Abstract
Purpose
The goal of this study was to determine which paraspinal approach provided a better transverse screw angle (TSA) for each vertebral level in lower lumbar surgery.
Methods
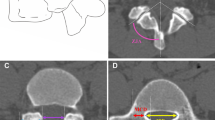
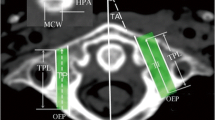
Axial computed tomography (CT) images of 100 patients, from L3 to S1, were used to measure the angulation parameters, including transverse pedicle angle (TPA) and transverse cleavage plane angle (TCPA) of entry from the two approaches. The difference value between TCPA and TPA, defined as difference angle (DA), was calculated. Statistical differences of DA obtained by the two approaches and the angulation parameters between sexes, and the correlation between each angulation parameter and age or body mass index (BMI) were analyzed.
Results
TPA ranged from about 16° at L3 to 30° at S1. TCPA through the Wiltse’s and Weaver’s approach ranged from about −10° and 25° at L3 to 12° and 32° at S1, respectively. The absolute values of DA through the Weaver’s approach were significantly lower than those through the Wiltse’s approach at each level. The angulation parameters showed no significant difference with sex and no significant correlation with age or BMI.
Conclusions
In the lower lumbar vertebrae (L3–L5) and S1, pedicle screw placement through the Weaver’s approach may more easily yield the preferred TSA consistent with TPA than that through the Wiltse’s approach. The reference values obtained in this paper may be applied regardless of sex, age or BMI and the descriptive statistical results may be used as references for applying the two paraspinal approaches.

Similar content being viewed by others
References
Kawaguchi Y, Matsui H, Tsuji H (1996) Back muscle injury after posterior lumbar spine surgery: a histologic and enzymatic analysis. Spine 21(8):941–944
Datta G, Gnanalingham KK, Peterson D, Mendoza N, O’Neill K, Van Dellen J, McGregor A, Hughes SPF (2004) Back pain and disability after lumbar laminectomy: is there a relationship to muscle retraction? Neurosurgery 54(6):1413–1420
Kaptanoglu E, Okutan O, Tekdemir I, Beskonakli E, Deda H (2003) Closed posterior superior iliac spine impeding pediculocorporeal S-1 screw insertion. J Neurosurg Spine 99(2):229–234
Robertson PA, Plank LD (1999) Pedicle screw placement at the sacrum: anatomical characterization and limitations at S1. J Spinal Disord Tech 12(3):227–233
Wiltse LL, Bateman JG, Hutchinson RH, Nelson WE (1968) The paraspinal sacrospinalis-splitting approach to the lumbar spine. J Bone Joint Surg Am 50(5):919–926
Wiltse L, Spencer C (1988) New uses and refinements of the paraspinal approach to the lumbar spine. Spine 13(6):696–706
Weaver EN Jr (2007) Lateral intramuscular planar approach to the lumbar spine and sacrum. J Neurosurg Spine 7(2):270–273
Acharya S, Dorje T, Srivastava A (2010) Lower dorsal and lumbar pedicle morphometry in Indian population: a study of four hundred fifty vertebrae. Spine 35(10):E378–E384
Arman C, Naderi S, Kiray A, Aksu FT, YIlmaz HS, Tetik S, Korman E (2009) The human sacrum and safe approaches for screw placement. J Clin Neurosci 16(8):1046–1049
Kosmopoulos V, Schizas C (2007) Pedicle screw placement accuracy: a meta-analysis. Spine 32(3):E111–E120
Brown CA, Lenke LG, Bridwell KH, Geideman WM, Hasan SA, Blanke K (1998) Complications of pediatric thoracolumbar and lumbar pedicle screws. Spine 23(14):1566–1571
Ota M, Neo M, Fujibayashi S, Takemoto M, Nakamura T (2010) Advantages of the paraspinal muscle splitting approach in comparison with conventional midline approach for s1 pedicle screw placement. Spine 35(11):E452–E457
Schulze CJ, Munzinger E, Weber U (1998) Clinical relevance of accuracy of pedicle screw placement: a computed tomographic-supported analysis. Spine 23(20):2215–2220
Ruland CM, McAfee P, Warden KE, Cunningham BW (1991) Triangulation of pedicular instrumentation. A biomechanical analysis. Spine 16(6 Suppl):S270–S276
Fujibayashi S, Neo M, Takemoto M, Ota M, Nakamura T (2010) Paraspinal-approach transforaminal lumbar interbody fusion for the treatment of lumbar foraminal stenosis. J Neurosurg Spine 13(4):500–508
Hoh DJ, Wang MY, Ritland SL (2010) Anatomic Features of the Paramedian Muscle-Splitting Approaches to the Lumbar Spine. Neurosurgery 66(3):13–24
Mirkovic S, Abitbol JJ, Steinman J, Edwards CC, Schaffler M, Massie J, Garfin SR (1991) Anatomic consideration for sacral screw placement. Spine 16(6S):S289–S294
Barber JW, Boden SD, Ganey T, Hutton WC (1998) Biomechanical study of lumbar pedicle screws: does convergence affect axial pullout strength? J Spinal Disord Tech 11(3):215–220
Smith SA, Abitbol JJ, Carlson GD, Anderson DR, Taggart KW, Garfin SR (1993) The effects of depth of penetration, screw orientation, and bone density on sacral screw fixation. Spine 18(8):1006–1010
Kim NH, Lee HM, Chung IH, Kim HJ, Kim SJ (1994) Morphometric study of the pedicles of thoracic and lumbar vertebrae in Koreans. Spine 19(12):1390–1394
Zindrick MR, Wiltse LL, Doornik A, Widell EH, Knight GW, Patwardhan AG, Thomas JC, Rothman SL, Fields B (1987) Analysis of the morphometric characteristics of the thoracic and lumbar pedicles. Spine 12(2):160–166
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cheng, X., Ni, B., Liu, Q. et al. Can intermuscular cleavage planes provide proper transverse screw angle? Comparison of two paraspinal approaches. Eur Spine J 22, 123–127 (2013). https://doi.org/10.1007/s00586-012-2464-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-012-2464-z