Abstract
Background
Few studies have investigated the potential impact of robotic assistance on cognitive ergonomics during advanced minimally invasive surgery. The purpose of this study was to assess the impact of robotic assistance on mental workload and downstream cognitive performance in surgical trainees.
Methods
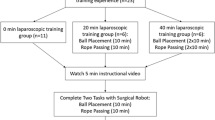
Robot-naïve trainees from general surgery, urology and gynaecology, stratified by specialty and level of training, were randomised to either laparoscopic surgery (LS) or robotic-assisted laparoscopic surgery (RALS) and performed a time-limited, complex laparoscopic suturing task after watching a 5-min instructional video. The RALS group received an additional 5-min orientation to the robotic console. Subjective mental workload was measured using NASA Task Load Index. Concentration and executive cognitive function were assessed using Psychomotor Vigilance Task (PVT) and Wisconsin Card Sorting Test (WCST), respectively. A p value of 0.05 was considered significant.
Results
Sixteen senior residents (SR; ≥ PGY3) and 14 junior residents (JR; PGY1-2) completed the study. There was no difference in mental workload between LS and RALS. Within JR there was no difference in task completion time comparing LS versus RALS; however, LS was associated with impaired concentration post-task versus pre-task (PVT reaction time 306 versus 324 ms, p = 0.03), which was not observed for RALS. In contrast, amongst SR, RALS took significantly longer than LS (10.3 vs. 14.5 min, p = 0.02) and was associated with significantly worse performance on WCST (p < 0.01).
Conclusions
Robotic assistance, in this setting, did not provide a technical performance advantage nor impact subjective mental workload with novice users regardless of level of surgery training. We observed a protective effect on cognitive performance offered by RALS to junior trainees with limited LS experience, yet a detrimental effect on senior trainees with greater LS ability and inadequate pre-study robotic training, suggesting that robotic consoles may be mentally taxing for robotic novices and consideration should be given to formal console training prior to initial clinical exposure.
Graphic abstract



Similar content being viewed by others
References
Park A, Lee G, Seagull FJ, Meenaghan N, Dexter D (2010) Patients benefit while surgeons suffer: an impending epidemic. J Am Coll Surg 210:306–313. https://doi.org/10.1016/j.jamcollsurg.2009.10.017
Carswell CM, Clarke D, Seales WB (2005) Assessing mental workload during laparoscopic surgery. Surg Innov 12:80–90
Heemskerk J, Zandbergen HR, Keet SWM, Martijnse I, van Montfort G, Peters RJA, Svircevic V, Bouwman RA, Baeten CGMI, Bouvy ND (2014) Relax, it’s just laparoscopy! A prospective randomized trial on heart rate variability of the surgeon in robot-assisted versus conventional laparoscopic cholecystectomy. Dig Surg 31:225–232. https://doi.org/10.1159/000365580
Guru KA, Esfahani ET, Raza SJ, Bhat R, Wang K, Hammond Y, Wilding G, Peabody JO, Chowriappa AJ (2015) Cognitive skills assessment during robot-assisted surgery: separating the wheat from the chaff. BJU Int 115:166–174. https://doi.org/10.1111/bju.12657
Yurko YY, Scerbo MW, Prabhu AS, Acker CE, Stefanidis D (2010) Higher mental workload is associated with poorer laparoscopic performance as measured by the NASA-TLX tool. Simul Healthc J Soc Simul Healthc 5:267–271. https://doi.org/10.1097/SIH.0b013e3181e3f329
Zheng B, Jiang X, Tien G, Meneghetti A, Panton ONM, Atkins MS (2012) Workload assessment of surgeons: correlation between NASA TLX and blinks. Surg Endosc 26:2746–2750. https://doi.org/10.1007/s00464-012-2268-6
Berguer R, Smith W (2006) An ergonomic comparison of robotic and laparoscopic technique: the influence of surgeon experience and task complexity. J Surg Res 134:87–92. https://doi.org/10.1016/j.jss.2005.10.003
Klein MI, Warm JS, Riley MA, Matthews G, Doarn C, Donovan JF, Gaitonde K (2012) Mental workload and stress perceived by novice operators in the laparoscopic and robotic minimally invasive surgical interfaces. J Endourol Endourol Soc 26:1089–1094. https://doi.org/10.1089/end.2011.0641
Stefanidis D, Wang F, Korndorffer JR, Dunne JB, Scott DJ (2010) Robotic assistance improves intracorporeal suturing performance and safety in the operating room while decreasing operator workload. Surg Endosc 24:377–382. https://doi.org/10.1007/s00464-009-0578-0
Boksem MAS, Meijman TF, Lorist MM (2005) Effects of mental fatigue on attention: an ERP study. Brain Res Cogn Brain Res 25:107–116. https://doi.org/10.1016/j.cogbrainres.2005.04.011
van der Linden D, Frese M, Meijman TF (2003) Mental fatigue and the control of cognitive processes: effects on perseveration and planning. Acta Psychol (Amst) 113:45–65
Young G, Zavelina L, Hooper V (2008) Assessment of workload using NASA Task Load Index in perianesthesia nursing. J Perianesthesia Nurs 23:102–110. https://doi.org/10.1016/j.jopan.2008.01.008
Mueller ST, Piper BJ (2014) The psychology experiment building language (PEBL) and PEBL test battery. J Neurosci Methods 222:250–259. https://doi.org/10.1016/j.jneumeth.2013.10.024
Marecik SJ, Chaudhry V, Jan A, Pearl RK, Park JJ, Prasad LM (2007) A comparison of robotic, laparoscopic, and hand-sewn intestinal sutured anastomoses performed by residents. Am J Surg 193:349–355. https://doi.org/10.1016/j.amjsurg.2006.09.018discussion 355
Panait L, Shetty S, Shewokis PA, Sanchez JA (2014) Do laparoscopic skills transfer to robotic surgery? J Surg Res 187:53–58. https://doi.org/10.1016/j.jss.2013.10.014
Chang L, Satava RM, Pellegrini CA, Sinanan MN (2003) Robotic surgery: identifying the learning curve through objective measurement of skill. Surg Endosc 17:1744–1748. https://doi.org/10.1007/s00464-003-8813-6
Stefanidis D, Hope WW, Scott DJ (2011) Robotic suturing on the FLS model possesses construct validity, is less physically demanding, and is favored by more surgeons compared with laparoscopy. Surg Endosc 25:2141–2146. https://doi.org/10.1007/s00464-010-1512-1
Ruurda JP, Broeders IA, Pulles B, Kappelhof FM, van der Werken C (2004) Manual robot assisted endoscopic suturing: time-action analysis in an experimental model. Surg Endosc 18:1249–1252. https://doi.org/10.1007/s00464-003-9191-9
Lee GI, Lee MR, Clanton T, Clanton T, Sutton E, Park AE, Marohn MR (2014) Comparative assessment of physical and cognitive ergonomics associated with robotic and traditional laparoscopic surgeries. Surg Endosc 28:456–465. https://doi.org/10.1007/s00464-013-3213-z
Engelmann C, Schneider M, Kirschbaum C, Grote G, Dingemann J, Schoof S, Ure BM (2011) Effects of intraoperative breaks on mental and somatic operator fatigue: a randomized clinical trial. Surg Endosc 25:1245–1250. https://doi.org/10.1007/s00464-010-1350-1
Gerdes J, Kahol K, Smith M, Leyba MJ, Ferrara JJ (2008) Jack Barney award: the effect of fatigue on cognitive and psychomotor skills of trauma residents and attending surgeons. Am J Surg 196:813–819. https://doi.org/10.1016/j.amjsurg.2008.07.030discussion 819–820
Balkin TJ, Bliese PD, Belenky G, Sing H, Thorne DR, Thomas M, Redmond DP, Russo M, Wesensten NJ (2004) Comparative utility of instruments for monitoring sleepiness-related performance decrements in the operational environment. J Sleep Res 13:219–227. https://doi.org/10.1111/j.1365-2869.2004.00407.x
Barceló F, Knight RT (2002) Both random and perseverative errors underlie WCST deficits in prefrontal patients. Neuropsychologia 40:349–356
Funding
This study was funded by Schulich School of Medicine and Dentistry.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Schlachta has no proprietary interest in the technologies studied, but has received honoraria from Ethicon (advisory, education support), Minogue Medical (proctoring), Stryker (speaking), Novadaq (advisory) and Verb (advisory). Drs. Lau and Alkhamesi have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lau, E., Alkhamesi, N.A. & Schlachta, C.M. Impact of robotic assistance on mental workload and cognitive performance of surgical trainees performing a complex minimally invasive suturing task. Surg Endosc 34, 2551–2559 (2020). https://doi.org/10.1007/s00464-019-07038-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07038-9