Abstract
Background
Up to 41 % of patients report pain after cholecystectomy and in most studies follow-up for these symptoms did not exceed 5 years. The episodic nature of abdominal pain associated with symptomatic cholelithiasis warrants long-term follow-up studies. We assessed which patient and surgical factors were associated with absence of pain and patient-reported success of surgery after ≥5 years of follow-up.
Methods
Patients of ≥18 years of age with symptomatic cholelithiasis, classified as ASA I or II, who had previously returned a preoperative questionnaire were sent a questionnaire consisting of the gastrointestinal quality of life index (GIQLI) and patient ratings of current versus presurgical abdominal symptoms and of surgery result. Logistic regression analysis was performed to determine associations.
Results
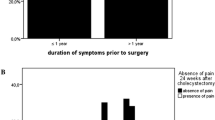
Questionnaires were sent to 197 patients and returned by 126 (64.0 %) patients (73.8 % female, mean age at surgery 47.5 ± 12.2 years) at a mean of 10.0 ± 1.0 years after cholecystectomy. Absence of abdominal pain was reported by 60.3 % of the patients. Patients classified as ASA II as opposed to ASA I were less likely to report absence of pain (OR 0.41, 95 % CI 0.17–0.99). A positive rating of long-term postsurgical versus presurgical abdominal symptoms was given by 89.7 % of the patients and 90.5 % considered the cholecystectomy result to be good. No variables were significantly associated with these latter two outcome measures.
Conclusions
We found a high patient-reported surgery success rate after >5 years of follow-up after cholecystectomy despite residual abdominal pain in some of these patients. None of the patient and surgery-related characteristics were consistently associated with all three outcome measures. This discrepancy between patient’ outcomes highlights the need for realistic expectations prior to cholecystectomy.


Similar content being viewed by others
References
Everhart JE, Ruhl CE (2009) Burden of digestive diseases in the United States Part III: liver, biliary tract, and pancreas. Gastroenterology 136:1134–1144
Shaffer EA (2006) Gallstone disease: epidemiology of gallbladder stone disease. Best Pract Res Clin Gastroenterol 20:981–996
Halldestam I, Enell EL, Kullman E, Borch K (2004) Development of symptoms and complications in individuals with asymptomatic gallstones. Br j surg 91:734–738
Heaton KW, Braddon FE, Mountford RA, Hughes AO, Emmett PM (1991) Symptomatic and silent gall stones in the community. Gut 32:316–320
Wittenburg H (2010) Hereditary liver disease: gallstones. Best Pract Res Clin Gastroenterol 24:747–756
Everhart JE, Ruhl CE (2009) Burden of digestive diseases in the United States part I: overall and upper gastrointestinal diseases. Gastroenterology 136:376–386
Jones C, Mawhinney A, Brown R (2012) The true cost of gallstone disease. Ulst med J 81:10–13
Keus F, de Jonge T, Gooszen HG, Buskens E, van Laarhoven CJ (2009) Cost-minimization analysis in a blind randomized trial on small-incision versus laparoscopic cholecystectomy from a societal perspective: sick leave outweighs efforts in hospital savings. Trials 10:80
Lamberts MP, Lugtenberg M, Rovers MM, Roukema AJ, Drenth JP, Westert GP, van Laarhoven CJ (2013) Persistent and de novo symptoms after cholecystectomy: a systematic review of cholecystectomy effectiveness. Surg Endosc 27:709–718
Thistle JL, Longstreth GF, Romero Y, Arora AS, Simonson JA, Diehl NN, Harmsen WS, Zinsmeister AR (2011) Factors that predict relief from upper abdominal pain after cholecystectomy. Clin Gastroenterol Hepatol 9:891–896
Ahmed R, Freeman JV, Ross B, Kohler B, Nicholl JP, Johnson AG (2000) Long term response to gallstone treatment–problems and surprises. Eur J surg 166:447–454
Konsten J, Gouma DJ, von Meyenfeldt MF, Menheere P (1993) Long-term follow-up after open cholecystectomy. Br J surg 80:100–102
Sand J, Pakkala S, Nordback I (1996) Twenty to thirty year follow-up after cholecystectomy. Hepatogastroenterology 43:534–537
Schmidt M, Sondenaa K, Vetrhus M, Berhane T, Eide GE (2011) A randomized controlled study of uncomplicated gallstone disease with a 14-year follow-up showed that operation was the preferred treatment. Dig Surgery 28:270–276
Vetrhus M, Berhane T, Soreide O, Sondenaa K (2005) Pain persists in many patients five years after removal of the gallbladder: observations from two randomized controlled trials of symptomatic, noncomplicated gallstone disease and acute cholecystitis. J Gastrointest Surg 9:826–831
Fisher ES, Wennberg DE, Stukel TA, Gottlieb DJ, Lucas FL, Pinder EL (2003) The implications of regional variations in medicare spending. Part 2: health outcomes and satisfaction with care. Ann Intern Med 138:288–298
Fisher ES, Wennberg DE, Stukel TA, Gottlieb DJ, Lucas FL, Pinder EL (2003) The implications of regional variations in medicare spending. Part 1: the content, quality, and accessibility of care. Ann Intern Med 138:273–287
Harrison EM, O’Neill S, Meurs TS, Wong PL, Duxbury M, Paterson-Brown S, Wigmore SJ, Garden OJ (2012) Hospital volume and patient outcomes after cholecystectomy in Scotland: retrospective, national population based study. BMJ 344:e3330
Keus F, de Vries J, Gooszen HG, van Laarhoven CJ (2008) Laparoscopic versus small-incision cholecystectomy: health status in a blind randomised trial. Surg Endosc 22:1649–1659
Eypasch E, Williams JI, Wood-Dauphinee S, Ure BM, Schmulling C, Neugebauer E, Troidl H (1995) Gastrointestinal Quality of Life Index: development, validation and application of a new instrument. Br J Surg 82:216–222
Nieveen Van Dijkum EJ, Terwee CB, Oosterveld P, Van Der Meulen JH, Gouma DJ, De Haes JC (2000) Validation of the gastrointestinal quality of life index for patients with potentially operable periampullary carcinoma. Br J Surg 87:110–115
Black N, Petticrew M, Hunter D, Sanderson C (1993) Day surgery: development of a national comparative audit service. Qual Health Care 2:162–166
Black N, Sanderson C (1993) Day surgery; development of a questionnaire for eliciting patients’ experiences. Qual Health Care 2:157–161
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP, Initiative S (2008) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61:344–349
Quintana JM, Cabriada J, Arostegui I, Oribe V, Perdigo L, Varona M, Bilbao A (2005) Health-related quality of life and appropriateness of cholecystectomy. Ann Surg 241:110–118
Weinert CR, Arnett D, Jacobs D Jr, Kane RL (2000) Relationship between persistence of abdominal symptoms and successful outcome after cholecystectomy. Arch Intern Med 160:989–995
Bitzer EM, Lorenz C, Nickel S, Dorning H, Trojan A (2008) Assessing patient-reported outcomes of cholecystectomy in short-stay surgery. Surg Endosc 22:2712–2719
Zapf M, Denham W, Barrera E, Butt Z, Carbray J, Wang C, Linn J, Ujiki M (2013) Patient-centered outcomes after laparoscopic cholecystectomy. Surg Endosc 27:4491–4498
Festi D, Reggiani ML, Attili AF, Loria P, Pazzi P, Scaioli E, Capodicasa S, Romano F, Roda E, Colecchia A (2010) Natural history of gallstone disease: expectant management or active treatment? Results from a population-based cohort study. J Gastroenterol Hepatol 25:719–724
Turner JA, Deyo RA, Loeser JD, Von Korff M, Fordyce WE (1994) The importance of placebo effects in pain treatment and research. JAMA 271:1609–1614
American College of P (2008) Information on cost-effectiveness: an essential product of a national comparative effectiveness program. Ann Intern Med 148:956–961
Disclosures
Mark P. Lamberts, Brenda L. Den Oudsten, Frederik Keus, Jolanda De Vries, Cornelis J. H. M. van Laarhoven, Gert P. Westert, Joost P. H. Drenth, Jan A. Roukema have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lamberts, M.P., Oudsten, B.L.D., Keus, F. et al. Patient-reported outcomes of symptomatic cholelithiasis patients following cholecystectomy after at least 5 years of follow-up. Surg Endosc 28, 3443–3450 (2014). https://doi.org/10.1007/s00464-014-3619-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3619-2