Abstract
Purpose
Total hip arthroplasty (THA) is commonly used worldwide in pelvic osteoarthritis treatment. This surgery can change the spinopelvic parameters, which in turn affects the performance of the patients after surgery. However, the relationship between functional disability following THA and spinopelvic alignment is not completely understood. The limited available studies have also been conducted on the population with spinopelvic malalignments. This study aimed to examine the changes in spinopelvic parameters after primary THA in patients with normal preoperative spinopelvic characteristics and the association of these parameters with the performance, gender, and age of the patients after THA.
Methods
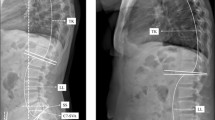
Fifty-eight eligible patients with unilateral primary hip osteoarthritis (HOA) scheduled for total hip arthroplasty between February and September 2021 were studied. Spinopelvic parameters including pelvic incidence (PI), sacral slope (SS), and pelvic tilt (PT) were measured before surgery and three months after surgery, and the relationship between these parameters and patients' performance (Harris hip score) was assessed. Also, the relationship between the age and gender of the patients with these parameters was evaluated.
Results
The mean age of study participants was 46.03 ± 14.25. Three months after THA, sacral slope decreased with the mean difference of 4.31 ± 10.26 degrees (p = 0.002) and Harris hip score (HHS) increased by 19.41 ± 26.55 points (p < 0.001). With increasing age in patients, the mean SS and PT decreased. Among the spinopelvic parameters, SS (β = 0.11) had a greater effect than PT on postoperative HHS changes and among the demographic parameters, age (β = −0.18) had a greater effect on HHS changes than gender.
Conclusion
Spinopelvic parameters are associated with age, gender, and patient's function after THA as sacral slope decreased and HHS increased after THA, and aging is accompanied by lowering of PT and SS.

Similar content being viewed by others
Availability of data and materials
The data of this study is available, but it will be sent to the requester privately, not publicly.
References
Innmann MM, Verhaegen JCF, Reichel F, Schaper B, Merle C, Grammatopoulos G (2022) Spinopelvic characteristics normalize 1 year after total hip arthroplasty: a prospective, longitudinal, case-controlled study. J Bone Joint Surg Am 104(8):675–683. https://doi.org/10.2106/jbjs.21.01127
Sousa VdC, Perini JA, Araújo Junior AEP, Guimarães JAM, Duarte MEL, Fernandes MBC (2020) Evaluation of the radiographic parameters of sagittal and spinopelvic alignment in patients with osteoarthritis submitted to total hip arthroplasty. Revista Brasileira de Ortopedia 55:591–596
Fu M, Zhou H, Li Y, Jin H, Liu X (2022) Global, regional, and national burdens of hip osteoarthritis from 1990 to 2019: estimates from the 2019 Global Burden of Disease Study. Arthritis Res Ther 24(1):1–11
Migliorini F, Trivellas A, Eschweiler J, Driessen A, Lessi F, Tingart M, Aretini P (2021) Nerve palsy, dislocation and revision rate among the approaches for total hip arthroplasty: a Bayesian network meta-analysis. Musculoskelet Surg 105(1):1–15
Sharma M, Behera P, Sen RK, Aggarwal S, Tripathy SK, Prakash M, Saini G, Saibaba B (2019) Total hip arthroplasty for arthritis following acetabular fractures—evaluation of radiological, functional and quality of life parameters. J Clin Orthop Trauma 10(1):131–137
Heckmann N, McKnight B, Stefl M, Trasolini NA, Ike H, Dorr LD (2018) Late dislocation following total hip arthroplasty: spinopelvic imbalance as a causative factor. JBJS 100(21):1845–1853
Okamoto Y, Wakama H, Okayoshi T, Matsuyama J, Otsuki S, Neo M (2022) Spinopelvic mismatch is associated with patient-reported outcome measures after total knee arthroplasty at a mean follow-up of 15 years. Knee 34:156–166. https://doi.org/10.1016/j.knee.2021.11.017
Zagra L, Benazzo F, Dallari D, Falez F, Solarino G, D’Apolito R, Castelli CC (2022) Current concepts in hip–spine relationships: making them practical for total hip arthroplasty. EFORT Open Rev 7(1):59–69
Bassani R, Querenghi A, Giacalone A, Brambilla L, Peretti G (2020) Modifications of spinopelvic parameters and acetabular orientation after spinal surgery for adult deformity in patient who underwent bilateral total hip arthroplasty. In: Congress of the Italian Orthopaedic Research Society 2019 Guest Editors: F. Castoldi, GM Peretti, A. Marmotti, L. Mangiavini, 2020. vol 4 Supplement 3, p 15
Homma Y, Ishii S, Yanagisawa N, Ochi H, Baba T, Nojiri H, Okuda T, Kaneko K (2020) Pelvic mobility before and after total hip arthroplasty. Int Orthop 44(11):2267–2274
van der Gronde B, Schlösser TPC, van Erp JHJ, Snijders TE, Castelein RM, Weinans H, de Gast A (2022) Current evidence for spinopelvic characteristics influencing total hip arthroplasty dislocation risk. JBJS Rev. https://doi.org/10.2106/jbjs.Rvw.22.00038
Sultan AA, Khlopas A, Piuzzi NS, Chughtai M, Sodhi N, Mont MA (2018) The impact of spino-pelvic alignment on total hip arthroplasty outcomes: a critical analysis of current evidence. J Arthroplast 33(5):1606–1616
Deckey DG, Rosenow CS, Lai C, Christopher ZK, Verhey JT, Schwartz AJ, Bingham JS (2022) Abnormal spinopelvic motion and spine deformity are associated with native femoral retroversion in the setting of total hip arthroplasty. Arthroplast Today 17:150–154. https://doi.org/10.1016/j.artd.2022.08.005
Sculco PK, Windsor EN, Jerabek SA, Mayman DJ, Elbuluk A, Buckland AJ, Vigdorchik JM (2021) Preoperative spinopelvic hypermobility resolves following total hip arthroplasty. Bone Joint J 103(12):1766–1773
Windsor EN, Sculco PK, Mayman DJ, Vigdorchik JM, Jerabek SA (2022) Spinopelvic hypermobility corrects after staged bilateral total hip arthroplasty. HSS J 18(4):541–549. https://doi.org/10.1177/15563316211050353
Okamoto Y, Wakama H, Okayoshi T, Otsuki S, Neo M (2021) Association of global sagittal spinal deformity with functional disability two years after total hip arthroplasty. BMC Musculoskelet Disord 22(1):1–10
Ochi H, Homma Y, Baba T, Nojiri H, Matsumoto M, Kaneko K (2017) Sagittal spinopelvic alignment predicts hip function after total hip arthroplasty. Gait Posture 52:293–300. https://doi.org/10.1016/j.gaitpost.2016.12.010
Nilsdotter A, Bremander A (2011) Measures of hip function and symptoms: Harris hip score (HHS), hip disability and osteoarthritis outcome score (HOOS), Oxford hip score (OHS), Lequesne index of severity for osteoarthritis of the hip (LISOH), and American Academy of orthopedic surgeons (AAOS) hip and knee questionnaire. Arthritis Care Res 63(S11):S200–S207
Piazzolla A, Solarino G, Bizzoca D, Montemurro V, Berjano P, Lamartina C, Martini C, Moretti B (2018) Spinopelvic parameter changes and low back pain improvement due to femoral neck anteversion in patients with severe unilateral primary hip osteoarthritis undergoing total hip replacement. Eur Spine J 27(1):125–134
Ben-Galim P, Ben-Galim T, Rand N, Haim A, Hipp J, Dekel S, Floman Y (2007) Hip-spine syndrome: the effect of total hip replacement surgery on low back pain in severe osteoarthritis of the hip. Spine 32(19):2099–2102
Eyvazov K, Eyvazov B, Basar S, Nasto LA, Kanatli U (2016) Effects of total hip arthroplasty on spinal sagittal alignment and static balance: a prospective study on 28 patients. Eur Spine J 25(11):3615–3621
Weng W-J, Wang W-J, Wu M-D, Xu Z-H, Xu L-L, Qiu Y (2015) Characteristics of sagittal spine–pelvis–leg alignment in patients with severe hip osteoarthritis. Eur Spine J 24(6):1228–1236
Tateuchi H (2019) Gait-and postural-alignment-related prognostic factors for hip and knee osteoarthritis: toward the prevention of osteoarthritis progression. Phys Ther Res 22(1):31–37
Yoshimoto H, Sato S, Masuda T, Kanno T, Shundo M, Hyakumachi T, Yanagibashi Y (2005) Spinopelvic alignment in patients with osteoarthrosis of the hip: a radiographic comparison to patients with low back pain. Spine 30(14):1650–1657
Kim Y, Pour AE, Lazennec JY (2020) How do global sagittal alignment and posture change after total hip arthroplasty? Int Orthop 44(2):267–273
Loeser RF (2010) Age-related changes in the musculoskeletal system and the development of osteoarthritis. Clin Geriatr Med 26(3):371–386
Franceschi C, Garagnani P, Morsiani C, Conte M, Santoro A, Grignolio A, Monti D, Capri M, Salvioli S (2018) The continuum of aging and age-related diseases: common mechanisms but different rates. Front Med 61
Ishihara Y, Morishita M, Kanzaki K, Toyone T (2020) Age-related progression of degenerative lumbar kyphoscoliosis: a retrospective study. Spine Surg Relat Res 2019-0113
Yukawa Y, Kato F, Suda K, Yamagata M, Ueta T, Yoshida M (2018) Normative data for parameters of sagittal spinal alignment in healthy subjects: an analysis of gender specific differences and changes with aging in 626 asymptomatic individuals. Eur Spine J 27(2):426–432
Merrill RK, Kim JS, Leven DM, Kim JH, Meaike JJ, Bronheim RS, Suchman KI, Nowacki D, Gidumal SS, Cho SK (2018) Differences in fundamental sagittal pelvic parameters based on age, sex, and race. Clin Spine Surg 31(2):E109–E114
MavČiČ B, Pompe B, Antolič V, Daniel M, Iglič A, Kralj-Iglič V (2002) Mathematical estimation of stress distribution in normal and dysplastic human hips. J Orthop Res 20(5):1025–1030
Mavčič B, Iglič A, Kralj-Iglič V, Brand RA, Vengust R (2008) Cumulative hip contact stress predicts osteoarthritis in DDH. Clin Orthop Relat Res 466:884–891
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Mohamad Qoreishy: Study design, data collection, manuscript preparation; Bahram Naghibi: Study design, data collection and analyses, primary manuscript preparation; Sohrab Keyhani: Data collection, manuscript revision; Mohammad Movahedinia: Methodology design, manuscript revision, study design; Bentolhoda Salehi: Manuscript revision, Study design; Mitra Goodarzi: Manuscript revision, Study design; All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical Approval
The study protocol was reviewed and approved by the local Ethics Committee.
Consent to participate
Written informed consent was obtained from all patients before initiation of the study.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Qoreishy, M., Movahedinia, M., Keyhani, S. et al. Evaluation of changes in radiographic spinopelvic parameters after primary total hip arthroplasty and its relationship with short-term patient function. Eur J Orthop Surg Traumatol 34, 225–230 (2024). https://doi.org/10.1007/s00590-023-03639-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-023-03639-2