Abstract
Introduction
Atherosclerotic cardiovascular disease (ASCVD) and Framingham risk scores (FRS) are used to calculate 10-year risk of coronary death, nonfatal myocardial infarction, or fatal/nonfatal stroke. Our goal is to evaluate the association between preoperative cardiovascular risk and weight loss.
Methods
We retrospectively reviewed bariatric surgeries from 2010 to 2016. Patients who met criteria for calculating 10-year ASCVD score and FRS were included. Data collected included baseline demographics, perioperative parameters, and postoperative outcomes at 12 months. Simple linear regression and multiple linear regression models were applied to test influence of individual or multiple factors of interest on 12-month weight loss outcomes.
Results
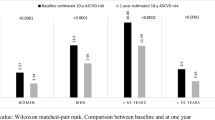
Of 1330 bariatric patients studied, 360 patients met criteria for ASCVD and FRS calculation. Sleeve gastrectomy (LSG) was the most prevalent surgery 63.05%, followed by Roux-en-Y gastric bypass (LRYGB) 20.55%, revision procedures 11.9%, and adjustable gastric banding (LAGB) 4.4%. Initial BMI was 42.71 ± 7.85 kg/m2 for females and 42.72k ± 7.42 kg/m2 for males, with a 12-month percentage of estimated BMI loss (%EBMIL) of 66.51% in females and 60.29% in males. Preoperative 10-year ASCVD score was higher in males than females with a 34.73% relative risk reduction (RRR) in males and 35.3% RRR in females at 12-month follow-up. Regarding FRS, preoperative risk was 33.13 ± 21.1% in males and 15.71 ± 14.52% in females, with an RRR of 25.8% in males and 32.2% in females. Univariate analysis of preoperative FRS and %EBMIL showed that for every percentage unit increase in the patient’s preoperative FRS, %EBMIL decreases 0.31 percentile unit (P < 0.001). Furthermore, preoperative ASCVD score is also significantly associated with %EMBIL—for every percentage unit increase in preoperative ASCVD score, %EBMIL decreases 0.42 percentile credits.
Conclusion
Study results suggest ASCVD and FRS are equally reduced after bariatric surgery, especially after LSG and LRYGB. Moreover, preoperative FRS and ASCVD risk score showed an inversely proportional relationship with %EBMIL loss at 12 months.
Similar content being viewed by others
References
Reges O, Greenland P, Dicker D, Leibowitz M, Hoshen M, Gofer I, Rasmussen-Torvik LJ, Balicer RD (2018) Association of bariatric surgery using laparoscopic banding, Roux-en-Y gastric bypass, or laparoscopic sleeve gastrectomy vs usual care obesity management with all-cause mortality. JAMA 319:279–290. https://doi.org/10.1001/jama.2017.20513
World Health Organization (WHO) (2000) Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Org Tech Rep Ser 894(i–xii):1–253
Thaler JP, Cummings DE (2009) Minireview: hormonal and metabolic mechanisms of diabetes remission after gastrointestinal surgery. Endocrinology 150:2518–2525. https://doi.org/10.1210/en.2009-0367
Aminian A, Brethauer SA, Andalib A, Punchai S, Mackey J, Rodriguez J, Rogula T, Kroh M, Schauer PR (2016) Can sleeve gastrectomy “cure” diabetes? Long-term metabolic effects of sleeve gastrectomy in patients with type 2 diabetes. Ann Surg 264:674–681. https://doi.org/10.1097/SLA.0000000000001857
Bays H, Kothari SN, Azagury DE, Morton JM, Nguyen NT, Jones PH, Jacobson TA, Cohen DE, Orringer C, Westman EC, Horn DB, Scinta W, Primack C (2016) Lipids and bariatric procedures part 2 of 2: scientific statement from the American Society for Metabolic and Bariatric Surgery (ASMBS), the National Lipid Association (NLA), and Obesity Medicine Association (OMA). Surg Obes Relat Dis 12:468–495. https://doi.org/10.1016/j.soard.2016.01.007
Schauer PR, Bhatt DL, Kirwan JP, Wolski K, Aminian A, Brethauer SA et al (2017) Bariatric surgery versus intensive medical therapy for diabetes—5-year outcomes. N Engl J Med 376:641–651. https://doi.org/10.1056/NEJMoa1600869
Cappellani A, Di Vita M, Zanghi A, Cavallaro A, Piccolo G, Veroux M, Berretta M, Malaguarnera M, Canzonieri V, Lo Menzo E (2012) Diet, obesity and breast cancer: an update. Front Biosci 4:90–108
Auclair A, Biertho L, Marceau S, Hould FS, Biron S, Lebel S, Julien F, Lescelleur O, Lacasse Y, Piché ME, Cianflone K, Parlee SD, Goralski K, Martin J, Bastien M, St-Pierre DH, Poirier P (2017) Bariatric surgery-induced resolution of hypertension and obstructive sleep apnea: impact of modulation of body fat, ectopic fat, autonomic nervous activity, inflammatory and adipokine profiles. Obes Surg. https://doi.org/10.1007/s11695-017-2737-z
Arterburn D, Schauer DP, Wise RE, Gersin KS, Fischer DR, Selwyn CA, Erisman A, Tsevat J (2009) Change in predicted 10-year cardiovascular risk following laparoscopic roux-en-Y gastric bypass surgery. Obes Surg 19:184–189. https://doi.org/10.1007/s11695-008-9534-7
Gutierrez-Blanco D, Funes-Romero D, Madiraju S, Perez-Quirante F, Lo Menzo E, Szomstein S, Rosenthal RJ (2017) Reduction of Framingham BMI score after rapid weight loss in severely obese subjects undergoing sleeve gastrectomy: a single institution experience. Surg Endosc Other Interv Tech. https://doi.org/10.1007/s00464-017-5799-z
van de Laar A (2012) Bariatric outcomes longitudinal database (BOLD) suggests excess weight loss and excess BMI loss to be inappropriate outcome measures, demonstrating better alternatives. Obes Surg 22:1843–1847. https://doi.org/10.1007/s11695-012-0736-7
Peterli R, Wölnerhanssen BK, Peters T, Vetter D, Kröll D, Borbély Y, Schultes B, Beglinger C, Drewe J, Schiesser M, Nett P, Bueter M (2018) Effect of laparoscopic sleeve gastrectomy vs laparoscopic Roux-en-Y gastric bypass on weight loss in patients with morbid obesity. JAMA 319:255. https://doi.org/10.1001/jama.2017.20897
Salminen P, Helmiö M, Ovaska J, Juuti A, Leivonen M, Peromaa-Haavisto P, Hurme S, Soinio M, Nuutila P, Victorzon M (2018) Effect of laparoscopic sleeve gastrectomy vs laparoscopic Roux-en-Y gastric bypass on weight loss at 5 years among patients with morbid obesity. JAMA 319:241. https://doi.org/10.1001/jama.2017.20313
Brethauer SA, Kim J, Chaar M, El Papasavas P, Eisenberg D, Rogers A, Ballem N, Kligman M, Kothari S (2015) Standardized outcomes reporting in metabolic and bariatric surgery. Surg Obes Relat Dis 11:489–506. https://doi.org/10.1016/j.soard.2015.02.003
D’Agostino RB, Vasan RS, Pencina MJ, Wolf PA, Cobain M, Massaro JM, Kannel WB (2008) General cardiovascular risk profile for use in primary care: the Framingham heart study. Circulation 117:743–753. https://doi.org/10.1161/CIRCULATIONAHA.107.699579
Eckel RH, Jakicic JM, Ard JD, De Jesus JM, Houston Miller N, Hubbard VS, Lee IM, Lichtenstein AH, Loria CM, Millen BE, Nonas CA, Sacks FM, Smith SC, Svetkey LP, Wadden TA, Yanovski SZ (2014) 2013 AHA/ACC guideline on lifestyle management to reduce cardiovascular risk: a report of the American College of cardiology/American Heart Association task force on practice guidelines. Circulation. https://doi.org/10.1161/01.cir.0000437740.48606.d1
Ponce J, DeMaria EJ, Nguyen NT, Hutter M, Sudan R, Morton JM (2016) American Society for Metabolic and Bariatric Surgery estimation of bariatric surgery procedures in 2015 and surgeon workforce in the United States. Surg Obes Relat Dis 12:1637–1639. https://doi.org/10.1016/j.soard.2016.08.488
ASMBS (2014) Estimate of bariatric surgery numbers. AsmbsOrg 1
Perrone F, Bianciardi E, Benavoli D, Tognoni V, Niolu C, Siracusano A, Gaspari AL, Gentileschi P (2016) Gender influence on long-term weight loss and comorbidities after laparoscopic sleeve gastrectomy and Roux-en-Y gastric bypass: a prospective study with a 5-year follow-up. Obes Surg 26:276–281. https://doi.org/10.1007/s11695-015-1746-z
Bays H, Kothari SN, Azagury DE, Morton JM, Nguyen NT, Jones PH, Jacobson TA, Cohen DE, Orringer C, Westman EC, Horn DB, Scinta W, Primack C (2016) Lipids and bariatric procedures Part 1 of 2: Scientific statement from the American Society for Metabolic and Bariatric Surgery (ASMBS), the National Lipid Association (NLA), and Obesity Medicine Association (OMA). Surg Obes Relat Dis 12:468–495. https://doi.org/10.1016/j.soard.2016.01.007
Schiavon CA, Bersch-Ferreira AC, Santucci EV, Oliveira JD, Torreglosa CR, Bueno PT, Frayha JC, Santos RN, Damian LP, Noujaim PM, Halpern H, Monteiro FLJ, Cohen RV, Uchoa CH, de Souza MG, Amodeo C, Bortolotto L, Ikeoka D, Drager LF, Cavalcanti AB, Berwanger O (2017) Effects of bariatric surgery in obese patients with hypertension: the GATEWAY randomized trial (gastric bypass to treat obese patients with steady hypertension). Circulation. https://doi.org/10.1161/CIRCULATIONAHA.117.032130
Romdhane H, Ebrahim S, Escobar C, Gueyffier F, Jackson R, Keil U, Lim S, Lindholm L, Snehalatha C (2007) Prevention of cardiovascular disease: guidelines for assessment and managment of cardiovascular risk. World Health Org. www.who.int/cardiovascular_diseases/guidelines/Full%20text.pdf
Donadelli SP, Salgado W, Marchini JS, Schmidt A, Amato CAF, Ceneviva R, Dos Santos JE, Nonino CB (2011) Change in predicted 10-year cardiovascular risk following Roux-en-Y gastric bypass surgery. Who benefits? Obes Surg 21:569–573. https://doi.org/10.1007/s11695-010-0348-z
Bastos ECL, Barbosa EMWG, Soriano GMS, dos Santos EA, Vasconcelos SML, Santos EA, Dos (2013) Determinants of weight regain after bariatric surgery. Arq Bras Cir Dig 26(Suppl 1):26–32
Odom J, Zalesin KC, Washington TL, Miller WW, Hakmeh B, Zaremba DL, Altattan M, Balasubramaniam M, Gibbs DS, Krause KR, Chengelis DL, Franklin BA, McCullough PA (2010) Behavioral predictors of weight regain after bariatric surgery. Obes Surg 20:349–356. https://doi.org/10.1007/s11695-009-9895-6
Reinhold RB (1982) Critical analysis of long term weight loss following gastric bypass. Surg Gynecol Obstet 155:385–394
Colquitt JL, Pickett K, Loveman E, Frampton GK (2014) Surgery for weight loss in adults. Cochrane Database Syst Rev 8:CD003641. https://doi.org/10.1002/14651858.CD003641.pub4
Daigle CR, Andalib A, Corcelles R, Cetin D, Schauer PR, Brethauer SA (2015) Bariatric and metabolic outcomes in the super-obese elderly. Surg Obes Relat Dis. https://doi.org/10.1016/j.soard.2015.04.006
Giordano S, Victorzon M (2015) Bariatric surgery in elderly patients: a systematic review. Clin Interv Aging 10:1627–1635. https://doi.org/10.2147/CIA.S70313
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
David Gutierrez Blanco, David Romero Funes, Giulio Giambartolomei, Emanuele Lo Menzo Samuel Szomstein, and Raul J. Rosenthal have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Blanco, D.G., Funes, D.R., Giambartolomei, G. et al. High cardiovascular risk patients benefit more from bariatric surgery than low cardiovascular risk patients. Surg Endosc 33, 1626–1631 (2019). https://doi.org/10.1007/s00464-018-6437-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-018-6437-0