Abstract
Introduction
Several reports highlight bariatric surgery as an efficient and long-lasting strategy for weight loss. Herein, we aimed to evaluate the impact of bariatric surgery on 10-year cardiovascular disease (CVD) risk and to compare the effectiveness of different surgical procedures, employing the Framingham Risk Score (FRS).
Methods
Retrospective longitudinal observational study of patients undergoing bariatric surgery. Data was assessed preoperatively and during a 4-year follow-up period.
Results
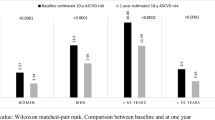
We evaluated 1449 individuals, 85.2% female, age of 42.4 ± 10.6 years, and preoperative BMI of 44.3 ± 5.8 kg/m2; 58.0% underwent Roux-en-Y gastric bypass (RYGB), 23.4% sleeve gastrectomy (SG), and 18.6% adjustable gastric band (AGB). The 10-year CVD risk decreased 43.6% in the first postoperative year. The decrease in FRS was more pronounced in the RYGB group (50.5% in the first postoperative year) (p < 0.001). Although there was a subsequent slight increase in FRS during the follow-up period, the cardiovascular benefits were maintained when compared with baseline. For all surgical procedures, CVD risk showed a quadratic trend with a J-shaped curve. A negative interaction between the RYGB group CVD risk and time was observed (β = − 0.072 (95% CI, − 0.109; − 0.035)). In the RYGB group, FRS decreased more when compared with the SG and AGB groups and, from the second postoperative year onwards, increased more slowly, regardless of gender. The SG group showed similar trend as that of the AGB (β = − 0.002 (95% CI, − 0.049; 0.053)).
Conclusion
Our study showed a significant reduction of 10-year CVD risk after bariatric surgery. This decrease was more pronounced in the first postoperative year, and RYGB was the procedure with the greatest decrease of the 10-year CVD risk.

Similar content being viewed by others
References
Muniesa PG, González MA, Martinez JA, et al. Obesity. Nat Rev Dis Primers. 2017;3:17034.
Finkelstein EA. How big of a problem is obesity? Surg Obes Relat Dis. 2014;10:569–70.
Sidney S, Quesenberry C, Jaffe M, et al. Recent trends in cardiovascular mortality in the United States and puplic health goals. JAMA Cardiol. 2016;1:584–99.
Koliaki C, Liatis S, Kokkinos A. Obesity and cardiovascular disease: revisiting an old relationship. Metabolism. 2019;92:98–107.
Boido A, Ceriani V, Cetta F, et al. Bariatric surgery and prevention of cardiovascular events and mortality in morbid obesity: mechanisms of action and choice of surgery. Nutr Metab Cardiovasc Dis. 2015;25(5):437–43.
Nyberg ST, Batty GD, Pentti J, et al. Obesity and loss of disease-free years owing to major non-communicable diseases: a multicohort study. Lancet Public Health. 2018;3(10):e490–7.
Riaz H, Khan MS, Siddiqi TJ, et al. Association between obesity and cardiovascular outcomes: a systematic review and meta-analysis of Mendelian randomization studies. JAMA Netw Open. 2018;1(7):e183788.
Benotti PN, Wood GC, Carey DJ, et al. Gastric bypass surgery produces a durable reduction in cardiovascular disease and reduces the long-term risks of congestive heart failure. JAHA. 2017:e005126.
Park JY, Kim YJ. Laparoscopic gastric bypass vs sleeve gastrectomy in obese Korean patients. World J Gastrenterol. 2015;21(44):12612–9.
Maciejewski ML, Arterburn DE, Scoyoc LV, et al. Bariatric surgery and long-term durability of weight loss. JAMA Surg. 2016;151(11):1046–55.
Magouliotis DE, Tasiopoulou VS, Sioka E, et al. Impact of bariatric surgery on metabolic and gut microbiota profile: a systematic review and meta-analysis. Obes Surg. 2017;27(5):1345–57.
D’Agostino RB, Vasan RS, Pencina MJ, et al. General cardiovascular risk profile for use in primary care: the Framingham Heart Study. Circulation. 2008;117:743–53.
Scott J, Johnson B, Blackhurst D, et al. Does bariatric surgery reduce the risk of major cardiovascular events? A retrospective cohort study of morbidly obese surgical patients. Surg Obes Relat Dis. 2013;9:32–41.
Sjostrom L, Peltonen M, Jacobson P, et al. Bariatric surgery and long-term cardiovascular events. JAMA. 2012;307:56–65.
Johnson B, Blackhurst D, Latham B, et al. Bariatric surgery is associated with a reduction in major macrovascular complications in moderately to severely obese patients with type 2 diabetes mellitus. J Am Coll Surg. 2013;216:545–58.
Borhanuddin B, Nawi AM, Shah SA, et al. 10-year cardiovascular disease risk estimation based on lipid profile-based and BMI-based Framingham Risk Scores across multiple sociodemographic characteristics: the Malayasian Cohort Project. Sci World J. 2018;2018:2979206.
Metcalf PA, Wells S, Jackson RT. Assessing 10-year coronary heart disease risk in people with Type 2 diabetes mellitus: Framingham versus United Kingdom prospective diabetes study. JDM. 2014;4(1):12–8.
Carlin AM, Zeni TM, English WJ, et al. Michigan Bariatric Surgery Collaborative. The comparative effectiveness of sleeve gastrectomy, gastric bypass, and adjustable gastric banding procedures for the treatment of morbid obesity. Ann Surg. 2013;257(5):791–7.
Chang SH, Stoll CR, Song J, et al. The effectiveness and risks of bariatric surgery: an updated systematic review and meta-analysis, 2003-2012. JAMA Surg. 2014;149:275–87.
Domienik-Karlowicz J, Rymarczyk Z, Dzikowska-Diduch O, et al. Emerging markers of atherosclerosis before and after bariatric surgery. Obes Surg. 2015;25:486–93.
Nerla R, Tarzia P, Sestito A, et al. Effect of bariatric surgery on peripheral flow- mediated dilatation and coronary microvacular function. Nutr Metab Cardiovasc Dis. 2012;22:626–34.
Hafida S, Mirshahi T, Nikolajczyk B. The impact of bariatric surgery on inflammation: quenching the fire of obesity. Curr Opin Endocrinol Diabetes Obes. 2016;23:373–8.
Bigornia S, Mott M, Hess D, et al. Long-term successful weight loss improves vascular endothelial function in severely obese individuals. Obesity (Silver Spring). 2010;18:754–9.
Osto E, Doytcheva P, Corteville C, et al. Rapid and body weight-independent improvement of endothelial and high-density lipoprotein function after Roux-en-Y gastric bypass. Role of glucagon-like peptide-1. Circulation. 2015;131:871–81.
Heffron SP, Parikh A, Volodarskiy A, et al. Changes in lipid profile of obese patients following contemporary bariatric surgery: a meta-analysis. Am J Med. 2016;129(9):952–9.
Benraoune F, Litwin SE. Reductions in cardiovascular risk after bariatric surgery. Curr Opin Cardiol. 2011;26(6):555–61.
Owen JG, Yazdi F, Reisin E. Bariatric surgery and hypertension. Am J Hypertens. 2018;31(1):11–7.
Zhang C, Yuan Y, Qiu C, et al. A meta-analysis of 2-year effect after surgery: laparoscopic Roux-en-y gastric bypass versus laparoscopic sleeve gastrectomy for morbid obesity and diabetes mellitus. Obes Surg. 2014;24:1528–35.
Souteiro P, Belo S, Magalhães D, et al. Long-term diabetes outcomes after bariatric surgery – managing medication withdrawal. Int J Obes. 2019:1–8. https://doi.org/10.1038/s41366-019-0320-5.
Ikramuddin S, Korner J, Lee WJ, et al. Roux-en-Y gastric bypass vs intensive medical management for the control of type 2 diabetes, hypertension, and hyperlipidemia: the Diabetes Surgery Study randomized clinical trial. JAMA. 2013;309:2240–9.
Laferrère B, Reilly D, Arias S, et al. Differential metabolic impact of gastric bypass surgery versus dietary intervention in obese diabetic subjects despite identical weight loss. Sci Transl Med. 2011;3:80re2.
Plum L, Ahmed L, Febres G, et al. Comparison of glucostatic parameters after hypo- caloric diet or bariatric surgery and equivalent weight loss. Obesity (Silver Spring). 2011;19:2149–57.
Quercia I, Dutia R, Kotler DP, et al. Gastrointestinal changes after bariatric surgery. Diabetes Metab. 2014;40:87–94.
Acknowledgments
We would like to acknowledge all the endocrinologists, surgeons, and nutritionists of the Multidisciplinary Group for Surgical Management of Obesity.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Ethical Approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
For this type of study, formal consent is not required.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Oliveira, S.C., Neves, J.S., Souteiro, P. et al. Impact of Bariatric Surgery on Long-term Cardiovascular Risk: Comparative Effectiveness of Different Surgical Procedures. OBES SURG 30, 673–680 (2020). https://doi.org/10.1007/s11695-019-04237-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-04237-0