Abstract
Background
Several interventions with variable efficacy are available as first-line therapy for patients with achalasia. We assessed the comparative efficacy of different strategies for management of achalasia, through a network meta-analysis combining direct and indirect treatment comparisons.
Methods
We identified six randomized controlled trials in adults with achalasia that compared the efficacy of pneumatic dilation (PD; n = 260), laparoscopic Heller myotomy (LHM; n = 309), and peroral endoscopic myotomy (POEM; n = 176). Primary efficacy outcome was 1-year treatment success (patient-reported improvement in symptoms based on validated scores); secondary efficacy outcomes were 2-year treatment success and physiologic improvement; safety outcomes were risk of gastroesophageal reflux disease (GERD), severe erosive esophagitis, and procedure-related serious adverse events. We performed pairwise and network meta-analysis for all treatments, and used GRADE criteria to appraise quality of evidence.
Results
Low-quality evidence, based primarily on direct evidence, supports the use of POEM (RR [risk ratio], 1.29; 95% confidence intervals [CI], 0.99–1.69), and LHM (RR, 1.18 [0.96–1.44]) over PD for treatment success at 1 year; no significant difference was observed between LHM and POEM (RR 1.09 [0.86–1.39]). The incidence of severe esophagitis after POEM, LHM, and PD was 5.3%, 3.7%, and 1.5%, respectively. Procedure-related serious adverse event rate after POEM, LHM, and PD was 1.4%, 6.7%, and 4.2%, respectively.
Conclusions
POEM and LHM have comparable efficacy, and may increase treatment success as compared to PD with low confidence in estimates. POEM may have lower rate of serious adverse events compared to LHM and PD, but higher rate of GERD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Achalasia is a chronic disorder characterized by esophageal dysmotility and inadequate lower esophageal sphincter (LES) relaxation commonly manifesting with dysphagia and regurgitation. In the absence of a cure, the therapeutic goals in achalasia include symptom reduction and improved esophageal emptying [1, 2]. Endoscopic pneumatic dilation (PD) and laparoscopic Heller myotomy (LHM) often combined with an anti-reflux procedure have historically been the two definitive first-line therapies for achalasia, while peroral endoscopic myotomy (POEM) has emerged as an efficacious endoscopic therapy for achalasia over the past decade. Oral and endoscopic pharmacologic treatments are reserved as second-line options for patients that are not candidates for first-line therapy [3, 4].
PD is the most commonly performed treatment worldwide, and is minimally invasive with long-term success in 50–93% patients, although it usually requires several treatment sessions [5, 6]. On the other hand, LHM combined with an anti-reflux procedure is a more invasive treatment often requiring only one treatment session with success rates of 71% to –92% [7]. In the European Achalasia trial, the success rate of PD and LHM was shown to depend on achalasia subtype with type II achalasia having the highest success rate at 5 years (PD 96%; LHM 88%) and type III achalasia with the poorest success rate at 5 years (PD 48%; LHM 86%) [8]. The success rate of POEM in prospective cohorts has been greater than 90% and maintained across achalasia subtypes, thought to be related to the ability to perform a proximal extended myotomy in type III, or spastic achalasia. A consistent observation with POEM has been a higher risk of gastroesophageal reflux disease (GERD) compared to PD or LHM [9, 10].
In the last year, two landmark multicenter RCTs comparing POEM to PD and POEM to LHM have been published providing a framework for assessing comparative efficacy and safety of these interventions to inform optimal first-line intervention for treatment of patients with achalasia [11, 12]. Hence, we performed a pairwise and network meta-analysis combining direct (from RCTs directly comparing treatments of interest) and indirect evidence (from RCTs comparing treatments of interest with a common comparator), to compare the relative efficacy and safety of PD, LHM, and POEM for the management of achalasia. We used Grading of Recommendations Assessment, Development and Evaluation (GRADE) criteria for network meta-analysis to appraise quality of evidence [13].
Methods
This systematic review is reported according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) for network meta-analyses (PRISMA-NMA) statement and was conducted following a priori established protocol [14]. We also followed good research practices as outlined in the ISPOR (International Society for Pharmacoeconomics and Outcomes Research) report on interpreting indirect treatment comparisons and network meta-analysis for health-care decision making.
Selection criteria
Studies included in this meta-analysis were RCTs with minimum follow-up of 1 year that met the following inclusion criteria: (a) Patients: adults (age > 18 years) with achalasia, treated with (b) Interventions and Comparators: PD, LHM, and POEM, and reported (c) Outcome: treatment success assessed at 1 year.
We excluded (a) observational or non-randomized studies, (b) RCTs of endoscopic botulinum toxin injection, as this is considered second-line therapy for patients who are not candidates for first-line therapy, (c) RCTs of oral therapies reserved for patients who are not candidates for first-line therapy (i.e., oral smooth muscle relaxants), and (c) trials with short duration of follow-up (< 1y) [15].
Search strategy
The search strategy was conducted updating a prior systematic literature review performed as part of the recent American Society of Gastrointestinal Endoscopy (ASGE) guidelines [16] through December 2019. Briefly, in this guideline, combinations of subject headings and text words were used, including Esophageal Achalasia OR cardiospasm OR achalasia OR megaesophagus OR mega-esophagus OR megaoesophagus OR mega-oesophagus AND Botulinum Toxins OR botulin* OR botox OR myotomy OR Heller OR peroral OR per oral OR POEM OR LHM OR Dilatation/OR dilatation. Detailed search strategies can be viewed in the ASGE guidelines [16] and Supplementary Table 1.
An updated literature search of Pubmed and conference proceedings of Digestive Disease Week (DDW), United European Gastroenterology Week (UEG week), European Society of Gastrointestinal Endoscopy (ESGE) days was performed on December 20, 2019 to identify additional studies.
Data abstraction and quality assessment
Data on study-, patient-, and treatment-related characteristics were abstracted onto a standardized form, by two authors independently (AF, RY). The risk of bias of individual studies was assessed in the context of the primary outcome, using the Cochrane Risk of Bias 2 assessment tool [17].
Outcomes assessed
The primary efficacy outcome was treatment success at 1 year. Treatment success was defined based on decrease of Eckardt score (which measures symptom severity for dysphagia, regurgitation, retrosternal pain, and weight loss) [18] to ≤ 3 in 3 RCTs [11, 12, 19], absence of dysphagia in 2 RCTs (according to a specific questionnaire in the study by Borges et al. [20], or patient-reported improvement of symptoms in the study by Kostic et al. [21]), and according to DeMeester grading of dysphagia in a single RCT [22].
Secondary efficacy outcomes included treatment success at 2 years and physiologic outcomes (reduction in basal pressure of the lower esophageal sphincter [LES]; decrease in integrated relaxation pressure [IRP], post-treatment height of barium contrast on timed barium esophagram). Primary safety outcome was risk of post-treatment GERD at 1 year from the therapy; secondary safety outcomes were risk of severe erosive esophagitis (LA Grade C or D), and procedure-related serious adverse events.
Statistical analysis
Direct meta-analysis was performed using the Mantel–Haenszel fixed-effects model (in the absence of conceptual heterogeneity and < 5 studies) to estimate pooled risk ratio (RR) and 95% confidence intervals (CI); with small number of studies, random effects models can be unstable [23].
We assessed statistical heterogeneity using I2 statistic, with values over 50% indicating substantial heterogeneity [24]. Due to the small number of trials, formal assessment of publication bias was not performed. Direct comparisons were performed using RevMan v5.3 (Cochrane Collaboration, Copenhagen, Denmark) (Review Manager (RevMan), ver. 5.3 ed: The Cochrane Collaboration, 2014). Next, we conducted network meta-analysis using a multivariate fixed-effects meta-regression as described elsewhere [25]. We used a frequentist approach based on a mixed-effects consistency model and provided a point estimate from the network along with 95% CI from the frequency distribution of the estimate.
The primary outcome (treatment success at 1 year) was analyzed using the network meta-analysis, while treatment success at 2 years was compared only through a direct meta-analysis. Pooled prevalence of procedure-related serious adverse events and of GERD outcomes was reported and pooled estimates, computed through the random effects model by DerSimonian and Laird test and expressed as mean and standard deviation, of physiological outcomes (reduction in basal pressure of LES, decrease in IRP, and post-treatment height of barium contrast on barium esophagogram) were calculated.
The quality of evidence derived from the pairwise and network meta-analysis was judged using the GRADE framework. In this approach, direct evidence from RCTs starts at high quality and can be rated down based on risk of bias, indirectness, imprecision, inconsistency (or heterogeneity) and/or publication bias, to levels of moderate, low, and very low quality (Supplementary Table 2). The rating of indirect estimates starts at the lowest rating of the two pairwise estimates that contribute as first-order loops to the indirect estimate but can be rated down further for imprecision or intransitivity (dissimilarity between studies in terms of clinical or methodological characteristics). If direct and indirect estimates were similar (i.e., coherent), then the higher of their rating was assigned to the network meta-analysis estimates.
Results
Studies
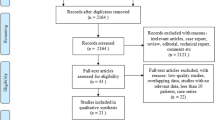
From 38,354 unique studies identified using the search strategy, 6 RCTs met inclusion criteria and are included in the network meta-analysis to compare three different strategies for management of achalasia. Figure 1 shows the flow chart of study selection.
Table 1 summarizes the RCTs included in the network meta-analysis. Overall, these six trials included 745 patients. All six RCTs were two-arm controlled trials, in which four compared LHM with PD [19,20,21,22], one compared POEM to PD [11] and one compared POEM with LHM [12]. Overall, 309 patients were treated with LHM, 260 with PD, and 176 with POEM. The network of the included trials is reported in Fig. 2.
Network geometry of trials. Network of included studies with the available direct comparisons between interventions for management of achalasia. The size of the nodes and the thickness of the edges are weighted according to the number of studies evaluating each treatment and direct comparison, respectively. PD pneumatic dilation, LHM laparoscopic Heller myotomy, POEM peroral endoscopic myotomy
All RCTs enrolled treatment-naïve patients except for the RCT by Werner et al. [12], in which 35.7% patients were previously treated for achalasia (26.2% treated with PD, 6.7% with botulin toxin injection and 2.7% with combined PD and botulinum toxin). LHM was combined with Dor fundoplication in four studies [12, 19, 20, 22] and with Toupet fundoplication in one RCT [21].
The primary outcome (treatment success at 1 year) was reported in all studies, whereas only 4 RCTs reported treatment success at 2 years [12, 19, 20, 22].
Serious adverse events were not consistently defined or reported in the trials.
Demographical and clinical characteristics of trial patients are reported in the Supplementary Table 3. Baseline patient characteristics and prognostic factors (namely, age, gender, body mass index (BMI), baseline Eckardt score, baseline LES pressure) were comparably distributed in the intervention and comparator groups and across different trials. Achalasia subtypes according to manometry findings were reported in 3 RCTs [11, 12, 19] with 111 (20.1%) achalasia type I, 358 achalasia type II (64.8%), and 49 achalasia type III (8.8%).
Out of 745 patients enrolled in the included trials, 397 were male (53.2%) and baseline Eckardt score ranged from 6 to 9 while mean baseline LES pressure ranged from 23.9 to 39.8 mmHg.
Risk of bias assessment was performed in the context of the primary outcome. Due to lack of blinding of patients and physicians (outcome assessors) for a subjective outcome, studies were deemed to be at high risk of performance and detection bias (Supplementary Fig. 1).
Comparative efficacy of first-line interventions
Treatment success at 1 year
Based on pairwise meta-analysis of 4 RCTs (376 patients) [19,20,21,22], LHM was more effective than PD (RR, 1.13; 95% CI 1.03–1.24; Fig. 3), albeit with considerable heterogeneity (I2 = 64%). Based on single RCTs, POEM was more effective than PD (RR, 1.50 [1.24–1.81]) [11] and similar to LHM [12] (RR, 1.02 [0.91–1.14]; Fig. 3). Evidence from direct estimates comparing LHM vs. PD and POEM vs. PD was rated down for serious risk of bias (lack of blinding) and serious imprecision (low event rate, with optimal information size threshold of 200 events not met).
On network meta-analysis, combining direct and indirect effect estimates, similar findings were observed. There was low confidence in estimates supporting higher efficacy of LHM vs. PD (RR, 1.18 [0.96–1.44]) and of POEM vs. PD (RR, 1.29 [0.99–1.69)]) (Table 2 and Supplementary Table 4). Quality of evidence, primarily based on direct evidence, was rated down due to serious risk of bias, and due to serious imprecision (lower limit of 95% CI crossing unity). No significant incoherence (differences in direct and indirect estimates) was observed in closed loops and no evidence of inconsistency was registered (Cochran’s Q test 2.37, p = 0.6684). No significant difference was observed in the efficacy of POEM vs. LHM, with very low confidence in estimates supporting the use of POEM and LHM due to very serious imprecision and serious risk of bias (Supplementary Table 4).
Secondary efficacy outcomes
Treatment success at 2 years
On direct meta-analysis, based on 2 RCTs (273 patients) [8, 20], there was no significant difference in treatment success at 2 years between LHM vs. PD (RR, 1.05 [0.94–1.16]; I2 = 0%) (Supplementary Fig. 2). POEM was more effective than PD at 2 years (RR, 1.76 [1.37–2.25]); Supplementary Fig. 2). The efficacy of LHM and POEM was comparable at 2 years (RR, 1.02 [0.90–1.15]).
Physiologic outcomes
Secondary physiologic outcomes assessed at 1 year are reported in supplementary table 5.
The decrease in LES basal pressure was of 18.5 mmHg ± 2.3 with PD (186 patients), 18.9 mmHg ± 4.0 after LHM (131 patients), and 17.1 mmHg ± 4.0 after POEM (64 patients). The decrease in integrated relaxation pressure (IRP) was of 10.3 mmHg ± 4.9 with PD (66 patients), 15.3 mmHg ± 5.6 after LHM (109 patients), and 16.3 mmHg ± 1 after POEM (176 patients).
At 1 year, no evidence of barium contrast retention was reported after PD and LHM, while the trial by Ponds et al. [11] reported 1.7 cm (interquartile range: 0–3.3) of barium contrast retention after POEM. At 2 years, 1.84 cm (0–8.8), 1.9 cm (0–6.8), and 2.3 cm (0–3.7) of barium contrast retention were registered after PD, LHM, and POEM, respectively (Supplementary Table 5).
Comparative safety of first-line interventions
Risk of gastroesophageal reflux disease (GERD)
The clinical and objective evaluation of GERD are reported in Table 3.
The pooled rate of endoscopic evidence of esophagitis was 14.7% (95% CI: 6.5%–13.1%) after PD based on 2 RCTs [11, 19], 24.9% (16.4%–33.3%) after LHM based on 2 RCTs [12, 19], and 45.4% (38.1%–52.9%) after POEM based on 2 RCTs [11, 12]. The overall incidence of severe esophagitis after LHM, PD, and POEM was 3.7% (0%–8.1%), 1.5% (0%–3.7%), and 5.3% (2%–8.6%), respectively. Abnormal acid exposure was registered in 20.4% (7.8%–32.9%) of patients after PD, 18.6% (2.5%–34.6%) after LHM, and 30% (19.3%–40.7%) after POEM while mean acid exposure time was 2.3% (1.5%–3.1%), 4.3% (2.2%–6.4%), 5.8% (5%–6.6%) after PD, LHM, and POEM, respectively.
Risk of treatment-related serious adverse events
Supplementary Table 6 reports the incidence of serious adverse events observed in the included trials. Risk of serious procedure-related adverse events with LHM, PD, and POEM was 6.7% (95% CI: 1.4%–11.9%), 4.2% (1.8%–6.6%), and 1.4% (0%–3.2%), The most frequent serious complication after PD was perforation, which ranged from 1.5% to 8% of treated patients. In two RCTs [19, 22], 12% of patients treated with LHM experienced a severe mucosal injury, while the perforation rate for LHM was 4% in the study by Hamdy and colleagues [22] and 2.7% in the trial by Werner et al. [12]. Overall, perforation rate was 4.2% after PD and 1.2% with LHM, while none of the patients treated with POEM experienced this complication.
Discussion
Treatment choice for achalasia represents a common challenge and a matter of debate in clinical practice. Though definitive endoscopic or surgical interventions have been studied, there has been limited synthesis of data on the comparative efficacy of these treatments, in particular since the development of POEM. Through a network meta-analysis, and using GRADE criteria to appraise quality of evidence, we made several key observations on the comparative efficacy and safety of these interventions. First, POEM and LHM may be more effective than PD, and comparable to each other, in decreasing achalasia-related symptoms at 1 year. Second, the risk of GERD was higher with POEM as compared to PD or LHM, but the risk of severe erosive esophagitis was low across all interventions. Overall risk of serious adverse events including perforation was lower with POEM as compared to PD or LHM.
Findings from this meta-analysis combined with consideration of relevant clinical factors can help guide clinicians and patients on treatment selection. Achalasia subtype is well established as critical prognostic factor. While we were unable to compare therapeutic efficacy across achalasia subtypes, prior experiences and studies suggest that efficacy in type III achalasia is greater following POEM with a proximal extended esophageal myotomy compared to LHM without extended myotomy or PD, due to the ability to treat not only the lower esophageal sphincter but also the spasticity in the distal esophageal smooth muscle. As such, the ASGE 2020 guideline on the management of achalasia, the American College of Gastroenterology 2020 guideline for Achalasia, as well as the Best Practice Advice from the American Gastroenterological Association Institute in 2017 recommend POEM as the preferred treatment for management of type III achalasia [16, 26].
Additional patient-specific and resource considerations are relevant to choice of therapy. A recent systematic review and meta-analysis by Oude Nijhuis and colleagues additionally identified older age and presence of sigmoid-shaped esophagus as poor predictors of treatment success [27]. Health-care utilization is additionally an important consideration. Compared to POEM, mean operative time, blood loss, and requirements for narcotics are generally greater with LHM and length of hospital stay is either similar or longer with LHM [28,29,30]. Overall, direct costs for both POEM and LHM do not significantly differ, though when considering quality adjusted life years, POEM appeared to be cost effective compared to LHM [31]. While PD utilizes fewer resources, patients should be aware that outcomes following PD are optimized with a sequential dilation protocol. In fact, in this network meta-analysis POEM remained more effective than PD at 2 years, though the observed efficacy of LHM vs PD was not apparent at 2 years. Discordancy in efficacy is likely driven by variation in PD protocols among studies, as depicted in Table 1, which challenges the ability to actually compare long-term efficacy outcomes. All things considered, the ultimate therapeutic decision should be patient centered based on shared decision-making models, and this is an area that requires further investigation and understanding.
An important strength of this network meta-analysis is the inclusion of RCTs alone and inclusion of new trials, in particular, the two landmark head-to-head RCTs comparing POEM to LHM and PD [11, 12]. Prior meta-analyses predated these RCTs, included both observational and randomized studies, and did not objectively appraise the overall quality of evidence using standardized GRADE methodology [7, 32].
Although the finding of increased rate of post-treatment GERD after POEM was expected, it is important to discuss the clinical implications. Ten to 20-year long-term follow-up after Heller myotomy reports high incidence of GERD and erosive complications including strictures, Barrett’s esophagus, and esophageal adenocarcinoma, which in turn contribute to the failure rate of myotomy at 10 years [33]. As such, Heller myotomy is often performed with an anti-reflux procedure. In POEM, the lack of a combined anti-reflux procedure to strengthen the integrity of the anti-reflux barrier [34] likely augments a gastroesophageal reflux physiology following POEM. However, the pooled estimate of severe erosive reflux disease following POEM in the short term is low. A previous meta-analysis found that approximately 30 patients should be treated with LHM over POEM to prevent 1 case of post-procedure severe esophagitis [34]. Further, initial experiences of endoscopic transoral incisionless fundoplication following POEM have been shown to reduce risks of esophagitis and esophageal acid exposure [35]. Nonetheless, long-term follow-up of consequences of GERD post POEM needs to be studied.
There are certain limitations, related to both the network meta-analysis as well as individual studies, which merit further discussion. The studies had a short duration of follow-up, and the primary outcome of this network meta-analysis was focused on short-term (1-year) success. Limited post-intervention follow-up prevents the ability to understand long-term comparative efficacy between interventions, which is critical for a chronic disease. There was also a paucity of direct head-to-head comparative trials, in particular comparing POEM to the other treatments. Further, performance and detection bias related to the non-blinded design of included trials introduced significant risk of bias. Performance and detection bias are not easily avoidable in RCTs testing new devices or techniques in surgery or endoscopy, given the nature of the intervention under study, and this represents a limitation in particular when considering subjective outcomes such as improvement of symptoms in patients with achalasia. Assessment of vital physiologic outcomes by blinded readers can overcome limitations related to blinding in these trials; however, these outcomes were infrequently and/or inconsistently reported in trials data which limit ability to compare post-treatment physiologic efficacy. Similarly, treatment-related adverse events were poorly reported and a thorough assessment of risk–benefit profile could not be performed. Finally, inherent to network meta-analyses is risk of misinterpretation due to conceptual heterogeneity, related to differences in participants, interventions, co-interventions/background treatment, and outcome assessment, which may limit comparability of trials; these cannot be adequately accounted for with study-level synthesis, and individual participant-level pooled analyses will be needed.
In conclusion, based on network meta-analysis, POEM and LHM may be comparable to each other, and both may be more effective than PD, in the definitive management of treatment-naïve patients with achalasia. While the risk of GERD is higher with POEM, overall rate of severe erosive esophagitis is low. Rate of treatment-related serious adverse events may be lower with POEM versus LHM or PD. Future prospective studies comparing long-term efficacy and safety of POEM, LHM, and PD, particularly across specific achalasia subtypes are warranted.
References:
Vaezi MF, Pandolfino JE, Vela MF (2013) ACG clinical guideline: diagnosis and management of achalasia. Am J Gastroenterol 108(8):1238–1250
Francis DL, Katzka DA (2010) Achalasia: update on the disease and its treatment. Gastroenterology 139(2):369–374
Vaezi MF, Richter JE (1998) Current therapies for achalasia: comparison and efficacy. J Clin Gastroenterol 27(1):21–35
Coccia G, Bortolotti M, Michetti P, Dodero M (1991) Prospective clinical and manometric study comparing pneumatic dilatation and sublingual nifedipine in the treatment of oesophageal achalasia. Gut 32(6):604–606
Vela MF, Richter JE, Khandwala F, Blackstone EH, Wachsberger D, Baker ME, Rice TW (2006) The long-term efficacy of pneumatic dilatation and Heller myotomy for the treatment of achalasia. Clin Gastroenterol Hepatol 4(5):580–587
Hulselmans M, Vanuytsel T, Degreef T, Sifrim D, Coosemans W, Lerut T, Tack J (2010) Long-term outcome of pneumatic dilation in the treatment of achalasia. Clin Gastroenterol Hepatol 8(1):30–35
Schoenberg MB, Marx S, Kersten JF, Rösch T, Belle S, Kähler G, Vassiliou MC, Lüth S, von Renteln D (2013) Laparoscopic Heller myotomy versus endoscopic balloon dilatation for the treatment of achalasia: a network meta-analysis. Ann Surg 258(6):943–952
Moonen A, Annese V, Belmans A, Bredenoord AJ, Bruley des Varannes S, Costantini M, Dousset B, Elizalde JI, Fumagalli U, Gaudric M, Merla A, Smout AJ, Tack J, Zaninotto G, Busch OR, Boeckxstaens GE (2016) Long-term results of the European achalasia trial: a multicentre randomised controlled trial comparing pneumatic dilation versus laparoscopic Heller myotomy. Gut 65(5):732–739
Khan MA, Kumbhari V, Ngamruengphong S, Ismail A, Chen YI, Chavez YH, Bukhari M, Nollan R, Ismail MK, Onimaru M, Balassone V, Sharata A, Swanstrom L, Inoue H, Repici A, Khashab MA (2017) Is POEM the answer for management of spastic esophageal disorders? A systematic review and meta-analysis. Dig Dis Sci 62(1):35–44
Evensen H, Kristensen V, Larssen L, Sandstad O, Hauge T, Medhus AW (2019) Outcome of peroral endoscopic myotomy (POEM) in treatment-naive patients. A systematic review. Scand J Gastroenterol 54(1):1–7
Ponds FA, Fockens P, Lei A, Neuhaus H, Beyna T, Kandler J, Frieling T, Chiu PWY, Wu JCY, Wong VWY, Costamagna G, Familiari P, Kahrilas PJ, Pandolfino JE, Smout AJPM, Bredenoord AJ (2019) Effect of peroral endoscopic myotomy vs pneumatic dilation on symptom severity and treatment outcomes among treatment-naive patients with achalasia: a randomized clinical trial. JAMA 322(2):134–144
Werner YB, Hakanson B, Martinek J, Repici A, von Rahden BHA, Bredenoord AJ, Bisschops R, Messmann H, Vollberg MC, Noder T, Kersten JF, Mann O, Izbicki J, Pazdro A, Fumagalli U, Rosati R, Germer CT, Schijven MP, Emmermann A, von Renteln D, Fockens P, Boeckxstaens G, Rösch T (2019) Endoscopic or surgical myotomy in patients with idiopathic achalasia. N Engl J Med 381(23):2219–2229
Puhan MA, Schünemann HJ, Murad MH, Li T, Brignardello-Petersen R, Singh JA, Kessels AG, Guyatt GH, GRADE Working Group (2014) A GRADE Working Group approach for rating the quality of treatment effect estimates from network meta-analysis. BMJ 349:g5630
Hutton B, Salanti G, Caldwell DM, Chaimani A, Schmid CH, Cameron C, Ioannidis JP, Straus S, Thorlund K, Jansen JP, Mulrow C, Catalá-López F, Gøtzsche PC, Dickersin K, Boutron I, Altman DG, Moher D (2015) The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: checklist and explanations. Ann Intern Med 162(11):777–784
Novais PA, Lemme EM (2010) 24-h pH monitoring patterns and clinical response after achalasia treatment with pneumatic dilation or laparoscopic Heller myotomy. Aliment Pharmacol Ther 32(10):1257–1265
Khashab MA, Vela MF, Thosani N, Agrawal D, Buxbaum JL, Abbas Fehmi SM, Fishman DS, Gurudu SR, Jamil LH, Jue TL, Kannadath BS, Law JK, Lee JK, Naveed M, Qumseya BJ, Sawhney MS, Yang J, Wani S (2020) ASGE guideline on the management of achalasia. Gastrointest Endosc 91(2):213–227
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng H-Y, Corbett MS, Eldridge SM, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Eckardt VF (2001) Clinical presentations and complications of achalasia. Gastrointest Endosc Clin N Am 11(2):281–vi
Boeckxstaens GE, Annese V, des Varannes SB, Chaussade S, Costantini M, Cuttitta A, Elizalde JI, Fumagalli U, Gaudric M, Rohof WO, Smout AJ, Tack J, Zwinderman AH, Zaninotto G, Busch OR, European Achalasia Trial Investigators (2011) Pneumatic dilation versus laparoscopic Heller's myotomy for idiopathic achalasia. N Engl J Med 364(19):1807–1816
Borges AA, Lemme EM, Abrahao LJ Jr, Madureira D, Andrade MS, Soldan M, Helman L (2014) Pneumatic dilation versus laparoscopic Heller myotomy for the treatment of achalasia: variables related to a good response. Dis Esophagus 27(1):18–23
Kostic S, Kjellin A, Ruth M, Lönroth H, Johnsson E, Andersson M, Lundell L (2007) Pneumatic dilatation or laparoscopic cardiomyotomy in the management of newly diagnosed idiopathic achalasia. Results of a randomized controlled trial. World J Surg 31(3):470–478
Hamdy E, EI Nakeeb A, EI Hanfy E, EI Hemaly M, Salah T, Hamed H, EI Hak NG (2015) Comparative study between laparoscopic Heller myotomy versus pneumatic dilatation for treatment of early achalasia: a prospective randomized study. J Laparoendosc Adv Surg Tech A 25(6):460–464
Murad MH, Montori VM, Ioannidis JP, Jaeschke R, Devereaux PJ, Prasad K, Neumann I, Carrasco-Labra A, Agoritsas T, Hatala R, Meade MO, Wyer P, Cook DJ, Guyatt G (2014) How to read a systematic review and meta-analysis and apply the results to patient care: users' guides to the medical literature. JAMA 312(2):171–179
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560
Dias S, Sutton AJ, Ades AE, Welton NJ (2013) Evidence synthesis for decision making 2: a generalized linear modeling framework for pairwise and network meta-analysis of randomized controlled trials. Med Decis Making 33(5):607–617
Kahrilas PJ, Katzka D, Richter JE (2017) Clinical practice update: the use of per-oral endoscopic myotomy in achalasia: expert review and best practice advice from the AGA Institute. Gastroenterology 153(5):1205–1211
Oude Nijhuis RAB, Prins LI, Mostafavi N, van Etten-Jamaludin FS, Smout AJPM, Bredenoord AJ (2019) Factors associated with achalasia treatment outcomes: systematic review and meta-analysis. Clin Gastroenterol Hepatol. in press.
Chan SM, Wu JC, Teoh AY, Yip HC, Ng EK, Lau JY, Chiu PW (2016) Comparison of early outcomes and quality of life after laparoscopic Heller's cardiomyotomy to peroral endoscopic myotomy for treatment of achalasia. Dig Endosc 28(1):27–32
Docimo S Jr, Mathew A, Shope AJ, Winder JS, Haluck RS, Pauli EM (2017) Reduced postoperative pain scores and narcotic use favor per-oral endoscopic myotomy over laparoscopic Heller myotomy. Surg Endosc 31(2):795–800
Wirsching A, Boshier PR, Klevebro F, Kaplan SJ, Seesing MF, El-Moslimany R, Ross A, Low DE (2019) Comparison of costs and short-term clinical outcomes of per-oral endoscopic myotomy and laparoscopic Heller myotomy. Am J Surg 218(4):706–711
Greenleaf EK, Winder JS, Hollenbeak CS, Haluck RS, Mathew A, Pauli EM (2018) Cost-effectiveness of per oral endoscopic myotomy relative to laparoscopic Heller myotomy for the treatment of achalasia. Surg Endosc 32(1):39–45
Aiolfi A, Bona D, Riva CG, Micheletto G, Rausa E, Campanelli G, Olmo G, Bonitta G, Bonavina L (2020) Systematic review and Bayesian network meta-analysis comparing laparoscopic Heller myotomy, pneumatic dilatation, and peroral endoscopic myotomy for esophageal achalasia. J Laparoendosc Adv Surg Tech A 30(2):147–155
Csendes A (1991) Results of surgical treatment of achalasia of the esophagus. Hepatogastroenterology 38(6):474–480
Repici A, Fuccio L, Maselli R, Mazza F, Correale L, Mandolesi D, Bellisario C, Sethi A, Khashab MA, Rösch T, Hassan C (2018) GERD after per-oral endoscopic myotomy as compared with Heller's myotomy with fundoplication: a systematic review with meta-analysis. Gastrointest Endosc 87(4):934–943
Tyberg A, Choi A, Gaidhane M, Kahaleh M (2018) Transoral incisional fundoplication for reflux after peroral endoscopic myotomy: a crucial addition to our arsenal. Endosc Int Open 6(5):E549–E552
Funding
Siddharth Singh: Research grants from AbbVie and Janssen; Personal fees from AbbVie, Takeda, Pfizer in the last 24 months. Syed M Abbas Fehmi: Consulting for Boston Scientific and Cook Medical. Rena Yadlapati: Consulting for Ironwood Pharmaceuticals, Medtronic, Diversatek. Advisory Board: Phatom Pharmaceuticals. Research grant from Ironwood Pharmaceuticals. Antonio Facciorusso, Vito Annese, John Lipham: None. Open access funding provided by Università di Foggia within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Contributions
Study concept and design: AF, SS, and RY. Acquisition of data: AF and RY. Analysis and interpretation of data: AF, SS, and RY. Drafting of the manuscript: all authors. Critical revision of the manuscript for important intellectual content: all authors. Approval of the final manuscript: all of the authors. Guarantor of the article: AF.
Corresponding author
Ethics declarations
Disclosures:
Drs Antonio Facciorusso, Siddharth Singh, Syed M Abbas Fehmi, Vito Annese, John Lipham, and Rena Yadlapati have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Facciorusso, A., Singh, S., Abbas Fehmi, S.M. et al. Comparative efficacy of first-line therapeutic interventions for achalasia: a systematic review and network meta-analysis. Surg Endosc 35, 4305–4314 (2021). https://doi.org/10.1007/s00464-020-07920-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07920-x