Abstract
Purpose
Spinal decompression surgery causes severe pain. Retrolaminar block (RLB) is block, which is done by infiltration of local anesthetic to block spinal nerves between the lamina and superior costotransversospinalis muscle. The primary aim of this study is to evaluate the effectiveness of RLB on postoperative analgesia in patients undergoing spinal surgery. Secondary aims are effects on additional anesthetic and analgesic consumption.
Methods
The sixty (60) patients who underwent lumbar spinal surgery between May 2020 and May 2021 under general anesthesia with or without applied preemptive RLB for postoperative analgesia were included in this prospective observational study. Group I received ultrasound-guided preemptive RLB. In Group II, no intervention was performed. Postoperative VAS scores were compared in groups as primary outcome, perioperative additional anesthetic and analgesic needs were compared as secondary outcome.
Results
There was a significant difference between the groups in favor of the RLB group in terms of postoperative VAS scores at rest [1.33 (0.33–3.509)] and movement [2.40 (1.20–4.00)] (p < 0.001). Perioperative sevoflurane consumption was significantly low in block group (p < 0.001). Postoperative tramadol consumption was lower in Group I compared with Group II [Group 1: 200 (100–300); Group 2: 37.5 (0–200); p < 0.001].
Conclusion
Preemptive RLB may be used to reduce patients' pain in lumbar decompression surgery as well as to be part of a multimodal analgesia and anesthesia regimen to reduce anesthetic and analgesic drug consumption.
Trial registration numberClinicalTrials.gov (No. NCT04209907).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Poorly controlled postoperative pain after spinal surgery may lead to increased morbidity as pulmonary and deep venous thrombosis, prolonged duration of hospital stay, increased opioid use, increased health-care expenditures and development of chronic pain [1]. Opioids are frequently used for postoperative spinal pain [2]. In order to reduce the side effects that may occur due to opioids (such as nausea, vomiting, respiratory depression), multiple methods are preferred instead of a single drug [3]. In recent years, the combination of nerve blocks with local anesthetics and non-steroidal anti-inflammatory drugs as multimodal analgesia is especially effective for patients for postoperative pain. They are also very effective in reducing the side effects that may occur due to opioids since the opioid sparing effect. Plane blocks are interventions that have started to be widely used for analgesic purposes with the widespread use of ultrasound. Retrolaminar block (RLB) is a new application called the paravertebral lamina technique, which was first performed by Pfeiffer for analgesia in a blind mastectomy patient [4]. On the other hand, successful analgesia in a patient with a rib fracture by touching the lamina with a needle under ultrasound guidance was provided in 2013 [5]. In this way, analgesia is performed by blocking the paraspinal nerves with a local anesthetic drug that spreads between the deep paraspinal muscles and the vertebral lamina [6]. Although there have been many studies on lung surgery, video-assisted thoracoscopic surgery and laparoscopic nephrectomy that have investigated the postoperative analgesic efficacy [7,8,9], there is no previously published prospective study about the analgesic effect of RLB in lumbar decompression surgery. This is the first prospective study with large participant related to pain reduced effect of RLB for lumbar decompression surgery with opioid sparing effect. Furthermore this is the first study that analysed the effect of RLB on perioperative inhaled anesthetic consumption. The aim of the present study is to investigate the effect of the preemptive RLB on postoperative pain scores, perioperative analgesic and anesthetic consumptions in lumbar decompression surgery.
Materials and methods
This prospective observational study was approved by lokal ethics committee and Turkey Drug and Medical Device Agency ( number: 66175679–514.05.03-E.50796; subject: 19-AKD-156). Written informed consent was obtained from all patients. This study is registered with ClinicalTrials.gov (NCT04209907).
Patients
Sixty patients (60) with American Society of Anesthesiologists (ASA) classification I-III, aged 18–75 years, who underwent for level 1 or 2 open lumbar decompression surgery in a university hospital between the dates of May 2020 and May 2021 in accordance with the Helsinki Declaration were included in the study.
Patients with severe liver, kidney, heart and hematological diseases, with infection, obese, with coagulation disorders, with infection at the intervention site, with severe central or peripheral neurologic disease, with a history of allergic reaction to drugs used during surgical duration, with psychological disorders, with a history of preoperative chronic opioid use, with alcohol and drug addiction were excluded from the study.
Sample size calculation and grouping
The sample size was calculated wıth G power software (G*Power 3.1.9.3) using the VAS score results obtained from the previous study [10]. Accordıng to the result of thıs study, wıth 80% power, a two-way alpha error of 0.05 and 1:1 allocation ratio, ıt was suffıcıent to take at least 28 number of patıents ın each group to detect the dıfference. Taking into account the possibility of a 10% case being excluded from the study, 30 patients for each group were included in the study. Groups were randomized 1:1 using the closed opaque envelope technique and assigned randomly. The patients were divided into groups according to whether or not the block was performed; RLB group and non-RLB group.
RLB block technique
All patients who underwent block intervention were taken to a separate regional anesthesia room, where we performed block applications half an hour before the operation. Pulse oximetry, noninvasive arterial blood pressure and electrocardiogram observation were applied to the patients as standard monitoring methods and patients were placed in the prone position. Midazolam (0.02 mg/kg) (demizolam 5 mg/ml, Pharmada Drugs, Istanbul) was administered intravenously to the patients for preoperative sedation. The intervention area was sterilized with povidone iodine before the procedure, covered by sterile drapes and a sterile sheath was applied to the ultrasound. The 1–7 MHz convex array ultrasound probe (Esaote My Lab 6 US Machine, Florance, Italy) was placed sagittally in the midline at the level of the lumbar decompression area (Lumbar 1–2-3–4 level) by experienced anesthesiologist resident. After the spinous processes were seen, the ultrasound probe was moved laterally 1–2 cm and vertebral laminae were observed. A 22 G 100 mm needle (B. Braun, Germany) was inserted from cranial to caudal direction with in plane technique. When the needle touch the lamina (Fig. 1), 2 ml saline was injected for confrmation of the location. After the location was confirmed, a 20 ml % 0.25 bupivacain was administered with low pressure (Fig. 2). The same intervention was performed on the other side of the vertebra lamina. After 20 min of sensory examination and evaluation of efficacy, the patients were transfered to the operating room. No intervention was applied to the other group of the study.
Anesthesia technique
Standard monitoring (peripheral oxygen saturation [sPO2], heart rate [HR], noninvasive mean blood pressure [MBP]) and standard general anesthesia (2 mg/kg propofol [Propofol, Fresenius Kabi, Melsungen, Germany] i.v., 1.5–2 mg/kg fentanyl [Fentanyl Citrate, Hospira, Lake Forest, Illinois, USA] and 0.6 mg/kg rocuronium [Esmeron, Organon, Kloosterstraat, the Netherlands] i.v.) was applied to all patients. After trakeal intübation, anesthesia was maintained with 1–2% sevoflurane (Sevorane, Abbott, Chicago, Illinois, USA) in 50% air and 50% O2 in 4L fresh gas flow, and if necessary 0.25–1 mcg/kg/minute remifentanil. The bispecteral index (BİS, A-2000, Aspect medical Systems) was kept between 40 and 50 values by changing the concentration of sevoflurane. The hemodynamic control was achived by administering or changing remifentanyl. Muscle relaxation was controlled by the train-of-four (TOF) and 0.2 mg/kg rocuronium was added when needed. Minumum alveolar concentration (MAC) values of sevoflurane, characteristics of anesthesia and surgery, total consumption of sevoflurane and remifentanyl were recorded during the procedure. Thirty minutes before the end of the surgery, for postoperative analgesia, 1 g paracetamol and dexketoprofen trometamol 50 mg i.v. was administered to all patients. After the end of the surgery, 2.5 mg neostigmine and 0.02 mg/kg atropine was administered and the patients were extubated. Then all patients were observed at postoperative recovery unit and they transfered to the wards after the 9 and more Aldrete scores were seen.
Pain assessment
Postoperative pain was evaluated by a researcher who was blinded to group allocation by using visual analog scale (VAS) indicating the pain severity (0–3; no to mild pain, 4–7; moderate pain, 8–10; severe pain) at 1st, 2nd, 4th, 6th, 12th and 24th hours of postoperative period at rest and with active movement by a blinded researcher to the study groups. If the VAS score of the patients was 4 or more, 1 mg/kg tramadol was administered. First analgesic requirement time and total analgesic consumption were also recorded.
Statistical analysis
Statistical analysis was performed by using package programme (SPSS) of version 20.0 (IBM Corporation, Armonk, NY). Kolmogorov–Smirnov test was used for the normality distribution analysis of variables. According to the distribution variables were presented as mean ± standard deviation (for parametric variables) and median [(min–max) for nonparametric variables]. Categorical variables were expressed as number and percentage. The analysis of the parametric data was made by independent t-test and nonparametric data was made by Mann–Whitney U test. p < 0.05 value was considered statistically significant.
Results
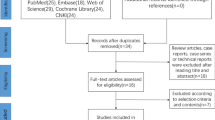
Sixty patients were enrolled in this study. Flow diagram of the patients is shown in Table 1. Characteristics of patients and surgery are presented in Table 2. There was not any significant difference between the 2 groups in terms of age, weight, height, sex, ASA status, duration of surgery, duration of anesthesia (P > 0.05). Perioperative hemodynamic parameters (MBP and HR) were similar between groups (P > 0.05). However MAC values were different in favor RLB group (lower than non-RLB, p < 0.001) (Table 3). Total sevoflurane and remifentanil consumption during operation was significantly lower in RLB group (p < 0.001and p = 0.01 respectively) (Table 3). Tramadol and paracetamol consumption was significantly lower in the RLB group compared with the non-RLB group at postoperative period (p < 0.001 and p = 0.01 respectively) (Table 3). However total dexketoprofen consumption were not different (P = 0.73). The first analgesic requirement time was significantly longer in the RLB Group than in the non-RLB Group [(2 (1–3) hour and 4 (2–12) hour respectively, P < 0.001)] (Table 3). Postoperative VAS scores were assessed at rest and with active movement. Scores were significantly lower in the RLB Group than in the non-RLB Group at all time intervals (P < 0.001) (Table 4, Fig. 3). There was not any complication in both groups.
Discussion
In the present study, we found that pain scores were lower in RLB block group compared with the non-block group and application of RLB block reduced perioperative analgesic and anesthetic consumption in patients underwent lumbar decompression surgery.
Lumbar decompression surgery is frequently performed in patients to relieve low back pain, reduce radiculopathy, and improve overall function. Inadequate pain management in the postoperative period may lead to delayed discharge or rehospitalization after surgery [11, 12]. At the same time, effective pain control increases postoperative results and patient satisfaction. Multimodal analgesia is a recommended practice to accelerate postoperative recovery [13]. The specific treatment of each procedure is important. Regional anesthesia techniques have increasingly become a part of multimodal analgesia in recent years. Thus, initiatives to reduce opioid consumption and its associated adverse effects in the postoperative period are supported [14]. At this point, different interventional methods can be applied [15,16,17]. The retrolaminar block we used in our study is one of these interventions.
Actually, RLB is a type of modified paravertebral block like other paravertebral fascial plane blocks. However, in RLB, as in classical paravertebral blocks, the target of the needle is not the paravertebral space. The needle targets the retrolaminar area closer to the midline, more medially [18]. Therefore, the risk of pleural damage is lower in terms of anatomy and needle placement compared to erector spinae plane block [15]. Again, from an anatomical point of view, besides its analgesic effectiveness, it can be said that it is easier to see the lamina with the help of ultrasound compared to thoracolumbar interfascial plane block (TLIP) and modified TLIP block [16, 17]. Because the acoustic window between the transverse processes is a narrow area, observing the paravertebral anatomy (muscle structure and fascial spaces) and inserting the needle is more difficult in other paravertebral area blocks [19].
The clinical effect is presumed to occur in RLB as the local anesthetic diffuses into the paravertebral space, epidural space, or intervertebral foramen via the superior costotransverse ligament [20]. In addition, in the cadaver study, the spread of local anesthetic given via the superior costotransverse ligament was also observed [21]. It was also stated that this spread changed with the amount of local anesthetic given. However, it was emphasized that compared to other paravertebral blocks, 20 ml solutions may accumulate more in RLB, especially in the posterior area, and affect the posterior muscle structures more [22, 23]. The analgesic efficacy of RLB in patients, especially in spinal surgical interventions, as in the present study, can be explained in this way.
We see that the amount of perioperative analgesics and anesthetics decreased in the RLB applied patient group. In our study, we have seen the opioid sparing effect, which has been on the agenda in recent years, especially in order to avoid side effects related to opioids [24]. In order to reduce opioid use, regional anesthesia methods are very important as a part of multimodal analgesia in spinal surgery [25]. In this study, we observed that there was less perioperative opioid consumption in the block group. Therefore, combination therapy or multimodal treatment for control of pain seems as the best approach in this regard. Again, we observed that the amount of inhalation anesthetic consumed in the group that underwent block during the intraoperative period was less. In this context, our study also supported the idea that the analgesic efficacy of regional anesthesia is a part of multimodal anesthesia [26]. The majority of the anesthetic agent used in a patient receiving inhalation anesthesia goes to the waste gas system and the atmosphere. Therefore, with the results of our study, another issue that may be useful in clinical practice will be discussed. Thus, the low amount of sevoflurane we use is important both economically and in terms of environmental pollution. By using less inhalation anesthetic, less damage to the atmosphere is provided, thus contributing to sustainable anesthesia [27]. Improved and ongoing awareness of practitioners regarding the climate impact of inhaled anesthetics is essential to bring change to routine practice [27]. In addition, inhaled anesthetics constitute a significant part of the costs of administering anesthesia to the patient. The cost of anesthesia for any surgical procedure depends on the type of anesthetic used and the volatile anesthetic concentration in the targeted patient. Different experiences with cost savings have already been reported [28]. Applying the regional anesthesia method as part of multimodal anesthesia, as in the present study, would be a cost-effective practical clinical approach.
Considering the clarity of the sonographic image, post-surgical anatomical changes would not give us a clear image. Therefore, in our study, we applied RLB in the preoperative period. Observation of at least 5 levels of spread of the given solution (20 ml) in the anatomical cadaver study [22] made us think that the analgesic efficacy will be at the entire lumbar level (L1-5) in the block procedure we performed at the level of lumbar 3 vertebra.
No complications were observed in any of our patients in our study. Retrolaminar block is ultimately a paravertebral block. Therefore, the risk of pneumothorax cannot be ignored. However, considering all paravertebral blocks, the least risk is with retrolaminar block. Because it is the PVB type performed anatomically furthest from the pleura. In addition, when the needle is entered 1–1.5 cm lateral to the spinous process with USG, it directly contacts the lamina. So it is easy to apply. The risk of hematoma or nerve damage may be considered during retrolaminar block application. However, there are no major vessels or nerves in the location of the needle. The possible risk may be in the form of intramuscular hematoma, which is not clinically significant. At the same time, as in all regional anesthesia applications, the retrolaminar block procedure is not performed or performed with appropriate procedures for patients receiving anticoagulation within the framework of the regional anesthesia and pain medicine evidence-based guidelines [29]. There may also be a risk of systemic toxicity due to local anesthetics used during retrolaminar block. However, as long as the dose of local anesthetic used does not exceed the systemic toxicity limit, it will not pose a problem. Considering the effect mechanism of retrolaminar block, it is reported that it also has epidural spread (20). Therefore, there will be epidural spread of the local anesthetic we use. This may present as motor weakness in the postoperative period. However, considering the width of the epidural space and the low dose of medication used, it may be a very rare situation. In such a case, low drug concentration will not affect hemodynamics. In addition, the effect of the drug on muscle strength will end until the patient is mobilized in the postoperative period.
There were some limitations in our study. First of all, we could not show exactly how many levels of local anesthetic that we gave was spread under ultrasound due to technical reasons. Although we perform dermatomal sensory examination, showing this spread would be a guide in future studies. Secondly, we did not follow the pain levels of the patients in the preoperative period. At the same time, we did not evaluate the psychological state of the patients. Factors such as these can affect patients' post-operative pain. Therefore, it can be considered as a limitation. In addition, the block operation we apply is a fairly new method. For this reason, it would be more appropriate to work with a larger sample number in order to observe the complications that may occur and to fully reflect the population. Many future studies are needed.
References
Gan TJ (2017) Poorly controlled postoperative pain: prevalence, consequences, and prevention. J Pain Res 10:2287–2298. https://doi.org/10.2147/JPR.S144066
Bajwa SJ, Haldar R (2015) Pain management following spinal surgeries: An appraisal of the available options. J Craniovertebr Junction Spine 6(3):105–110. https://doi.org/10.4103/0974-8237.161589
Jogie J, Jogie JA (2023) A comprehensive review on the efficacy of nerve blocks in reducing postoperative anesthetic and analgesic requirements. Cureus 15(5):e38552. https://doi.org/10.7759/cureus.38552
Juttner T, Werdehausen R, Hermanns H, Monaca E, Danzeisen O et al (2011) The paravertebral lamina technique: a new regional anesthesia approach for breast surgery. J Clin Anesth 23:443–450. https://doi.org/10.1016/j.jclinane.2010.12.015
Zeballos JL, Voscopoulos C, Kapottos M, Janfaza D, Vlassakov K (2013) Ultrasound-guided retrolaminar paravertebral block. Anaesthesia 68:649–651. https://doi.org/10.1111/anae.12296
Yang HM, Choi YJ, Kwon HJ, Cho TH, Kim SH (2018) Comparison of injectate spread and nerve involvement between retrolaminar and erector spinae plane blocks in the thoracic region: a cadaveric study. Anaesthesia 73(10):1244–1250
Sugiyama T, Kataoka Y, Shindo K, Hino M, Itoi K et al (2021) Retrolaminar block versus paravertebral block for pain relief after less-invasive lung surgery: a randomized, non-inferiority controlled trial. Cureus 13(2):e13597. https://doi.org/10.7759/cureus.13597
Wang Q, Wei S, Li S, Yu J, Zhang G et al (2021) Comparison of the analgesic effect of ultrasound-guided paravertebral block and ultrasound-guided retrolaminar block in Uniportal video-assisted Thoracoscopic surgery: a prospective, randomized study. BMC Cancer 21(1):1229. https://doi.org/10.1186/s12885-021-08938-7
Liu D, Xu X, Zhu Y, Liu X, Zhao F et al (2021) Safety and efficacy of ultrasound-guided retrolaminar block of multiple injections in retroperitoneal laparoscopic nephrectomy: a prospective randomized controlled study. J Pain Res 5(14):333–342. https://doi.org/10.2147/JPR.S282500
Şahin A, Baran O, Gültekin A, Şahin G, Arar C (2021) Ultrasound-guided erector spinae plane block for lumbar spinal stenosis surgery. Open J Anesthesiol 11:72–84. https://doi.org/10.4236/ojanes.2021.113008
Elsharydah A, Duncan KL, Rosero EB, Minhajuddin A, Somasundaram A, Joshi GP (2021) Readmission rate after 2-level lumbar decompression: a propensity-matched cohort study comparing inpatient and outpatient settings. Clin Spine Surg. https://doi.org/10.1097/BSD.0000000000000990
Mundell BF, Gates MJ, Kerezoudis P, Alvi MA, Freedman BA, Nassr A, Hohmann SF, Bydon M (2018) Does patient selection account for the perceived cost savings in outpatient spine surgery? A meta-analysis of current evidence and analysis from an administrative database. J Neurosurg Spine 29(6):687–695. https://doi.org/10.3171/2018.4.SPINE1864
Joshi GP, Kehlet H (2019) Postoperative pain management in the era of ERAS: An overview. Best Pract Res Clin Anaesthesiol 33(3):259–267. https://doi.org/10.1016/j.bpa.2019.07.016
Naftalovich R, Singal A, Iskander AJ (2022) Enhanced recovery after surgery (ERAS) protocols for spine surgery - review of literature. Anaesthesiol Intensive Ther 54(1):71–79. https://doi.org/10.5114/ait.2022.113961
Hamilton DL (2018) Pneumothorax following erector spinae plane block. J Clin Anesthesia 52:17. https://doi.org/10.1016/j.jclinane.2018.08.026
Hand WR, Taylor JM, Harvey NR, Epperson TI, Gunselman RJ et al (2015) Thoracolumbar interfascial plane (TLIP) block: a pilot study in volunteers. Can J Anaesth 62(11):1196–1200. https://doi.org/10.1007/s12630-015-0431-y
Ahiskalioglu A, Yayik AM, Alici HA (2017) Ultrasound-guided lateral thoracolumbar interfascial plane (TLIP) block: Description of new modified technique. J Clin Anesth 40:62. https://doi.org/10.1016/j.jclinane.2017.04.015
Pfeiffer G, Oppitz N, Schöne S, Richter-Heine I, Höhne M et al (2006) Analgesia of the axilla using a paravertebral catheter in the lamina technique. Anaesthesist 55:423–427. https://doi.org/10.1007/s00101-005-0969-0
Bouman EAC, Sieben JM, Balthasar AJR, Joesten EA, Gramke HF et al (2017) Boundaries of the thoracic paravertebral space: potential risks and benefits of the thoracic paravertebral block from an anatomical perspective. Surg Radiol Anat 39(10):1117–1125. https://doi.org/10.1007/s00276-017-1857-4
Onishi E, Toda N, Kameyama Y, Yamauchi M (2019) Comparison of clinical efficacy and anatomical investigation between retrolaminar block and erector spinae plane block. Biomed Res Int. https://doi.org/10.1155/2019/2578396
Costache I, Sinclair J, Farrash FA, Nguyen TB, McCartney CJ et al (2016) Does paravertebral block require access to the paravertebral space? Anaesthesia 71:858–859. https://doi.org/10.1111/anae.13527
Adhikary SD, Bernard S, Lopez H, Chin KJ (2018) Erector spinae plane block versus retrolaminar block: a magnetic resonance imaging and anatomical study. Reg Anesth Pain Med 43:756–762. https://doi.org/10.1097/AAP.0000000000000798
Damjanovska M, Stopar Pintaric T, Cvetko E, Vlassakov K (2018) The ultrasound-guided retrolaminar block: volume-dependent injectate distribution. J Pain Res 11:293–299. https://doi.org/10.2147/JPR.S153660
Shanthanna H, Ladha KS, Kehlet H, Joshi GP (2021) Perioperative opioid administration. Anesthesiology 134(4):645–659. https://doi.org/10.1097/ALN.0000000000003572
Kurd MF, Kreitz T, Schroeder G, Vaccaro AR (2017) The role of multimodal analgesia in spine surgery. J Am Acad Orthop Surg 25(4):260–268. https://doi.org/10.5435/JAAOS-D-16-00049
Nordquist D, Halaszynski TM (2014) Perioperative multimodal anesthesia using regional techniques in the aging surgical patient. Pain Res Treat 2014:902174. https://doi.org/10.1155/2014/902174
Varughese S, Ahmed R (2021) Environmental and occupational considerations of anesthesia: a narrative review and update. Anesth Analg 133(4):826–835. https://doi.org/10.1213/ANE.0000000000005504
Gaya da Costa M, Kalmar AF, Struys MMRF (2021) Inhaled anesthetics: environmental role, occupational risk, and clinical use. J Clin Med 10(6):1306. https://doi.org/10.3390/jcm10061306
Horlocker TT, Vandermeuelen E, Kopp SL et al (2018) Regional anesthesia in the patient receiving antithrombotic or thrombolytic therapy: american society of regional anesthesia and pain medicine evidence-based guidelines. Reg Anesth Pain Med 43:263–309. https://doi.org/10.1097/AAP.0000000000000763
Acknowledgements
There is not any conflict of interest between authors.
Funding
Open access funding provided by the Scientific and Technological Research Council of Türkiye (TÜBİTAK).
Author information
Authors and Affiliations
Contributions
Conception or design of the work: KP, SAP; Data collection: KP, MÖ, GA, IG, AGS, ATş, SAP; Data analysis and interpretation: KP, SAP; Drafting the article: KP, SAP; Critical revision of the article: KP, MÖ, GA, IG, AGS, ATş, SAP; Other (Study supervision, fundings, materials…): KP, MÖ, GA, IG, AGS, ATş, SAP.
Corresponding author
Ethics declarations
Conflict of interest
All authors have not any conflict of interest, financial or otherwise.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Peker, K., Aydın, G., Gençay, I. et al. The effect of preemptive retrolaminar block on lumbar spinal decompression surgery. Eur Spine J (2024). https://doi.org/10.1007/s00586-024-08219-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00586-024-08219-4