Abstract
Aims
High glucose levels and Glucose-6-Phosphate Dehydrogenase deficiency (G6PDd) have both tissue inflammatory effects. Here we determined whether G6PDd accelerates arterial aging (information linked stiffening) in diabetes.
Methods
Plasma glucose, interleukin 6 (IL6), and arterial stiffness (indexed as carotid-femoral Pulse Wave Velocity, PWV) and red blood cell G6PD activity were assessed in a large (4448) Sardinian population.
Results
Although high plasma glucose in diabetics, did not differ by G6DP status (178.2 ± 55.1 vs 169.0 ± 50.1 mg/dl) in G6DPd versus non-G6PDd subjects, respectively, IL6, and PWV (adjusted for age and glucose) were significantly increased in G6PDd vs non-G6PDd subjects (PWV, 8.0 ± 0.4 vs 7.2 ± 0.2 m/sec) and (IL6, 6.9 ± 5.0 vs 4.2 ± 3.0 pg/ml). In non-diabetics, neither fasting plasma glucose, nor IL6, nor PWV were impacted by G6PDd.
Conclusion
G6PDd in diabetics is associated with increased inflammatory markers and accelerated arterial aging.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
High glucose levels in diabetics are associated with reduced glucose-6-phosphate dehydrogenase (G6PD) activity [1,2,3], decreased levels of the reduced form of nicotinamide adenine dinucleotide phosphate (NADPH) cellular levels and increased pro-inflammatory markers, and accelerated arterial aging due to stiffening of large arteries [4].
Cytosolic NADP + /NADPH ratio which in fact is regulated by G6PD activity impacts on glucose metabolism, nucleotide and aromatic amino acid synthesis [5], and also regulates the level of Reactive Oxygen Species (ROS): G6PD-deficient cells are sensitive to oxidizing stimuli and more easily succumb to oxidative stress than non-G6DP deficient cells [6]. Exposure to high glucose levels decreases G6PD activity, triggering an insufficient NADPH supply and accumulation of ROS in different tissues [1,2,3], which activate proinflammatory pathways in G6PD deficiency [7].
Arterial aging can be evaluated as arterial stiffness (indexed as carotid-femoral Pulse Wave Velocity—PWV) [8], which captures the continuum from the early (accelerated) vascular aging to the “lower than average” arterial aging, i.e. Healthy Vascular Aging [9]; is associated with CV mortality and disability independently of conventional CV risk factors [10,11,12]. Additionally, we firstly reported and, then, confirmed that specific clusters of metabolic alterations are selectively associated with arterial aging [4, 13].
The island of Sardinia is characterized by the highest prevalence (~ 8–15%) in G6PD deficiency, worldwide [14]. The aim of the present study was to investigate the impact of diabetes mellitus on plasma inflammatory markers and arterial stiffness in subjects with and without G6PD deficiency in a large Sardinian population.
Research design and methods
Red blood cell G6PD activity was determined using a quantitative assay in a 4448 (1879 men and 2569 women) participants of the SardiNIA Study aged 30 + years [15].
Blood pressure, anthropometry, metabolic risk factors, and cytokine levels were measured as previously described [4]. G6PD deficiency was defined as G6PD activity < 0.8 UI/g Hb.
Diabetes was defined according to American Diabetic Association definition [16]. Arterial Stiffness was measured as carotid-femoral Pulse Wave Velocity (PWV) [15]. Given that PWV is a highly age-associated trait, Healthy Vascular Ageing (HVA) and Early Vascular Ageing (EVA) were defined, respectively, and as a PWV value below the age-quintile specific 10th percentile, and as a PWV value above the age-quintile specific 90th percentile [9].
Using SAS University, ANCOVA analysis -including age and glucose levels as covariates- tested for interaction between diabetes mellitus and G6PD deficiency.
Results
Diabetes was associated with greater levels of glucose and PWV (Table 1), in non-diabetics, glucose levels and PWV did not differ with those subjects with normal or deficient levels of G6PD activity. In diabetics G6PD deficient subjects had significantly greater IL6 levels, and PWV compared to diabetic subjects without G6PD deficiency. The significant (p < 0.05) interaction of Diabetes withG6PD deficiency for all the three variables mentioned above indicated that the impact of G6PD deficiency on glucose levels, arterial stiffness, and IL6 levels significantly differed according to the presence of diabetes. Of note, although HVA was more common in non-diabetics with G6PD deficiency, a significantly greater proportion of subjects with stiffer arteries (EVA, a PWV value above the age-quintile specific 90th percentile) was observed in diabetic subjects with G6PD deficiency.4
Although, PWV increases with both age and higher glucose levels, after adjustment for age and glucose, differences in PWV and IL6 in diabetics with and without G6PD deficiency remained significant.
Conclusions
This is the first study to demonstrate that G6PD deficiency in diabetics, but not non-diabetics, is associated with higher plasma IL6 levels and stiff arteries.
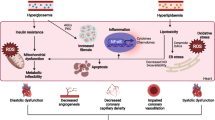
The observation of increased IL6 levels deserves further comment. Adipose tissue inflammation has more and more emerged as a critical path with complex regulation [17, 18] leading to adipose tissue and, then, to systemic insulin resistance—a key step in the onset of type 2 diabetes mellitus [19]. The hypothesized time-dependent alterations start with adipocyte hypertrophy, followed by increased levels of macrophage stimulating factor and eventually with higher IL-6 levels in plasma [19, 20]. Therefore, IL6 circulating levels are a facet of mechanistically relevant alteration occurring at adipose tissue level.
Notably, genetic loci recently identified are associated with insulin resistance at a lower level of adiposity [21] and promote endothelium-specific insulin resistance [22].
Endothelial insulin-resistance may trigger alteration in vascular extracellular matrix composition and increased oxidative stress of its components [23]. Alteration in vascular extracellular matrix composition is emerging as key determinant of greater arterial stiffness and accelerated arterial aging [24].
Of note, G6PD deficiency is further reduced by nonenzymatic glycation in states of hyperglycemia, creating a self-reinforcing loop [25], reducing endothelial nitric oxide bioavailability [26, 27] and increasing oxidative stress with activation of proinflammatory pathways in G6PD [7], eventually resulting in arterial stiffening and remodelling [28].
Future studies are needed to clarify tissue-specific G6PD contribution to arterial stiffening in diabetic subjects, and its possible role for the development of new therapeutic agents able to reduce the cardiovascular burden of diabetes mellitus.
References
Xu Y, Osborne BW, Stanton RC (2005) Diabetes causes inhibition of glucose-6-phosphate dehydrogenase via activation of PKA, which contributes to oxidative stress in rat kidney cortex. Am J Physiol Renal Physiol 289:F1040–F1047. https://doi.org/10.1152/ajprenal.00076.2005
Zhang Z, Liew CW, Handy DE et al (2010) High glucose inhibits glucose-6-phosphate dehydrogenase, leading to increased oxidative stress and beta-cell apoptosis. FASEB J 24:1497–1505. https://doi.org/10.1096/fj.09-136572
Zhang W, Ni C, Sheng J et al (2013) 2013 TLQP-21 protects human umbilical vein endothelial cells against high-glucose-induced apoptosis by increasing G6PD expression. PLoS ONE 8:e79760. https://doi.org/10.1371/journal.pone.0079760
Scuteri A, Najjar SS, Orru’ M et al (2010) The central arterial burden of the metabolic syndrome is similar in men and women: the SardiNIA Study. Eur Heart J 31:602–613. https://doi.org/10.1093/eurheartj/ehp491
Frederiks WM, Kummerlin IP, Bosch KS et al (2007) NADPH production by the pentose phosphate pathway in the zona fasciculata of rat adrenal gland. J Histochem Cytochem 55:975–980. https://doi.org/10.1369/jhc.7A7222.2007
Tian WN, Braunstein LD, Apse K et al (1999) Importance of glucose-6-phosphate dehydrogenase activity in cell death. Am J Physiol Cell Physiol 276:C1121–C1131. https://doi.org/10.1152/ajpcell.1999.276.5.C1121
Ham M, Lee J-W, Choi AH (2013) Macrophage glucose-6-phosphate dehydrogenase stimulates proinflammatory responses with oxidative stress. Mol Cell Biol 33:2425–2435. https://doi.org/10.1128/MCB.01260-12
Calimport SRG, Bentley BL, Stewart CE et al (2019) To help aging populations, classify organismal senescence. Science 366:576–578. https://doi.org/10.1126/science.aay7319
Nilsson PN, Laurent S, Cunha PG et al (2018) Characteristics of healthy vascular ageing in pooled population-based cohort studies: the global Metabolic syndrome and Artery REsearch (MARE) Consortium. J Hypertens 36:2340–2349. https://doi.org/10.1097/HJH.0000000000001824
Scuteri A, Rovella V, Alunni Fegatelli D et al (2018) An operational definition of SHATS (systemic hemodynamic atherosclerotic syndrome): role of arterial stiffness and blood pressure variability in elderly hypertensive subjects. Int J Cardiol 263:132–137. https://doi.org/10.1016/j.ijcard.2018.03.117
Vlachopoulos C, Aznaouridis K, Stefanadis C (2010) Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. JACC 55:1318–1327. https://doi.org/10.1016/j.jacc.2009.10.061
Scuteri A, Benetos A, Sierra C et al (2021) Routine assessment of cognitive function in older patients with hypertension seen by primary care physicians: why and how-a decision-making support from the working group on hypertension and the brain’ of the European Society of Hypertension and from the European Geriatric Medicine Society. J Hypertens 39:90–100. https://doi.org/10.1097/HJH.0000000000002621
Scuteri A, Cunha PG, Agabiti Rosei E et al (2014) Arterial stiffness and influences of the metabolic syndrome: a cross-countries study. Atherosclerosis 233:654–660. https://doi.org/10.1016/j.atherosclerosis.2014.01.041
Cocco P, Todde P, Fornera S, Manca MB, Manca M, Sias AR (1998) Mortality in a cohort of men expressing the Glucose-6-Phosphate Dehydrogenase deficiency. Blood 91:706–709
Scuteri A, Morrell CH, Orru’ M, AlGhatrif M, Saba PS, Terracciano A et al (2016) Gender specific profiles of white coat and masked hypertension impacts on arterial structure and function in the SardiNIA study. Int J Cardiol 217:92–98. https://doi.org/10.1016/j.ijcard.2016.04.172
American Diabetes Association (2010) Diagnosis and classification of diabetes mellitus. Diabetes Care 33(Suppl 1):S62–S69. https://doi.org/10.2337/dc10-S062
Britton KA, Massaro JM, Murabito JM, Kreger BE, Hoffmann U, Fox CS (2013) Body fat distribution, incident cardiovascular disease, cancer, and all-cause mortality. JACC 62:921–925. https://doi.org/10.1016/j.jacc.2013.06.027
Feraco A, Marzolla V, Scuteri A, Armani A, Caprio M (2020) Mineralocorticoid receptors in metabolic syndrome: from physiology to disease. Trends Endocrinol Metab 31:205–217. https://doi.org/10.1016/j.tem.2019.11.006
Perry RJ, Camporez JG, Kursawe R, Titchenell PM, Zhang D, Perry CJ et al (2015) Hepatic acetyl CoA links adipose tissue inflammation to hepatic insulin resistance and type 2 diabetes. Cell 160:745–758. https://doi.org/10.1016/j.cell.2015.01.012
Scherer PE (2019) The many secret lives of adipocytes: implications for diabetes. Diabetologia 62:223–232. https://doi.org/10.1007/s00125-018-4777-x
Shungin D, Winkler TW, Croteau-Chonka DC et al (2015) New genetic loci link adipose and insulin biology to body fat distribution. Nature 518:187–196. https://doi.org/10.1038/nature14132
Bacci S, Prudente S, Copetti M et al (2013) Joint effect of insulin signaling genes on cardiovascular events and on whole body and endothelial insulin resistance. Atherosclerosis 226:140–145. https://doi.org/10.1016/j.atherosclerosis.2012.10.035
Stöhr R, Kappel BA, Carnevale D et al (2015) TIMP3 interplays with apelin to regulate cardiovascular metabolism in hypercholesterolemic mice. Mol Metab 4:741–752. https://doi.org/10.1016/j.molmet.2015.07.007
Lacolley P, Regnault V, Laurent S (2020) Mechanisms of arterial stiffening: from mechano-transduction to epigenetics. Arterioscler Thromb Vasc Biol 40:1055–1062. https://doi.org/10.1161/ATVBAHA.119.313129
Leong A, Lim VJY, Wang C et al (2020) Association of G6PD variants with hemoglobin A1c and impact on diabetes diagnosis in East Asian individuals. BMJ Open Diabetes Res Care 8(1):e001091. https://doi.org/10.1136/bmjdrc-2019-001091
Leopold JA, Cap A, Scribner AW, Stanton RC, Loscalzo J (2001) Glucose-6-phosphate dehydrogenase deficiency promotes endothelial oxidant stress and decreases endothelial nitric oxide bioavailability. FASEB J 15:1771–1773. https://doi.org/10.1096/fj.00-0893fje
Scuteri A, Stuehlinger MC, Cooke JP et al (2003) Nitric oxide inhibition as a mechanism for blood pressure increase during salt loading in normotensive postmenopausal women. J Hypertens 21:1339–1346. https://doi.org/10.1097/00004872-200307000-00023
AlGhatrif M, Lakatta EG, Morrell CH et al (2023) Dilated hypertrophic phenotype of the carotid artery is associated with accelerated age-associated central arterial stiffening. Geroscience 45:1001–1013. https://doi.org/10.1007/s11357-022-00699-w
Acknowledgements
AS: contributed to study conceptualization and to planning of the SardiNIA Study; drafted the manuscript. CHM: contributed to data analysis. MAG: contributed to study implementation. EF: contributed to the recruitment of study participants. MM: contributed to data collection and cleaning. DS: contributed to Study Funding and to planning of the SardiNIA Study. FC: contributed to Study Funding and to planning of the SardiNIA Study. EGL: contributed to study conceptualization, to Study Funding, and to planning of the SardiNIA: Study. All Authors critically reviewed and edited the manuscript and subsequently approved the submitted version to be published
Funding
Open access funding provided by Università degli Studi di Cagliari within the CRUI-CARE Agreement. This research was supported in part by the Intramural Research Program of the US National Institutes of Health, National Institute on Aging (No. HHSN271201600005C).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No Author has any conflict of interest to disclose.
Ethical approval
The present study complies with the Declaration of Helsinki, that the locally appointed ethics committee has approved the research protocol.
Informed consent
Informed consent has been obtained from the subjects (or their legally authorized representative).
Additional information
Managed By Massimo Federici.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Scuteri, A., Morrell, C.H., AlGhatrif, M. et al. Glucose-6-phosphate dehydrogenase deficiency accelerates arterial aging in diabetes. Acta Diabetol 61, 127–130 (2024). https://doi.org/10.1007/s00592-023-02118-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-023-02118-8