Abstract
Background
The project aimed at testing the feasibility of a quality improvement system based on patient-reported outcomes in short-stay surgery for cholecystectomy.
Methods
In two centers for short-stay surgery, patients referred for laparoscopic cholecystectomy were surveyed between Aug 1999 and Jan 2002. Patients reported on health-related quality of life (SF-36), symptoms (gallstone symptom checklist, GSCL) and other indicators preoperatively (T0), 14 days (T1) and 6 months postoperatively (T2). The SF-36 subscales physical functioning, bodily pain, and role physical as well as the GSCL and treatment satisfaction at T2 were considered as main outcomes. The main outcomes were analyzed by generalized linear models with regard to predictors.
Results
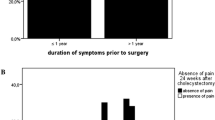
At T0 a total of 205 patients were included. The response rate at T2 was 63.4% (74.6% females, 53.6 years of age). The GSCL score at T0 (29.4% preoperatively) fell slightly to 27.9% at T1 and decreased to 14.8% at T2 (T0–T2: p < 0.001). The SF-36 subscales showed a different course over time (decrease of health-related quality of life at T1 and large increase at T2). The level of satisfaction with the outcome of cholecystectomy was 82.3%. The patient-reported outcomes were mainly influenced by the preoperative level, age and self-reported postoperative complaints.
Conclusion
The low response rate was mainly due to nondelivery of questionnaires at T1 during the regular postoperative visit by the operating physician. Though nonresponse occurs under conditions of routine care, meaningful information was gained, which should be used for quality improvement activities. Because the preoperative level is a major determinant of the postoperative health outcomes, the prospective pre–post measurement should be preferred if institutional comparisons are intended.

Similar content being viewed by others
Abbreviations
- BP:
-
Bodily pain
- GHP:
-
General health perception
- GSCL:
-
Gall stone symptom checklist
- MH:
-
Mental health
- PF:
-
Physical functioning
- RE:
-
Role emotional
- RP:
-
Role physical
- SF:
-
Social functioning
- SF-36:
-
Short form-36
- VI:
-
Vitality
References
Bardsley MJ, Venables CW, Watson J, Goodfellow J, Wright PD (1992) Evidence for validity of a health status measure in assessing short term outcomes of cholecystectomy. Qual Health Care 1:10–14
Berthou J, Dron B, Charbonneau P, Moussalier K, Pellissier L (2007) Evaluation of laparoscopic treatment of common bile duct stones in a prospective series of 505 patients: indications and results. Surg Endosc. doi:10.1007/s00464-007-9387-5, May 24, 2007
Bitzer EM, Grobe TG, Dörning H, Schwartz FW (2006) GEK-Report akut-stationäre Versorgung 2006. Asgard, St. Augustin
Bitzer EM, Nickel S, Lorenz C, Dörning H, Trojan A (2006) Prozess- und ergebnisorientiertes Qualitätsmanagement in der Kurzzeitchirurgie mit Patientenbefragungen. Z Ärztl Fortbild Qualitätssich 100:189–195
Black NA, Thompson E, Sanderson CFB, ECHSS Group (1994) Symptoms and health status before and after six weeks after open cholecystectomy: a European cohort study. Gut 35:1301–1305
BQS-Bundesgeschäftsstelle Qualitätssicherung (2007) BQS-Bundesauswertung 2006 - Cholezystektomie. BQS-Outcome. Available at: http://www.bqs-outcome.de/2006/ergebnisse/leistungsbereiche/cholezystektomie/bu_Gesamt_12n1_2006_9n0.pdf. Accessed 15 February 2007
Bullinger M (1996) Erfassung der gesundheitsbezogenen Lebensqualität mit dem SF-36 Health Survey: Hinweise auf Bewertungsinstrumente zur Qualitätssicherung in der Rehabilitation - Blatt 7. Rehabilitation 35:XVII–XXXX
Bullinger M, Kirchberger I (1998) Der SF-36 Fragebogen zum Gesundheitszustand. Handanweisung. Hogrefe, Göttingen
Burney RE, Jones KR (2002) Ambulatory and admitted laparoscopic cholecystectomy patients have comparable outcomes but different functional health status. Surg Endosc 16:921–926
Eypasch E, Williams JI, Wood-Dauphinee S, Ure BM, Schmulling C, Neugebauer E, Troidl H (1995) Gastrointestinal Quality of Life Index: development, validation and application of a new instrument. Br J Surg 82:216–222
Garratt A, Schmidt L, Mackintosh A, Fitzpatrick R (2002) Quality of life measurement: bibliographic study of patient assessed health outcome measures. Br Med J 324:1417
Höfler M, Pfister H, Lieb R, Wittchen HU (2005) The use of weights to account for non-response and drop-out. Soc Psychiatr Psychiatr Epidemiol 40:291–299
Junginger T, Küchle R, Dutkowski P, Thumerer A (1998) Systematische klinikinterne Qualitätskontrolle in der Chirurgie 1993 bis 1997. Z. Ärztl. Fortbild. Qualitätssich 92:705–714
Kohlmann T, Steinke I, Berger K, Deck R, John J, Pohlabeln H, Rieger J, Nickel S, Uhlig S (2000) Empfehlungen zur Auswahl und Anwendung von Erhebungsinstrumenten und Auswertungsverfahren in der Public Health-Forschung. Public Health Forum 8:11–13
Lienert GA, Raatz U (1998) Testaufbau und Testanalyse. Beltz, Psychologie-Verl.-Union, Weinheim
McCullagh P, Nelder JA (1989) Generalized linear models, 2nd edn. Chapman and Hall, London
Norman GR, Wyrwich KW, Patrick DL (2007) The mathematical relationship among different forms of responsiveness coefficients. Qual Life Res 16:815–822
Rubin DB (1987) Multiple imputation for nonresponse in surveys. Wiley, New York
Schafer JL (1997) Analysis of incomplete multivariate data. Monographs on Statistics and Applied Probability 72. Chapman and Hall, New York
Schwartz FW, Bitzer EM, Dörning H, Walter U (2002) Evaluation und Qualitätsmanagement. In: Hurrelmann K, Laser E (Hg) Handbuch für Gesundheitswissenschaften. Juventa, Weinheim
Topcu O, Karakayali F, Kuzu MA, Ozdemir S, Erverdi N, Elhan A, Aras N (2003) Comparison of long-term quality of life after laparoscopic and open cholecystectomy. Surg Endosc 17:291–295
Troidl H, Kusche J, Vestweber KH, Eypasch E, Koeppen L, Bouillon B (1987) Quality of life: an important endpoint both in surgical practice and research. J Chronic Dis 40:523–528
Velanovich V (2000) Laparoscopic vs open surgery: a preliminary comparison of quality-of-life outcomes. Surg Endosc 14:16–21
Victorzon M, Tolonen P, Vuorialho T (2007) Day-case laparoscopic cholecystectomy: treatment of choice for selected patients? Surg Endosc 21:70–73
Wright CJ, Chambers GK, Robens-Paradise Y (2002) Evaluation of indications for and outcomes of elective surgery. CMAJ 167:461–466
Acknowledgements
We like to thank both cooperating surgical units, the Interdisciplinary Centre for Short-Stay Surgery at the Klinikum Nord-Heidberg and the Short-Stay Unit of the Klinik Eilbek, both located in Hamburg. The study was funded within the Northern German Public Health Research Association by the Federal Ministry of Education, Science, Research and Technology (Grant ID: 01 EG 9814/9).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bitzer, E.M., Lorenz, C., Nickel, S. et al. Assessing patient-reported outcomes of cholecystectomy in short-stay surgery. Surg Endosc 22, 2712–2719 (2008). https://doi.org/10.1007/s00464-008-9878-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-008-9878-z