Abstract
Background
Published support exists for using lightweight polypropylene mesh (PPM) to repair inguinal hernias with increased biocompatibility and decreased foreign body reaction and pain. However, quality of life (QOL) has not been assessed. We assess QOL in patients undergoing laparoscopic totally extraperitoneal hernia repair (TEP) with lightweight PPM.
Methods
We performed an IRB-approved study of patients undergoing TEP hernia repair. Demographic information and hernia characteristics were collected perioperatively. Baseline Short Form-36 (SF-36), Carolinas Comfort Scale (CCS), and visual analog scale (VAS) for pain were performed preoperatively, and then after 1, 26, and 52 weeks.
Results
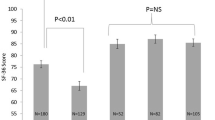
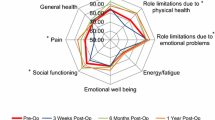
Forty-eight patients undergoing TEP with mesh were selected. Average age was 43.2 years (SD = 13.2), and average BMI was 26.1 kg/m2 (SD = 4.3). Procedures include bilateral hernia, right inguinal hernia, and left inguinal hernia repairs. Mean scores on the CCS® and VAS were low during the immediate post-op period and 1 year. SF-36 mean scores for body pain, physical function, and role physical showed decreases at the postoperative survey and then subsequent increases. Pain-associated scores increased during the immediate post-op period. CCS and SF-36 scores demonstrated improvement after 1 year. There was no significant difference in VAS. Bilateral repair patients reported more pain and reduced physical function versus unilateral repairs. Patients with larger mesh reported greater pain scores and reduced physical function scores.
Conclusions
Laparoscopic inguinal hernia repair is associated with initial declines in QOL in the postoperative period. Improvements appear in the long term. General health does not appear to be impacted by laparoscopic TEP. Smaller mesh and unilateral repairs are associated with improved QOL following laparoscopic TEP with PPM. Multiple metrics for QOL are required to reflect patient recovery.



Similar content being viewed by others
References
Klosterhalfen B, Klinge U (2013) Retrieval study at 623 human mesh explants made of polypropylene-impact of mesh class and indication for mesh removal on tissue reaction. J Biomed Mater Res Part B 101B:1393–1399
Schopf S, von Ahnen T, von Ahnen M, Schardey H (2011) Chronic pain after laparoscopic transabdominal preperitoneal hernia repair: a randomized comparison of light and extralight titanized polypropylene mesh. World J Surg 35(2):302–310. doi:10.1007/s00268-010-0850-4
Tamme C, Scheidbach H, Hampe C, Schneider C, Köckerling F (2003) Totally extraperitoneal endoscopic inguinal hernia repair (TEP). Surgical Endoscopy and Other Interventional Techniques 17(2):190–195
Gholghesaei M, Langeveld HR, Veldkamp R, Bonjer HJ (2005) Costs and quality of life after endoscopic repair of inguinal hernia vs open tension-free repair: a review. Surg Endosc 19:816–821
Bower C, Hazey JW, Jones EL, Perry KA, Davenport DL, Roth JS (2014) Laparoscopic inguinal hernia repair with a novel hernia mesh incorporating a nitinol alloy frame compared with a standard lightweight polypropylene mesh. Surg Innov. doi:10.1177/1553350614557594
Rutkow IM (1997) Surgical operations in the United States: then (1983) and now (1994). Arch Surg 132(9):983–990
Horstmann R, Hellwig M, Classen C, Röttgermann S, Palmes D (2006) Impact of polypropylene amount on functional outcome and quality of life after inguinal hernia repair by the TAPP procedure using pure, mixed, and titanium-coated meshes. World J Surg 30(9):1742–1749
Agarwal BB, Agarwal KA, Sahu T, Mahajan KC (2010) Traditional polypropylene and lightweight meshes in totally extraperitoneal inguinal herniorrhaphy. Int J Surg 8(1):44–47
Harrell AG, Novitsky YW, Cristiano JA, Gersin KS, Norton HJ, Kercher KW, Heniford BT (2007) Prospective histologic evaluation of intra-abdominal prosthetics four months after implantation in a rabbit model. Surg Endosc 21(7):1170–1174
Li J, Ji Z, Cheng T (2012) Lightweight versus heavyweight in inguinal hernia repair: a meta-analysis. Hernia 16(5):529–539
Weyhe D, Belyaev O, Müller C, Meurer K, Bauer KH, Papapostolou G, Uhl W (2007) Improving outcomes in hernia repair by the use of light meshes—a comparison of different implant constructions based on a critical appraisal of the literature. World J Surg 31(1):234–244
Myers E, Browne KM, Kavanagh DO, Hurley M (2010) Laparoscopic (TEP) versus Lichtenstein inguinal hernia repair: a comparison of quality-of-life outcomes. World J Surg 34(12):3059–3064
Lau H, Patil NG (2004) Acute pain after endoscopic totally extraperitoneal (TEP) inguinal hernioplasty: multivariate analysis of predictive factors. Surg Endosc Interv Tech 18(1):92–96
Lawrence K, McWhinnie D, Goodwin A, Doll H, Gordon A, Gray A et al (1995) Randomised controlled trial of laparoscopic versus open repair of inguinal hernia: early results. BMJ 311:981
Fitzgibbons RJ Jr, Giobbie-Hurder A, Gibbs JO, Dunlop DD, Reda DJ, McCarthy M Jr, Neumayer LA, Barkun JS, Hoehn JL, Murphy JT, Sarosi GA Jr, Syme WC, Thompson JS, Wang J, Jonasson O (2006) Watchful waiting vs repair of inguinal hernia in minimally symptomatic men: a randomized clinical trial. JAMA 295(3):285–292
Fitzgibbons RJ Jr, Ramanan B, Arya S, Turner SA, Li X, Gibbs JO, Reda DJ (2013) Investigators of the original trial. Long-term results of a randomized controlled trial of a nonoperative strategy (watchful waiting) for men with minimally symptomatic inguinal hernias. Ann Surg 258(3):508–515
Agarwal BB, Agarwal KA, Mahajan KC (2009) Prospective double-blind randomized controlled study comparing heavy-and lightweight polypropylene mesh in totally extraperitoneal repair of inguinal hernia: early results. Surg Endosc 23(2):242–247
Dąbrowiecki S, Pierściński S, Szczęsny W (2012) Original paper the Glubran 2 glue for mesh fixation in Lichtenstein’s hernia repair: a double-blind randomized study. Videosurg Miniinvasive Tech 7(2):96–104
Taylor C, Layani L, Liew V, Ghusn M, Crampton N, White S (2008) Laparoscopic inguinal hernia repair without mesh fixation, early results of a large randomized clinical trial. Surg Endosc 22(3):757–762
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
John. E. Wennergren, Margaret Plymale, Daniel Davenport, Salomon Levy, Jeffrey Hazey, Kyle A. Perry, Kyle Stigall, and J. Scott Roth have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Wennergren, J.E., Plymale, M., Davenport, D. et al. Quality-of-life scores in laparoscopic preperitoneal inguinal hernia repair. Surg Endosc 30, 3467–3473 (2016). https://doi.org/10.1007/s00464-015-4631-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-015-4631-x