Abstract
Purpose
Although not as life-threatening as anastomotic leakage, anastomotic stricture reduces the quality of life. The risk factors for such an important life complication have not been revealed. This article examines the risk factors affecting anastomotic strictures due to colorectal cancers.
Methods
Patients who underwent anterior and low anterior resection for colorectal cancer under elective conditions between 2015 and 2021 were included in the study. The patients were divided into two groups, those who developed anastomotic stricture and those who did not. The parameters determined between the two groups were compared, and multivariate analysis of statistically significant parameters was performed.
Results
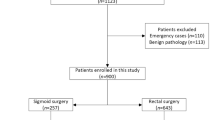
A total of 375 patients were included in the study. The anastomotic stricture was detected in 36 (9.6%) patients. In the multivariate analysis, non-mobilization of the splenic flexure and a proximal clean surgical margin of < 10 cm and a distal surgical margin of < 2 cm were identified as risk factors affecting anastomotic stricture. The risk factor with the highest odds ratio in the development of anastomotic stricture is the non-mobilization of the splenic flexure (p = 0.001, OR 11.375).
Conclusion
It is recommended that the mobilization of the splenic flexure to reduce the development of strictures. In addition, a clean surgical margin of 10 cm proximally and 2 cm distally and high ligation of the inferior mesenteric artery may reduce the development of stricture.
Graphical abstract


Similar content being viewed by others
Data availability
The data are stored locally.
Code availability
Not applicable.
References
Bray F, Ferlay J, Soerjomataram I et al (2018) Global cancer statistics: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424
Jayne DG, Guillou PJ, Thorpe H, Quirke P, Copeland J, Smith AM, Heath RM, Brown JM (2007) Randomized trial of laparoscopic-assisted resection of colorectal carcinoma: 3-year results of the UK MRC CLASICC trial group. J Clin Oncol 25(21):3061–3068. https://doi.org/10.1200/JCO.2006.09.7758
Pramateftakis MG, Kanellos D, Vrakas G, Tsachalis T, Raptis D, Makrantonakis A, Koukouritaki Z, Kanellos I (2010) Progress in rectal cancer staging and treatment. Tech Coloproctol 14(1):29–31. https://doi.org/10.1007/s10151-010-0619-7
Somashekhar SP, Reddy GRK, Deshpande AY, Ashwin KR, Kumar R (2021) A prospective study of real-time identification of line of transection in robotic colorectal cancer surgery by ICG. J Robotic Surg 15:369–374. https://doi.org/10.1007/s11701-020-01095-2
Mirnezami A, Mirnezami R, Chandrakumaran K, Sasapu K, Sagar P, Finan P (2011) Increased local recurrence and reduced survival from colorectal cancer following anastomotic leak: systematic review and meta-analysis. Ann Surg 253(5):890–899. https://doi.org/10.1097/SLA.0b013e3182128929
Arron MNN, Greijdanus NG, Ten Broek RPG, Dekker JWT, van Workum F, van Goor H, Tanis PJ, de Wilt JHW (2021) Trends in risk factors of anastomotic leakage after colorectal cancer surgery (2011–2019): a dutch population-based study. Colorectal Dis 23(12):3251–3261. https://doi.org/10.1111/codi.15911. (Epub 2021 Oct 7 PMID: 34536987)
Sparreboom CL, van Groningen JT, Lingsma HF, Wouters MWJM, Menon AG, Kleinrensink GJ, Jeekel J, Lange JF, Dutch ColoRectal Audit Group (2018) Different risk factors for early and late colorectal anastomotic leakage in a nationwide audit. Dis Colon Rectum 61(11):1258–1266. https://doi.org/10.1097/DCR.0000000000001202. (PMID: 30239395)
Qu H, Liu Y, Bi DS (2015) Clinical risk factors for anastomotic leakage after laparoscopic anterior resection for rectal cancer: a systematic review and meta-analysis. Surg Endosc 29(12):3608–3617. https://doi.org/10.1007/s00464-015-4117-x. (Epub 2015 Mar 6 PMID: 25743996)
Biraima M, Adamina M, Jost R, Breitenstein S, Soll C (2016) Long-term results of endoscopic balloon dilation for treatment of colorectal anastomotic stenosis. Surg Endosc 30(10):4432–4437. https://doi.org/10.1007/s00464-016-4762-8
Chan RH, Lin SC, Chen PC, Lin WT, Wu CH, Lee JC, Lin BW (2020) Management of colorectal anastomotic stricture with multidiameter balloon dilation: long-term results. Tech Coloproctol 24(12):1271–1276. https://doi.org/10.1007/s10151-020-02318-2. (Epub 2020 Aug 5. PMID: 32757156; PMCID: PMC7661393)
Kraenzler A, Maggiori L, Pittet O, Alyami MS, la Denise PÀJ, Panis Y, (2017) Anastomotic stenosis after coloanal, colorectal, and ileoanal anastomosis: what is the best management? Colorectal Dis 19(2):O90–O96. https://doi.org/10.1111/codi.13587. (PMID: 27996184)
Schlegel RD, Dehni N, Parc R, Caplin S, Tiret E (2001) Results of reoperations in colorectal anastomotic strictures. Dis Colon Rectum 44(10):1464–1468. https://doi.org/10.1007/BF02234598. (PMID: 11598475)
Polese L, Vecchiato M, Frigo AC, Sarzo G, Cadrobbi R, Rizzato R, Bressan A, Merigliano S (2012) Risk factors for colorectal anastomotic stenoses and their impact on quality of life: what are the lessons to learn? Colorectal Dis 14(3):e124–e128. https://doi.org/10.1111/j.1463-1318.2011.02819.x. (PMID: 21910814)
Picazo-Ferrera K, Jaurrieta-Rico C, Manzano-Robleda M, Alonso-Lárraga J, de la Mora-Levy J, Hernández-Guerrero A, Ramírez-Solis M (2021) Risk factors and endoscopic treatment for anastomotic stricture after resection in patients with colorectal cancer. Rev Gastroenterol Mex (Engl Ed). 86(1):44–50. https://doi.org/10.1016/j.rgmx.2020.03.001. (Epub 2020 May 6. PMID: 32386994)
Bannura GC, Cumsille MA, Barrera AE, Contreras JP, Melo CL, Soto DC (2004) Predictive factors of stenosis after stapled colorectal anastomosis: prospective analysis of 179 consecutive patients. World J Surg 28(9):921–925. https://doi.org/10.1007/s00268-004-7375-7
Bertocchi E, Barugola G, Benini M, Bocus P, Rossini R, Ceccaroni M, Ruffo G (2019) Colorectal anastomotic stenosis: lessons learned after 1643 colorectal resections for deep infiltrating endometriosis. J Minim Invasive Gynecol 26(1):100–104. https://doi.org/10.1016/j.jmig.2018.03.033. (Epub 2018 Apr 17 PMID: 29678755)
Silva-Velazco J, Stocchi L, Costedio M, Gorgun E, Kessler H, Remzi FH (2016) Is there anything we can modify among factors associated with morbidity following elective laparoscopic sigmoidectomy for diverticulitis? Surg Endosc 30:3541–3551. https://doi.org/10.1007/s00464-015-4651-6
Qin Q, Ma T, Deng Y, Zheng J, Zhou Z, Wang H, Wang L, Wang J (2016) Impact of preoperative radiotherapy on anastomotic leakage and stenosis after rectal cancer resection: post hoc analysis of a randomized controlled trial. Dis Colon Rectum 59(10):934–942. https://doi.org/10.1097/DCR.0000000000000665. (PMID: 27602924)
Terzi C, Bingul M, Arslan NC, Ozturk E, Canda AE, Isik O, Yilmazlar T, Obuz F, Birkay Gorken I, Kurt M, Unlu M, Ugras N, Kanat O, Oztop I (2020) Randomized controlled trial of 8 weeks’ vs 12 weeks’ interval between neoadjuvant chemoradiotherapy and surgery for locally advanced rectal cancer. Colorectal Dis 22(3):279–288. https://doi.org/10.1111/codi.14867. (Epub 2019 Oct 20 PMID: 31566843)
Rondelli F, Pasculli A, De Rosa M, Avenia S, Bugiantella W (2021) Is routine splenic flexure mobilization always necessary in laparotomic or laparoscopic anterior rectal resection? A systematic review and comprehensive meta-analysis. Updates Surg 73(5):1643–1661. https://doi.org/10.1007/s13304-021-01135-y
Hiranyakas A, Da Silva G, Denoya P, Shawki S, Wexner SD (2013) Colorectal anastomotic stricture: is it associated with inadequate colonic mobilization? Tech Coloproctol 17(4):371–375. https://doi.org/10.1007/s10151-012-0929-z
Rink AD, Kienle P, Aigner F, Ulrich A (2020) How to reduce anastomotic leakage in colorectal surgery-report from German expert meeting. Langenbecks Arch Surg 405(2):223–232. https://doi.org/10.1007/s00423-020-01864-5. (Epub 2020 Mar 18 PMID: 32189067)
Yasuda K, Kawai K, Ishihara S, Murono K, Otani K, Nishikawa T, Tanaka T, Kiyomatsu T, Hata K, Nozawa H, Yamaguchi H, Aoki S, Mishima H, Maruyama T, Sako A, Watanabe T (2016) Level of arterial ligation in sigmoid colon and rectal cancer surgery. World J Surg Oncol 14:99. https://doi.org/10.1186/s12957-016-0819-3.PMID:27036117;PMCID:PMC4818479
Khatri VP, Rodrigues-Bigas MA, Flewell R, Petrelli NJ (2018) Operative approach to rectal cancer: an anatomical and technical description. Surg Oncol 27(2):A5–A15. https://doi.org/10.1016/j.suronc.2018.05.033. (PMID: 29937190)
Park IJ, Kim JC (2010) Adequate length of the distal resection margin in rectal cancer: from the oncological point of view. J Gastrointest Surg 14(8):1331–1337. https://doi.org/10.1007/s11605-010-1165-3
Manegold P, Taukert J, Neeff H, Fichtner-Feigl S, Thomusch O (2019) The minimum distal resection margin in rectal cancer surgery and its impact on local recurrence—a retrospective cohort analysis. Int J Surg 69:77–83. https://doi.org/10.1016/j.ijsu.2019.07.029. (Epub 2019 Jul 27 PMID: 31362126)
Cong ZJ, Fu CG, Wang HT, Liu LJ, Zhang W, Wang H (2009) Influencing factors of symptomatic anastomotic leakage after anterior resection of the rectum for cancer. World J Surg 33(6):1292–1297. https://doi.org/10.1007/s00268-009-0008-4. (PMID: 19363687)
Qin Q, Zhu Y, Wu P, Fan X, Huang Y, Huang B, Wang J, Wang L (2019) Radiation-induced injury on surgical margins: a clue to anastomotic leakage after rectal-cancer resection with neoadjuvant chemoradiotherapy? Gastroenterol Rep 7(2):98–106. https://doi.org/10.1093/gastro/goy042. (Epub 2018 Dec 11 PMID: 30976422; PMCID: PMC6454846)
Lee SY, Kim CH, Kim YJ, Kim HR (2018) Anastomotic stricture after ultralow anterior resection or intersphincteric resection for very low-lying rectal cancer. Surg Endosc 32(2):660–666. https://doi.org/10.1007/s00464-017-5718-3. (Epub 2017 Jul 19 PMID: 28726144)
Funding
The authors also declare that they have no competing financial interests.
Author information
Authors and Affiliations
Contributions
AS contributed to design and writing of the study. All authors have contributed in data collection, analysis and critical revision.
Corresponding author
Ethics declarations
Disclosures
Ahmet Surek, Turgut Donmez, Eyup Gemici, Ahmet Cem Dural, Cevher Akarsu, Arif Kaya, Sina Ferahman, Mehmet Abdussamet Bozkurt, Mehmet Karabulut and Halil Alis have no conflict of interest or financial ties to disclose.
Ethical approval
The ethics committee approval for the study was obtained from the local ethics committee (Ethics committee approval date: 07.06.2021 Decision no: 2011–11-18).
Informed consent
For this study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Surek, A., Donmez, T., Gemici, E. et al. Risk factors affecting benign anastomotic stricture in anterior and low anterior resections for colorectal cancer: a single-center retrospective cohort study. Surg Endosc 37, 5246–5255 (2023). https://doi.org/10.1007/s00464-023-10002-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10002-3