Abstract
Gut microbiota and its metabolites have been shown to influence multiple physiological mechanisms related to human health. Among microbial metabolites, short-chain fatty acids (SCFA) are modulators of different metabolic pathways. On the other hand, several studies suggested that diet might influence gut microbiota composition and activity thus modulating the risk of metabolic disease, i.e. obesity, insulin resistance and type 2 diabetes. Among dietary component, dietary fibre may play a pivotal role by virtue of its prebiotic effect on fibre-fermenting bacteria, that may increase SCFA production. The aim of this review was to summarize and discuss current knowledge on the impact of dietary fibre as modulator of the relationship between glucose metabolism and microbiota composition in humans. More specifically, we analysed evidence from observational studies and randomized nutritional intervention investigating the relationship between gut microbiota, short-chain fatty acids and glucose metabolism. The possible mechanisms behind this association were also discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The gut microbiota is a complex and dynamic ecosystem that interacts with the host while maintaining a mutualistic relationship with it. Indeed, it may influence multiple physiological mechanisms related to human health, i.e. synthesis of micronutrients, defence against pathogens, regulation of glucose and lipid metabolism, and immune function [1].
Therefore, it has been suggested that the modulation of gut microbiota could be a reliable tool to prevent metabolic and inflammatory diseases. In particular, animal studies support a causal role between the composition of the gut microbiota and development of obesity, insulin resistance and type 2 diabetes (T2D). In addition, observational studies have confirmed the presence of altered gut microbiota composition, named “dysbiosis”, in prediabetic or T2D patients compared to healthy subjects [2, 3]. However, no specific microbial communities related to the onset of these diseases have been identified so far.
Nevertheless, more evidence is available on the microbial activities linked to the beneficial effect of the gut microbiota against T2D [4]. The main mechanisms can be summarized as follows: (1) maintenance of the integrity of intestinal barrier; (2) reduction in bacteria translocation and, consequently, systemic inflammation (endotoxemia); (3) production of short-chain fatty acids (SCFA) (acetate, propionate and butyrate) which can influence metabolic pathways [5].
The first two effects (maintenance of intestinal barrier and reduction in endotoxemia) seem to be more closely linked to the onset of diseases. Conversely, the production of SCFA could represent a tool to both prevent and modulate T2D [6, 7].
Against this background, several researches have been carried out to identify potential strategies to induce specific changes in the gut microbiota composition towards microbial species with high fermentative activity.
Gut microbiota composition is influenced by internal and external factors. Recently, it was shown that genetics plays a marginal role in the definition of microbiota composition [8]. As for external factors, faecal transplantations and antibiotics have dramatic but temporary effects on the host microbiota [9]. Conversely, dietary changes could be more effective to induce lasting changes in the composition of gut microbiota. Among dietary components, dietary fibres play a pivotal role. In fact, it is well known that fibres are the main substrate for bacterial metabolism. Furthermore, recent findings demonstrated that habitual fibre intake can endorse a “virtuous cycle”, consisting in the overgrowth of fibre-fermenting microbial groups while inhibition of other species [10].
Within this context, the prebiotic effect of dietary fibres might be a feasible strategy to prevent T2D, through the modulation of metabolic response. However, to date, there is no conclusive evidence to support this thesis, likely due to the lack of studies focusing primarily on the relationship between the composition of the gut microbiota and metabolic response.
Therefore, in this review, we summarized current evidence from observational and intervention studies performed in humans investigating the relationship between the composition of the gut microbiota, concentration of SCFA and glucose metabolism. Furthermore, the possible mechanisms underlying this association were also discussed.
Methods
Literature searching for this review was conducted by searching PubMed database for observational studies and randomized controlled clinical trials on humans adults published in the English language, during the last 20 years. The terms “dietary fibre OR fibre OR fibre-rich diet”, “short-chain fatty acids OR butyrate OR acetate OR propionate”, “microbiota OR microbiome OR bacteria”, “type 2 diabetes OR prediabetes OR glucose intolerance OR insulin resistance OR insulin response”, combined with the Boolean operator “AND”, were employed for the research.
This review includes studies published in journals in the highest impact factor quartile in the “Endocrinology and Metabolism” or “Nutrition and Dietetics” areas. We excluded reviews, acute studies and those not specifically related to each issue of interest. Overall, our search retrieved a total of 18 studies suitable for our review, 10 observational studies and 8 randomized controlled trials (Fig. 1).
Observational studies
Observational studies showed that the composition of the gut microbiota is strictly related to the host metabolic state (Table 1). In particular, two large cohort studies [11, 12] analysed the composition of microbiota into three groups of individuals with different glucose tolerance: normal glucose tolerance, prediabetes and T2D. Greater abundance of butyrate-producing bacteria was observed in individuals with normal glucose tolerance than the other two groups.
In line with these results, metagenomic studies showed significant differences in the composition of the gut microbiota of healthy patients compared to diabetic patients in two separate cohorts in China and Europe. In particular, Roseburia and Faecalibacterium prausnitzii were identified as highly discriminating bacteria between normoglycaemic individuals and those with T2D [13, 14]. In addition, in a cohort of 900 healthy individuals, Senna et al. [15] observed that the abundance of butyrate-producing bacteria is associated with a better insulin response during an oral glucose tolerance test, i.e. a proxy of improved β cell function.
Looking at how dietary habits may influence the composition of the gut microbiota, the study by De Filippo et al. [16] pointed out relevant differences in the composition of gut microbiota in children from Africa and Italy. Specifically, African children had increased Bacteroides (mainly Prevotella and Xylanibacter) and reduced Firmicutes, whereas Italian children presented an inverse trend. This finding can be ascribed to different dietary habits in the two cohorts: the former used to a plant-based diet (minor cereals like millet and sorghum, legumes and vegetables) than the latter consuming an animal-based diet rich in fat and protein. This hypothesis is supported by the presence of bacterial strains that hydrolyse fibres, in particular cellulose and xylans, inducing a greater production of faecal SCFA in African children compared to Italian children.
As for other dietary pattern, the relationship between Mediterranean Diet (MD), characterized by a high-fibre intake, and microbial fermentation was explored in different studies. Many authors highlighted that the more adhesion to MD, the greater increase of Bacteroides abundance, mainly Prevotella [17, 18], or Bifidobacteria [19] and Roseburia [20]. In addition, in all these studies individuals more compliant with MD showed increased concentrations of faecal butyrate or faecal propionate [17,18,19,20].
Intervention trials
Randomized nutritional trials focusing on dietary modulation of microbial composition and activity were carried out using high-fibre diets or fibre-rich foods (Table 2).
As for high-fibre diets, a short-term randomized controlled clinical trials (4 days) in a small group of healthy individuals compared the prebiotic effect of a Western diet (WD) –based on the consumption of animal foods (meat, eggs and cheese)—with low fibre intake (9.36 ± 2.1 g/1000 kcal) or a plant-based diet, rich in fibre (25.6 ± 1.1 g/1000 kcal) from wholegrains, legumes, fruits and vegetables. The results showed that plant-based diet increased plant-polysaccharide metabolizing bacteria (Prevotella and Roseburia) with an higher concentration of faecal SCFA in particular butyrate, as compared to Western diet [21].
More recently, an 8-week Mediterranean diet, rich in fibre (fibre: 19.3 ± 3.1 g/1000 kcal), has shown to increase Intestinimonas butyriciproducens and Akkermansia muciniphila abundance, and postprandial plasma butyrate concentrations, with an improvement in postprandial glucose and insulin sensitivity in individuals with high cardiometabolic risk, compared to Control Diet (fibre: 8.1 ± 2.3 g/1000 kcal). Interestingly, butyrate concentrations directly correlated with postprandial insulin sensitivity, evaluated by OGIS [22].
Even in individuals with T2D, a 12-week high-fibre diet (fibre: 37.1 ± 1.9 g) has shown to increase faecal butyrate concentrations that associated with the reduction in fasting glucose and HbA1c concentrations [23].
In addition, another trial in a small group of individuals with metabolic syndrome has demonstrated that plant-based diets may selectively increase some bacterial species, depending on the type of fibres consumed. Indeed, in a long-term clinic trial (1 year), a high-fibre diet (fibre: 14.1 ± 0.2 g/1000 kcal mainly from wholegrains) increased Prevotella, while Mediterranean Diet (fibre: 12.9 ± 0.2 g/1000 kcal, mainly from vegetables and nuts) enhanced Roseburia abundance. Meanwhile both diets increased Faecalibacterium prausnitzii. Interestingly, an improved insulin sensitivity was observed after both diets [24].
Among high-fibre foods, wholegrains have been extensively studied by virtue of their high fibre content. Indeed, it has been shown that cereal fibre (arabinoxylans and bran) is highly fermentable and may increase faecal short-chain fatty acid concentrations after just 4 weeks [25].
Moreover, a 12-week wholegrain-based diet (cereal fibre: 28.9 ± 1.1 g/day) has shown to increase plasma propionate concentration compared to a refined-cereal-based diet used as control (cereal fibre: 11.8 ± 0.4 g/day), and this increase correlated with an improved insulin postprandial response in individuals with Metabolic Syndrome [26].
As for the effect of specific foods, two studies [27, 28] have showed that the consumption of barley kernel-based bread (fibre: 37.6 g/day) increased Prevotella while reduced Bacteroides after only 3 days compared to wheat bread (fibre: 9.1 g/day) in healthy volunteers. This change was associated with the reduction in postprandial glucose response [27, 28] which correlated with the increased total serum SCFA concentration [28].
In conclusion, although many studies have been performed in small groups and with a short duration, the results from the main intervention trials (Table 2) indicate that high-fibre diets and fibre-rich foods are able to improve glucose metabolism and this improvement is associated with changes in gut microbiota and increased SCFA concentration.
Possible mechanisms of action
Dietary fibre has shown to influence glucose metabolism by several mechanisms in healthy individuals and people with T2D, mainly driven by its functional properties (viscosity, water solubility, and fermentation rate) [29]. New insights into the capacity of dietary fibre to modulate microbial composition and activity triggered more attention on microbial metabolites, particularly SCFA.
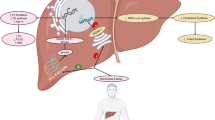
Accumulating evidence supports local—meaning in gastrointestinal tract—and systemic effect of SCFA that might affect glucose metabolism (Fig. 2).
Studies in vitro and in vivo showed that SCFA are potent secretagogues for glucagon-like peptide‑1 (GLP-1) and peptide YY (PYY) that increase satiety feeling through the gut–brain axis. As a consequence, they might indirectly reduce appetite and consequent food intake, thus preventing body weight gain, a well-known risk factor T2D. Moreover, SCFA might regulate blood glucose concentrations through a GLP-1-mediated increase in insulin secretion [30].
In the liver, SCFA has shown to decrease glycolysis and gluconeogenesis, and to increase glycogen synthesis and fatty acids oxidation [30,31,32,33,34].
As for extra intestinal effects, SCFA have shown to improve glucose uptake in skeletal muscle and adipose tissue by increasing the expression of GLUT4, through AMP Kinase (AMPK) activity. In addition, in the skeletal muscle, SCFA reduce glycolysis with a consequent accumulation of glucose-6-phosphate and increase in glycogen synthesis [31,32,33,34,35,36,37].
The possible effects of SCFA, in particular butyrate and propionate, in the modulation of glucose metabolism in humans, pushed to carry out intervention studies with propionate and butyrate supplementation. However, the evidence is not conclusive since the studies are few and have been performed in small groups of individuals. Nevertheless, they seem to indicate that: 1) an inulin-propionate supplementation (10 g/day) increases GLP-1 and PYY, and reduces food intake [38, 39] thus contributing to body weight regulation, and 2) sodium butyrate supplementation (4 g/day) improves insulin sensitivity only in lean subjects and not in individuals with metabolic syndrome [40].
Conclusion
Based on the current evidence, gut microbiota might play a pivotal role in the regulation of glucose metabolism and, therefore, may be associated with a reduction in type 2 diabetes risk. As already mentioned in Introduction, this association may be mediated by several mechanisms (i.e. maintenance of the integrity of intestinal barrier, reduced endotoxemia, and production of microbial metabolites). Some bacteria (i.e. Akkermansia muciniphila, Lactobacillus and Bifidobacteria) may reduce intestinal permeability and inflammation [5, 41]. As for microbial metabolites, short-chain fatty acids (SCFAs) have shown pleiotropic effects in different sites that regulate glucose metabolism. SCFAs acids are produced by microbiota through the fermentation of dietary fibre. At the same time, a fibre-rich diet has shown a prebiotic effect towards SCFA-producing microbial species (i.e. Roseburia, Faecalibacterium prausnitzii, Prevotella) [42, 43]. This evidence supports microbiota as key actor in the interplay between fibre intake and the prevention and management of metabolic diseases.
Therefore, the well-known effect of dietary fibres in preventing T2D [44] may be explained, at least in part, also throughout this mechanism. Unfortunately, no studies have evaluated specifically whether soluble and insoluble fibres may differently affect microbiota. According to fibre used in the studies (i.e. β-glucan and arabinoxylans from wholegrains, pectins from fruit, vegetables, and legumes, and resistant starch), it could be hypothesized that soluble readily fermented fibres might be more effective in mediating the interplay between diet and microbiota in the improvement of glucose homeostasis than other types of fibres [29]. Conversely, insoluble fibre might reduce T2D risk through other mechanisms (i.e. promoting body weight management, increasing faecal glucose-excretion) [29, 45].
Therefore, individuals with prediabetes or diabetes should be advised to increase dietary fibre intake, favouring the consumption of wholegrain, legumes, fruit and vegetables. So far, no recommendation can be stated for fibre supplements or SCFA-based formulations.
Another point to consider is that the relationship between fibre intake, SCFAs, and microbiota has been observed in the context of traditional diets. More extreme diets (i.e. carbohydrate-restricted and ketogenic diets) have shown dramatic effects on microbiota composition and activity. Indeed, a reduction in SCFA-producing microbial species and Bifidobacteria, and SCFAs concentrations has been observed after short-term carbohydrate-restricted diets [46, 47]. The long-term effects of these diets in the relationship between microbiota and health status need further investigations.
In conclusion, increasing daily fibre intake in the context of a healthy dietary pattern might be a valid tool to improve microbiota composition and activity to prevent metabolic diseases.
References
Makki K, Deehan EC, Walter J et al (2018) The impact of dietary fiber on gut microbiota in host health and disease. Cell Host Microbe 23:705–715. https://doi.org/10.1016/j.chom.2018.05.012
Ley RE, Bäckhed F, Turnbaugh P et al (2005) Obesity alters gut microbial ecology. PNAS 102(31):1070–11075. https://doi.org/10.1073/pnas.0504978102
Kreznar JH, Keller MP, Traeger LL et al (2017) Host genotype and gut microbiome modulate insulin secretion and diet-induced metabolic phenotypes. Cell Rep 18(7):1739–1750. https://doi.org/10.1016/j.celrep.2017.01.062
Federici M (2019) Gut microbiome and microbial metabolites a new system affecting metabolic disorders. J Endocrinol Invest 42(9):1011–1018. https://doi.org/10.1007/s40618-019-01022-9
Salgaço MK, Oliveira LGS, Costa GN et al (2019) Relationship between gut microbiota, probiotics, and type 2 diabetes mellitus. Appl Microbiol Biotechnol 103(23–24):9229–9238. https://doi.org/10.1007/s00253-019-10156-y
Kappel BA, Federici M (2019) Gut microbiome and cardiometabolic risk. Rev Endocr Metab Disord 20(4):399–406. https://doi.org/10.1007/s11154-019-09533-9
Abdul Rahim MBH, Chilloux J, Martinez-Gili L et al (2019) Diet induced metabolic changes of the human gut microbiome: importance of short-chain fatty acids, methylamines and indoles. Acta Diabetol. 56:493–500
Rothschild D, Weissbrod O, Barkan E et al (2018) Environment dominates over host genetics in shaping human gut microbiota. Nature 555:210–215. https://doi.org/10.1038/nature25973
Lynch SV, Pedersen O (2016) The human intestinal microbiome in health and disease. N Engl J Med 375(24):2369–2379. https://doi.org/10.1056/NEJMra1600266
Flint HJ, Scott KP, Louis P et al (2012) The role of the gut microbiota in nutrition and health. Nat Rev Gastroenterol Hepatol 9(10):577–589. https://doi.org/10.1038/nrgastro.2012.156
Zhang X, Shen D, Fang Z et al (2013) Human gut microbiota changes reveal the progression of glucose intolerance. PLoS ONE 8(8):e71108. https://doi.org/10.1371/journal.pone.0071108
Wu H, Tremaroli V, Schmidt C et al (2020) The gut microbiota in prediabetes and diabetes: a population-based cross-sectional study. Cell Metab. 32:379–390
Karlsson FH, Tremaroli V, Nookaew I et al (2013) Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature 498:99–103. https://doi.org/10.1038/nature12198
Qin J, Li Y, Cai Z et al (2012) A metagenome-wide association study of gut microbiota in type 2 diabetes. Nature 490:55–60. https://doi.org/10.1038/nature11450
Sanna S, van Zuydam NR, Mahajan A et al (2019) Causal relationships among the gut microbiome, short-chain fatty acids and metabolic diseases. Nat Genet 51:600–605. https://doi.org/10.1038/s41588-019-0350-x
De Filippo C, Cavalieri D, Di Paola M et al (2010) Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa. Proc Natl Acad Sci USA 107:14691–14696. https://doi.org/10.1073/pnas.1005963107
Garcia-Mantrana I, Selma-Royo M, Alcantara C et al (2018) Shifts on gut microbiota associated to mediterranean diet adherence and specific dietary intakes on general adult population. Front Microbiol 9:890. https://doi.org/10.3389/fmicb.2018.00890
Gutiérrez-Díaz I, Fernández-Navarro T, Sánchez B et al (2016) Mediterranean diet and faecal microbiota: a transversal study. Food Funct 7:2347–2356. https://doi.org/10.1039/C6FO00105J
Mitsou EK, Kakali A, Antonopoulou S et al (2017) Adherence to the Mediterranean diet is associated with the gut microbiota pattern and gastrointestinal characteristics in an adult population. Br J Nutr 117:1645–1655. https://doi.org/10.1017/S0007114517001593
De Filippis F, Pellegrini N, Vannini L et al (2016) High-level adherence to a Mediterranean diet beneficially impacts the gut microbiota and associated metabolome. Gut 65:1812–1821. https://doi.org/10.1136/gutjnl-2015-309957
David LA, Maurice CF, Carmody RN et al (2014) Diet rapidly and reproducibly alters the human gut microbiome. Nature 505:559–563. https://doi.org/10.1038/nature12820
Vitale M, Giacco R, Laiola M et al (2020) Acute and chronic improvement in postprandial glucose metabolism by a diet resembling the traditional Mediterranean dietary pattern: can SCFAs play a role? Clin Nutr S0261–5614(20):30260. https://doi.org/10.1016/j.clnu.2020.05.025
Zhao L, Zhang F, Ding X et al (2018) Gut bacteria selectively promoted by dietary fibers alleviate type 2 diabetes. Science 359:1151–1156. https://doi.org/10.1126/science.aao5774
Haro C, Montes-Borrego M, Rangel-Zúñiga OA et al (2016) Two healthy diets modulate gut microbial community improving insulin sensitivity in a human obese population. J Clin Endocrinol Metab 101:233–242. https://doi.org/10.1210/jc.2015-3351
Hald S, Schioldan AG, Moore ME et al (2016) Effects of arabinoxylan and resistant starch on intestinal microbiota and short-chain fatty acids in subjects with metabolic syndrome: a randomised crossover study. PLoS ONE 11(7):e0159223. https://doi.org/10.1371/journal.pone.0159223.eCollection
Vetrani C, Costabile G, Luongo D et al (2016) Effects of whole-grain cereal foods on plasma short chain fatty acid concentrations in individuals with the metabolic syndrome. Nutrition 32:217–221. https://doi.org/10.1016/j.nut.2015.08.006
Kovatcheva-Datchary P, Nilsson A, Akrami R et al (2015) Dietary fiber-induced improvement in glucose metabolism is associated with increased abundance of prevotella. Cell Metab 22:971–982. https://doi.org/10.1016/j.cmet.2015.10.001
Nilsson AC, Johansson-Boll EV, Björck IM (2015) Increased gut hormones and insulin sensitivity index following a 3-d intervention with a barley kernel-based product: a randomised cross-over study in healthy middle-aged subjects. Br J Nutr 114:899–907. https://doi.org/10.1017/S0007114515002524
Bozzetto L, Costabile G, Della Pepa G et al (2018) Dietary fibre as a unifying remedy for the whole spectrum of obesity-associated cardiovascular risk. Nutrients 10:943. https://doi.org/10.3390/nu10070943
Canfora EE, Jocken JW, Blaak EE (2015) Short-chain fatty acids in control of body weight and insulin sensitivity. Nat Rev Endocrinol 11:577–591. https://doi.org/10.1038/nrendo.2015.128
Fushimi T, Tayama K, Fukaya M et al (2001) Acetic acid feeding enhances glycogen repletion in liver and skeletal muscle of rats. J Nutr J 13:1973–1977. https://doi.org/10.1093/jn/131.7.1973
Li H, Gao Z, Zhang J et al (2012) Sodium butyrate stimulates expression of fibroblast growth factor 21 in liver by inhibition of histone deacetylase 3. Diabetes 61(4):797–806. https://doi.org/10.2337/db11-0846
Li X, Chen H, Guan Y et al (2013) Acetic acid activates the AMP-activated protein kinase signaling pathway to regulate lipid metabolism in bovine hepatocytes. PLoS ONE 8:e67880. https://doi.org/10.1371/journal.pone.0067880
He J, Zhang P, Shen L et al (2020) Short-chain fatty acids and their association with signalling pathways in inflammation, glucose and lipid metabolism. Int J Mol Sci 21:6356. https://doi.org/10.3390/ijms21176356
Gao Z, Yin J, Zhang J et al (2009) Butyrate improves insulin sensitivity and increases energy expenditure in mice. Diabetes 58:1509–1517. https://doi.org/10.2337/db08-1637
Yamashita H, Maruta H, Jozuka M et al (2009) Effects of acetate on lipid metabolism in muscles and adipose tissues of type 2 diabetic Otsuka Long-Evans Tokushima Fatty (OLETF) rats. Biosci Biotechnol Biochem 73:570–6. https://doi.org/10.1271/bbb.80634
Yamashita H (2016) Biological function of acetic acid-improvement in obesity and glucose tolerance by acetic acid in type 2 diabetic rats. Crit Rev Food Sci Nutr 56:S171–S175. https://doi.org/10.1080/10408398.2015.1045966
Chambers ES, Viardot A, Psichas A et al (2015) Effects of targeted delivery of propionate to the human colon on appetite regulation, body weight maintenance and adiposity in overweight adults. Gut 64:1744–1754. https://doi.org/10.1136/gutjnl-2014-307913
Byrne CS, Chambers ES, Preston T et al (2019) Effects of inulin propionate ester incorporated into palatable food products on appetite and resting energy expenditure: a randomised crossover study. Nutrients 11:861. https://doi.org/10.3390/nu11040861
Bouter K, Bakker GJ, Levin E et al (2018) Differential metabolic effects of oral butyrate treatment in lean versus metabolic syndrome subjects. Clin Transl Gastroenterol 9:155. https://doi.org/10.1038/s41424-018-0025-4
Bui TPN, de Vos WM (2021) Next-generation therapeutic bacteria for treatment of obesity, diabetes, and other endocrine diseases. Best Pract Res Clin Endocrinol Metab 17:101504. https://doi.org/10.1016/j.beem.2021.101504
Hosseini E, Grootaert C, Verstraete W, Van de Wiele T (2011) Propionate as a health-promoting microbial metabolite in the human gut. Nutr Rev 69:245–258. https://doi.org/10.1111/j.1753-4887.2011.00388.x
Fu X, Liu Z, Zhu C, Mou H, Kong Q (2019) Nondigestible carbohydrates, butyrate, and butyrate-producing bacteria. Crit Rev Food Sci Nutr 59:130–152. https://doi.org/10.1080/10408398.2018.1542587
Reynolds AN, Akerman AP, Mann J (2020) Dietary fibre and whole grains in diabetes management: systematic review and meta-analyses. PLoS Med 17:e1003053. https://doi.org/10.1371/journal.pmed.1003053
Barber TM, Kabisch S, Pfeiffer AFH, Weickert MO (2020) The health benefits of dietary fibre. Nutrients 12:3209. https://doi.org/10.3390/nu12103209
Mardinoglu A, Wu H, Bjornson E et al (2018) An integrated understanding of the rapid metabolic benefits of a carbohydrate-restricted diet on hepatic steatosis in humans. Cell Metab 27:559–571. https://doi.org/10.1016/j.cmet.2018.01.005
Ang QY, Alexander M, Newman JC et al (2020) Ketogenic diets alter the gut microbiome resulting in decreased intestinal Th17 cells. Cell 181:1263–1275. https://doi.org/10.1016/j.cell.2020.04.027
Funding
Open access funding provided by Università degli Studi di Napoli Federico II within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Managed by Massimo Federici .
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Salamone, D., Rivellese, A.A. & Vetrani, C. The relationship between gut microbiota, short-chain fatty acids and type 2 diabetes mellitus: the possible role of dietary fibre. Acta Diabetol 58, 1131–1138 (2021). https://doi.org/10.1007/s00592-021-01727-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-021-01727-5