Abstract
Background
Although enhanced recovery programs (ERPs) have been proven to be beneficial after laparoscopic colon surgery, they may result in adverse clinical outcomes following failure. This study analyzed risk factors associated with ERP failure after laparoscopic colon cancer surgery.
Methods
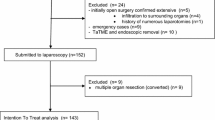
We analyzed the outcomes of 208 patients who underwent ERPs following laparoscopic colon cancer surgery between June 2007 and April 2013. The ERP included early oral feeding, early ambulation, and regular laxative administration. ERP failure was defined as postoperative hospital stay of more than 5 days related to postoperative complications, unplanned readmission within 30 days of surgery, or death.
Results
Surgical procedures included anterior resection (n = 101), right hemicolectomy (n = 90), and left hemicolectomy (n = 17). The mean postoperative hospital stay was 6.5 ± 2.3 days (range 3–24 days). ERP failure occurred in 36 patients (17.3 %), with no mortality; reasons included ileus (n = 14), wound infection (n = 4), chylous drainage (n = 3), anastomotic bleeding (n = 3), pneumonia (n = 1), or readmission (n = 11) owing to delayed complications. Univariable analysis showed that ERP failure was associated with proximal colon cancer, side-to-side anastomosis, longer operation time, increased blood loss, and longer resected specimen length. Multivariable analysis showed that side-to-side anastomosis [odds ratio (OR) 4.534; 95 % confidence interval (CI) 1.902–10.811; P = 0.001] and increased blood loss (OR 1.004; 95 % CI 1.001–1.008; P = 0.041) were independent risk factors for ERP failure.
Conclusions
We showed that increased blood loss and side-to-side anastomosis in comparison with end-to-end anastomosis were independent risk factors associated with ERP failure after laparoscopic colon cancer surgery. This suggests that intraoperative elements may be important determinants to obtain successful postoperative recovery in the era of ERP.

Similar content being viewed by others
References
Chestovich PJ, Lin AY, Yoo J (2013) Fast-track pathways in colorectal surgery. Surg Clin N Am 93:21–32
Wind J, Hofland J, Preckel B, Hollmann MW, Bossuyt PM, Gouma DJ, van Berge Henegouwen MI, Fuhring JW, Dejong CH, van Dam RM, Cuesta MA, Noordhuis A, de Jong D, van Zalingen E, Engel AF, Goei TH, de Stoppelaar IE, van Tets WF, van Wagensveld BA, Swart A, van den Elsen MJ, Gerhards MF, de Wit LT, Siepel MA, van Geloven AA, Juttmann JW, Clevers W, Bemelman WA (2006) Perioperative strategy in colonic surgery; LAparoscopy and/or FAst track multimodal management versus standard care (LAFA trial). BMC surg 6:16
Soop M, Carlson GL, Hopkinson J, Clarke S, Thorell A, Nygren J, Ljungqvist O (2004) Randomized clinical trial of the effects of immediate enteral nutrition on metabolic responses to major colorectal surgery in an enhanced recovery protocol. Br J Surg 91:1138–1145
Kehlet H, Wilmore DW (2008) Evidence-based surgical care and the evolution of fast-track surgery. Ann Surg 248:189–198
Wilmore DW, Kehlet H (2001) Management of patients in fast track surgery. BMJ 322:473–476
Nicholson A, Lowe MC, Parker J, Lewis SR, Alderson P, Smith AF (2014) Systematic review and meta-analysis of enhanced recovery programmes in surgical patients. Br J Surg 101:172–188
Lee TG, Kang SB, Kim DW, Hong S, Heo SC, Park KJ (2011) Comparison of early mobilization and diet rehabilitation program with conventional care after laparoscopic colon surgery: a prospective randomized controlled trial. Dis Colon Rectum 54:21–28
Vlug MS, Wind J, Hollmann MW, Ubbink DT, Cense HA, Engel AF, Gerhards MF, van Wagensveld BA, van der Zaag ES, van Geloven AA, Sprangers MA, Cuesta MA, Bemelman WA, group Ls (2011) Laparoscopy in combination with fast track multimodal management is the best perioperative strategy in patients undergoing colonic surgery: a randomized clinical trial (LAFA-study). Ann Surg 254:868–875
Zhuang CL, Ye XZ, Zhang XD, Chen BC, Yu Z (2013) Enhanced recovery after surgery programs versus traditional care for colorectal surgery: a meta-analysis of randomized controlled trials. Dis Colon Rectum 56:667–678
Brown SR, Mathew R, Keding A, Marshall HC, Brown JM, Jayne DG (2014) The impact of postoperative complications on long-term quality of life after curative colorectal cancer surgery. Ann Surg 259:916–923
Keller DS, Bankwitz B, Nobel T, Delaney CP (2014) Using frailty to predict who will fail early discharge after laparoscopic colorectal surgery with an established recovery pathway. Dis Colon Rectum 57:337–342
Stottmeier S, Harling H, Wille-Jorgensen P, Balleby L, Kehlet H (2012) Postoperative morbidity after fast-track laparoscopic resection of rectal cancer. Colorectal Dis 14:769–775
Choi YS, Lee SI, Lee TG, Kim SW, Cheon G, Kang SB (2007) Economic outcomes of laparoscopic versus open surgery for colorectal cancer in Korea. Surg Today 37:127–132
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications. Ann Surg 240:205–213
Neville A, Lee L, Antonescu I, Mayo NE, Vassiliou MC, Fried GM, Feldman LS (2014) Systematic review of outcomes used to evaluate enhanced recovery after surgery. Br J Surg 101:159–170
Aarts MA, Okrainec A, Glicksman A, Pearsall E, Victor JC, McLeod RS (2012) Adoption of enhanced recovery after surgery (ERAS) strategies for colorectal surgery at academic teaching hospitals and impact on total length of hospital stay. Surg Endosc 26:442–450
Bergman S, Feldman LS, Barkun JS (2006) Evaluating surgical outcomes. Surg Clin N Am 86:129–149
Lawrence VA, Hazuda HP, Cornell JE, Pederson T, Bradshaw PT, Mulrow CD, Page CP (2004) Functional independence after major abdominal surgery in the elderly. J Am Coll Surg 199:762–772
Kulaylat AN, Dillon PW, Hollenbeak CS, Stewart DB (2015) Determinants of 30-d readmission after colectomy. J Surg Res 193:528–535
Kassin MT, Owen RM, Perez SD, Leeds I, Cox JC, Schnier K, Sadiraj V, Sweeney JF (2012) Risk factors for 30-day hospital readmission among general surgery patients. J Am Coll Surg 215:322–330
Wu WC, Trivedi A, Friedmann PD, Henderson WG, Smith TS, Poses RM, Uttley G, Vezeridis M, Eaton CB, Mor V (2012) Association between hospital intraoperative blood transfusion practices for surgical blood loss and hospital surgical mortality rates. Ann Surg 255:708–714
Stowers M, Lemanu DP, Coleman B, Hill AG, Munro JT (2014) Review article: perioperative care in enhanced recovery for total hip and knee arthroplasty. J Orthop Surg (Hong Kong) 22:383–392
Artinyan A, Nunoo-Mensah JW, Balasubramaniam S, Gauderman J, Essani R, Gonzalez-Ruiz C, Kaiser AM, Beart RW Jr (2008) Prolonged postoperative ileus-definition, risk factors, and predictors after surgery. World J Surg 32:1495–1500
He X, Chen Z, Huang J, Lian L, Rouniyar S, Wu X, Lan P (2014) Stapled side-to-side anastomosis might be better than handsewn end-to-end anastomosis in ileocolic resection for Crohn’s disease: a meta-analysis. Dig Dis Sci 59:1544–1551
Guo Z, Li Y, Zhu W, Gong J, Li N, Li J (2013) Comparing outcomes between side-to-side anastomosis and other anastomotic configurations after intestinal resection for patients with Crohn’s disease: a meta-analysis. World J Surg 37:893–901
Kyzer S, Gordon PH (1992) The stapled functional end-to-end anastomosis following colonic resection. Int J Colorectal Dis 7:125–131
Yamamoto T, Keighley MR (1999) Stapled functional end-to-end anastomosis in Crohn’s disease. Surg Today 29:679–681
Clawson DK (1953) Side-to-side intestinal anastomosis complicated by ulceration, dilatation, and anemia: a physiologically unsound procedure; review of the literature and presentation of a case. Surgery 34:254–257
Ackland TH (1961) Complications and dangers of side-to-side intestinal anastomosis. ANZ J Surg 30:265–267
Abbruzzese AA, Curtis LE (1966) Chronic blood loss as a late complication of side-to-side small bowel anastomosis. Gastroenterology 51:399–402
Adachi Y, Matsushima T, Mori M, Sugimachi K, Oiwa T (1993) Blind loop syndrome: multiple ileal ulcers following side-to-side anastomosis. Pathology 25:402–404
Lennert KA (1979) The small-intestine-stasis syndrome following side-to-side anastomosis. Chirurg 50:21–25
Walfish J, Frankel A (1979) Chronic pseudo-obstruction secondary to side-to-side intestinal anastomosis. Arch Surg 114:1075–1078
Moon SB, Park KJ, Moon JS, Choe EK, So IS, Jung SE (2011) Migrating motor complex changes after side-to-side ileal bypass in mouse ileum ex vivo: mechanism underlying the blind loop syndrome? J Korean Surg Soc 80:251–259
Nygren J, Thorell A, Ljungqvist O (2001) Preoperative oral carbohydrate nutrition: an update. Curr Opin Clin Nutr Metab Care 4:255–259
Rahbari NN, Zimmermann JB, Schmidt T, Koch M, Weigand MA, Weitz J (2009) Meta-analysis of standard, restrictive and supplemental fluid administration in colorectal surgery. Br J Surg 96:331–341
Zingg U, Miskovic D, Hamel CT, Erni L, Oertli D, Metzger U (2009) Influence of thoracic epidural analgesia on postoperative pain relief and ileus after laparoscopic colorectal resection: benefit with epidural analgesia. Surg Endosc 23:276–282
Slim K, Vicaut E, Launay-Savary MV, Contant C, Chipponi J (2009) Updated systematic review and meta-analysis of randomized clinical trials on the role of mechanical bowel preparation before colorectal surgery. Ann Surg 249:203–209
Gustafsson UO, Scott MJ, Schwenk W, Demartines N, Roulin D, Francis N, McNaught CE, MacFie J, Liberman AS, Soop M, Hill A, Kennedy RH, Lobo DN, Fearon K, Ljungqvist O (2012) Guidelines for perioperative care in elective colonic surgery: Enhanced Recovery After Surgery (ERAS(R)) Society recommendations. Clin Nutr 31:783–800
Collin A, Jung B, Nilsson E, Pahlman L, Folkesson J (2014) Impact of mechanical bowel preparation on survival after colonic cancer resection. Br J Surg 101:1594–1600
Acknowledgments
The Medical Research Collaborating Center, Seoul National University Bundang Hospital, Korea, provided support for statistical analysis. The authors are indebted to J. Patrick Barron, Professor Emeritus of Tokyo Medical University and Adjunct Professor of Seoul National University Bundang Hospital for his contributions to manuscript editing.
Disclosures
Heung-Kwon Oh, Myong Hun Ihn, Il Tae Son, Jin Taek Park, Jaebong Lee, Duck-Woo Kim, and Sung-Bum Kang have no potential conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Oh, HK., Ihn, M.H., Son, I.T. et al. Factors associated with failure of enhanced recovery programs after laparoscopic colon cancer surgery: a single-center retrospective study. Surg Endosc 30, 1086–1093 (2016). https://doi.org/10.1007/s00464-015-4302-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-015-4302-y