Abstract
Background
Ureteral injury is a feared complication in colorectal surgery that has been increasing over the past decade. Some have attributed this to an increased adoption of minimally invasive surgery (MIS), but the literature is hardly conclusive. In this study we aim to further assess the overall trend of ureteral injuries in colorectal surgery, and investigate propensity adjusted contributions from open and MIS to include robotic-assisted surgery.
Methods
This is a retrospective analysis of colorectal surgeries from 2006 to 2016 using the Nationwide Inpatient Sample (NIS) database. Multivariable logistic regression was performed to identify predisposing and protective factors. Demographics, hospital factors, and case-mix differences for open and MIS were accounted for via propensity analysis. The NIS coding structure changed in 2015, which could introduce a potential source of incongruity in complication rates over time. As a result, all statistical analyses included only the first nine years of data, or were conducted before and after the change for comparison.
Results
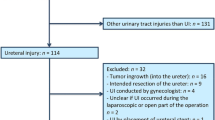
Of 514,162 colorectal surgeries identified there were 1598 ureteral injuries (0.31%). Ureteral injuries were found to be increasing through 2015 (2.3/1000 vs 3.3/1000; p < 0.001) and through the coding transition to 2016 (4.8/1000; p < 0.001). This trend was entirely accounted for by injuries made during open surgery, with decreasing injury rates for MIS over time. Adjusted odds ratio (OR) for ureteral injury with all MIS vs. open cases was 0.81 (95% CI 0.70–0.93, p = 0.003) and for robotic-assisted surgery alone versus open cases was 0.50 (95% CI 0.33–0.77, p = 0.001).
Conclusions
The incidence rate of ureteral injuries during open colorectal surgery is increasing over time, but have been stable or decreasing for MIS cases. These findings hold even after using propensity score analysis. More research is needed to further delineate the impact of MIS and robotic-assisted surgery on ureteral injuries.



Similar content being viewed by others
References
Palaniappa NC, Telem DA, Ranasinghe NE, Divino CM (2012) Incidence of iatrogenic ureteral injury after laparoscopic colectomy. Arch Surg 147:267–271. https://doi.org/10.1001/archsurg.2011.2029
Andersen P, Andersen LM, Iversen LH (2015) Iatrogenic ureteral injury in colorectal cancer surgery: a nationwide study comparing laparoscopic and open approaches. Surg Endosc 29:1406–1412. https://doi.org/10.1007/s00464-014-3814-1
Marcelissen TAT, Den Hollander PP, Tuytten TRAH, Sosef MN (2016) Incidence of iatrogenic ureteral injury during open and laparoscopic colorectal surgery. Surg Laparosc Endosc Percutan Tech 26:513–515. https://doi.org/10.1097/sle.0000000000000335
Halabi WJ, Jafari MD, Nguyen VQ, Carmichael JC, Mills S, Pigazzi A, Stamos MJ (2014) Ureteral injuries in colorectal surgery. Dis Colon Rectum 57:179–186. https://doi.org/10.1097/dcr.0000000000000033
Gild P, Kluth LA, Vetterlein MW, Engel O, Chun FKH, Fisch M (2018) Adult iatrogenic ureteral injury and stricture–incidence and treatment strategies. Asian J Urol 5:101–106. https://doi.org/10.1016/j.ajur.2018.02.003
Selzman AA, Spirnak JP (1996) Iatrogenic ureteral injuries: 20-year experience in treating 165 injuries. J Urol 155:878–881. https://doi.org/10.1016/S0022-5347(01)66332-8
Douissard J, Ris F, Morel P, Buchs NC (2018) Current strategies to prevent iatrogenic ureteral injury during colorectal surgery. Surg Technol Int 32:119–124
Gilmour DT, Baskett TF (2005) Disability and litigation from urinary tract injuries at benign gynecologic surgery in Canada. Obstet Gynecol 105:109–114. https://doi.org/10.1097/01.AOG.0000144127.78481.8c
Parpala-Spårman T, Paananen I, Santala M, Ohtonen P, Hellström P (2008) Increasing numbers of ureteric injuries after the introduction of laparoscopic surgery. Scand J Urol Nephrol 42:422–427. https://doi.org/10.1080/00365590802025857
Romero V, Akpinar H, Smith JJ, Assimos DG (2011) Changing patterns in iatrogenic ureteral injuries. Rev Urol 13:e179–e183
Sawkar HP, Kim DY, Thum DJ, Zhao L, Cashy J, Bjurlin M, Bhalani V, Boller A-M, Kundu S (2014) Frequency of lower urinary tract injury after gastrointestinal surgery in the nationwide inpatient sample database. Am Surg 80:1216–1221. https://doi.org/10.1016/j.juro.2011.02.2662
Zafar SN, Ahaghotu CA, Libuit L, Ortega G, Coleman PW, Cornwell EE, Tran DD, Fullum TM (2014) Ureteral injury after laparoscopic versus open colectomy. JSLS J Soc Laparoendosc Surg 18(e2014):00158. https://doi.org/10.4293/jsls.2014.00158
Kang CY, Chaudhry OO, Halabi WJ, Nguyen V, Carmichael JC, Stamos MJ, Mills S (2012) Outcomes of laparoscopic colorectal surgery: data from the Nationwide Inpatient Sample 2009. Am J Surg 204:952–957. https://doi.org/10.1016/j.amjsurg.2012.07.031
Frankman EA, Wang L, Bunker CH, Lowder JL (2010) Lower urinary tract injury in women in the United States, 1979–2006. Am J Obstet Gynecol 202:495.e1–495.e5. https://doi.org/10.1016/j.ajog.2010.01.013
Simon KL, Frelich MJ, Gould JC, Zhao HS, Szabo A, Goldblatt MI (2015) Inpatient outcomes after elective versus nonelective ventral hernia repair. J Surg Res 198:305–310. https://doi.org/10.1016/j.jss.2015.03.073
Lapar DJ, Bhamidipati CM, Mery CM, Stukenborg GJ, Jones DR, Schirmer BD, Kron IL, Ailawadi G (2010) Primary payer status affects mortality for major surgical operations. Ann Surg 252:544–550. https://doi.org/10.1097/SLA.0b013e3181e8fd75
Steele SR, Brown TA, Rush RM, Martin MJ (2008) Laparoscopic vs open colectomy for colon cancer: results from a large nationwide population-based analysis. J Gastrointest Surg 12:583–591. https://doi.org/10.1007/s11605-007-0286-9
Guller U, Jain N, Hervey S, Purves H, Pietrobon R (2003) Laparoscopic vs open colectomy: outcomes comparison based on Large Nationwide Databases. Arch Surg 138:1179–1186. https://doi.org/10.1001/archsurg.138.11.1179
Saclarides TJ, Ko ST, Airan M, Dillon C, Franklin J (1991) Laparoscopic removal of a large colonic lipoma: report of a case. Dis Colon Rectum 34:1027–1029. https://doi.org/10.1007/BF02049970
Jeong S-Y, Park JW, Nam BH, Kim S, Kang S-B, Lim S-B, Choi HS, Kim D-W, Chang HJ, Kim DY, Jung KH, Kim T-Y, Kang GH, Chie EK, Kim SY, Sohn DK, Kim D-H, Kim J-S, Lee HS, Kim JH, Oh JH (2014) Open versus laparoscopic surgery for mid-rectal or low-rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): survival outcomes of an open-label, non-inferiority, randomised controlled trial. Lancet Oncol 15:767–774. https://doi.org/10.1016/S1470-2045(14)70205-0
van der Pas MH, Haglind E, Cuesta MA, Fürst A, Lacy AM, Hop WCJ, Bonjer HJ (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14:210–218. https://doi.org/10.1016/S1470-2045(13)70016-0
Clinical Outcomes of Surgical Therapy Study Group, Nelson H, Sargent DJ, Wieand HS, Fleshman J, Anvari M, Stryker SJ, Beart RW, Hellinger M, Flanagan R, Peters W, Ota D (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med. https://doi.org/10.1056/NEJMoa032651
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith AM, Heath RM, Brown JM (2005) Short-term endpoints of conventional versus laparoscopic-assisted surgery in patients with colorectal cancer (MRC CLASICC trial): multicentre, randomised controlled trial. Lancet 365:1718–1726. https://doi.org/10.1016/S0140-6736(05)66545-2
Lim PC, Crane JT, English EJ, Farnam RW, Garza DM, Winter ML, Rozeboom JL (2016) Multicenter analysis comparing robotic, open, laparoscopic, and vaginal hysterectomies performed by high-volume surgeons for benign indications. Int J Gynecol Obstet 133:359–364. https://doi.org/10.1016/j.ijgo.2015.11.010
Dunn MD, Portis AJ, Shalhav AL, Elbahnasy AM, Heidorn C, Mcdougall EM, Clayman RV (2000) Laparoscopic versus open radical nephrectomy: a 9-year experience. J Urol 164:1153–1159. https://doi.org/10.1016/S0022-5347(05)67131-5
Lee J, El-Tamer M, Schifftner T, Turrentine FE, Henderson WG, Khuri S, Hanks JB, Inabnet WB (2008) Open and laparoscopic adrenalectomy: analysis of the National Surgical Quality Improvement Program. J Am Coll Surg 206:953–959. https://doi.org/10.1016/j.jamcollsurg.2008.01.018
Sgourakis G, Gockel I, Radtke A, Musholt TJ, Timm S, Rink A, Tsiamis A, Karaliotas C, Lang H (2010) Minimally invasive versus open esophagectomy: meta-analysis of outcomes. Dig Dis Sci 55:3031–3040
Trastulli S, Cirocchi R, Desiderio J, Coratti A, Guarino S, Renzi C, Corsi A, Boselli C, Santoro A, Minelli L, Parisi A (2015) Robotic versus laparoscopic approach in colonic resections for cancer and benign diseases: systematic review and meta-analysis. PLoS ONE 10:e0134062. https://doi.org/10.1371/journal.pone.0134062
Schootman M, Hendren S, Ratnapradipa K, Stringer L, Davidson NO (2016) Adoption of robotic technology for treating colorectal cancer. Dis Colon Rectum 59:1011–1018. https://doi.org/10.1097/DCR.0000000000000688
Eswara JR, Raup VT, Potretzke AM, Hunt SR, Brandes SB (2015) Outcomes of iatrogenic genitourinary Injuries during colorectal surgery. Urology 86:1228–1234. https://doi.org/10.1016/j.urology.2015.06.065
Althumairi AA, Efron JE (2016) Genitourinary considerations in reoperative and complex colorectal surgery. Clin Colon Rectal Surg 29:145–151. https://doi.org/10.1055/s-0036-1580629
Willett CG (2018) Management of locoregional rectal cancer. J Natl Compr Cancer Netw 16:617–619. https://doi.org/10.6004/jnccn.2018.0037
Nfonsam V, Aziz H, Pandit V, Khalil M, Jandova J, Joseph B (2016) Analyzing clinical outcomes in laparoscopic right vs. left colectomy in colon cancer patients using the NSQIP database. Cancer Treat Commun 8:1–4. https://doi.org/10.1016/j.ctrc.2016.03.006
Riss S, Mittlböck M, Riss K, Chitsabesan P, Stift A (2014) Intraoperative complications have a negative impact on postoperative outcomes after rectal cancer surgery. Int J Surg 12:833–836. https://doi.org/10.1016/j.ijsu.2014.07.003
American Medical Association (2014) Preparing for the ICD-10 Code Set: October 1, 2015 Compliance Date. https://www.ama-assn.org/sites/ama-assn.org/files/corp/media-browser/premium/washington/icd10-icd9-differences-fact-sheet_0.pdf. Accessed 25 June 2019
Rubenstein J (2016) ICD-10 Changes for october 1, 2016 of interest to urologists. Rev Urol 18:110–113. https://doi.org/10.3909/riu0718
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Mayo, Brazer, Bogenberger, Tavares, Conrad, Gillern, Park, Richards, and Mr. Lustik have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Disclaimer
The views expressed in this abstract/manuscript are those of the author(s) and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
Rights and permissions
About this article
Cite this article
Mayo, J.S., Brazer, M.L., Bogenberger, K.J. et al. Ureteral injuries in colorectal surgery and the impact of laparoscopic and robotic-assisted approaches. Surg Endosc 35, 2805–2816 (2021). https://doi.org/10.1007/s00464-020-07714-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07714-1