza A H1N1 virus circulation: a modelling study. Lancet Infect Dis 12(9):687–695
Perez, Sorrell EM, Donis RO (2005) Avian influenza: an omnipresent pandemic threat. Pediatr Infect Dis J 24(11 Suppl):S208–S216 discussion S215
Yong E (2012) Influenza: Five questions on H5N1 Nature 486:456–458
Imai M, Watanabe T, Kawaoka Y et al (2012) Experimental adaptation of an influenza H5 HA confers respiratory droplet transmission to a reassortant H5 HA/H1N1 virus in ferrets. Nature 486:420–428
Herfst S, Schrauwen EJ, Fouchier RA et al (2012) Airborne transmission of influenza A/H5N1 virus between ferrets. Science 336(6088):1534–1541
Russell CA, Fonville JM, Smith DJ et al (2012) The potential for respiratory droplet-transmissible A/H5N1 influenza virus to evolve in a mammalian host. Science 336(6088):1541–1547
Calfee DP, Hayden FG (1998) New approaches to influenza chemotherapy. Neuraminidase inhibitors. Drugs 56(4):537–553
Kim CU, Chen X, Mendel DB (1999) Neuraminidase inhibitors as anti-influenza virus agents. Antivir Chem Chemother 10(4):141–154
Bardsley-Elliot A, Noble S (1999) Oseltamivir. Drugs 58(5):851–860 discussion 861–862
Sidwell RW, Smee DF (2000) In vitro and in vivo assay systems for study of influenza virus inhibitors. Antiviral Res 48(1):1–16
Kashiwagi S, Yoshida S, Yamaguchi F et al (2012) Clinical efficacy of long-acting neuraminidase inhibitor laninamivir octanoate hydrate in postmarketing surveillance. J Infect Chemother [Epub ahead of print]
Ison MG, Hui DS, Alexander WJ et al (2012) A clinical trial of intravenous peramivir compared with oral oseltamivir for the treatment of seasonal influenza in hospitalized adults. Antivir Ther [Epub ahead of print]
Feng E, Ye D, Liu H et al (2012) Recent advances in neuraminidase inhibitor development as anti-influenza drugs. ChemMedChem 7(9):1527–1536
CDC HEALTH ADVISORY (2006) CDC recommends against the use of amantadine and rimantadine for the treatment or prophylaxis of influenza in the United States during the 2005–06 influenza season. CDCHAN-00240-2006-01-14-ADV-N
Deyde VM, Xu X, Klimov AI et al (2007) Surveillance of resistance to adamantanes among influenza A(H3N2) and A(H1N1) viruses isolated worldwide. J Infect Dis 196(2):249–257
Reece PA (2007) Presence of oseltamivir-resistant pandemic A/H1N1 minor variants before drug therapy with subsequent selection and transmission. J Med Virol 79(10):1577–1586
Järhult JD (2012) Oseltamivir (Tamiflu(®)) in the environment, resistance development in influenza A viruses of dabbling ducks and the risk of transmission of an oseltamivir-resistant virus to humans—a review. Infect Ecol Epidemiol 2:18385
Ghedin E, Holmes EC, Boivin G et al (2012) Presence of oseltamivir-resistant pandemic A/H1N1 minor variants before drug therapy with subsequent selection and transmission. J Infect Dis 206(10):1504–1511
Boivin G, Coulombe Z, Wat C (2003) Quantification of the influenza virus load by real-time polymerase chain reaction in nasopharyngeal swabs of patients treated with oseltamivir. J Infect Dis 188(4):578–580
Nicholson KG, Aoki FY, Osterhaus AD et al (2000) Efficacy and safety of oseltamivir in treatment of acute influenza: a randomised controlled trial. Lancet 355:1845–1850
Kiso M, Mitamura K, Kawaoka Y et al (2004) Resistant influenza A viruses in children treated with oseltamivir: descriptive study. Lancet 364(9436):759–765
Sato M, Hosoya M, Kato K, Suzuki H (2005) Viral shedding in children with influenza virus infections treated with neuraminidase inhibitors. Pediatr Infect Dis J 24:931–932
Baz M, Abed Y, McDonald J, Boivin G (2006) Characterization of multidrug-resistant influenza A/H3N2 viruses shed during 1 year by an immunocompromised child. Clin Infect Dis 43(12):1555–1561
Gooskens J, Jonges M, Claas EC, Meijer A, Kroes AC (2009) Prolonged influenza virus infection during lymphocytopenia and frequent detection of drug-resistant viruses. J Infect Dis 199(10):1435–1441
Graitcer SB, Gubareva L, Fry AM et al (2011) Characteristics of patients with oseltamivir-resistant pandemic (H1N1) 2009, United States. Emerg Infect Dis 17(2):255–257
Mehta T, McGrath E, Alangaden GJ et al (2010) Detection of oseltamivir resistance during treatment of 2009 H1N1influenza virus infection in immunocompromised patients: utility of cycle threshold values of qualitative real-time reverse transcriptase PCR. J Clin Microbiol 48(11):4326–4328
Yamaoka Y, Kawakita T, Nomoto K (2001) Protective effect of a traditional Japanese medicine Hochu-ekki-to (Chinese name: Bu-zhong-yi-qi-tang) on the susceptibility against Listeria monocytogenes in infant mice. Int Immunopharmacol 1:1669–1677
Kataoka T, Akagawa KS, Tokunaga T, Nagao S (1989) Activation of macrophages with Hochu-ekiito. Jpn J Cancer Chemother 16:1490–1493
Utsuyama M, Seidler H, Kitagawa M, Hirokawa K (2001) Immunological restoration and anti-tumor effect by Japanese herbal medicine in aged mice. Mech Ageing Dev 122:341–352
Kiyohara H, Nagai T, Yamada H et al (2006) Stimulating effect of Japanese herbal (kampo) medicine, hochuekkito on upper respiratory mucosal immune system. Evid Based Complement Alternat Med 3(4):459–467
Kiyohara H, Nonaka K, Yamada H et al (2011) Polysaccharide-containing macromolecules in a kampo (traditional Japanese herbal) medicine, hochuekkito: dual active ingredients for modulation of immune functions on intestinal peyer’s patches and epithelial cells. Evid Based Complement Alternat Med 2011:492691
Mori K, Kido T, Komatsu Y et al (1999) Effect of Hochu-ekki-to (TJ-41), a Japanese herbal medicine, on the survival of mice infected with influenza virus. Antiviral Res 44(2):103–111
Abe S, Tansho S, Yamaguchi H et al (1999) Protection of immunosuppressed mice from lethal Candida infection by oral administration of a Kampo medicine, hochu-ekki-to. Immunopharmacol Immunotoxicol 21:331–342
Hossain MS, Takimoto H, Nomoto K et al (1999) Protective effects of hochu-ekki-to, a Chinese traditional herbal medicine against murine cytomegalovirus infection. Immunopharmacology 41(3):169–181
Kido T, Mori K, Sasaki H et al (2000) The protective effect of hochu-ekki-to (TJ-41), a Japanese herbal medicine, against HSV-1 infection in mitomycin C-treated mice. Anticancer Res 20(6A):4109–4113
Yamaya M, Sasaki T, Nakayama K et al (2007) Hochu-ekki-to inhibits rhinovirus infection in human tracheal epithelial cells. Br J Pharmacol 150(6):702–710
Hosokawa T, Hosono M, Takeda T et al (1987) Immune responses in newly developed short-lived SAM mice. I. Age-associated early decline in immune activities of cultured spleen cells. Immunology 62:419–423
Hosokawa T, Hosono M, Takeda T et al (1987) Immune responses in newly developed short-lived SAM mice. II. Selectively impaired T-helper cell activity in in vitro antibody response. Immunology 62:425–429
Hanada K, Hosono M, Takeda T et al (1989) Immune responses in newly developed short-lived SAM mice. III. Genetic control of defective helper T-cell activity in in vitro primary antibody response. Immunology 68:540–546
Guo Z, Toichi E, Mori M et al (2000) Genetic analysis of lifespan in hybrid progeny derived from the SAMP1 mouse strain with accelerated senescence. Mech Ageing Dev 118:35–44
Bouvier NM, Lowen AC (2010) Animal models for influenza virus pathogenesis and transmission. Viruses 2(8):1530–1563
Treanor JJ, Hayden FG, Mills RG et al (2000) Efficacy and safety of the oral neuraminidase inhibitor oseltamivir in treating acute influenza: a randomized controlled trial. JAMA 283(8):1016–1024
Ward P, Small I, Smith J, Suter P, Dutkowski R (2005) Oseltamivir (Tamiflu) and its potential for use in the event of an influenza pandemic. J Antimicrob Chemother 55(Suppl 1):i5–i21
Kuroiwa A, Liou S, Nagayama A et al (2004) Effect of a traditional Japanese herbal medicine, hochu-ekki-to (Bu-Zhong-Yi-Qi Tang), on immunity in elderly persons. Int Immunopharmacol 4(2):317–324
Julkunen I, Melén K, Matikainen S et al (2000) Inflammatory responses in influenza A virus infection. Vaccine 19(Suppl 1):S32–S37
Sládková T, Kostolanský F (2006) The role of cytokines in the immune response to influenza A virus infection. Acta Virol 50(3):151–162
Cavaillon JM (1994) Cytokines and macrophages. Biomed Pharmacother 48(10):445–453
Ellermann-Eriksen S (2005) Macrophages and cytokines in the early defence against herpes simplex virus. Virol J 2:59
Wang J, Nikrad MP, Mason RJ et al (2012) Innate immune response of human alveolar macrophages during influenza A infection. PLoS One 7(3):e29879
Short KR, Brooks AG, Reading PC, Londrigan SL (2012) The fate of influenza A virus after infection of human macrophages and dendritic cells. J Gen Virol 93(Pt 11):2315–2325
Acknowledgements
This work was supported by JSPS KAKENHI Grant Number 19590697 and Japan Kampo Medicines Manufacturers Association.
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ohgitani, E., Kita, M., Mazda, O. et al. Combined administration of oseltamivir and hochu-ekki-to (TJ-41) dramatically decreases the viral load in lungs of senescence-accelerated mice during influenza virus infection. Arch Virol 159, 267–275 (2014). https://doi.org/10.1007/s00705-013-1807-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00705-013-1807-3